Nutrition B 260 Fundamentals of Nursing Nursing Knowledge

Nutrition B 260: Fundamentals of Nursing

Nursing Knowledge Base • The five components of a nutrition assessment: – – – Screening for malnutrition for risk factors Anthropometry BMI Labs and tests Dietary history 2

Nursing Knowledge Base • Factors influencing nutrition – Environmental factors – Developmental needs • Infants through school age • Adolescents • Young and middle adults • Older adults 3

Nursing Knowledge Base • Alternative Food Patterns – Based on religion, cultural background, ethics, health beliefs, and preference – Vegetarian diet consists predominantly of plant foods 4

Assessment • Screening a patient is a quick method of identifying malnutrition or risk of malnutrition using sample tools: – Height – Weight change – Primary diagnosis – Comorbidities – Screening tools (3 used in practice) 5

Assessment • Assess patients for malnutrition – Conditions that interfere with their ability to ingest, digest, or absorb adequate nutrients. – Congenital anomalies and surgical revisions of the GI tract – Only IV therapy – Chronic diseases or increased metabolic requirements – Infants and older adults are at great risk 6

Assessment – An ideal body weight (IBW) provides an estimate of what a person should weigh. – Body mass index (BMI) measures weight corrected for height and serves as an alternative to traditional height-weight relationships. • Laboratory – Albumin: 3. 5 -5. 0 g/d. L (half life 21 days) – Transferrin and total iron-binding capacity (TIBC) – Hemoglobin (12 -18%) – Prealbumin (half life 1. 9 days) 7
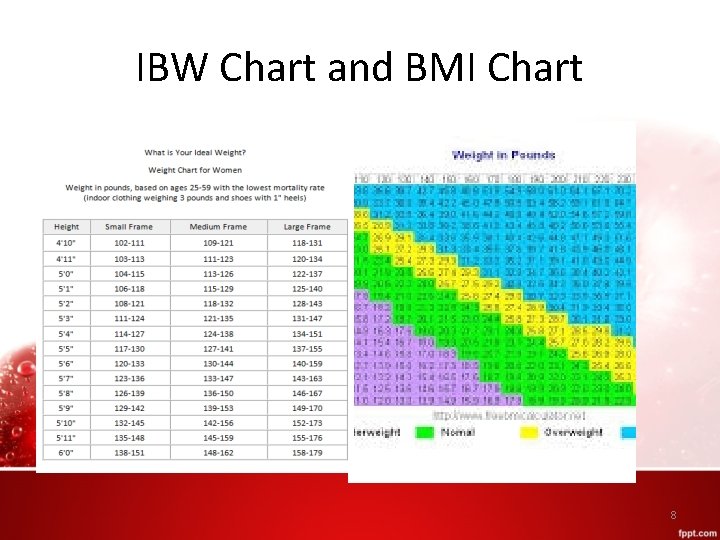
IBW Chart and BMI Chart 8

Assessment • Dietary and health history – Health status; age; cultural background; religious food patterns; socioeconomic status; personal food preferences; psychological factors; use of alcohol or illegal drugs; use of vitamin, mineral, or herbal supplements; prescription or over-the-counter (OTC) drugs; and the patient’s general nutrition knowledge • Physical examination • Dysphagia (difficulty swallowing) – 4 Screening tools 9
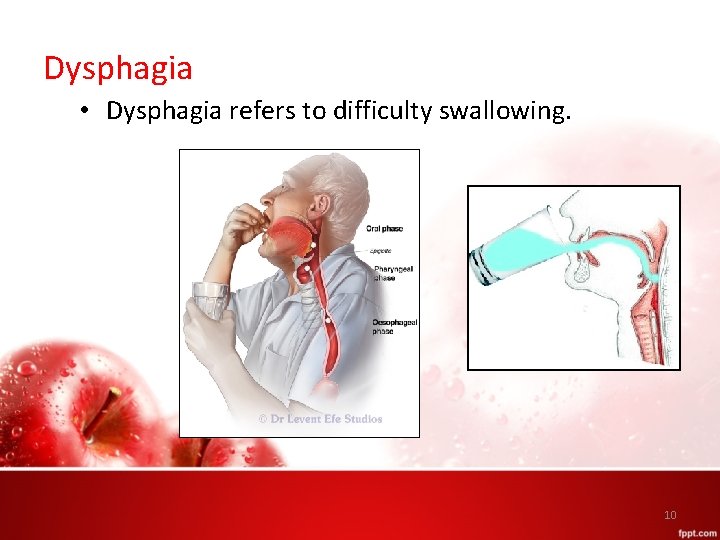
Dysphagia • Dysphagia refers to difficulty swallowing. 10

Nursing Diagnosis Risk for Aspiration r/t impaired swallowing Outcome: Patient will maintain patent airway and clear lung sounds. Nursing Interventions 1. Monitor for s/s of difficulty in swallowing 1. Cough during eating; change in voice tone or quality after swallowing; abnormal movements of the mouth, tongue, or lips; and slow, weak, imprecise, or uncoordinated speech. 2. Abnormal gag, delayed swallowing, incomplete oral clearance or pocketing, regurgitation, pharyngeal pooling, delayed or absent trigger or swallow, and inability to speak consistently 8

Nursing Diagnosis Risk for Aspiration r/t impaired swallowing 1. 2. 3. 4. 5. Monitor Respiratory rate, depth, and effort Auscultate lung sounds q 4 hrs Monitor bowel sounds q 4 hrs Take VS q 4 hrs, esp. temp Feed slowly with small bites and allow time for chewing and swallowing 6. Place food on strong side of mouth (do not use straw) 7. Have patient sit upright when eating and keep HOB 3045 degrees for an hour after eating 8. Encourage patient to use chin tuck when swallowing 9. Provide rest periods 10. Consult HCP for speech consult for swallow study 12

Enteral Tube Feedings • Enteral nutrition (EN) provides nutrients into the GI tract. • Feedings are provided for patients who can not swallow and have a functioning GI tract. • Feedings can be delivered through a nasogastric (NGT), jejunal (JT) or gastric tube (GT). 13

Nursing Diagnosis Risk for Aspiration r/t NGT feeding Outcome: Patient will maintain patent airway and clear lung sounds. Nursing Interventions 1. Determine if patient is at high risk for aspiration: coughing, hx of GERD, nasotracheal suction, an artificial airway, decreased LOC, and lying flat. 2. Keep HOB up to 30 -45 degrees at all times 3. Measure gastric residual volumes every 4 -6 hrs. – 250 ml or more on 2 consecutive assessments: delayed gastric emptying or if 500 ml on assessment – Discuss follow up with HCP 14

Nursing Diagnosis Risk for Aspiration r/t NGT feeding 4. Stop feedings if aspiration occurs 5. Administer metoclopramide (Reglan) if ordered 6. Monitor for nausea, vomiting, cramping and diarrhea and tube occlusion. 7. Increase rate per order 15

Acute Care Considerations • The nutritional care of acutely ill patients requires monitoring. – Patients are interrupted at meal time – NPO status – Poor appetites – Fatigued or feel uncomfortable – Patient who are NPO and receive only IV fluids for more than 4 -7 days are at nutritional risk. – Parental or Enteral feeding 16

• Clear liquids: broth, coffee, tea, clear soda & juice, jello, popsicle • Full: above + smooth dairy • Pureed: above + scrambled eggs, pureed meat – vegetables –fruits, mashed potatoes • Mechanical soft: above + diced meats, flaked fish, cottage cheese, rice, potatoes, etc. • Soft/low residue: low fiber foods, pasta, tender meat, canned fruits/vegetables This is the same order that we advance diets 17 Box 44 -10 pg 1017 Diets Orders

Nutrition: Types of Diets • High fiber: fresh fruit, steamed vegetables, bran, oatmeal, dried fruit • Low sodium: 4 g, 2 g, 1 g • Low cholesterol: 300 mg/day • Diabetic: usually 1800 cal/day • Regular: no restrictions

Nursing Diagnosis Imbalanced Nutrition: less than body requirements r/t poor appetite Outcome: Patient will eat 50% of breakfast, lunch and dinner. Nursing Interventions 1. Monitor food intake; recorded percentages of served food that is eaten 2. Monitor patient ability to eat (time involved, motor skills, visual acuity, and ability to swallow) 3. Offer small frequent meals 4. Assist with ordering meals, encouraging familiar foods 5. Avoid interruptions during mealtimes 19

Nursing Diagnosis Imbalanced Nutrition: less than body requirements r/t poor appetite 6. Provide a calm, peaceful, pain free, odor free environment 7. Provide social interaction by encouraging family to visit during meal times. 8. Encourage or provide oral care prior to meal time 9. Provide rest periods before meals 10. Consult with HCP for a Dietary consult 11. Teach the importance of having good nutrition during the time of an illness. 20
- Slides: 20