Obstetric Haemorrhage Aims To recognise Obstetric Haemorrhage To
Obstetric Haemorrhage

Aims ü To recognise Obstetric Haemorrhage ü To practise the skills needed to respond to a woman who is bleeding ü To achieve competence in those skills

Haemorrhage is common ü Most common cause of maternal death worldwide ü Accounts for ~30% of maternal deaths ü Deaths from haemorrhage could often be avoided. (In SA, over 80% haemorrhage deaths are avoidable)

SAVING MOTHERS REPORT FOR SOUTH AFRICA, 2005 – 2007 OBSTETRIC HAEMORRHAGE • Accounted for 491 maternal deaths in South Africa during 2005 – 2007. (12. 4% of total deaths and the third most common cause of maternal death) • Most common causes of haemorrhage deaths were: APH: Abruptio placentae PPH: uterine atony (prolonged labour) retained placenta ruptured uterus bleeding associated with caesarean section

Haemorrhage is often not recognized ü Blood loss is underestimated because in pregnancy signs of hypovolaemia do not show until the losses are large ü This is because mother compensates for blood loss by shutting off the blood supply to the fetoplacental unit ü Mother can lose up to 35% of circulating blood volume (2000 mls) before showing signs of hypovolaemia

Haemorrhage – signs ü Pale ü Confused ü Increased HR, reduced BP ü FH abnormalities ü Reduced urine output ü Obvious or hidden bleeding

ü WHEN SIGNS ARE THEY ARE SIGNIFICANT, HAVE HIGH SUSPICION AND ACT QUICKLY!

Haemorrhage - management ü Have an accessible protocol (poster form) ü ABCs ü C replace the volume and stop the bleeding

Haemorrhage ü ABCs ü Circulation üIV access by 2 large bore cannulae üSend off blood samples üGive iv fluids and blood if available üBe aware of potential coagulation disorders

NB: Establish the CAUSE of the Haemorrhage ü Pregnancy § Abortion, ectopic, abruptio, praevia ü Labour § Abruption, praevia, ruptured uterus ü After delivery (4 Ts) § uterine a. Tony, § Trauma (cervical or perineal, or ruptured uterus) § re. Tained placenta § re. Tained products ü Post Caesarean bleeding § Atony, trauma, placental site bleeding ü Any of the above +/- coagulation disorder

Haemorrhage – stop the bleeding • Good history and systematic examination to determine cause • CALL for help: Resuscitation and diagnosis of cause of bleeding plus treatment must occur concurrently. • How to stop bleeding for most causes will be covered in breakout sessions • Stepwise approach in case of uterine atony

Suspected Uterine Atony ü Empty bladder ü Give Oxytocics (oxytocin, ergometrine, prostaglandin) ü Massage uterus / bimanual compression ü Aortic compression ü Ongoing bleeding -- look for other cause ü Ongoing bleeding– Uterine balloon tamponade ü Ongoing bleeding - EUA - laparotomy
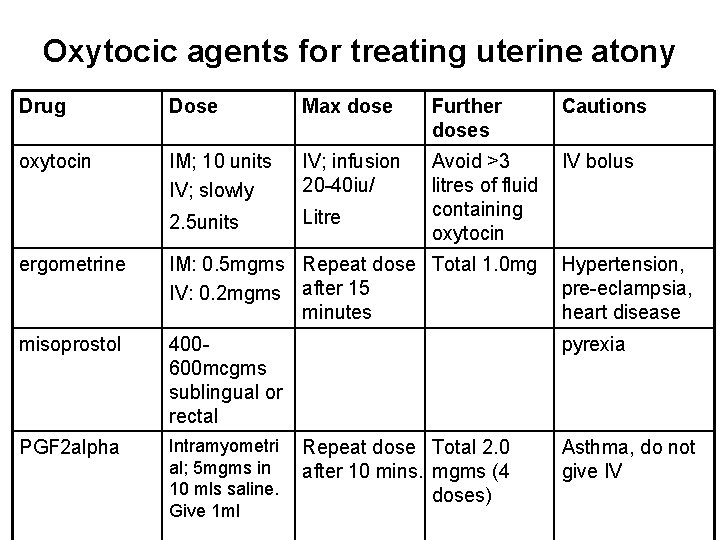
Oxytocic agents for treating uterine atony Drug Dose Max dose Further doses Cautions oxytocin IM; 10 units IV; slowly IV; infusion 20 -40 iu/ IV bolus 2. 5 units Litre Avoid >3 litres of fluid containing oxytocin ergometrine IM: 0. 5 mgms Repeat dose Total 1. 0 mg IV: 0. 2 mgms after 15 minutes Hypertension, pre-eclampsia, heart disease misoprostol 400600 mcgms sublingual or rectal pyrexia PGF 2 alpha Intramyometri al; 5 mgms in 10 mls saline. Give 1 ml Repeat dose Total 2. 0 after 10 mins. mgms (4 doses) Asthma, do not give IV

Treatment of PPH from other causes • Retained placenta…. Manual removal. (Efficacy of Intraumbilical cord oxytocin injection not proven) • Suspected retained placental products…. uterine evacuation under anaesthesia • Cervical and vaginal trauma…. . Repair with good light/ understanding of the anatomy. • Ruptured uterus …. Laparotomy • Unknown cause…Early recourse to Examination under Anaesthesia and possible laparotomy

Haemorrhage - Laparotomy ü Compression of the aorta ü Uterine compression suture (eg B-lynch) ü Uterine vessel ligation ü Hysterectomy

Prevention of PPH § Routine iron supplementation in pregnancy § Anticipate / Be prepared § Detect at risk women to deliver at referral hospital § Available supplies - IV fluids, cannulae, oxytocics, misoprostol, blood transfusion services § § § Prevent prolonged labour Active management of third stage of labour Routine postpartum and post caesarean section monitoring of vital signs and bleeding


RECAP üRecognising Obstetric Haemorrhage üCauses üManagement § Protocol § ABC § Blood replacement § Diagnosis of cause of bleeding üMethods to arrest haemorrhage
- Slides: 18