OCT Vulnerable Plaque Natural History Studies Sergio Waxman

OCT & Vulnerable Plaque: Natural History Studies Sergio Waxman, M. D. Associate Director, Cardiac Catheterization Laboratory Director, Interventional Cardiology Training Program Director, Interventional Cardiology Research Lahey Clinic, Burlington, MA Associate Professor of Medicine Tufts University School of Medicine, Boston, MA

Sergio Waxman, MD I have no real or apparent conflicts of interest to report.

Natural History Studies for VP “Those who don’t know history are destined to repeat it” Edmund Burke (1729 -1797)

Natural History Studies of VP: What did we learn from PROSPECT? • Low rate of serious non-culprit events in that population (1% MI, no deaths). PROSPECT Events: Median 3. 4 year f/u

Natural History Studies of VP: What did we learn from PROSPECT? • Low rate of serious non-culprit events in that population (1% MI, no deaths). • The prevalence of high-risk lesions is relatively low (~1 in 4 pts).
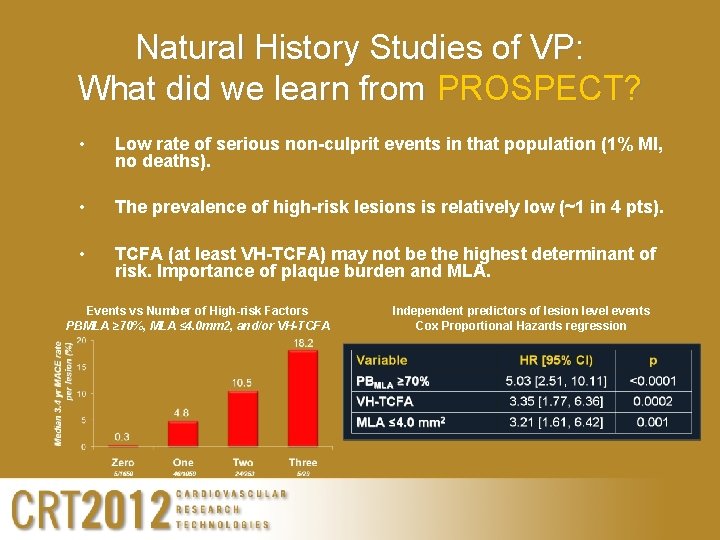
Natural History Studies of VP: What did we learn from PROSPECT? • Low rate of serious non-culprit events in that population (1% MI, no deaths). • The prevalence of high-risk lesions is relatively low (~1 in 4 pts). • TCFA (at least VH-TCFA) may not be the highest determinant of risk. Importance of plaque burden and MLA. Events vs Number of High-risk Factors PBMLA ≥ 70%, MLA ≤ 4. 0 mm 2, and/or VH-TCFA Independent predictors of lesion level events Cox Proportional Hazards regression

Natural History Studies of VP: What did we learn from PROSPECT? • Low rate of serious non-culprit events in that population (1% MI, no deaths). • The prevalence of high-risk lesions is relatively low (~1 in 4 pts). • TCFA (at least VH-TCFA) may not be the highest determinant of risk. Importance of plaque burden and MLA. • 3 -vessel imaging is not risk-free (1. 6% major complication rate).

Natural History Studies of VP: What did we learn from PROSPECT? • Low rate of serious non-culprit events in that population (1% MI, no deaths). • The prevalence of high-risk lesions is relatively low (~1 in 4 pts). • TCFA (at least VH-TCFA) may not be the highest determinant of risk. Importance of plaque burden and MLA. • 3 -vessel imaging is not risk-free (1. 6% major complication rate). • When high-risk lesions become symptomatic they usually present with angina and not death or MI (? dent in VP paradigm? ).

Natural History Studies of VP Using Intracoronary Imaging: • Are they really “natural history”? – Selected patients – On optimal medical treatment as per SOC • What are we imaging? How sensitive are technologies to detect “true” VP? – VH-IVUS – NIRS – OCT • What will we do with new knowledge? • Can we prove VP paradigm: Detection Treatment Outcome, or should we focus instead on more practical applications? (what are they? )

Natural History Studies of VP: Available Opportunities from Clinical Reality • What we can do are large registries, culprit vessel imaging (? Non-culprit vessels) • Focus on findings that may be associated with a measurable clinical effect and possibly related to an outcome • Study whether treatment strategy assigned to a finding can improve outcome(s) • Multimodality imaging may be a necessity

From technical feasibility to clinical adoption: Now that we can do it, what do we do with it? The following sequence has to be proven to have clinical acceptance: Imaging Finding Measurable effect Therapy Outcome Angioscopy IVUS OCT NIR-S Against: ● Risk ● Cost Possible clinical applications: • Optimizing PCI results: • Stent postdilatation to avoid underexpansion • Stent type according to healing response dependent on plaque type • Stent length dependent upon true lesion length (true margins) • Distal protection • Decision to treat intermediate lesions and VP • Intensity of adjuvant therapy (statins/DAPT) vs disease burden/plaque type
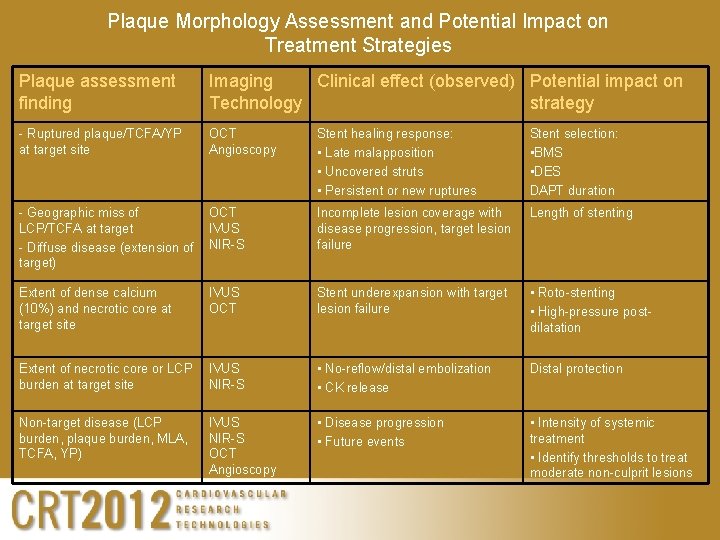
Plaque Morphology Assessment and Potential Impact on Treatment Strategies Plaque assessment finding Imaging Clinical effect (observed) Potential impact on Technology strategy - Ruptured plaque/TCFA/YP at target site OCT Angioscopy Stent healing response: • Late malapposition • Uncovered struts • Persistent or new ruptures Stent selection: • BMS • DES DAPT duration - Geographic miss of LCP/TCFA at target - Diffuse disease (extension of target) OCT IVUS NIR-S Incomplete lesion coverage with disease progression, target lesion failure Length of stenting Extent of dense calcium (10%) and necrotic core at target site IVUS OCT Stent underexpansion with target lesion failure • Roto-stenting • High-pressure postdilatation Extent of necrotic core or LCP burden at target site IVUS NIR-S • No-reflow/distal embolization • CK release Distal protection Non-target disease (LCP burden, plaque burden, MLA, TCFA, YP) IVUS NIR-S OCT Angioscopy • Disease progression • Future events • Intensity of systemic treatment • Identify thresholds to treat moderate non-culprit lesions
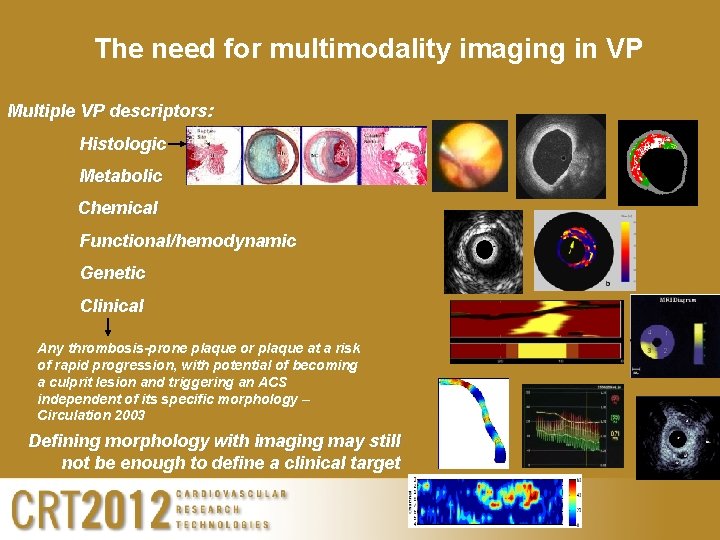
The need for multimodality imaging in VP Multiple VP descriptors: Histologic Metabolic Chemical Functional/hemodynamic Genetic Clinical Any thrombosis-prone plaque or plaque at a risk of rapid progression, with potential of becoming a culprit lesion and triggering an ACS independent of its specific morphology – Circulation 2003 Defining morphology with imaging may still not be enough to define a clinical target
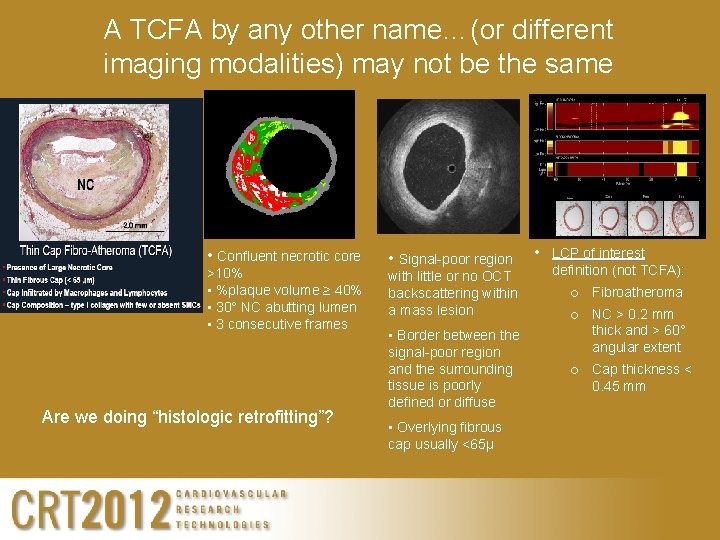
A TCFA by any other name…(or different imaging modalities) may not be the same • Confluent necrotic core >10% • %plaque volume ≥ 40% • 30° NC abutting lumen • 3 consecutive frames Are we doing “histologic retrofitting”? • Signal-poor region with little or no OCT backscattering within a mass lesion • Border between the signal-poor region and the surrounding tissue is poorly defined or diffuse • Overlying fibrous cap usually <65μ • LCP of interest definition (not TCFA): ¡ Fibroatheroma ¡ NC > 0. 2 mm thick and > 60° angular extent ¡ Cap thickness < 0. 45 mm
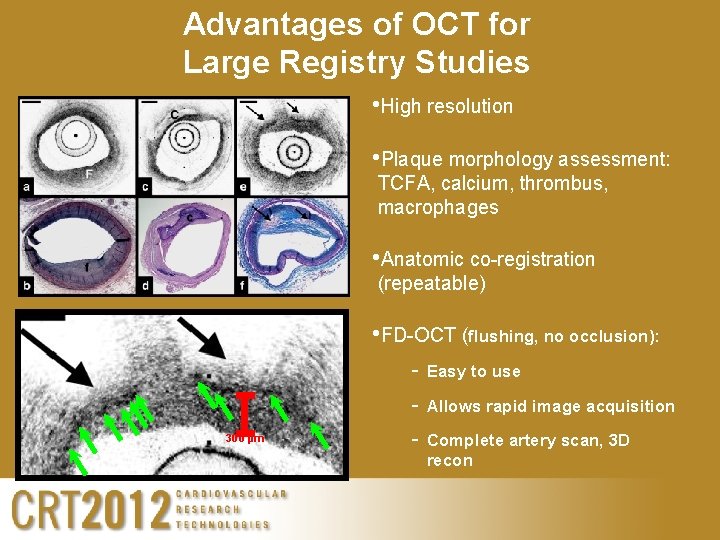
Advantages of OCT for Large Registry Studies • High resolution • Plaque morphology assessment: TCFA, calcium, thrombus, macrophages • Anatomic co-registration (repeatable) • FD-OCT (flushing, no occlusion): 300 µm - Easy to use - Allows rapid image acquisition - Complete artery scan, 3 D recon

Limitations of OCT • Depth information not possible • Limited ability to image ostial RCA/LM • Standardization of measurements required • Automatization of data acquisition and analysis/quantification required and need to be developed further • VP may be a moving target
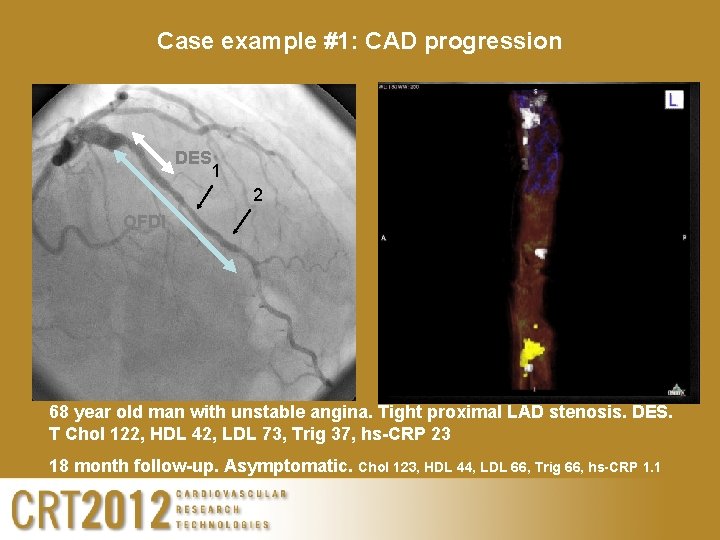
Case example #1: CAD progression DES 1 1 2 2 OFDI 68 year old man with unstable angina. Tight proximal LAD stenosis. DES. T Chol 122, HDL 42, LDL 73, Trig 37, hs-CRP 23 18 month follow-up. Asymptomatic. Chol 123, HDL 44, LDL 66, Trig 66, hs-CRP 1. 1
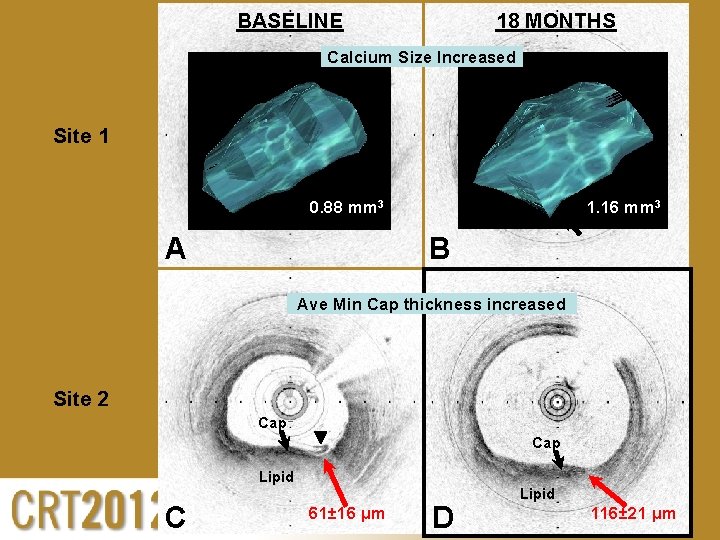
BASELINE 18 MONTHS Calcium Size Increased Site 1 0. 88 mm 3 A 1. 16 mm 3 B Ave Min Cap thickness increased Site 2 Cap Lipid C 61± 16 µm D Lipid 116± 21 µm
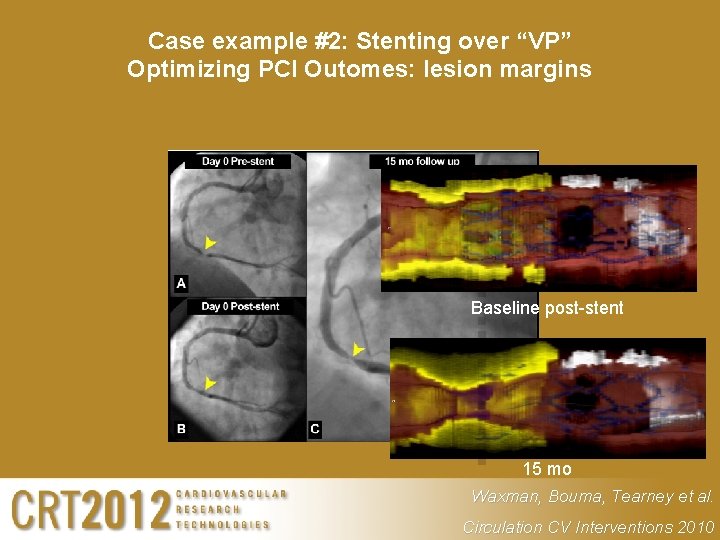
Case example #2: Stenting over “VP” Optimizing PCI Outomes: lesion margins Baseline post-stent 15 mo Waxman, Bouma, Tearney et al. Circulation CV Interventions 2010
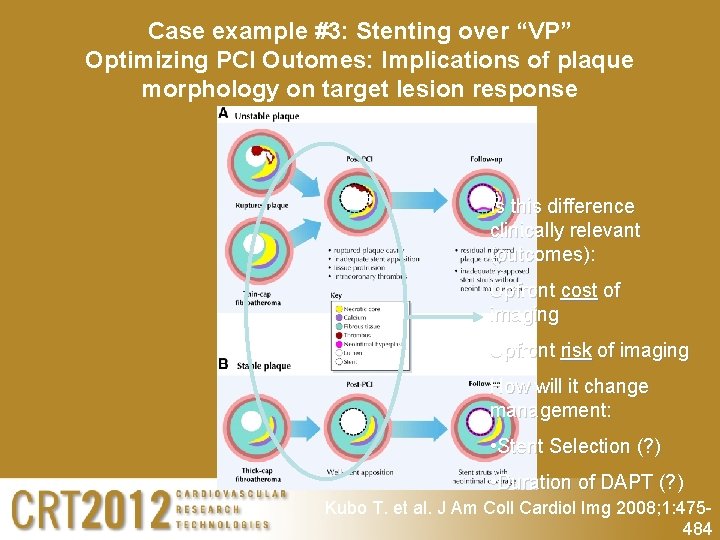
Case example #3: Stenting over “VP” Optimizing PCI Outomes: Implications of plaque morphology on target lesion response Is this difference clinically relevant (outcomes): Upfront cost of imaging Upfront risk of imaging How will it change management: • Stent Selection (? ) • Duration of DAPT (? ) Kubo T. et al. J Am Coll Cardiol Img 2008; 1: 475484

Importance of Natural History Studies Large Registry Studies • Understand progression/behavior of CAD, define vulnerable plaque • Optimize treatment of culprit lesions: – Lesion-specific treatment algorithms - Stent selection (DES, BMS or BVS), duration of antiplatelet therapy, length of stented area • Prevention of target lesion-related events (TLR and ST) Optimize treatment of non-culprit/non-target disease: – Development of treatment algorithms for intermediate stenoses and high risk lesions: - • Intensity of systemic therapy, thresholds for non-culprit intervention Guide efforts for non-invasive screening (mortality benefit? ): – Imaging (CT/MRI/Nuclear), biomarkers

MGH OCT Registry • Target 3000 patients x 3 years • 20 sites from Australia, China, Singapore, Japan, Korea, USA • Data collection started in 6/2010. More than 1, 000 pts enrolled as of November 2011 • PI: Dr. IK Jang
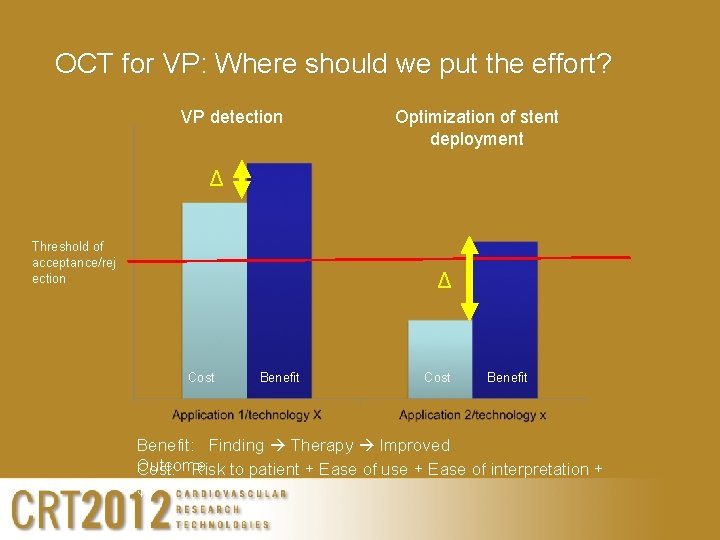
OCT for VP: Where should we put the effort? VP detection Optimization of stent deployment Δ Threshold of acceptance/rej ection Δ Cost Benefit: Finding Therapy Improved Outcome Cost: Risk to patient + Ease of use + Ease of interpretation + $$

Summary • The VP paradigm detection treatment outcome may be difficult to prove as indicated by prior “natural history” studies • Large Registry Studies using novel imaging modalities are needed to learn more about “VP”, but their true value may derive from identifying immediate applications of imaging (optimization of PCI results, treatment of intermediate lesions) • OCT is well positioned to provide clinically useful information that will enable clinicians to start asking the right questions

Summary (cont. ) • While OCT overcomes some of the limitations of VH-IVUS and other imaging technologies (higher resolution, more detail), its own limitations (no depth information) may require multimodality imaging, in particular for detection of VP • Efforts to put together large registry studies using OCT (alone or in combination with other modalities) are likely to derive benefits for more immediate applications than VP

Thank you
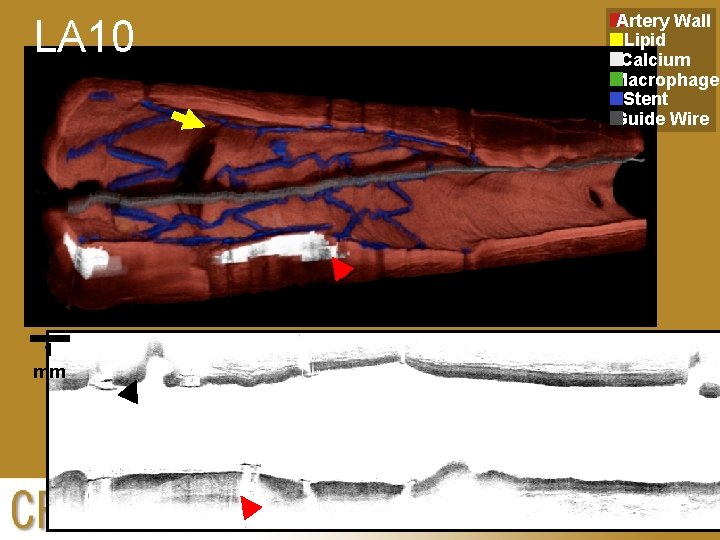
LA 10 1 mm Artery Wall Lipid Calcium Macrophages Stent Guide Wire
- Slides: 27