Objectives Categorize urinary tract infections by group Asymptomatic


Objectives Categorize urinary tract infections by group Asymptomatic bacteriuria Cystitis Pyelonephritis Complicated urinary tract infection/Catheter-associated UTI Recognize how to distinguish “Infection” from “Bacteriuria” and when to NOT given antibiotics for “UTI” Discuss the approach to cystitis Define pyelonephritis and identify evidence-based therapies Consider complicated pyelonephritis, catheter-associated UTI (CA-UTI) and treatment of highly-resistant organisms

IDSA guidelines Asymptomatic bacteriuria 1 Catheter-associated UTI 2 Cystitis and pyelonephritis 3

Asymptomatic bacteriuria 1 (ASB) Presence of bacteria in urine in the absence of symptoms Women: 2 consecutive voided urine specimens with SAME bacterial strain ≥ 105 cfu/m. L Men: Single clean-catch urine with 1 species ≥ 105 cfu/m. L Men and women: Single catheterized urine with 1 species ≥ 102 Pyuria without symptoms is NOT an indication for antimicrobial treatment
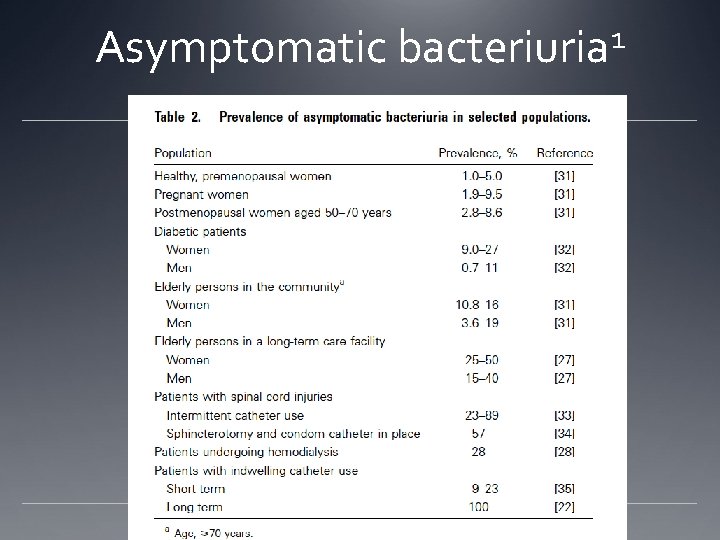
Asymptomatic 1 bacteriuria

Asymptomatic bacteriuria DO NOT TREAT ASYMPTOMATIC PATIENTS!! Not in non-pregnant women, diabetics, old people, institutionalized people, spinal cord injury, or in patients with catheters. Treating even in renal transplant patients is controversial. UNLESS!!!!! 1. Pregnant women should be screened in early pregnancy Treat 3 – 7 days if positive 2. Prior to TURP Start night before or immediately pre-procedure, stop postprocedure 3. Prior to urologic procedure where mucosal bleeding is anticipated

Why is asymptomatic bacteriuria over-treated? 20 – 80% of ASB is inappropriately treated Survey of 95 resident physicians who managed bacteriuria 10 32% of ASB inappropriately treated with antibiotics Presented with 7 vignettes 37% correct Reasons cited for improperly treating ASB in survey: Concern for post-op infection Elevated inflammatory markers Abnormal urinalysis
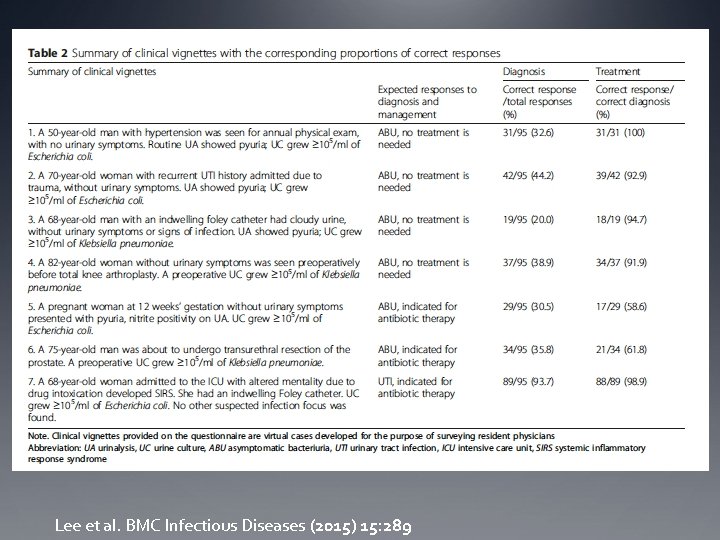
Lee et al. BMC Infectious Diseases (2015) 15: 289

Do not screen or treat ASB prior to surgical procedures No benefit prior to CT or spine surgery 11, 13 ASB not associated with post-operative joint replacement infections 12 Clin Infect Dis 2014; 59(1): 41– 7

Cystitis 3 Common in otherwise healthy women NO FEVER, NO FLANK PAIN Nitrofurantoin 100 mg bid x 5 d Cephalexin 500 mg bid x 3 -7 days 4 AVOID: Trimethoprim/sulfa: most sites >20% E. coli resistance Fluoroquinolones: unnecessarily broad, more C. diff, antipseudomonal/pneumococcal spectrum not needed Amoxicillin/clavulanate: poor empiric E. coli activity

Pyelonephritis 3 Fever, flank pain, and/or nausea and vomiting Get a urine culture first!! Option 1: Oral fluoroquinolone (if local E. coli sensitivity ≥ 90%) Higher cure rates than 14 days of trimethoprim/sulfa 5 Ciprofloxacin 500 mg po bid x 7 days 5, or Levofloxacin 750 mg po daily x 5 days 6 If baseline resistance >10%, can consider ceftriaxone 1 g x 1 then PO quinolone while sensitivities pending if follow-up can be assured Option 2: Beta-lactam 7 or TMP/SMX 5 as follows: Ceftriaxone 1 g IV or IM x 1, then cephalexin 8 1 g PO TID x 10 -14 days total, OR Ceftriaxone 1 g x 1 then TMP/SMX DS 1 po bid x 14 days

Bacteremia and pyelonephritis If bacteremic and not improving, repeat blood cx and consider imaging to rule-out complicated pyelonephritis Good data with quinolones and tmp/smx Caution with oral beta lactam regimen We give several days IV until clinically improved then finish with high dose oral beta lactam or swap to quinolone to finish

“Complicated” UTI Historical, messy term Cystitis or pyelonephritis accompanied by abnormality of the urinary tract 9 Obstruction: strictures, stones, prostatic hypertrophy, congenital Instrumentation: catheters, tubes, stents, procedures Poor voiding: reflux, neurogenic bladder, cystocele Transplant Infections are harder to eradicate in these patients If there is hydronephrosis suggesting obstruction, in the presence of infection this is a medical emergency; infected kidneys must be decompressed emergently! Indwelling catheters are most common cause of complicated UTI

Catheter-associated UTI (CA-UTI) IDSA guideline 20092 SYMPTOMS of UTI plus ≥ 103 cfu/m. L ≥ 1 organism from catheter specimen or midstream void <48 h after catheter removal Fever, rigors, AMS, malaise, or lethargy with NO other cause Flank pain, CVA tenderness, acute hematuria, pelvic pain IF NO SYMPTOMS IT IS CA-ASB!!!! Smelly or cloudy urine is NOT a symptom! Massive pyuria is NOT a symptom! Do NOT screen for ASB prior to or immediately after catheter placement

Culturing catheterized patients Catheters rapidly become colonized at a rate of 3 – 8% each day 14 Can’t get CA-UTI without a catheter! When in doubt get it out!!! If catheter in place 2 weeks or more, replace and send culture from NEW catheter before starting antibiotics We replace prior to cultures if >72 h catheter duration Do not treat yeast in the urine 15 Only 3% treated in large cohort, no complications 29% had catheter changed

Preventing CA-UTI and CA-ASB Minimize catheter use! Create guideline for post-op removal Nurse-driven protocol to remove when indication no longer met Keep system closed Minimize breaks, bag changes Do not flush junk into bladder! Do not flush at all… if plugged up, replace No dependent loops; use securing device Good perineal care daily

CA-UTI treatment 2 Tailor to culture results 7 days for prompt response 10 -14 days for delayed response 5 days levofloxacin is an option that decreases duration 6 3 days if cystitis, female <65, and catheter removed

ESBL E. coli and UTI 3% of isolates in Anchorage Limited drug options Gentamicin 3 mg/kg IV or IM q 24 h Ertapenem 1 g IV q 24 h Nitrofurantoin 100 mg po bid x 5 days (if no allergy, susceptible, and preserved renal function) Amoxicillin/clavulanate 500/125 mg BID x 5 -7 d 16 Use ONLY for cystitis and ONLY if MIC ≤ 8 Cure rate 93% for MIC 8 or less, 54% for MIC 16 or higher Possible role for amoxicillin/clavulanate PLUS oral 3 rd generation cephalosporin but NOT YET DEFINED 17

ESBL E. coli UTI and Fosfomycin Broad coverage of GNR and gram positives Long urinary excretion from single 3 g PO dose Highly active against ESBL E. coli (96%)18 Lower efficacy vs. Klebsiella ESBL (54%) Poorer microbiologic cure but similar clinical efficacy of ~90%3, 19 For cystitis in patients with highly resistant E. coli or with allergies precluding other agents, fosfomycin 3 g PO x 1 is a feasible option 19 that we use in Anchorage once or twice/month

References 1. Clinical Infectious Diseases 2005; 40: 643– 54 11. Interactive Cardio. Vascular and Thoracic Surgery 0 (2016) 1– 7 2. Clinical Infectious Diseases 2010; 50: 625– 663 12. Clin Infect Dis 2014; 59(1): 41– 7 3. Clinical Infectious Diseases 2011; 52(5): e 103– e 120 13. J Korean Neurosurg Soc 47 : 265 -270, 2010 4. JAMA. 1995 Jan 4; 273(1): 41 -5. 14. N Engl J Med 1974; 291: 215– 219 5. JAMA 2000; 283: 1583– 90. 15. American Journal of Infection Control 43 (2015) e 19 -e 22 6. Urology 2008; 71: 17– 22. 16. Arch Intern Med. 2008; 168(17): 1897 -1902 7. Emerg Med J 2002; 19: 19– 22. 17. Antimicrob Agents Chemother 60: 424 – 430. 8. Obstet Gynecol 1990; 76: 28– 32. 18. Antimicrob Agents Chemother 60: 1134 – 1136. 9. Can J Infect Dis Med Microbiol. 2005 16(6): 349 -360 19. Antimicrob Agents Chemother 59: 7355– 7361 10. Lee et al. BMC Infectious Diseases (2015) 15: 289
- Slides: 20