NURSING MANAGEMENT OF COPD Physiology Respiratory Upper Goal













- Slides: 22

NURSING MANAGEMENT OF COPD

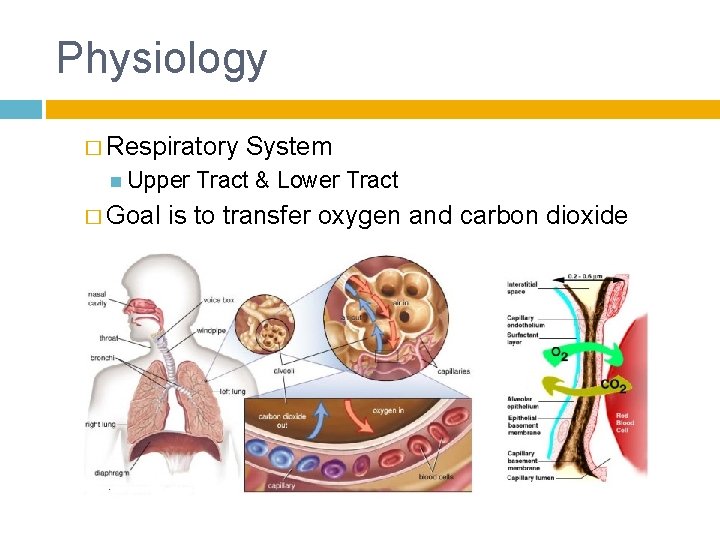
Physiology � Respiratory Upper � Goal System Tract & Lower Tract is to transfer oxygen and carbon dioxide

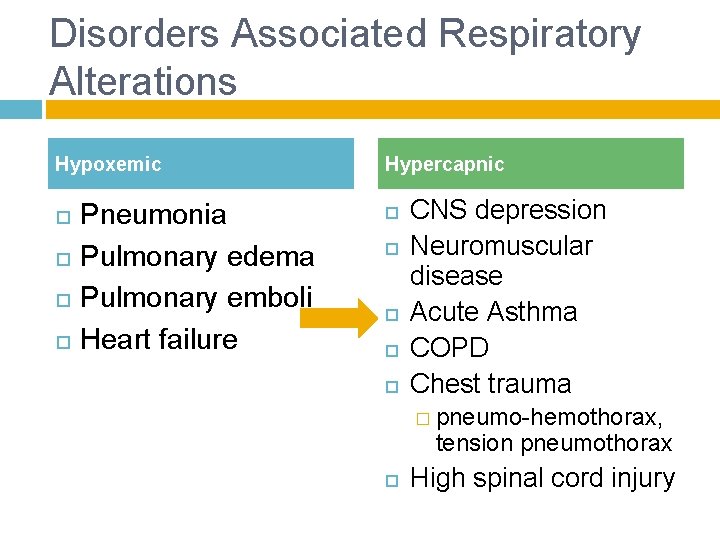
Disorders Associated Respiratory Alterations Hypoxemic Pneumonia Pulmonary edema Pulmonary emboli Heart failure Hypercapnic CNS depression Neuromuscular disease Acute Asthma COPD Chest trauma � pneumo-hemothorax, tension pneumothorax High spinal cord injury

Etiology Cigarette smoking is the main precipitating factor 3 rd leading cause of death Upwards of 5. 4 million people died in 2005 and it is estimated to grow to 8. 3 million deaths/year in 2030 (World Health Organization) Greater risk population: � Women, whites, age 65 -74, lower economic status, current or former smokers, history of http: //www. nhlbi. nih. gov/health-topics/copd/causes asthma http: //www. cdc. gov/copd/index. html

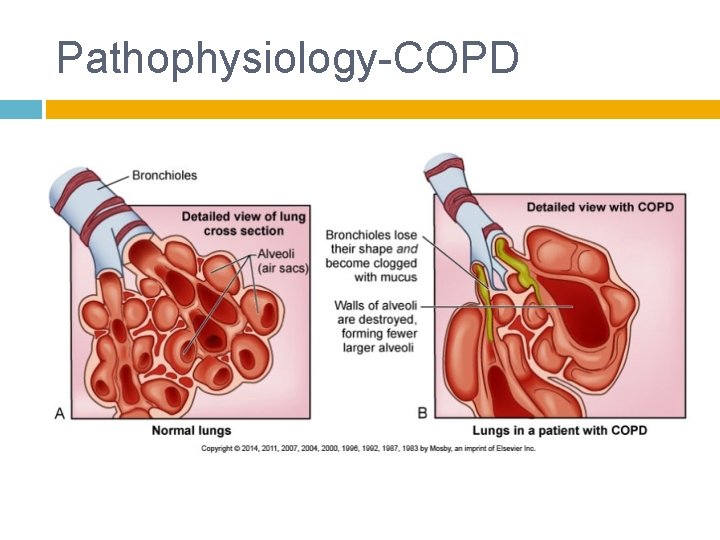
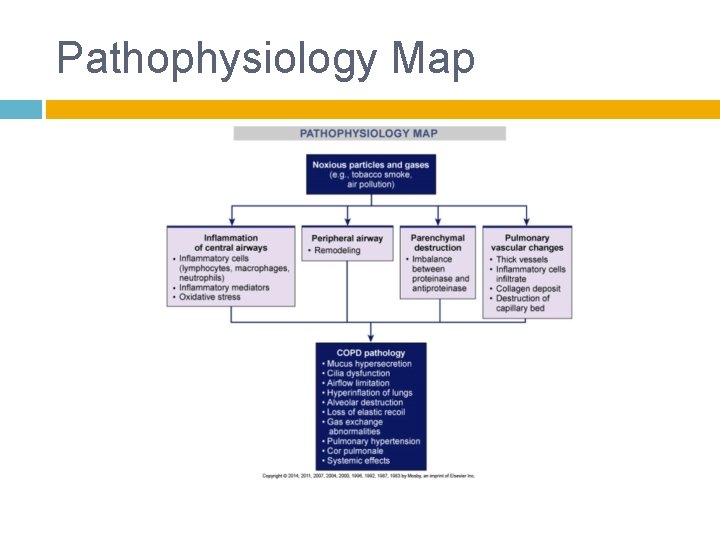
Pathophysiology Progressive destruction of alveoli related to chronic inflammation � Alveoli collapse The cause related to air trapping in respiratory bronchioles, alveoli, and alveolar ducts The gas exchange (oxygen carbon dioxide) that normally occurs has been impaired due to the alveoli destruction over time

Pathophysiology-COPD

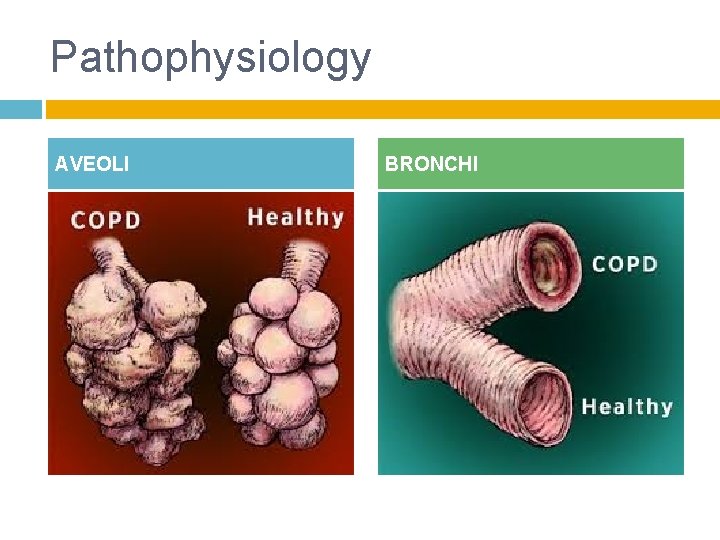
Pathophysiology AVEOLI BRONCHI

Pathophysiology Map

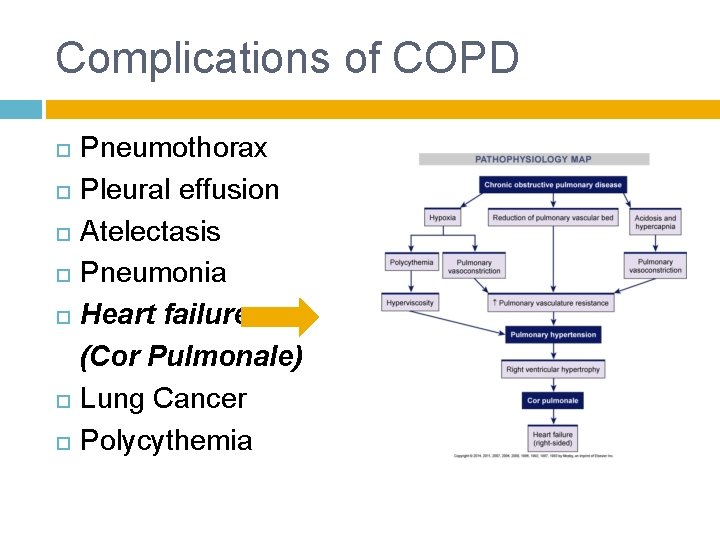
Complications of COPD Pneumothorax Pleural effusion Atelectasis Pneumonia Heart failure (Cor Pulmonale) Lung Cancer Polycythemia

Arterial Blood Gas interpretation p. H Acidosis p. H Pa. CO 2 HCO 3 7. 35 - 7. 45 Alkalosis 45 – 35 22 – 26 p. H = 7. 35 -7. 45 (normal range) Pa. CO 2 = 45 -35 (normal range)-respiratory HCO 3 = 22 -26 (normal range)-metabolic p. O 2 = 80 -100 Oxygen Saturation = 95 – 100 %

ABG Interpretation ACIDOTIC (Respiratory) 7. 32 p. H 48 Pa. CO 2 NORMAL 21 HCO 3 uncompensated 35 Pa. HCO 3 fully compensated p. H: 7. 32 (7. 35 -7. 45) Pa. CO 2: 48 (45 -35) Pa. HCO 3: 30 (22 -26) ALKALOTIC (Metabolic) 30 Pa. HCO 3 1. What is the p. H? acidosis, normal, or alkalosis Acidosis 2. What is the Pa. CO 2? acidosis, normal or alkalosis 3. What is the Pa. HCO 3? acidosis, normal or alkalosis 4. Is this patient in a compensated or uncompensated Compensated state? Don’t forget to look at the Pa. O 2 (80 -100)!!! Anything less than 60 is acute respiratory Partially Compensated Respiratory Acidosis

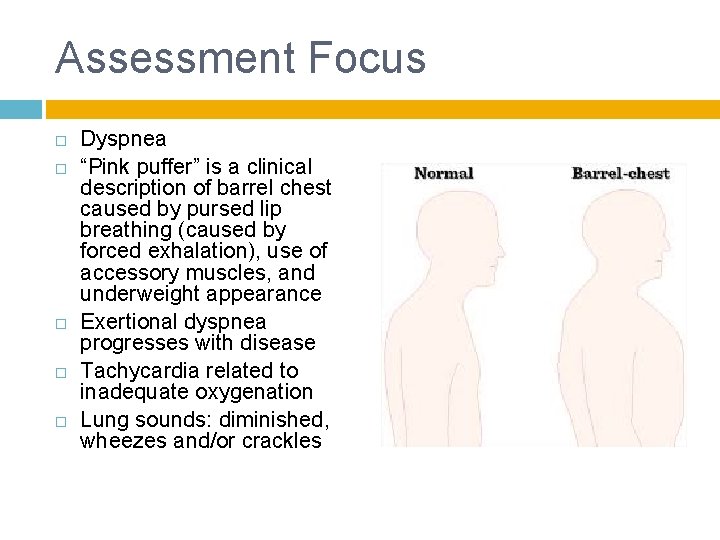
Assessment Focus Dyspnea “Pink puffer” is a clinical description of barrel chest caused by pursed lip breathing (caused by forced exhalation), use of accessory muscles, and underweight appearance Exertional dyspnea progresses with disease Tachycardia related to inadequate oxygenation Lung sounds: diminished, wheezes and/or crackles

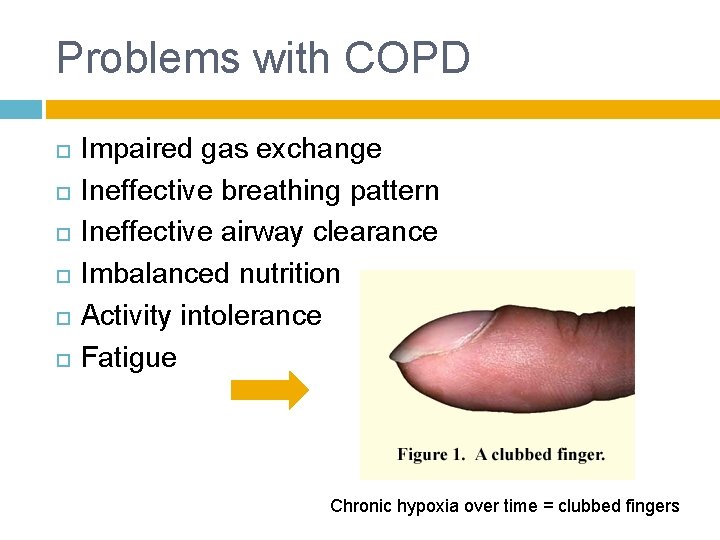
Problems with COPD Impaired gas exchange Ineffective breathing pattern Ineffective airway clearance Imbalanced nutrition Activity intolerance Fatigue Chronic hypoxia over time = clubbed fingers

Plan of Care The client will have adequate oxygenation and ventilation

Interventions Promotion of Oxygenation & Ventilation � Positioning ( HOB) � Apply oxygen and titrate to keep oxygen sats > 93% � Cough & deep breathing exercises (teaching) � Purse lip breathing (teaching) � Incentive spirometer (teaching)

Interventions-Medication Use Inhaled Bronchodilators � � Inhaled Corticosteroids � � Short-acting (albuterol) and long-acting (salmeterol, iprotropium, spiriva) Relax the muscle, open bronchioles Reduce inflammation Flovent, Pulmicort (bedesonide) � � Symbicort (Budesonide/formoterol) Advair (fluticasone/salmeterol) Theophyline Phosphodiesterase-4 (PDE -4) Inhibitors (roflumilast) Combination inhalers � Methylxanthines improve quality of life Antibiotics for infections Oral and or IV corticosteroids – only used for acute exacerbations (prednisone, methylprednisone) Oxygen therapy (for home) Vaccines http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 2699952/

Education on Meter-Dose Inhalers (MDIs)

Inhaler with Spacer

Interventions-cont. Pulmonary rehabilitation (PR) � exercise, diet Patient teaching � Smoking cessation � Corticosteroid use Weight gain-water retention Immunosuppression Increased glucose levels Rinse mouth after use of inhaler (increase risk of thrush) insomnia � Bronchodilators Increased heart rate, jitteriness

Evaluation of the Interventions Focus your attention on the interventions Reassess and adjust according to the evaluation � Lung sounds � Patient complaints and ability to function with the disease

Patient Education Acute exacerbation - Hospital Pneumococcal Vaccine Influenza Vaccine Chronic Disease – Home Care Pneumococcal Vaccine Influenza Vaccine Oxygen Therapy � Flammable

References Ignatavicius, D. D. & Workman, M. L. (2010). Medical-surgical nursing: patient-centered collaborative care (6 th ed. ). St. Louis, MO: Saunders Elsevier. Lewis, S. L. , Heitkemper, M. M. , Dirksen, S. R. , & Bucher, L. (2014). Medical-surgical nursing: Assessment & management of client problems (9 th ed. ). St. Louis, MO: Mosby Hogan, M. , Dentlinger, N. C. , & Ramdin, V. (2014). Medical-surgical: nursing pearson nursing reviews and rationales (3 rd ed. ). Boston, MA: Pearson.