Nutrition Therapy for Metabolic Stress and Critical Illness

Nutrition Therapy for Metabolic Stress and Critical Illness Lauren Hoover & Clare Howard KNH 411 November 8, 2016

Patient Chris Mc. Kinley, Male, 37 y. o. -Summary: Patient has weighed over 250 pounds. since age 15 with steady weight gain, recently reaching a high of 424 pounds, then lost 24 pounds prior to his bariatric surgery. Four months ago, he received the Roux-en-Y gastric bypass. Total weight loss to date is approx. 100 pounds. However, now he is admitted to the MICU from the ER with probable sepsis. -Vital Signs (Admitting)-Temp. : 102. 5 BP: 135/90 Pulse: 98 Resp. Rate: 23 Height: 5’ 10” Weight: 325 lbs.

Patient History -Onset of disease: Experienced flu-like symptoms over previous 48 hours, became acutely SOB - brought to ER -Medical Hx: Type 2 DM, Htn, hyperlipidemia, osteoarthritis -Medications: Lovastatin 60 mg/day (Also has been off diabetes medications for 2 mo. ) -Tobacco Use: none -Alcohol Use: Socially, none since surgery -Family Hx: Father - Type 2 DM, CAD, Htn, COPD; Mother - Type 2 DM, CAD, osteoporosis
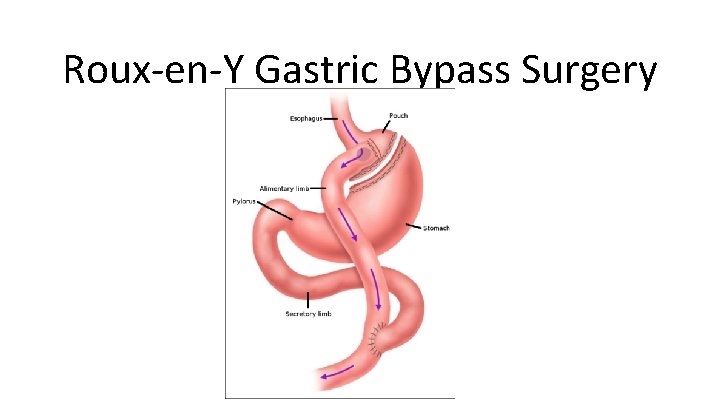
Roux-en-Y Gastric Bypass Surgery

Sepsis/SIRS • Etiology - Combination of pro-inflammatory cytokine release, coagulation factor imbalance, altered cell metabolism, hypoperfusion, and hypotension • Diagnosis - increased WBC count, HR, and respirations, and fever or hypothermia. Others include inflammatory variables • Pathophysiology - originating source of infection/trauma, initial inflammatory response resulting in vascular permeability, continues to an anti-inflammatory response with resulting organ dysfunction. – Increased gluconeogenesis = catabolism of muscle mass

Patient’s Laboratory Results Reference Range 2/23 Value Potassium (m. Eq/L) 3. 5 -5. 1 5. 8 Carbon dioxide (m. Eq/L) 23 -29 31 Glucose (mg/d. L) 70 -99 385 Phosphate (mg/d. L) 2. 2 -4. 6 2. 1 Bilirubin, total (mg/d. L) <1. 2 1. 3 Bilirubin, direct (mg/d. L) <0. 3 0. 7
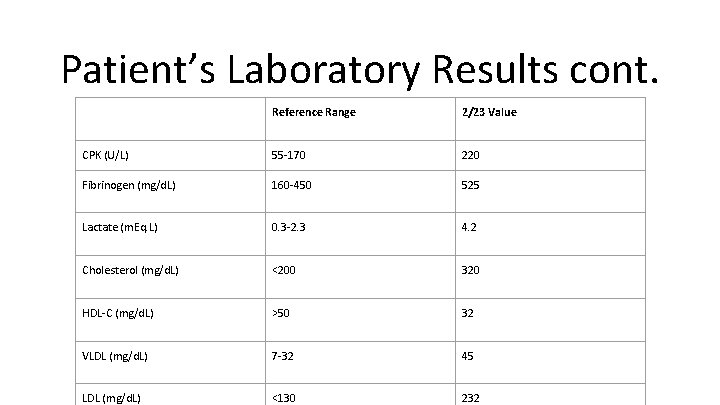
Patient’s Laboratory Results cont. Reference Range 2/23 Value CPK (U/L) 55 -170 220 Fibrinogen (mg/d. L) 160 -450 525 Lactate (m. Eq. L) 0. 3 -2. 3 4. 2 Cholesterol (mg/d. L) <200 320 HDL-C (mg/d. L) >50 32 VLDL (mg/d. L) 7 -32 45 LDL (mg/d. L) <130 232
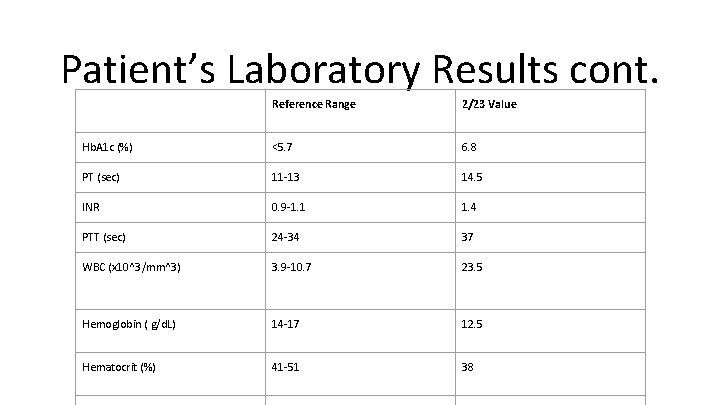
Patient’s Laboratory Results cont. Reference Range 2/23 Value Hb. A 1 c (%) <5. 7 6. 8 PT (sec) 11 -13 14. 5 INR 0. 9 -1. 1 1. 4 PTT (sec) 24 -34 37 WBC (x 10^3/mm^3) 3. 9 -10. 7 23. 5 Hemoglobin ( g/d. L) 14 -17 12. 5 Hematocrit (%) 41 -51 38

Patient’s Laboratory Results cont. Urinalysis results: -Protein, glucose ketones, and Bact present,

Treatment for Sepsis • Treat the infection first • Support patient with ventilation, antibiotics, hemodynamic, renal, and metabolic support • Insulin therapy, antimicrobial agents, coagulation-modulating drugs

Physician’s Assessment/Plan -Diagnosis of severe sepsis, pneumonia -Maintain current mechanical ventilation, continue vancomycin, Zosyn -Sedated with Versed and fentanyl -Initiate enteral feeding per nutrition consult

Nutrition Therapy - Assessment Height = 5’ 10” = 1. 78 m Current Wt. = 325 lbs. = 147. 73 kg Usual BW = 425 lbs. %Usual BW = 76. 5 % Ideal BW (using Hamwi method) = 166 lbs. = 75. 5 kg BMI = 46. 6 kg/m^2

Nutrition Therapy - Diagnosis • Inadequate protein-energy intake related to NPO current diet, as evidenced by lab results, specifically total protein, albumin, and prealbumin • Increased nutrient needs related to inability to consume regular diet as evidenced by intubation and sedated state.

Nutrition Therapy - Intervention Calculation of Energy, Protein and Fluid needs: Energy - 25 -30 kcal/kg IBW Protein - 1. 2 -1. 5 g/kg IBW Energy - 1890 -2270 kcals Protein - 91 -113 g Fluids - 1 m. L/kcal Fluids - 1890 -2270 m. L

Nutrition Therapy - Intervention Enteral Nutrition Plan: -Formula chosen - Isocal HN Plus (1. 20 kcal/m. L, 54 g protein/L) -For continuous feeding - 1800 m. L/24 hours = 75 m. L/hr. via pump -For bolus feeding - 1800 m. L/4 feedings = 450 m. L/feeding Initial start rate of 20 m. L/hour, increase by 15 m. L every 4 hours to achieve 75 m. L/hr, change to bolus feeding 6 times/day (300 m. L), then to 4 times/day (450 m. L).

Nutrition Therapy - Intervention Enteral Nutrition: 1800 m. L of Isocal HN Plus provides -1800 m. L fluid -2160 kcals -97 g protein *An additional 100 -200 m. L of fluid can be given.

Nutrition Therapy Monitoring/Evaluation -Initially (if unstable): I/O, electrolytes, BUN, creatinine, weight, hydration status, vital signs, bowel function, blood glucose daily, and TG, liver function tests weekly. -When Stable: I/O, electrolytes, BUN, creatinine, weight, hydration status, vital signs, bowel function, blood glucose 1 -3 times/week, and TG, liver function tests as needed. -Monitor any intolerance via symptoms, such as vomiting, nausea, diarrhea, abdominal pain, etc. Change feeding progression if needed .

References International Dietetic & Nutrition Terminology (IDNT): Reference Manual. Standardized Language for Nutrition Care Process. Academy of Nutrition and Dietetics, 2014. Retrieved from ncpt. webauthor. com Mahan, L. K. , Escott-Stump, S. , Raymond, J. L. Krause’s Food Nutrition & Diet Therapy, 13 th ed. Philadelphia, PA: W. B. Saunders Company, 2012 Nelms M. Medical Nutrition Therapy A Case Study Approach 5 th ed. , Cengage Learning, 2017. Nelms M. Sucher K, Lacey, K. Nutrition Therapy and Pathophysiology. 3 rd ed. Cengage Learning, 2016.

Questions?
- Slides: 19