Nutrition and hydration in woundcare Date 25 June


























- Slides: 30

Nutrition and hydration in woundcare Date : 25 June 2018 Presented by: Susan Clarke, Dietitian, WSCCG and IESCCG 1

Nutrition & hydration in wound care • Nutrition & hydration play a vital role in the prevention & treatment of wounds and ulcers • A healthy balanced diet and maintaining a suitable weight encourages wound healing • Nutritional status has a direct influence on the health and repair of body tissue • Each stage of healing process requires a range of nutrients 2

Phases of wound healing & key nutrients involved 3 Haemostasis Energy, protein, vitamin K Inflammation Energy, protein, vitamins A, C, E, selenium, antioxidants Proliferation or granulation Energy, protein, copper, iron, vitamin A, vitamin B 6, zinc, vitamin C Remodelling or maturation Energy, protein, zinc, vitamin C, iron

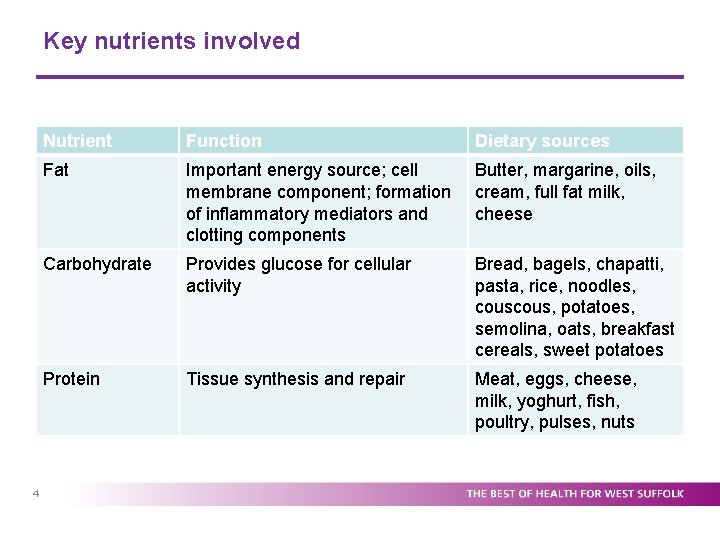
Key nutrients involved 4 Nutrient Function Dietary sources Fat Important energy source; cell membrane component; formation of inflammatory mediators and clotting components Butter, margarine, oils, cream, full fat milk, cheese Carbohydrate Provides glucose for cellular activity Bread, bagels, chapatti, pasta, rice, noodles, cous, potatoes, semolina, oats, breakfast cereals, sweet potatoes Protein Tissue synthesis and repair Meat, eggs, cheese, milk, yoghurt, fish, poultry, pulses, nuts

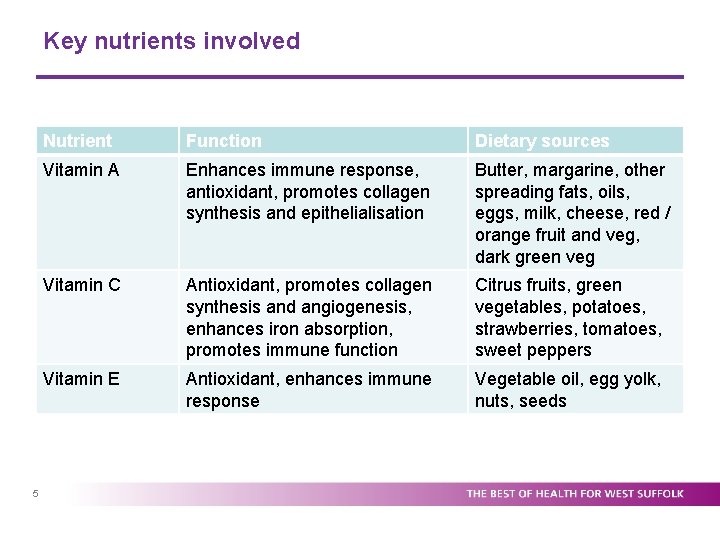
Key nutrients involved 5 Nutrient Function Dietary sources Vitamin A Enhances immune response, antioxidant, promotes collagen synthesis and epithelialisation Butter, margarine, other spreading fats, oils, eggs, milk, cheese, red / orange fruit and veg, dark green veg Vitamin C Antioxidant, promotes collagen synthesis and angiogenesis, enhances iron absorption, promotes immune function Citrus fruits, green vegetables, potatoes, strawberries, tomatoes, sweet peppers Vitamin E Antioxidant, enhances immune response Vegetable oil, egg yolk, nuts, seeds

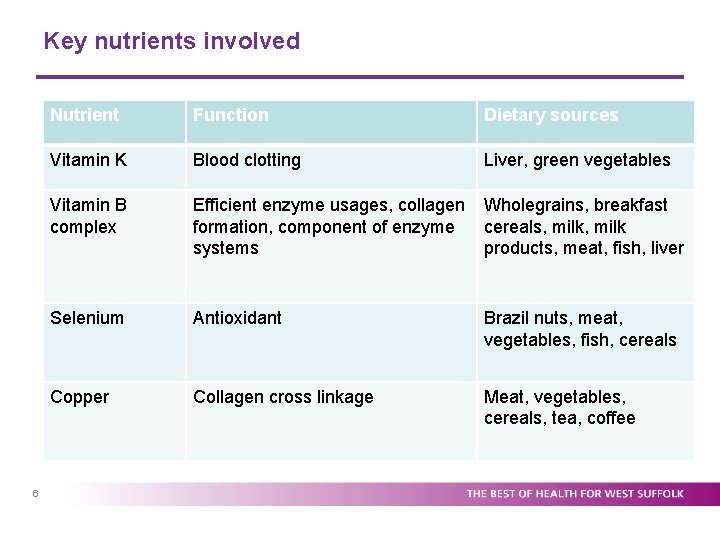
Key nutrients involved 6 Nutrient Function Dietary sources Vitamin K Blood clotting Liver, green vegetables Vitamin B complex Efficient enzyme usages, collagen formation, component of enzyme systems Wholegrains, breakfast cereals, milk products, meat, fish, liver Selenium Antioxidant Brazil nuts, meat, vegetables, fish, cereals Copper Collagen cross linkage Meat, vegetables, cereals, tea, coffee

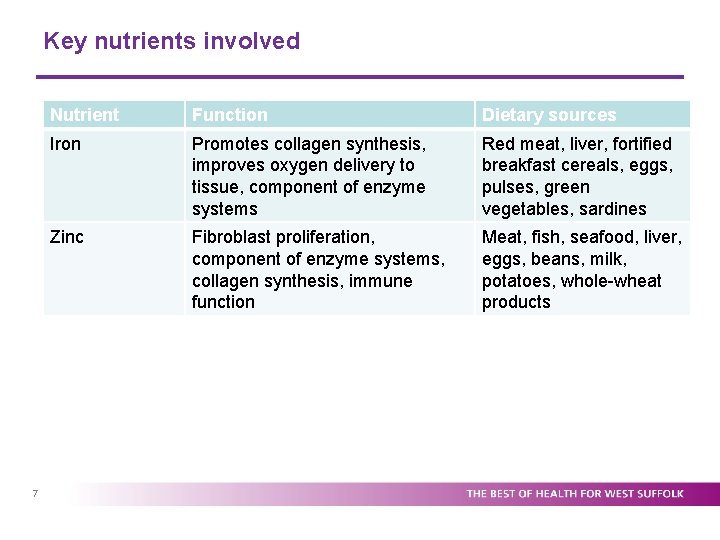
Key nutrients involved 7 Nutrient Function Dietary sources Iron Promotes collagen synthesis, improves oxygen delivery to tissue, component of enzyme systems Red meat, liver, fortified breakfast cereals, eggs, pulses, green vegetables, sardines Zinc Fibroblast proliferation, component of enzyme systems, collagen synthesis, immune function Meat, fish, seafood, liver, eggs, beans, milk, potatoes, whole-wheat products

Nutrition in chronic and complex wounds • Complicated by malnutrition, dehydration, infection • Malnutrition: state of nutrition in which a deficiency or excess (or imbalance) of energy, protein and other nutrients causes measurable adverse effects both on tissue / body structure and function and clinical outcome. 8

Nutrition in chronic and complex wounds • Malnutrition is a reversible risk factor for wounds • Early identification & treatment of malnutrition is vital • Nutritional screening: Malnutrition Universal Screening Tool • Protein energy malnutrition: muscle wasting, oedema, altered plasma proteins, fatigue, weakness 9

Malnutrition • Treatment - high protein / energy diet - fortified diet - nutritional supplements - vitamin / mineral supplements - enteral tube feeding 10

Dehydration • Dehydrated skin is less elastic, fragile, more susceptible to breakdown • Dehydration can reduce tissue perfusion at wound site • Fluid loss as result of wound exudate • Fluid requirements: c. 1500 ml daily (8 -10 cups or glasses) • Fluid requirements: 30 -35 ml/kg daily 11

Weight management: obese / overweight • Obese / overweight can be undernourished in essential nutrients • Weight reduction not primary / appropriate aim for acute wounds • Aim: meet nutritional requirements and preserve muscle mass; 5 -10% weight loss over 3 -6 months in most chronic cases 12

Weight management: underweight • Aim: maintain / ideally increase body mass and correct nutritional difficulties • High protein / energy diet 13

Summary • Healthy eating and regular physical activity help prevent chronic illnesses that can lead to wounds and ulcers • Adequate nutrition plays a key role in woundhealing process • Healing delayed by imbalance / lack of nutrients • Identify malnutrition early • Hydration status equally important • Improved nutrition can improve Qo. L 14

References • Johnson, E (2007)The role of nutrition in tissue viability, Wound Essentials, vol. 2, 10 -21 • Guidance on optimising nutrition for chronic wound healing, Southern Health NHS Foundation Trust • Hurd, T, Nutrition and Wound-care Management / Prevention, Wound Care Canada, Vol. 2, No. 2 15

Nutritional management of stomas Date : 25 June 2018 Presented by: Susan Clarke, Dietitian, WSCCG and IESCCG 16

Goals of dietary management • • • 17 Risk of malnutrition preoperatively Ongoing screening of nutritional status Promote healing of stoma wound Aim to keep stools normal post-surgery Prevent stoma blockages after surgery Minimise unpleasant GI upset

Stoma healthy eating guidelines • • • 18 Low fibre/residue diet initially Chew food thoroughly Add one new food at a time Eat at regular intervals Consume a wide variety of food May require a multivitamin

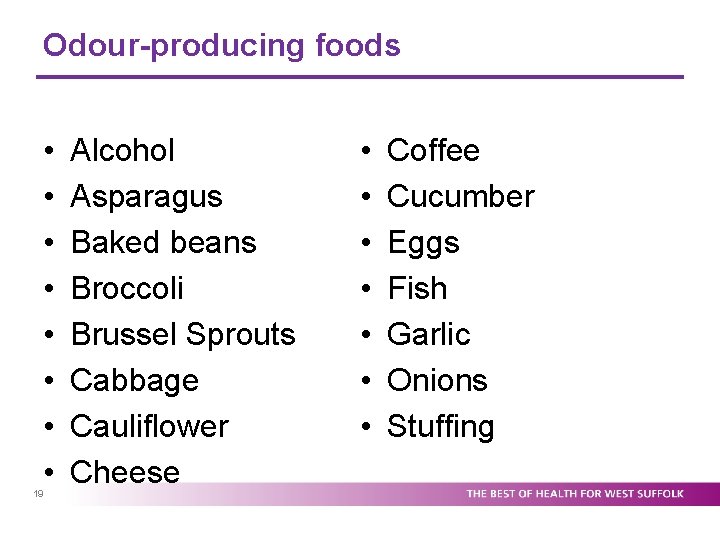
Odour-producing foods • • 19 Alcohol Asparagus Baked beans Broccoli Brussel Sprouts Cabbage Cauliflower Cheese • • Coffee Cucumber Eggs Fish Garlic Onions Stuffing

Odour-reducing foods and drinks • • • Apples Buttermilk Charcoal tablets Cranberry juice Green leafy vegetables • Live yoghurt 20 • Orange juice • Parsley • Tomato juice

Foods that may cause wind • • • 21 Asparagus Baked beans Beer Broccoli Brussel Sprouts Cabbage Cauliflower Chewing gum Cucumber • • Dried peas and beans Fish Fizzy drinks Melons Milk products Onions Spicy foods Sweetcorn

Foods that may relieve wind • • 22 Angelica Charcoal tablets Cinnamon Fennel – eat or as tea Peppermint oil / tea Sage Tomato juice Yoghurt

May cause obstruction • • 23 Chinese vegetables • • Coconut • Dried fruit • Fruit / Veg skins • Fruit with seeds • Mushrooms Nuts and seeds • Onions Peas Peppers Pineapple Popcorn Potato skins Sweetcorn Tomatoes

To relieve constipation • Increase hydration • Higher fibre foods: - cooked fruits / veg - raw fruits / veg - bran cereals - whole wheat bread - whole grain cereals - fruit juice • Liquorice 24

Causes of diarrhoea • Baked beans • Beer • Broccoli • Brown / wholemeal rice, pasta, bread • • Chocolate • Cheese / yoghurts with • added fruit • • Coffee • • 25 Dried fruit / nuts Fruit juice Hard fruits Unpeeled fruit, pips, stalks, seeds & pith Highly spiced foods Large meals Soup

To thicken flow • • • 26 • Cooked apple • Arrowroot • Boiled milk Bananas (under-ripe) • • Buttermilk • Plain dairy foods Jelly babies Lean meats, fish, eggs • Marshmallows Plain noodles (Smooth) peanut butter Potato Pretzels Semolina White bread, rice, pasta Tinned fruit

High output stomas • Salt - ½ - 1 tsp daily • Cook meals with salt • Salty foods, e. g. cheese, bacon, ham, sausages, smoked fish, shellfish, fish in brine, meat / fish paste, yeast extracts, salted crisps, savoury / salty biscuits 27

High output stomas • Meal pattern - regular meals - smaller, more frequent meals - take time and chew foods well - avoid heavy meals / snacks before bedtime - avoid alcohol / caffeinated drinks before bedtime - avoid eating and drinking at same time 28

High output stomas • Fluids - restrict amount you drink - take oral rehydration solution (St Mark’s) - increase salt intake - avoid drinking around mealtimes • St Mark’s Solution: - 6 level 5 ml tsp glucose - 1 level 5 ml tsp salt - ½ heaped 5 ml tsp sodium bicarbonate - 1 litre of water 29

References • https: //patient. info/health/inflammatory-boweldisease/stoma-dietary-care • Dietary advice for Ostomates, Coloplast • Eating and drinking when you have a high stoma output leaflet, St Mark’s Hospital 30