Occupational low back pain Dr mehdi habibollahi LBP

Occupational low back pain Dr mehdi habibollahi

LBP definition Low back pain was defined as pain and discomfort, localized below the costal margin and above the inferior gluteal folds, with or without leg pain (sciatica) (Omokhodion et al, 2002), and as “pain limited to the region between the lower margins of the 12 th rib and the glutei folds” with or without leg pain (sciatica) (Manek and Macgregor, 2005)

Low Back Pain epidemiology Back pain is second to the common cold as a cause of lost days at work. About 80% of people have at least one episode of low back pain during their lifetime. The most common age groups are the 30 s - 50 s. It usually feels like an ache, tension or stiffness in back.

Low Back Pain epidemiology Annual prevalence is 15 -20% 2 nd most common symptomatic reason for visits to primary care physicians. 90% of all episodes will resolve within 6 weeks regardless of treatment 90% of all persons disabled for more than 1 year will never work again without intense intervention

Low Back Pain epidemiology Most common cause of disability in people younger than 45. 1% of population is chronically disabled due to back problems.
Definitions Acute LBP: Back pain <6 weeks duration Sub acute LBP: back pain >6 weeks but <3 months duration Chronic LBP: Back pain disabling the patient from some life activity >3 months Recurrent LBP: Acute LBP in a patient who has had previous episodes of LBP from a similar location.

Categories of low back pain 1 -non specific LBP 2 - specific LBP

Categories of low back pain 1 - mechanical LBP 2 - non mechanical LBP

Differential: Mechanical LBP Lumbar Strain or Sprain (70%) Degenerative processes of disc and facets (10%) Herniated disc (4%) Osteoporotic Compression Fracture (4%) Spinal Stenosis (3%) Spondylolisthesis (2%) Traumatic Fractures (<1%) Congenital disease (<1%) Severe Kyphosis or Scoliosis Transitional Vertebrae Spondylolysis Internal Disc Disruption/Discogenic Back Pain Presumed Instability

Differential - Nonmechanical LBP: Neoplasia (0. 7%) Multiple Myeloma Metastatic Carcinoma Lymphoma and Leukemia Spinal Cord Tumors Retroperitoneal Tumors Primary Vertebral Tumors Infection (0. 01%) Osteomyelitis Septic Discitis Paraspinous Abscess Epidural Abscess Shingles Inflammatory Arthritis (0. 3%) – note HLA-B 27 association. Ankylosing Spondylitis Reiter Syndrome Inflammatory Bowel Disease Scheuermann Disease (osteochondrosis) Paget Disease

Differential – Visceral Disease: Pelvic organ involvement: Prostatitis Endometriosis Chronic Pelvic Inflammatory Disease Renal involvement Nephrolithiasis Pyelonephritis Perinephric Abscess Aortic Aneurysm Gastrointestinal involvement Pancreatitis Cholecystitis Penetrating Ulcer

Symptoms of Benign LBP Dull and achy quality Diffuse aching with associated muscle tenderness Exacerbated with movement Relieved with rest in recumbent position No radiation, paresthesias No dermatomal pattern Pt. is able to find a position of comfort DTR are within normal limits

Symptoms of Inflammatory back pain Gradually in onset. Throbbing in nature. Morning stiffness. Exacerbates by rest and relived by activity. Intensity increase in night and early morning. It is chronic backache.

LOW BACK PAIN RISK FACTORS Low back pain is a multifactor problem It is a biopsychosocial problem

BACK PAIN RISK FACTORS NON OCCUPATIONAL genome Poor posture Poor conditioning Weakness Stiffness Faulty body mechanics Poor work, sleep, or eating habits Smoking Psychosocial--bad attitude, stress, emotional Other pathology (i. e. fibromyalgia, chronic fatigue or pain syndrome, osteoporosis)
BACK PAIN RISK FACTORS Occupational risk factors Heavy Lifting Twisting Vibration Reaching & Lifting Carrying & Lifting Awkward Postures Sitting or Standing Slips, Trips & Falls
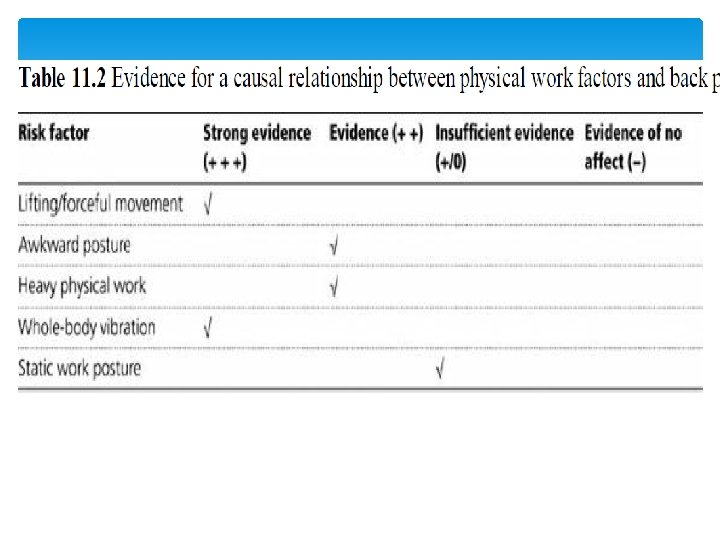

DIAGNOSIS Specific diagnosis is impossible in 80% Differentiation of muscle, joint, ligamentous structures Mechanical versus systemic disorders is possible Categorize by clinical symptoms Subtyping will improve therapy

Physical Examination Inspection Palpation Range of motion Strength testing Neurologic examination Special tests

Inspection Ideally with back and legs exposed. Posture ? Scoliosis ? Kyphosis Skin café-au-lait spots, hairy patches, signs of psoriasis. Prolapsed disc may cause a lumbar scoliosis, flattening or reversal of normal lumbar lordosis

Palpation Check for bone tenderness – this may indicate serious pathology eg infection, fracture, malignancy With patient leaning forwards check for tenderness between the vertebral spines and paraspinal muscles. Eg prolapsed disc, mechanical back pain SI joints Palpable steps may indicate spondylolisthesis

Movements Flexion – schobers test <5 cm = abnormal Extension – pain and restricted extension in prolapsed disc and spondylolisthesis Lateral Flexion Rotation – seated, movement is thoracic

Hip and SI joint examination Check hip joints for pain and limitation – internal rotation is often the earliest sign hip disease. FABER test. Place foot across knee of opposite leg, apply gentle pressure to knee and opposite ASIS. Pain in SI area may indicate a problems with these joints.

Abdominal and Cardiovascular examination Consider non musculoskeletal causes of back pain

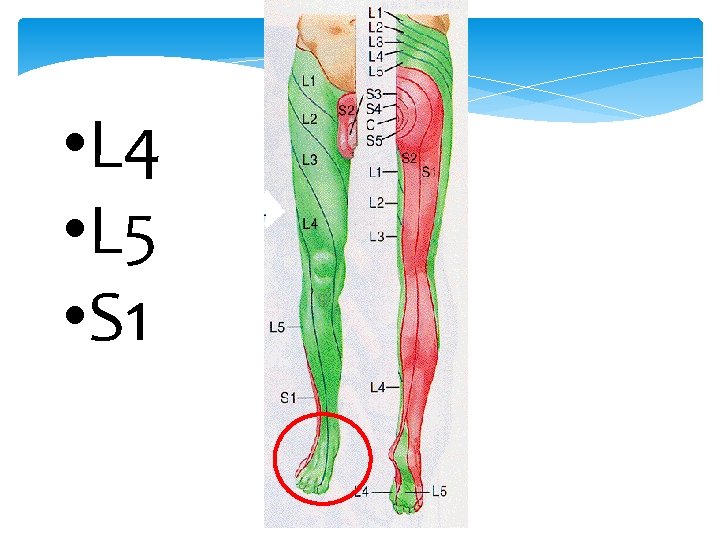
Straight leg raising Looking for nerve root irritation L 5 - S 1 Patient supine, passively raise leg with knee extended, stop when back or leg pain. <45 o positive Lower leg until the pain disappears then dorsiflex foot, pain or paraesthesia aggravated.

Look for further evidence of neurological involvement Patella (L 3 -4) Achilles (L 5 - S 1) reflexes Lower Limb power Test sensation to pin prick
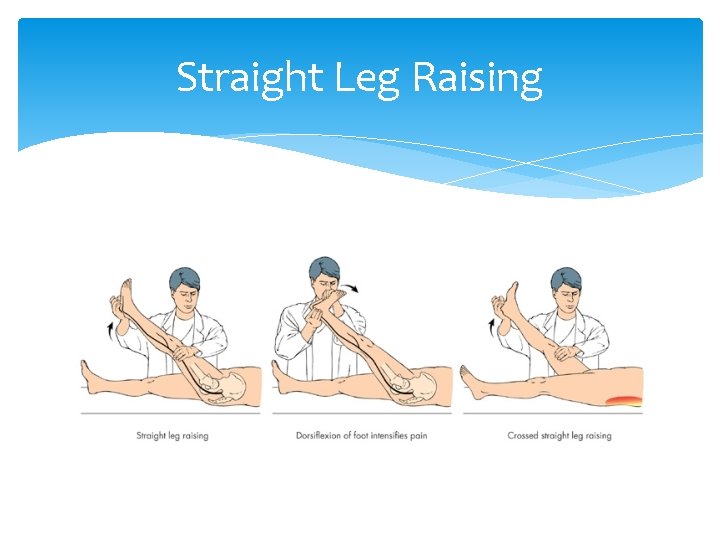
Straight Leg Raising

“Red Flags” in back pain Age < 15 or > 50 Fever, chills, UTI Significant trauma Unrelenting night pain; pain at rest Progressive sensory deficit Neurologic deficits Saddle-area anesthesia Urinary and/or fecal incontinence Major motor weakness Unexplained weight loss Hx or suspicion of Cancer Hx of Osteoporosis Hx of IV drug use, steroid use, immunosuppression Failure to improve after 6 weeks conservative tx

management
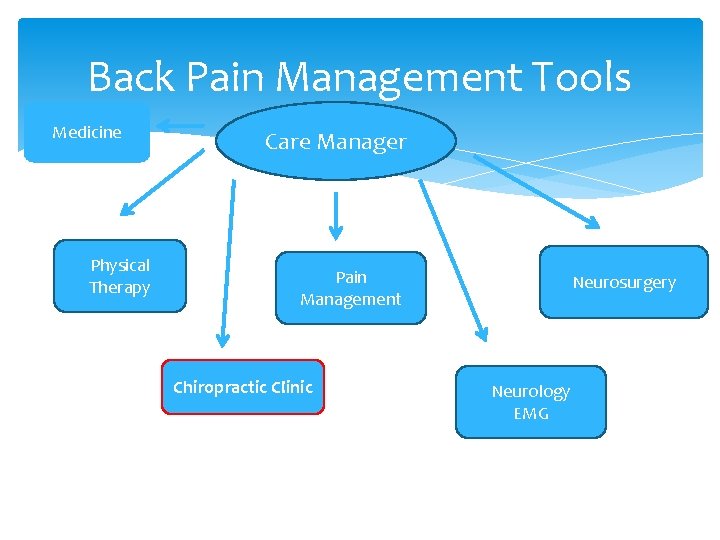
Back Pain Management Tools Medicine Physical Therapy Care Manager Pain Management Chiropractic Clinic Neurosurgery Neurology EMG

Pain Management: A More Flexible Approach* Different time frames Multiple therapies at one time Different starting points Complementary medicine, behavioral program s, adjuvant meds Corrective surgery Intrathecal therapy or neurostimulation Physical therapy, TENS NSAIDs, over-the-counter drugs Long-term oral opioids Chronic Pain Patient Neuroablation

Management Initially rest - perhaps with a board under the bed - was recommended for back pain. The new guidelines recommended active rehabilitation. The new principles of management involve keeping the patient active and giving analgesia to facilitate this. Give information, reassurance and advice. DO NOT prescribe bed rest. Advise to stay as active as possible. Prescribe regular pain relief (paracetamol, non-steroidal anti-inflammatory drugs) and consider a short course of muscle relaxants.

Other treatment options acupuncture – fine needles are inserted into your skin at certain points on the body exercise classes – aerobic exercise, muscle strengthening and stretching manual therapy – your back is massaged or manipulated

Referral guidance If red flags suggest a serious condition, refer with appropriate urgency. This means immediately for CES. If there is progressive, persistent or severe neurological deficit, refer for neurosurgical or orthopaedic assessment, preferably to be seen within 1 week. If pain or disability remain problematic for more than a week or two, consider early referral for physiotherapy or other physical therapy. If, after 6 weeks, sciatica is still disabling and distressing, refer for neurosurgical or orthopaedic assessment, preferably to be seen within 3 weeks. If pain or disability continue to be a problem despite appropriate pharmacotherapy and physical therapy, consider referral to a multidisciplinary back pain service or a chronic pain clinic.

Prevention Goal of the occupational medicine
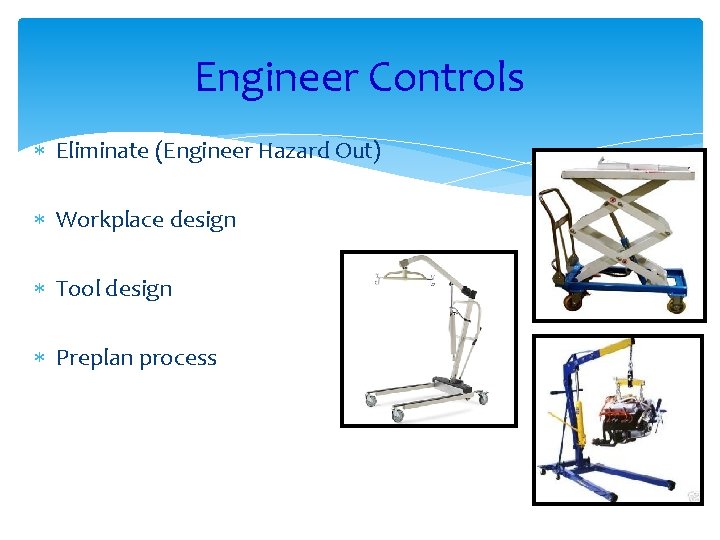
Engineer Controls Eliminate (Engineer Hazard Out) Workplace design Tool design Preplan process

Eliminate the Lift Use mechanical lifts when possible

Administrative Controls Training of employees and management Job rotation
Job Rotation Rotate to non-lifting tasks

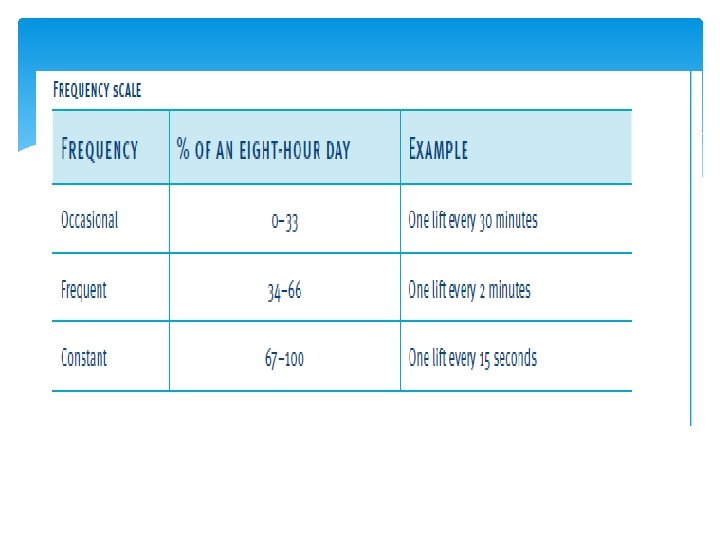
Pay Special Attention 1. Heavy lifting 2. Frequent lifting 3. Awkward lifting

Reduce Heavy Lifting 60 -70 pound wood pallet “Substitute” 20 pound plastic pallet
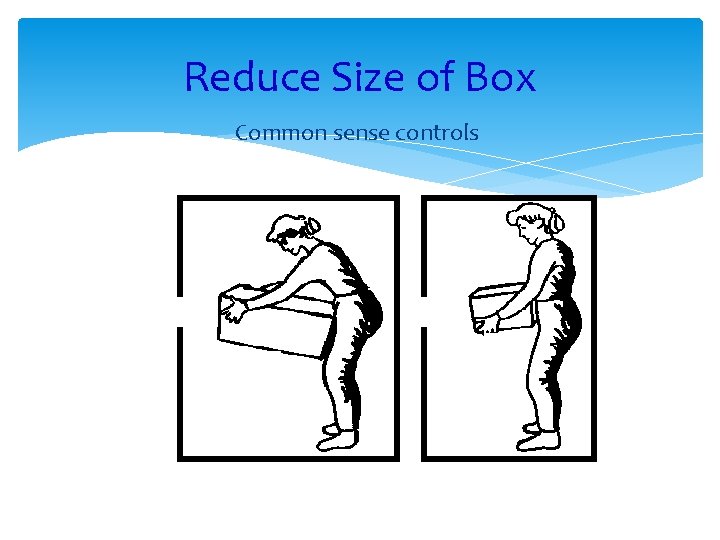
Reduce Size of Box Common sense controls

Reduce Heavy Lifting Use mechanical assistance

Slide Instead of Lift

Reduce Heavy Lifting Team Lifting*

Reduce Frequency Mechanical Assistance

Reduce Frequency Use Mobile Storage*

Reduce Awkward Lifting Raise load mechanically

Awkward Lifting Add Handles

Awkward Lifting Rearrange Storage

Awkward Lifting Mechanical assistance Stacker – stacks up to 12 feet high

Awkward Lifting To reduce twisting – use conveyors *

Size Up The Load Make sure you can lift the weight. Test load by picking up one end!

Proper Lifting Think defensively about your back Use common sense Follow good lifting techniques Keep load close to body
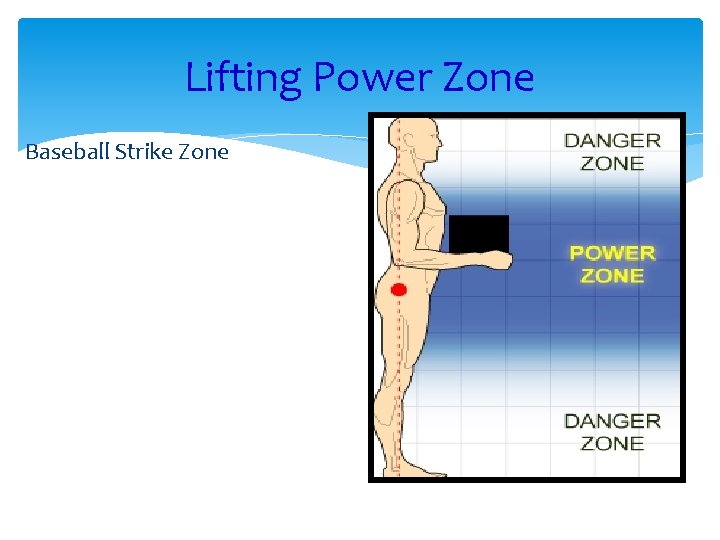
Lifting Power Zone Baseball Strike Zone

Lifting Techniques Lift with your legs, not your back Place your feet close to the object Center yourself over the load

Lifting Techniques Bend your knees Get a good hand hold Lift straight up smoothly

Don’t Twist or Turn Feet facing the lift Keep it steady No twisting/turning

Know Your Path! Is your path clear? Are there any holes? Are there any spilled liquids? Check your footing.

Set it Down Safely Just as critical to back safety as lifting Bend knees slowly Let legs do the work Don’t let go of the load until it is secure on the floor

Push vs. Pull If the object is on rollers, push Pushing puts less strain on your back Uses largest muscle group

RETURN TO WORK I CANNOT RETURN TO WORK!!!!!!!
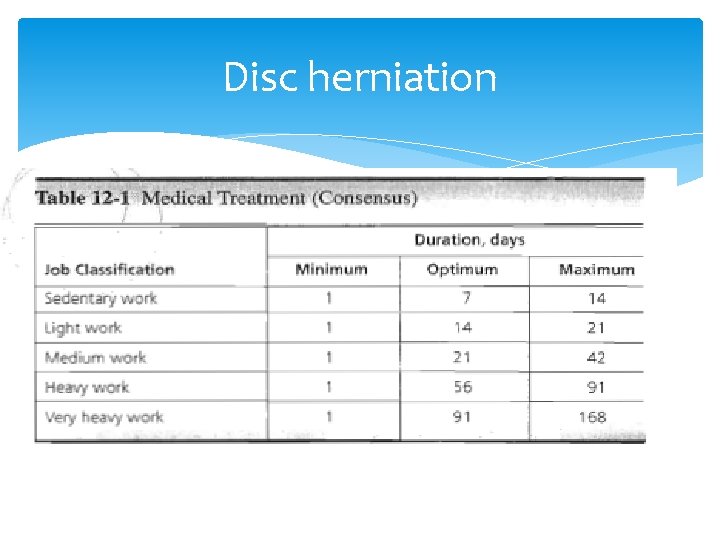
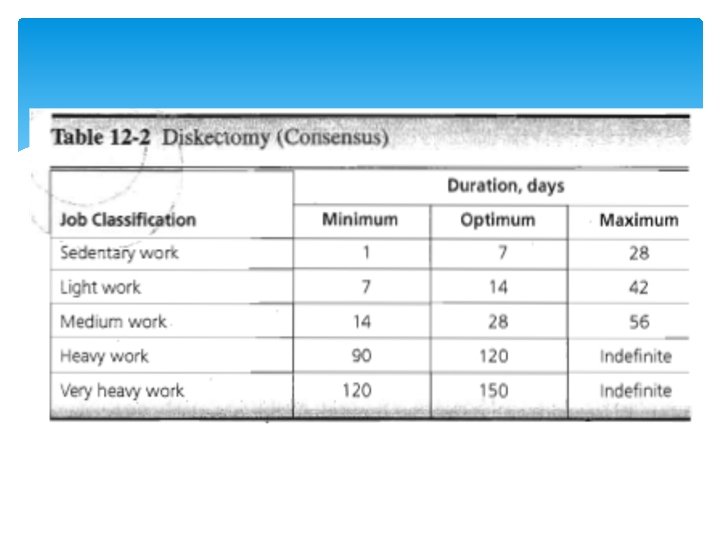
Disc herniation

PEARLS

Correlating Clinical and MRI Scan Findings in Low Back Pain.

Indications for MRI lumbar spine • Progressive neurological deficit- weakness most important • Cauda equina syndrome- bowel/bladder retention/incontinence, saddle anesthesia • No significant improvement with 4 -8 weeks of conservative therapy/PT • Severe, intractable pain • Red flags- fever, weight loss, previous cancer, IV drug use
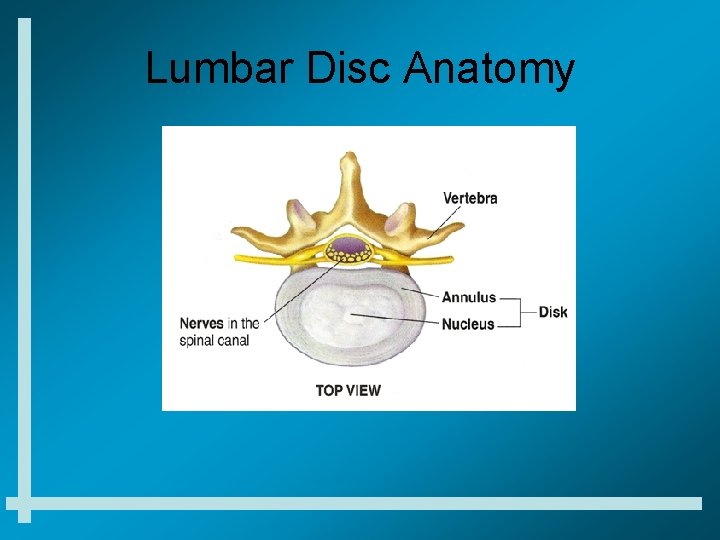
Lumbar Disc Anatomy
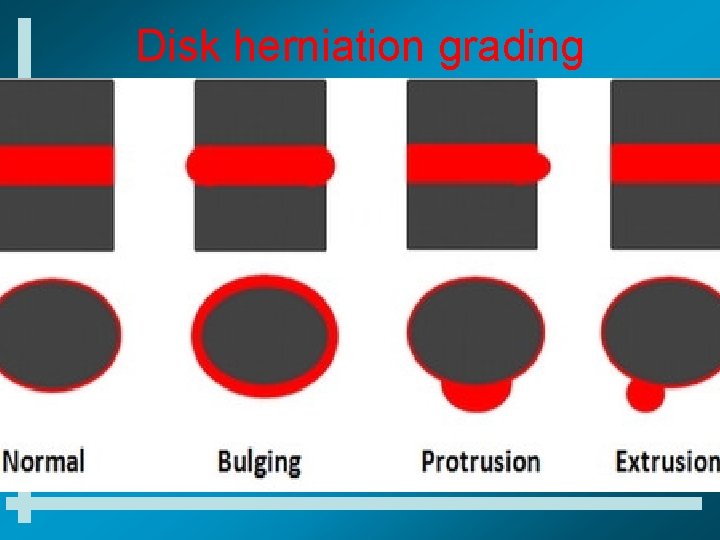
Disk herniation grading

Disc protrusion patterns • Central disc protrusion • Lateral disc protrusion • Far lateral/Foraminal disc protrusion
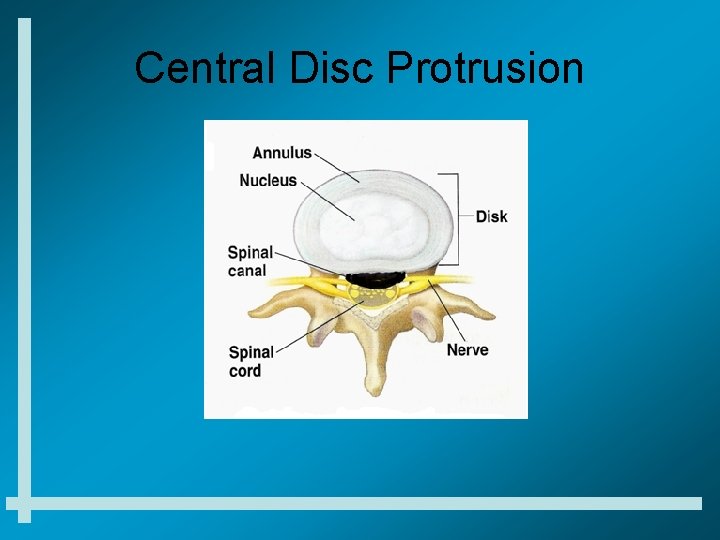
Central Disc Protrusion

Central Disc Protrusion General Characteristics • Frequent cause of recurrent mechanical/axial low back pain in the <50 year-old • Frequently injured/aggravated by flexion • Pain is frequently worse with coughing, sneezing, laughing or valsalva • Pain is frequently worse with prolonged sitting/long car ride • Normal lower extremity neuro exam
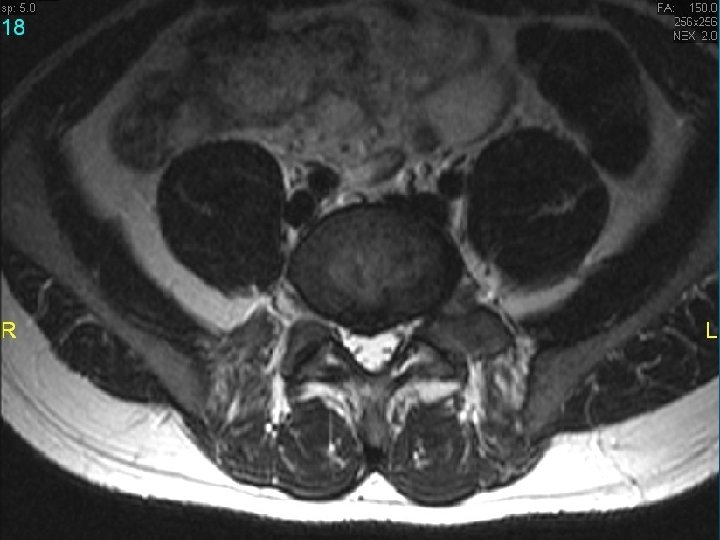
MRI scan slide #1
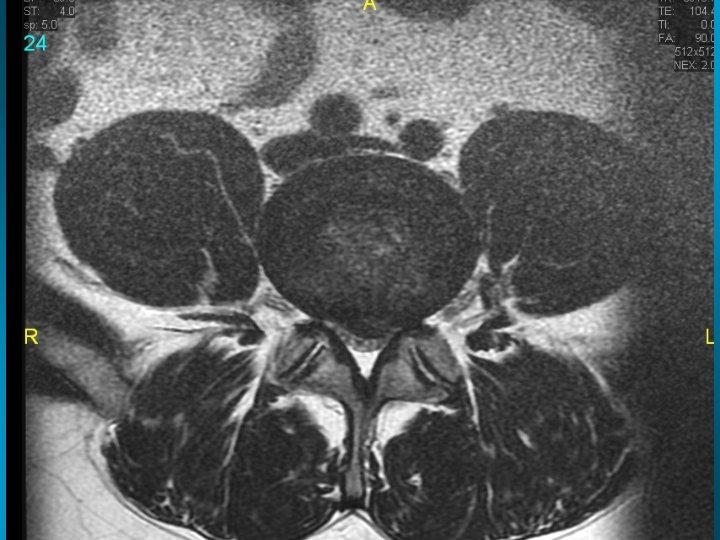
MRI scan slide #2
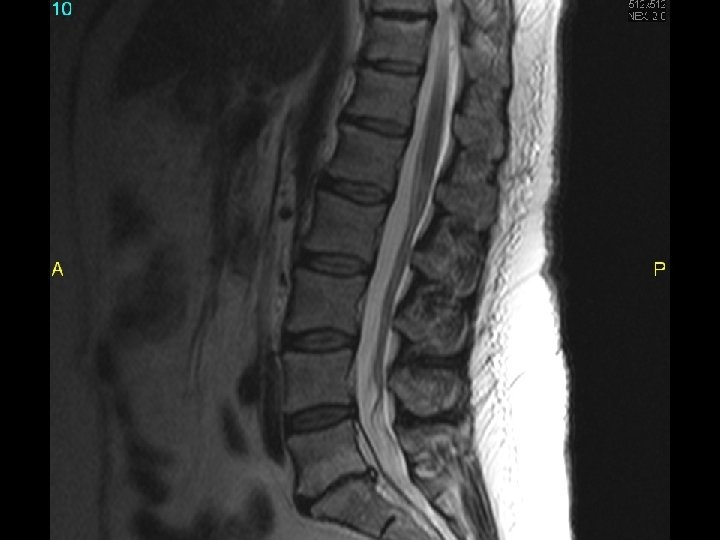
MRI scan slide #3
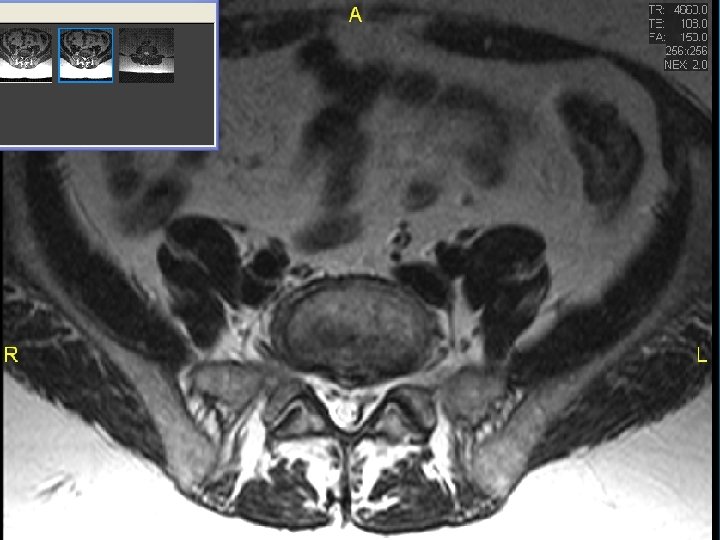
MRI scan slide #4
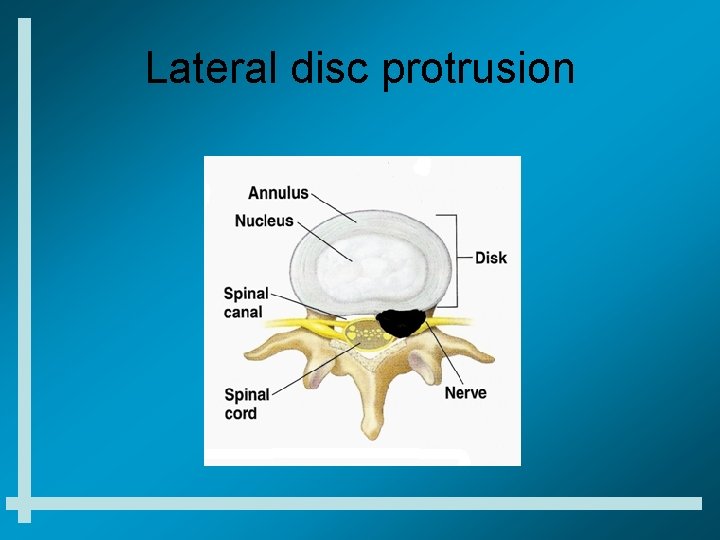
Lateral disc protrusion

Lateral disc protrusion general characteristics • Lower extremity radicular pain worse than low back pain • Lower extremity pain follows radicular and dermatomal pattern • Pain is generally worse with coughing and sneezing, valsalva maneuvers • Pain is generally worse with flexion and sitting • L 3 -4 disc-L 4 radicular pain, L 4 -5 disc- L 5 radicular pain, L 5 -S 1 disc- S 1 radicular pain

Lateral disc protrusion continued • Careful lower extremity neuro exam may be able to identify specific nerve root lesion • Straight leg raising usually reproduces radicular pain • May respond to oral steroids or transforaminal epidural steroid injections • Persisting pain may need discectomy to relieve lower extremity pain
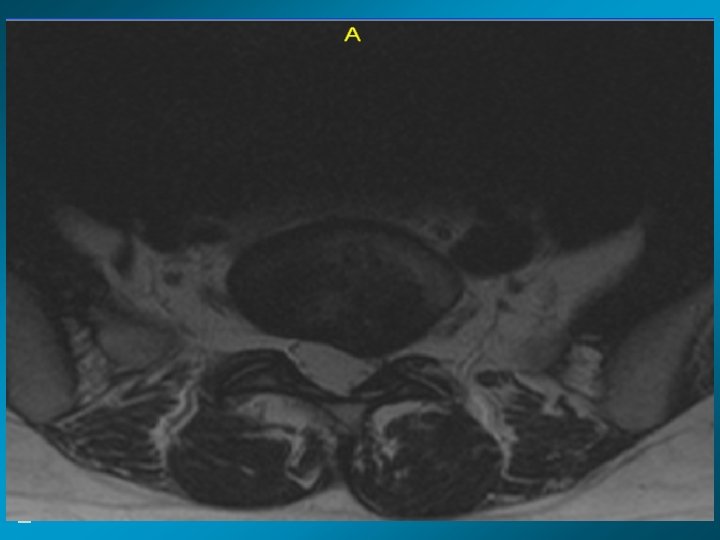
MRI scan slide #5
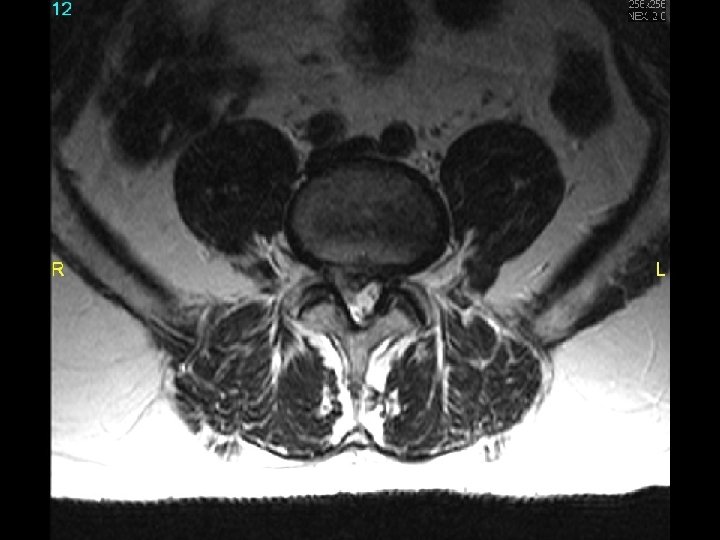
MRI scan slide #6
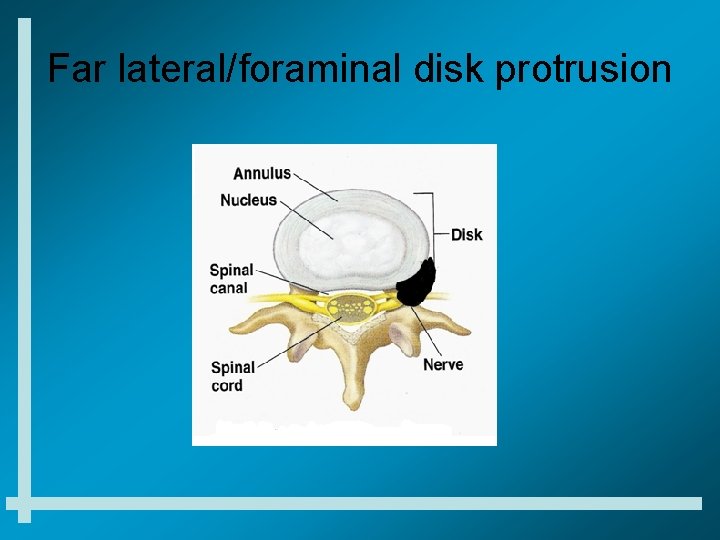
Far lateral/foraminal disk protrusion

Far lateral/foraminal disk protrusion general characteristics • Lower extremity radicular pain much worse with standing and walking, usually improved with sitting • Lower extremity pain follows radicular and dermatomal pattern • Usually not worsened by coughing or sneezing • Careful lower extremity neuro exam may be able to identify specific nerve root involvement • Diskectomy can be difficult because of facet joint blocking exposure
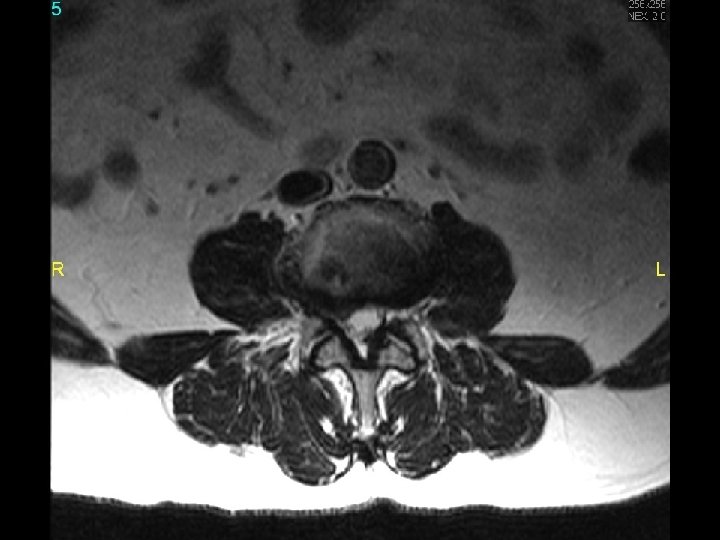
MRI scan slide #8
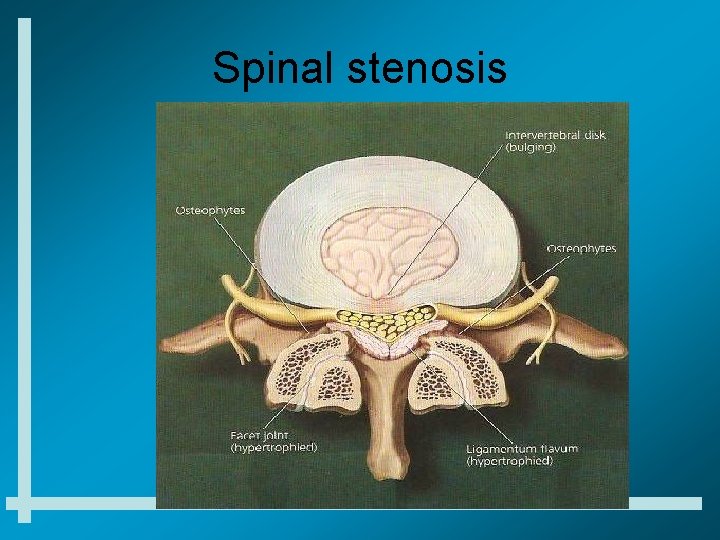
Spinal stenosis
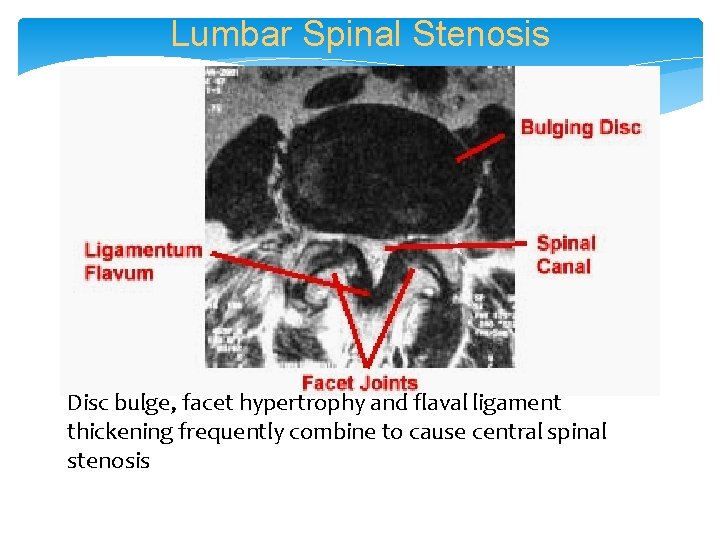
Lumbar Spinal Stenosis Disc bulge, facet hypertrophy and flaval ligament thickening frequently combine to cause central spinal stenosis
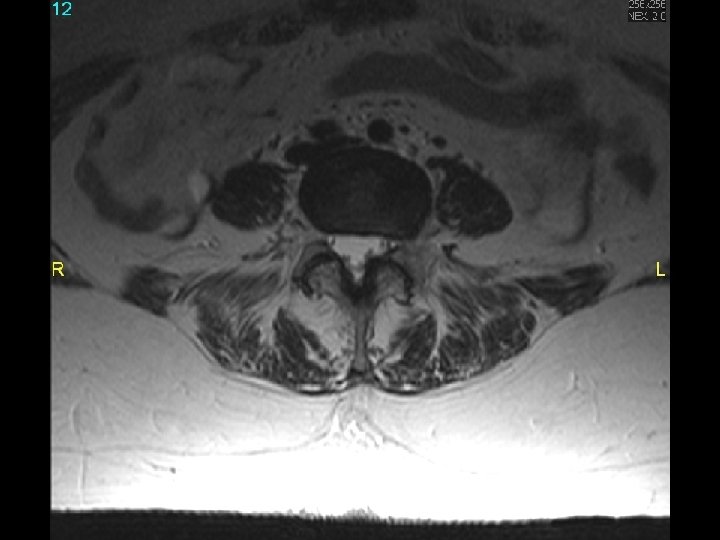
MRI scan slide # 12

Spinal stenosis • Low back pain with radiation to bilateral buttocks and lower extremities which is worse with prolonged standing and walking • Neurogenic claudication may need to rule out vascular claudication first • PT for stabilization and flexibility • Caudal epidural steroid injections • Surgical decompression for resistant cases
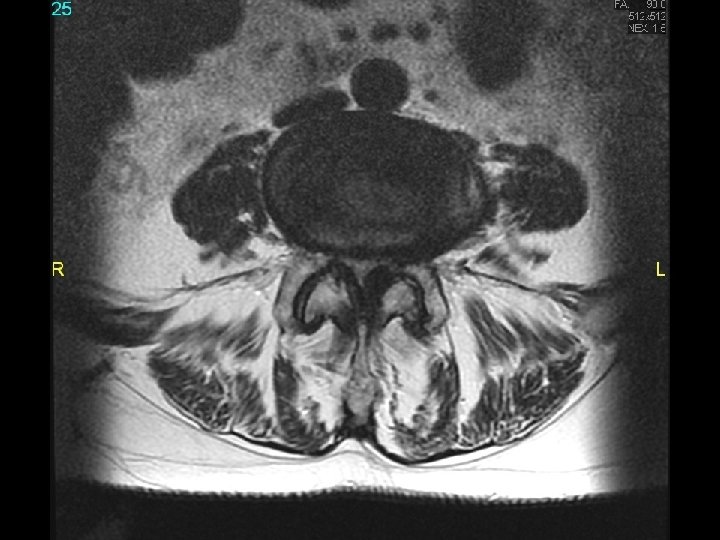
MRI scan slide #13
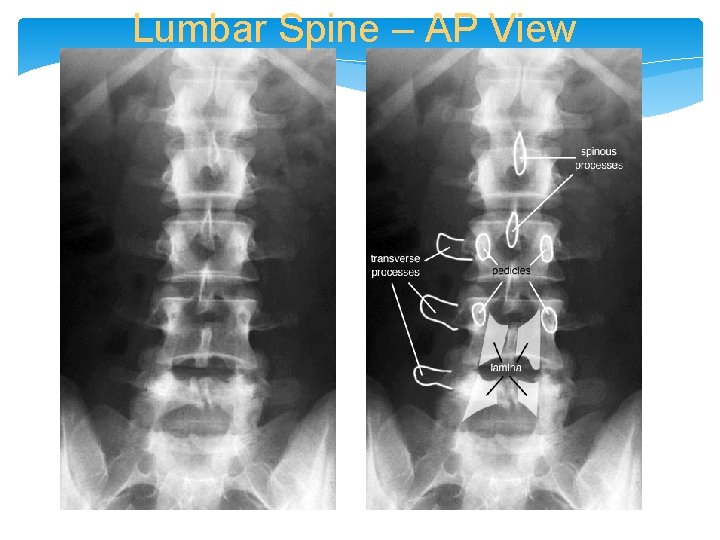
Lumbar Spine – AP View
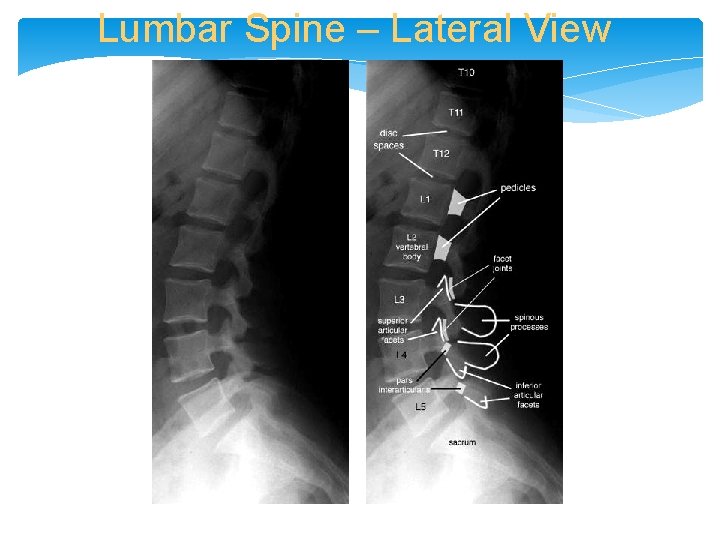
Lumbar Spine – Lateral View
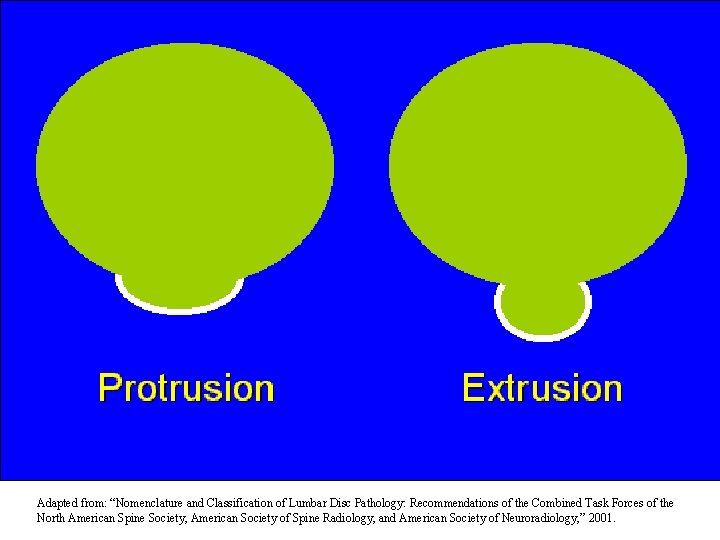
Adapted from: “Nomenclature and Classification of Lumbar Disc Pathology: Recommendations of the Combined Task Forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology, ” 2001.
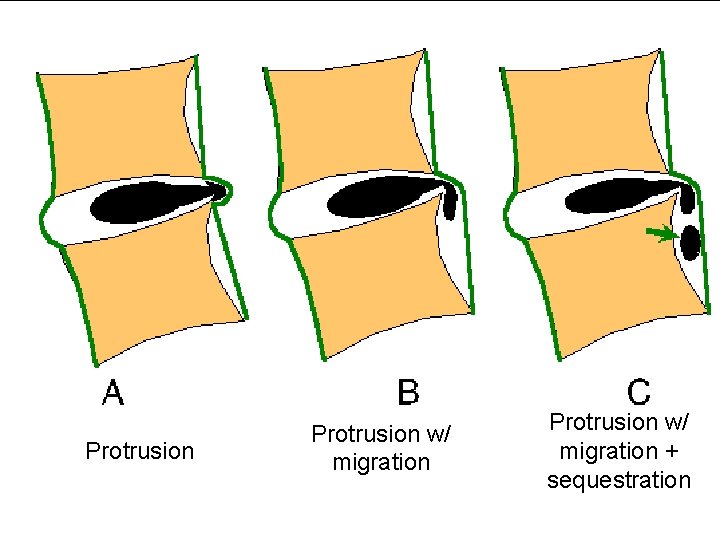
Protrusion w/ migration + sequestration
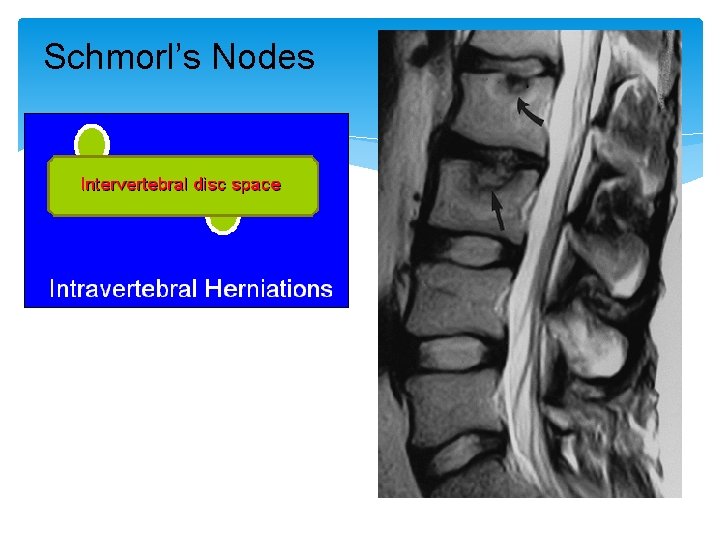
Schmorl’s Nodes

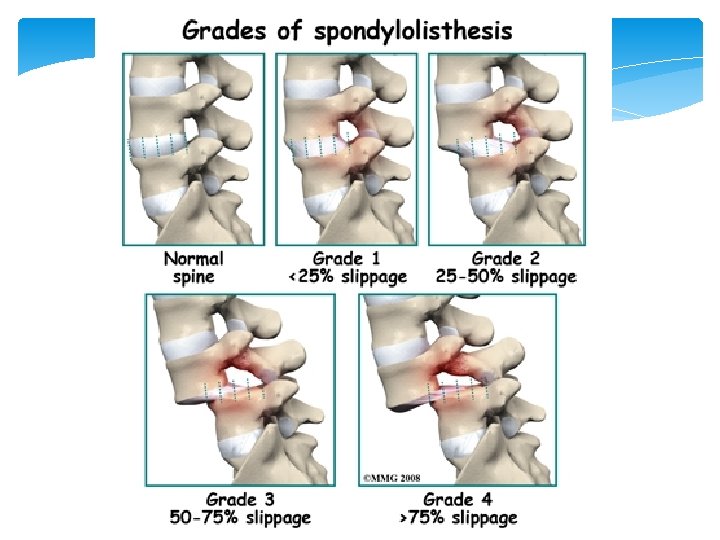
Confusing “Spondy-” Terminology • Spondylosis = “spondylosis deformans” = degenerative spine • Spondylitis = inflamed spine (e. g. ankylosing, pyogenic, etc. ) • Spondylolysis = chronic fracture of pars interarticularis with nonunion (“pars defect”) • Spondylolisthesis = anterior slippage of vertebra typically resulting from bilateral pars defects • Pseudospondylolisthesis = “degenerative spondylolisthesis” (spondylolisthesis resulting from degenerative disease rather than pars defects)
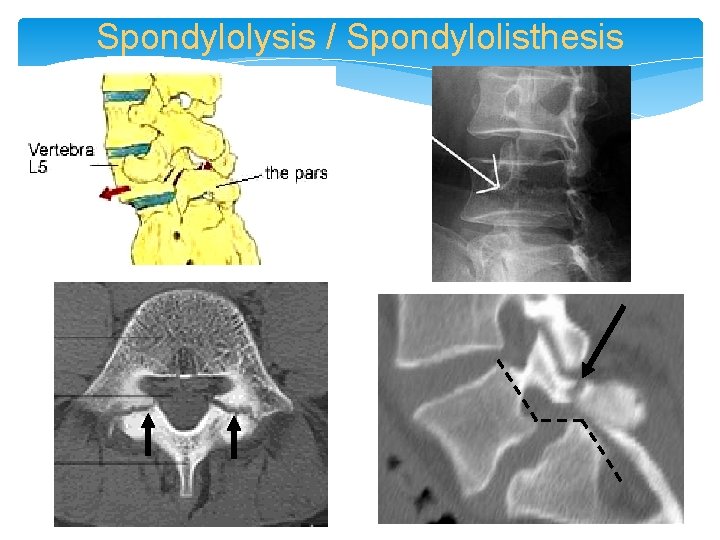
Spondylolysis / Spondylolisthesis
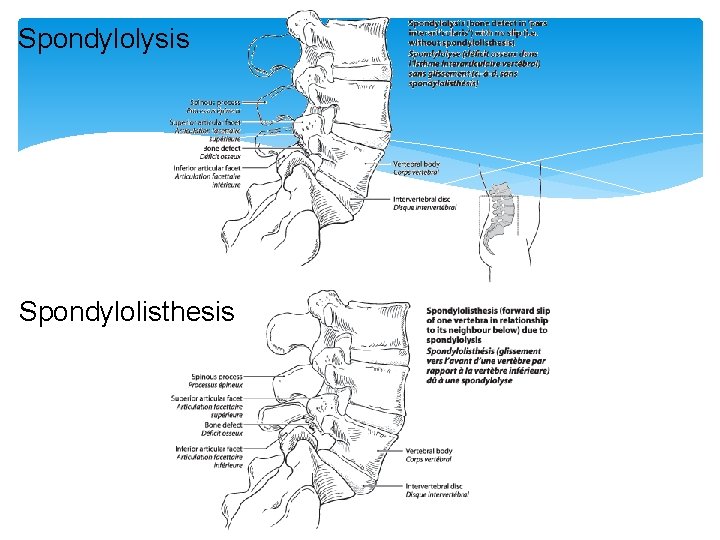
Spondylolysis Spondylolisthesis
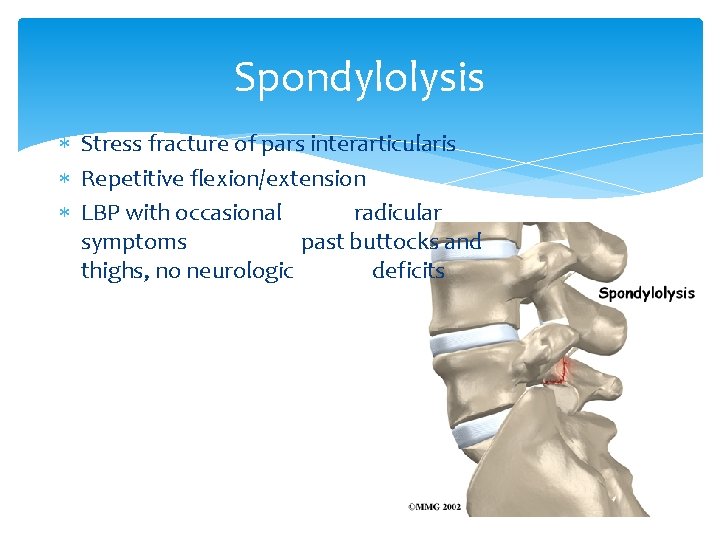
Spondylolysis Stress fracture of pars interarticularis Repetitive flexion/extension LBP with occasional radicular symptoms past buttocks and thighs, no neurologic deficits
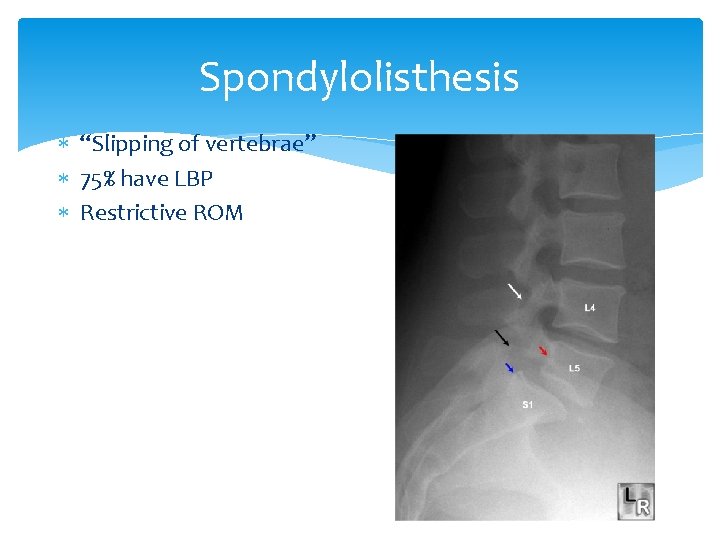
Spondylolisthesis “Slipping of vertebrae” 75% have LBP Restrictive ROM
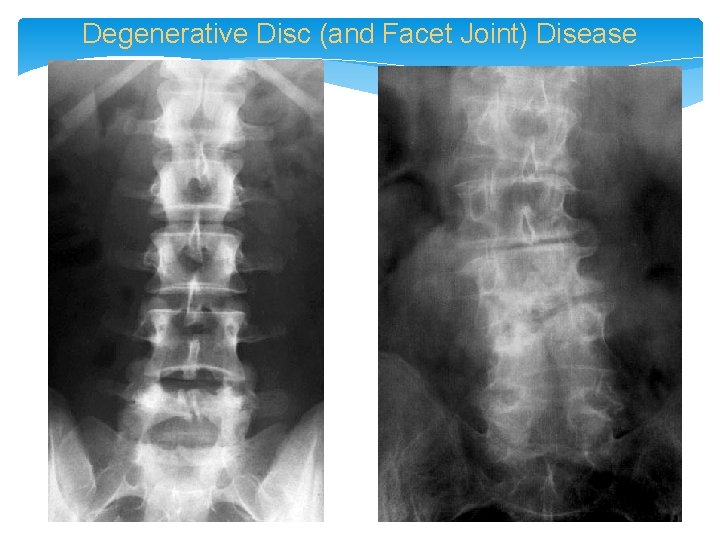
Degenerative Disc (and Facet Joint) Disease
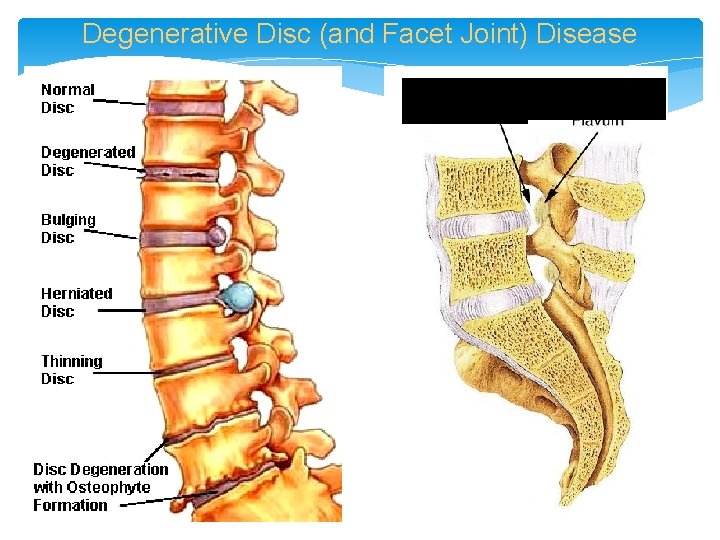
Degenerative Disc (and Facet Joint) Disease Foraminal stenosis Thickening/Buckling of Ligamentum Flavum

- Slides: 107