Occupational Medicine and NeedleStick Injuries Cass Djurfors October

Occupational Medicine and Needle-Stick Injuries Cass Djurfors October 10, 2002

Objectives: n Define Occupational Exposure n Review Infection Control Measures n Needlestick Injuries: risks n HIV n Hepatitis C n Hepatitis B n Post-exposure prophylaxis n Latex Allergy

Occupational Exposure: n Occupational Safety and Health Administration (USA): a “reasonably anticipated skin, eye, mucous membrane, or parenteral contact with blood or other potentially infectious materials that may result from the performance of the employee’s duties. ”

Occupational Exposure n At risk groups: n Health Care Workers: nurses, physicians, dentists, dental workers, lab and blood bank technologists, medical examiners, phlebotomists, ED personnel, intensive care and operating room technicians, orderlies, housekeeping staff, laundry workers n Non Health Care Workers: law enforcement, fire, rescue, EMS, correctional facilities, research lab workers, funeral industry employees

At risk activities: n Intravenous access n Suturing n Phlebotomy n Ng and og n Recapping of n n needles Specimen handling Med injection Lumbar puncture Chest tube insertion n n placement Intubation Urinary catheter insertion Hemorrhage control Any airborne or direct contact

Infectious Agents: n Parenteral: HIV, Hepatitis B and C n Airborne/droplet: measles, varicella, TB, H. flu, N. meningitidis, pertussis, adenovirus, influenza, mumps, rubella, the plague and others n Contact: C. difficile, pediculosis, scabies, diphtheria, HSV, enteric organisms (E. coli, Hepatitis A, etc. ), RSV, viral hemorrhagic infections (Ebola, Lassa, Marburg) and others

Infection Control Measures: n Although risk estimation may be made by history, there is no reliable method of identifying all infectious patients, therefore… Universal Precautions!!!

Infection Control: n Handwashing n Cleaning, sterilizing and disinfecting of patient care equipment and exposed surfaces n Laundering of contaminated uniforms, clothing and linens n Proper sharps and infectious waste disposal n Appropriate isolation and patient placement

Infection Control: n Personal Protective Equipment (PPE): n Gloves n Masks n Eye protection n Face shields n Gowns/aprons

Needlestick Injuries: n Exposure is common: 52% of health care workers report at least one prior exposure, 24% within the preceding year n Under-reported: estimates suggest that only 10% of exposures are actually reported
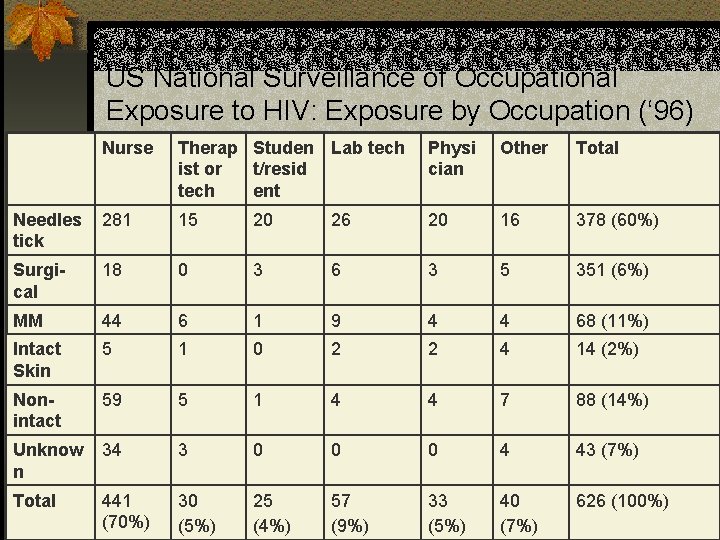
US National Surveillance of Occupational Exposure to HIV: Exposure by Occupation (‘ 96) Nurse Therap Studen Lab tech ist or t/resid tech ent Physi cian Other Total Needles tick 281 15 20 26 20 16 378 (60%) Surgical 18 0 3 6 3 5 351 (6%) MM 44 6 1 9 4 4 68 (11%) Intact Skin 5 1 0 2 2 4 14 (2%) Nonintact 59 5 1 4 4 7 88 (14%) Unknow n 34 3 0 0 0 4 43 (7%) Total 441 (70%) 30 (5%) 25 (4%) 57 (9%) 33 (5%) 40 (7%) 626 (100%)
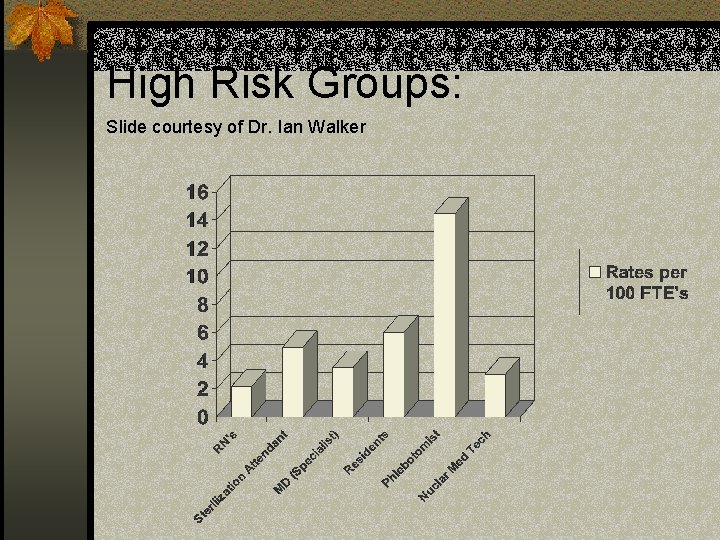
High Risk Groups: Slide courtesy of Dr. Ian Walker
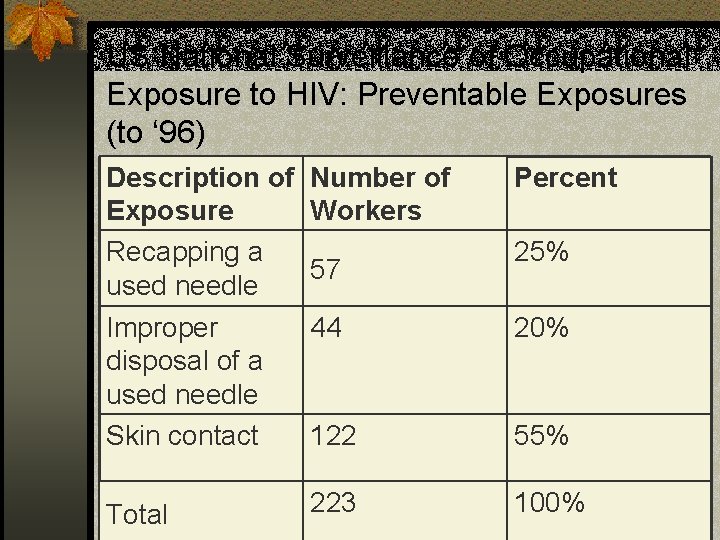
US National Surveillance of Occupational Exposure to HIV: Preventable Exposures (to ‘ 96) Description of Number of Exposure Workers Recapping a 57 used needle Percent Improper disposal of a used needle Skin contact 44 20% 122 55% Total 223 100% 25%

HIV: The Risk n Generally reported in the literature as 0. 3% on average for a percutaneous exposure n Mucous Membrane: 0. 1% n Skin exposure: <0. 1% n Seroconversion has been reported with non -intact skin. No reported events have occurred with intact skin although a theorectical risk remains.
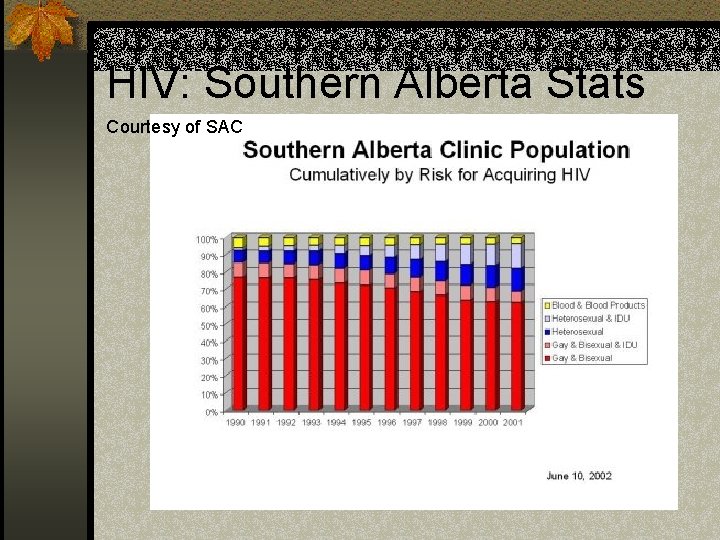
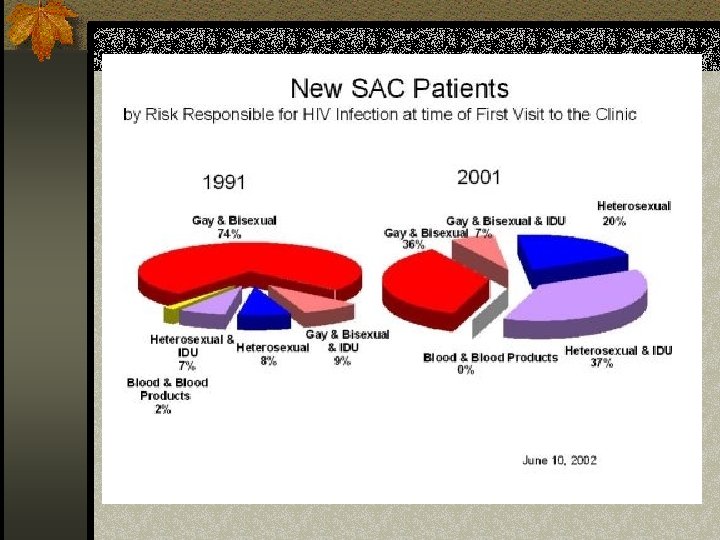
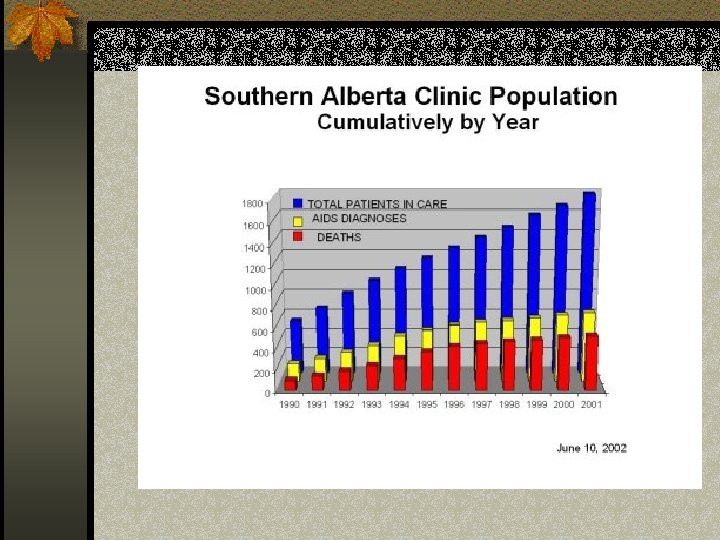
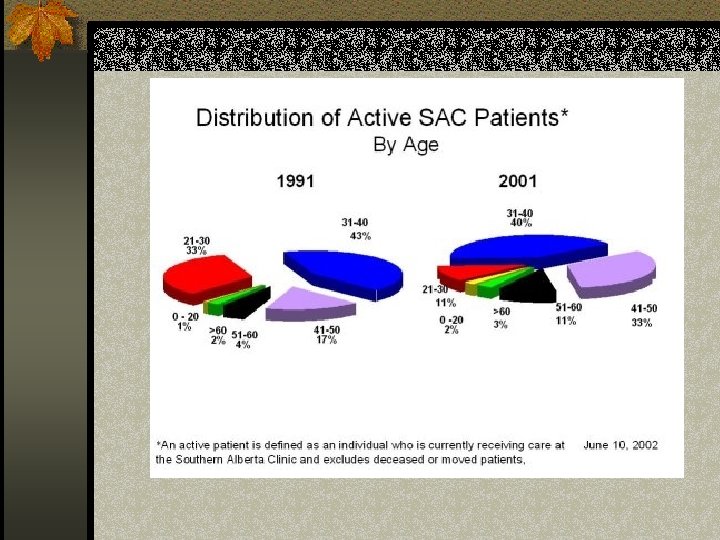
HIV: Southern Alberta Stats Courtesy of SAC
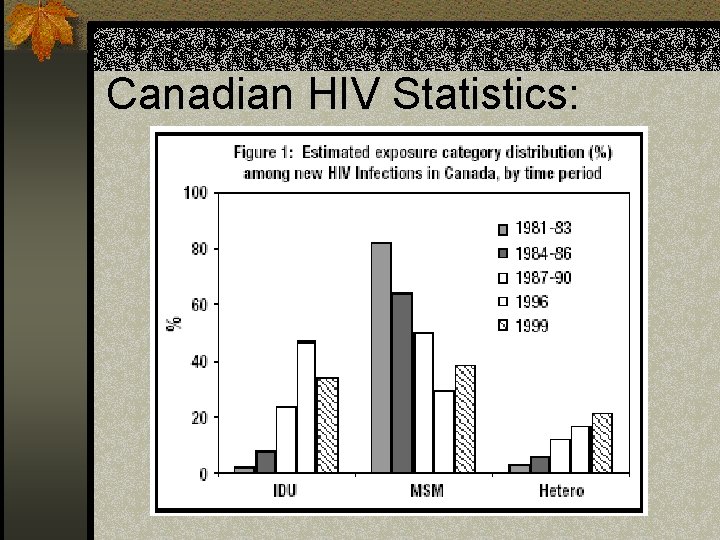
Canadian HIV Statistics:

HIV Risk Assessment: Needlesticks n Risk is increased by: n High viral load in source patient n Deep injury n Volume of blood/visible blood on device n Death of source patient of AIDS in 60 days n Gauge of needle n Procedure involving an artery or vein

Post Exposure Prophylaxis n The evidence: n 1994 study showing that zidovudine administered to an HIV-infected mother during pregnancy and labour, then to the infant post-partum reduced the risk of HIV transmission to the baby from 25% to 9% (67% relative risk reduction) n Case-control study of HCWs the showed zidovudine PEP reduced seroconversion by 79% (however, ARR=0. 24, NNT=417) n PEP has had documented failures

When to give PEP? n Most effective within 1 to 2 hours post- exposure. n May be given up to 72 hours post. n Consider it for anyone who has received a percutanous or acute sexual exposure n Start ASAP and continue for 4 weeks

Who gets PEP? n The current SAC (and CDC) guidelines state: n “Prophylaxis is recommended for incidents with highest or increased risk of transmission following percutaneous exposure to blood. Prophylaxis is not offered for percutaneous skin exposure to nonbloody body fluids. In other situations of intermediate risk, prophylaxis is offered and the decision rests with the individual to make a decision whether to initiate prophylaxis based on the best information available and their personal acceptance of risk. ”

PEP: the drugs n Basic Regimen: n Combivir (AZT 300 mg + 3 TC 150 mg) bid n Expanded Regimen: n Basic Regimen + Nelfinavir 1250 mg bid n Other: n consider other drugs for source patients already on antiretrovirals or for patients with a known resistant virus

Who gets What? n Basic regimen is given to most exposures n Expanded regimen is prescribed in consultation with ID for those patients with significant exposure to known HIV +ve source n Studies done with AZT alone, but 3 TC is added out of concern for resistance and from known superiority in treatment of HIV+ patients

Current SAC Guidelines 1 Is the source known HIV+? n Yes: proceed to step 2 of protocol n No: n Test source (with consent) using rapid point-ofcare HIV test available through CLS at any Emergency Room or 8 th and 8 th health centre n If negative, and no risk of “window period”, reassure n If source unknown or refuses testing and has risks for or symptoms of HIV, proceed to step 2 of protocol n Consider source testing for HBV, HCV

Current SAC Guidelines 2 Timing and Type of Exposure: n Assess fluid type, volume, viral titre, mode of exposure. n Assess exact timing of exposure 3 Decision: n Make a decision for or against PEP based on risk assessment

Current SAC Guidelines 1. Drug Selection n Basic Regimen for most exposures n Expanded regimen for significant exposure to a known HIV+ source (concern is that a resistant organism may have been transmitted) n If the source patient is already on antiretrovirals or has a virus with know resistance, alternative drugs may be used

Current SAC Guidelines 1. Duration of Prophylaxis: n Start ASAP and continue for 4 weeks 2. Adverse reactions: n 88% with two-drug prophylaxis n 97% with three-drug prophylaxis n Majority are GI: N/V/D and can be managed with antiemetics/antidiarrheals n Long-term adverse effects such as lipodystrophy and DM are rare with PEP

Current SAC Guidelines 7 Access and Cost: n Starter kits contain 72 hours of drugs n Free for occupational exposure and nonvoluntary or violent (assault) exposures n Non-occupational voluntary exposures (needles or sex): PEP is available, but cost not absorbed by CHR

Current SAC Guidelines 8 Follow-up: n Baseline HIV, HBV, HCV, CBC, Cr, and LFTs should be done in recipient n Follow-up with ID at HPTP clinic within 72 hours n HIV testing at 6 wks, 12 wks, 6 months

Current SAC Guidelines 9 Other considerations: n For occupational exposures: n WCB Physician’s First Report n Employee Accident Report form #00169 n Prevent transmission while in 6 month window period: n Abstain from intercourse or use condoms n Avoid pregnancy n Discontinue breastfeeding n Do not donate blood, plasma, organs, tissues. . . n Do not share toothbrushes, razors, needles etc.

When to Speak to ID n Source patient already on antiretrovirals or has known resistant virus n Delayed exposure n Significant renal or hepatic disease n Unknown source n Pregnant or breast feeding patients

Rapid Point-Of-Care Testing n CLS test: Sensitivity and Specificity both 99. 9% n Current turn around time 1 hr 24 min n Confirmed by Western Blot at Prov Lab n Can be done as an “add-on” to serum sample n Legal and ethical issues involving incompetent, unconscious or dead patients

Hepatitis C n Virus discovered in 1988 n First immunoassay for anti-HCV available in 1990 n Most common chronic blood-borne infection in USA n n n (1 -2% of general population, prevalence no higher in health care workers) Acute infection usually asymptommatic Persistent infection develops in >85% Chronic hepatitis in 60 -70% Cirrhosis in 10 -20% Severity and progression of disease influenced by Et. OH, increasing age at time of infection, male sex, immunodeficiency

Hepatitis C n Prior to 1990: blood and blood product transfusion responsible for 90% of infections n Today: n risk with transfusion < 1 in 100 000 per unit n IVDU most common risk factor (60% of infections) n Average seroconversion rate with sharps exposure is 1. 8% n No PEP available

Hepatitis B n Adult infections: n 95% resolve spontaneously n 5% develop chronic hepatitis n Neonatal infections: n 90% progress to chronic infections

Hepatitis B n Vaccine available since 1982 n Unclear need for booster - consider at 10 years post immunization n Passive immunity available as HBIG: indicated for both unimmunized adults and neonates post exposure n Give within 12 hours n n Risk of seroconversion with needlestick: n 20% if source is HBSAg +ve n 66% is source is HBSAg +ve and HBe. Ag +ve

Hepatitis D n Co-infection with HBV or superinfection with chronic HBV carriers n Worsens severity of HBV illness
Latex Allergy n Latex: milky cytosol from rubber tree (Hevea brasiliensis) n Gloves, IV tubing, intravascular balloon catheters, airways, endotracheal tubes, oxygen masks, tourniquets, blood pressure cuffs, ECG leads, tape, dressings

Latex Allergy n Immune reactions may be n irritant n contact dermatitis (type IV) n Ig. E (type I)

Latex Allergy n Higher risk workers: n multiple allergies n eczema n multiple food allergies (banana, avocado) n frequent surgical or dental procedures n multiple urogenital procedures n spina bifida n congenital urinary anomalies n sensitivity to ethylene oxide

Thank you’s… n Dr. Ian Walker n SAC n FMC Pharmacy n Tintinalli n www
- Slides: 43