Obstructive Lung disease Lung Cancer Rob Nicholson Finals

Obstructive Lung disease + Lung Cancer Rob Nicholson

Finals simplified Every Condition: What is it? What causes it? What do patients present with? How do we investigate it? How do we treat it acutely? How do we treat it chronically?

COPD What is it? Chronic bronchitis: Cough for 3 months for 2 consecutive years. Emphysema: Enlarged air spaces distal to the terminal bronchiole

COPD
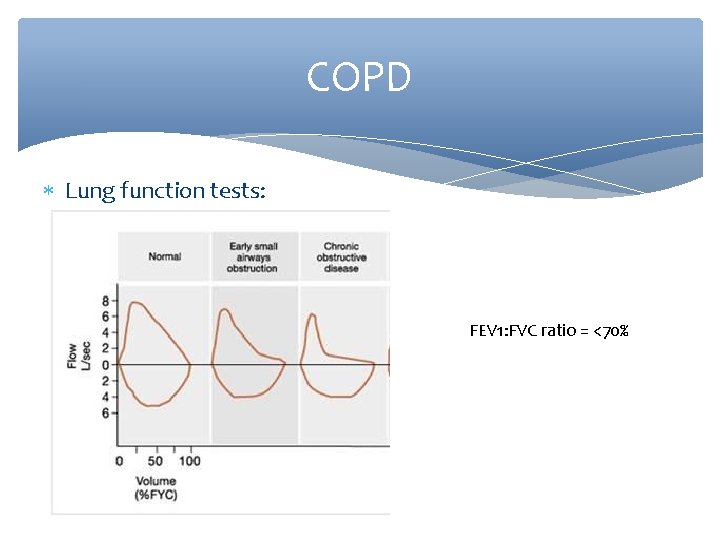
COPD Lung function tests: FEV 1: FVC ratio = <70%

COPD What causes it? Smoking Pollution Alpha 1 antitrypsin deficiency

COPD What to patients present with? History: Increased SOB Cough (productive white normally) Weight loss Depression Chest pain?

COPD

COPD How do we investigate it? History and examination Bloods Radiology Special tests

COPD Routine bloods: Increased Hb: Polycythemia Increased inflammatory markers in an exacerbation

COPD ABG: Type I respiratory failure • P 02 low • PCO 2 normal/low • p. H: normal Type II respiratory failure • PO 2 low • PCO 2 high • p. H: low
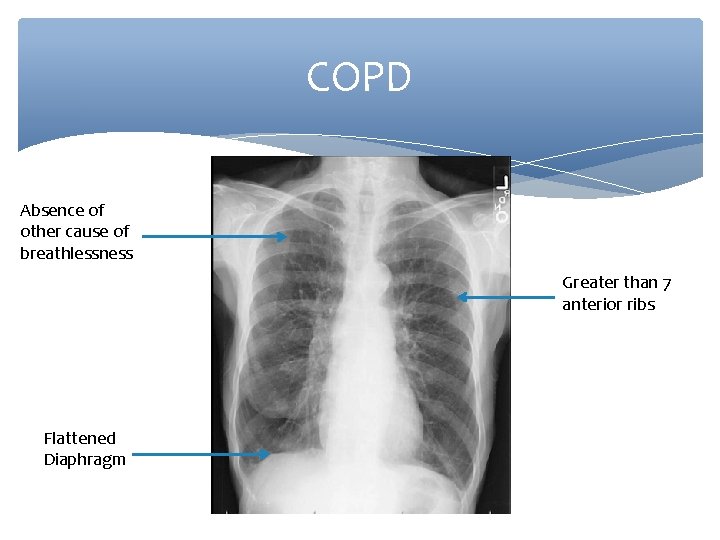
COPD Absence of other cause of breathlessness Greater than 7 anterior ribs Flattened Diaphragm
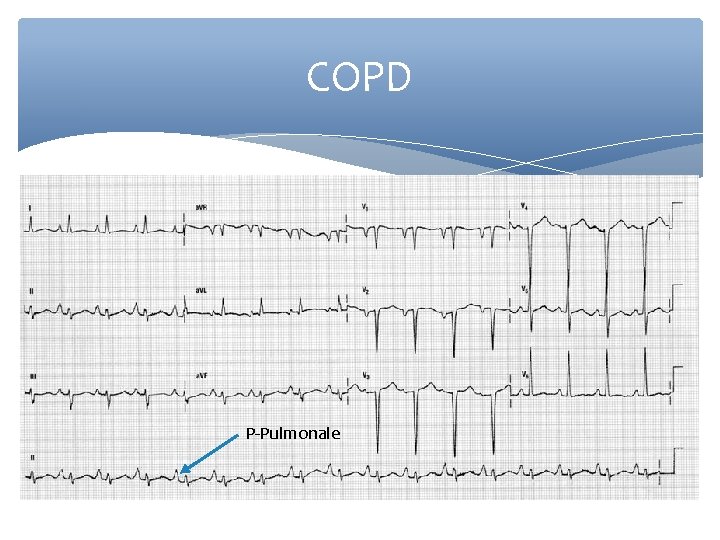
COPD P-Pulmonale

COPD Lung function tests: Decreased FEV 1 Dramatically decreased FEV 1/FVC ratio

COPD Treating an acute exacerbation of COPD: Steroids Nebulisers +/- antibiotics Oxygen? NIV?

COPD Chronic: Stop smoking!
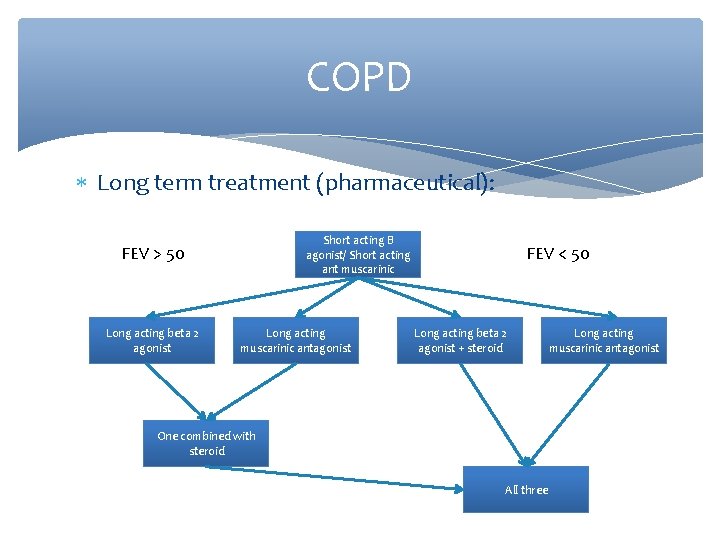
COPD Long term treatment (pharmaceutical): Short acting B agonist/ Short acting ant muscarinic FEV > 50 Long acting beta 2 agonist Long acting muscarinic antagonist FEV < 50 Long acting beta 2 agonist + steroid One combined with steroid All three Long acting muscarinic antagonist

COPD Long term oxygen therapy. Differs if have cardiac disease or not Essentially low O 2 on two separate occasions on ABG (<7. 3 if no cardiac Hx) Non-smokers Clinically stable
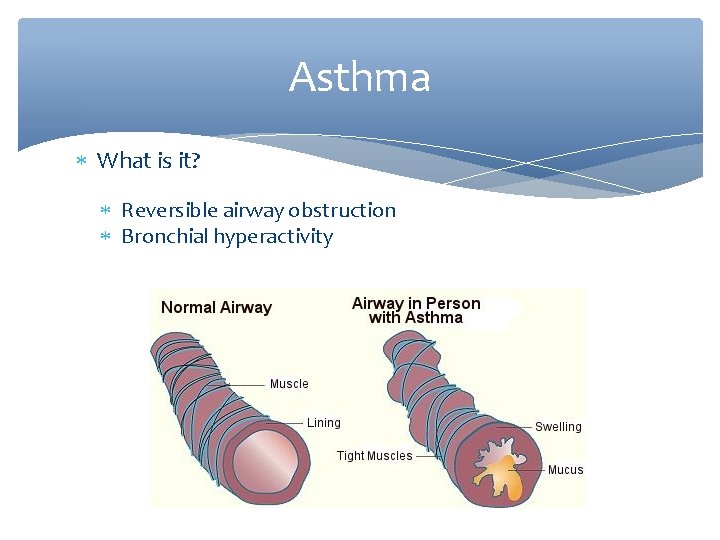
Asthma What is it? Reversible airway obstruction Bronchial hyperactivity

Asthma What do they present with? Increased cough (particularly bad at night) Diurnal variation of all symptoms Wheeze Dyspnea (Atopic symptoms) Triggers

Asthma Clinical examination: Use of accessory muscles Tachycardia and tachypnea Widespread polyphonic wheeze (Signs of steroid usage)
Asthma How do we investigate it? Bloods: Eosinophilia Raised Ig. E

Asthma Radiology: Chest X-ray: Chronically shows the same signs as COPD. Acutely very little
Asthma Special tests: Spirometry: Obstructive pattern that displays >15% reversibility. PEFR: diurnal variation / morning dipping Atopy: RAST testing and skin prick testing

Asthma Treatment: Bio, psycho social……. . Technique Avoidance Monitor Educate
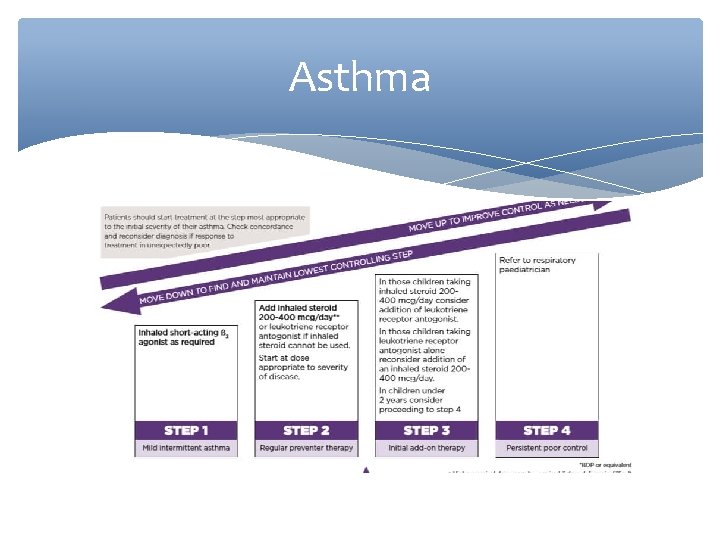
Asthma
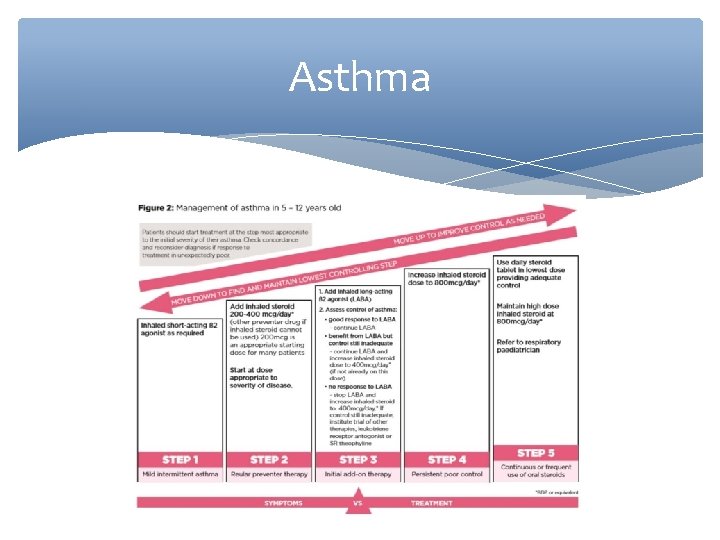
Asthma
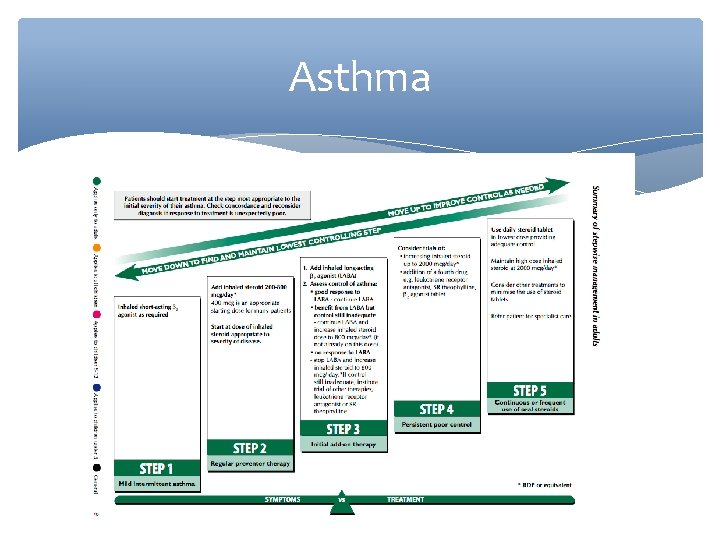
Asthma

Asthma Essentially: Under 5: Beta 2 agonist----steroid----LTA----REFER 5 -12’S: Beta 2 agonist----steroid----LOBA----increase steroid-----oral steroids --- REFER Adults: Same but try everything else before referral

Asthma Acute asthma: Severity Symptoms Mild asthma exacerbation Deterioration in normal resp function Moderate asthma exacerbation 50 -75% PEFR Severe asthma exacerbation 33 -50% PEFR, incomplete sentences, RR>25, HR >110 Life threatening asthma exacerbation O 2 < 92%, p. O 2 < 8, silent chest, decreased conscious level

Asthma Treatment: Nebs Steroids Theophylline Magnesium sulphate OXYGEN Leukotriene ITU

Lung Cancer What is it? Squamous cell carcinoma Adenocarcinoma Large cell carcinoma Small cell carcinoma

Lung Cancer What do they present with? Weight loss Cough +/- haemoptysis Chest pain Recurrent pneumonia’s Hoarse voice Beware Horners syndrome….
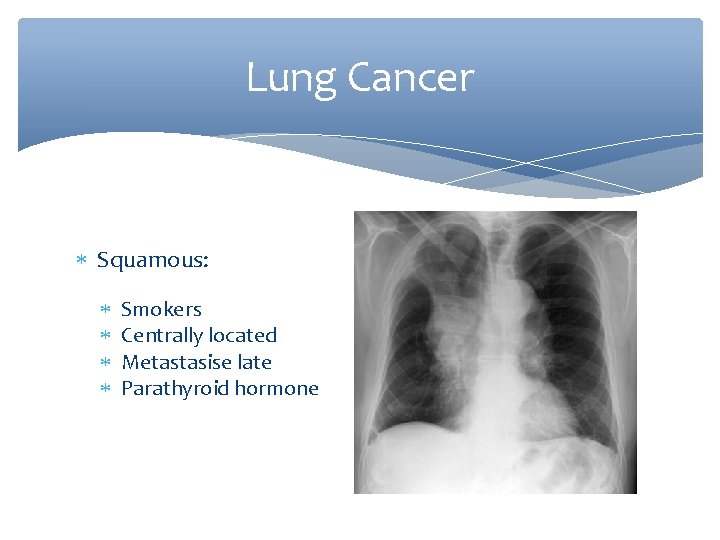
Lung Cancer Squamous: Smokers Centrally located Metastasise late Parathyroid hormone
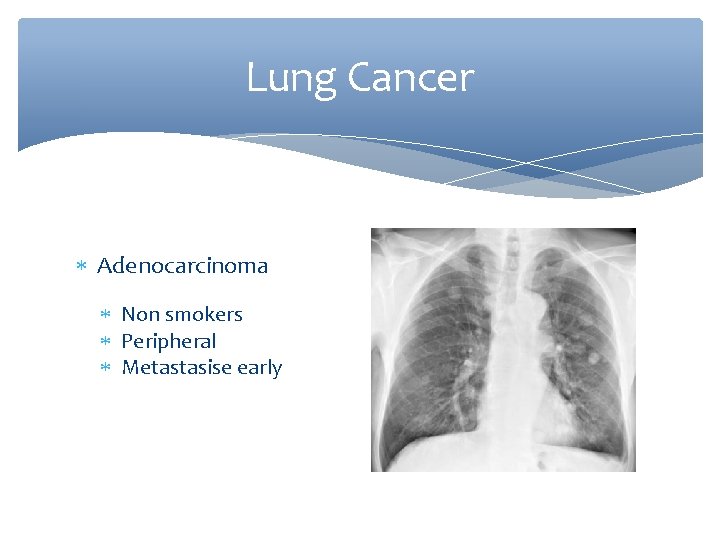
Lung Cancer Adenocarcinoma Non smokers Peripheral Metastasise early
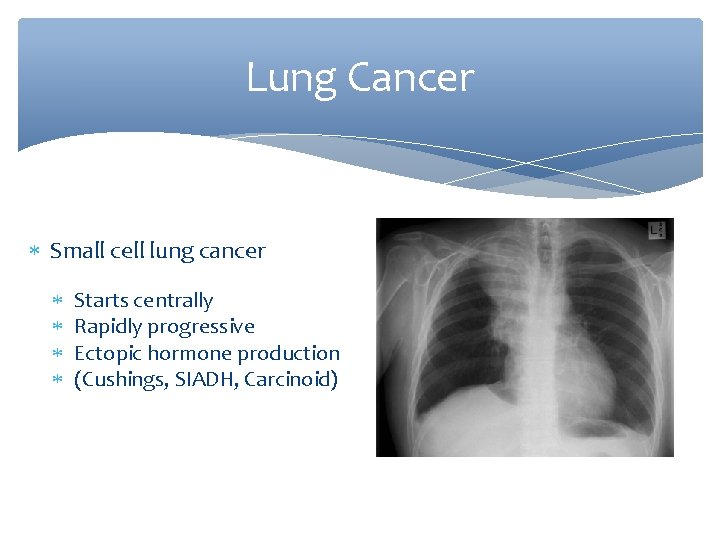
Lung Cancer Small cell lung cancer Starts centrally Rapidly progressive Ectopic hormone production (Cushings, SIADH, Carcinoid)

Lung cancer Investigations: Bloods: FBC, Ca 2+, LFT’s, Alk phos Radiology: CT, MRI, bronchoscopy Special tests: Biopsy, cytology

Lung Cancer Treatment: BIOPSYCHOSOCIAL MDT Chemo Radiotherapy Surgery Palliation
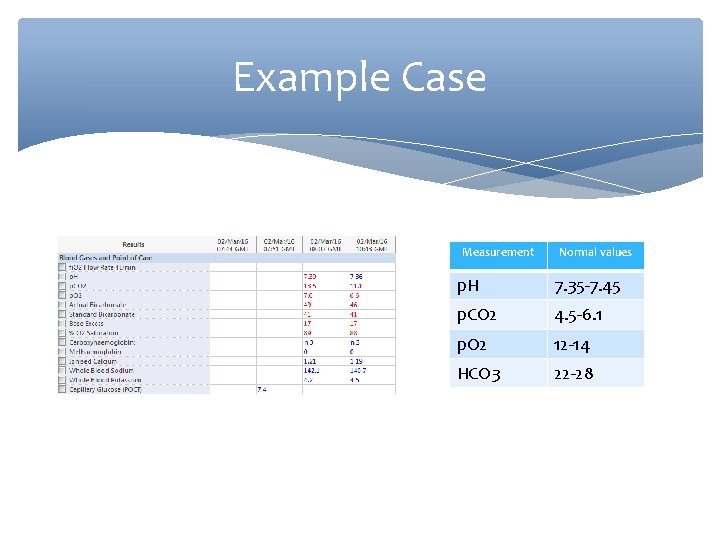
Example Case Measurement Normal values p. H 7. 35 -7. 45 p. CO 2 4. 5 -6. 1 p. O 2 12 -14 HCO 3 22 -28

Example case

Any questions?

Thanks to: Radiology masterclass British lung foundation Google images BLS guidelines NICE guidance SIGN guidelines
- Slides: 42