Nursing Care of Children with altered Genitourinary Function
































- Slides: 36

Nursing Care of Children with altered Genitourinary Function (2) Dr. Manal Kloub

Outline • Nephrotic Syndrome • Renal Failure 1. Acute 2. Chronic

Nephrotic Syndrome ( Nephrosis ) v It is a clinical state that includes massive v 1. 2. Proteinuria, Hypoalbuminemia , hyperlipidemia and edema The disorder can occur as A primary disease known as idiopathic Nephrosis. Childhood Nephrosis, Minimal change nephritic Syndrome (MCNS). A secondary disorder that occur as a clinical manifestation after or in association with Glomerular damage

Nephrotic Syndrome 3. Congenital form inherited as an autosomal recessive disorder. • Nephrotic Syndrome occur in children between 2 -7 years of age ; it is rare in children younger than 6 months of age • Patients with (MCNS) are twice as likely to be male.

Pathophysiology • It is not understood • There may be a metabolic , biochemical, physiochemical or immune- mediated disturbances that cause the basement membrane of the glomeruli to become increasingly permeable to protein

Pathophysiology • Renal Glomerular damage -----Proteinuria ( massive) ---- hypoprotienemia • Hypoprotienemia– increased hepatic synthesis of protein and lipids --hyperlipidemia • hypoprotienemia – deceased oncotic pressure 1 - edema 2 - hypovolemia

Pathophysiology 1. Decreased renal blood flow --- Renin 2. release ---- vasoconstriction increased secretion of ADH and aldosterone --- Na+ and water reabsorption --- Edema

Assessment Clinical Manifestation • Weight gain • Periorbital edema especially in morning from head dependent position • abdominal cavity edema ( ascities ) • Scrotal edema extremely marked • anorexia , vomiting • Diarrhea caused by intestinal edema and poor absorption by edematous membrane • Pleural effusion • Ankle/leg swelling. • Irritability, easily fatigued , lethargic

Diagnostic Evaluation q. Blood pressure normal or slightly decreased q. Susceptibility to infections q. Urine alterations decreased volume and frothy q. Laboratory studies reveal a. Marked Proteinuria ( +3 or higher ) which almost b. q entirely albumin low serum protein concentration , reduced serum albumin significantly , elevated plasma lipids serum and platelets count may be elevated Renal biopsy if the patient dose not respond to a 4 -8 weeks courses of steroids

Management • Dietary restriction includes a low salt diet and fluid • • restriction Diuretic therapy Sometimes infusions of 25% albumin are used Acute infection are treated with appropriate antibiotics Corticosteroids are the first line of therapy for MCNS Relapse are treated with a repeated course of high dose steroid therapy MCNS episodes often happen in conjunction with viral or bacterial infection Relapses in children may continue over many years

Complications • Infection peritonitis, cellulites and pneumonia • Circulatory insufficiency secondary to hypovolemia • Thromboembolism

Prognosis • The prognosis for ultimate recovery in most cases is good • It is self limited disease • In children who respond to steroid therapy the tendency to relapse decreases with time

Nursing care • • • Daily monitoring of intake and out put Weight the child daily Examine urine daily for albumin Measure abdominal girth daily Assessment of edema (pitting, color& texture of skin Monitor V/S to detect any signs of shock or infections( respiratory )

Nursing care • Formulate a nutritionally adequate and • • attractive diet Adjust activities according to children tolerance level Edema and fluids restricted during the edema phase and allowed when edema subsides. • Family support and home care ( urine examination , medication taken , prevent infection)

Renal Failure (RF) • RF Is the inability of the kidney to excrete waste material, concentrate urine and conserve electrolytes. • The disorder can be 1. Acute 2. Chronic Terms used in RF • Azotemia : a accumulation of nitrogenous waste products within the blood • Uremia: retention of notoriousness products produce toxic symptoms often involve other body systems • and its a life threatening


Acute Versus Chronic • Acute – – sudden onset rapid reduction in urine output Usually reversible Tubular cell death and regeneration – – – Progressive Not reversible Nephron loss • Chronic • 75% of function can be lost before its noticeable

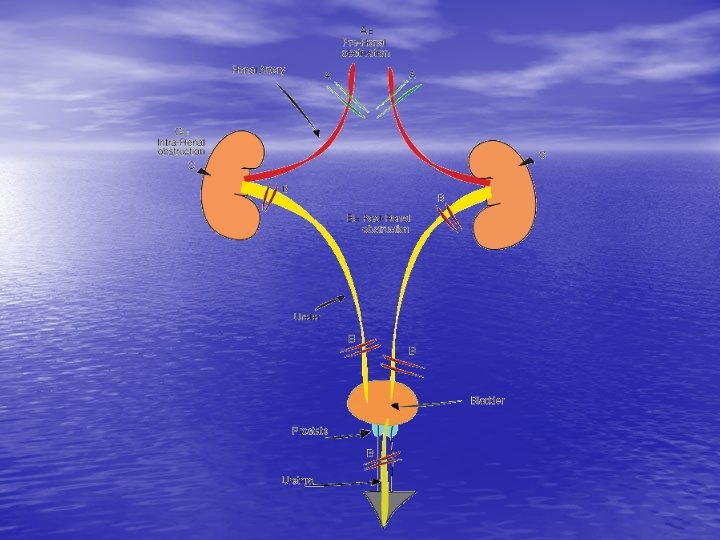
Acute Renal Failure • Most often occurs because of sudden body insult such as • • • 1. 2. 3. sever dehydration Resulted in Oliguria Azotemia Acidosis Diverse electrolytes disturbance Causes Prerenal Intrinsic renal Post renal

Causes of ARF • Pre-renal = – vomiting, diarrhea, poor fluid intake, fever, use of diuretics, and heart failure – cardiac failure, liver dysfunction, or septic shock • Intrinsic = – Interstitial nephritis, acute glomerulonephritis, tubular necrosis, ischemia, toxins • Post-renal = – prostatic hypertrophy, cancer of the prostate or cervix, or retroperitoneal disorders – neurogenic bladder – bilateral renal calculi, papillary necrosis, coagulated blood, bladder carcinoma, and fungus


Assessment • • • Decrease urine output (70%) Edema, esp. lower extremity Mental changes Heart failure Nausea, vomiting Pruritus Anemia Tachypenic Cool, pale, moist skin

Diagnosis of Renal Failure • 1. 2. 3. 4. • Blood studies include BUN and creatinine elevated Hyperkalemia ( 6 meq/l ) Hypocalcaemia which leads to osteodystrophy Increase phosphorus Urine creatinine clearance urine specific gravity decreased

Acute Renal Failure Management • Treat life threatening conditions • Identify the cause if possible • Treat reversible elements – Hydrate – Remove drug – Relieve obstruction


Hyperkalemia Symptoms • • • Weakness Lethargy Muscle cramps Paresthesias Lowered blood pressure Dysrhythmias


Hyperkalemia Treatment • • • Calcium gluconate (carbonate) Sodium Bicarbonate Insulin/glucose Kayexalate Lasix Hemodialysis

Diet • • • low in protein, potassium , sodium Increase Carbohydrates Restrict fluids Daily weight Accurate recording for intake & out put

Chronic Renal Failure • It begins when the diseased kidneys can no • longer maintain the normal chemical structure of body fluids under normal conditions Glomerular filtration rate decreased below 10 to 15 % of normal.

Chronic Renal Failure Causes • The most common causes before 5 years are congenital renal and urinary tract malformation such as renal hypoplasia, obstructive uropathy & Vesicoureteral reflux • Glomerular and hereditary diseases in children ages 5 -15 years • Chronic pyelonephritis , chronic glomerulonephritis • Systematic diseases such as (Lupus erythematosus, anaphylactic purpura) • Polycystic kidney disease • Renal vascular disorder such as hemolytic Uremic syndrome (HUS) vascular thrombosis

CRF Symptoms • • Malaise Weakness Fatigue Neuropathy CHF Anorexia Nausea Vomiting • • • Seizure Constipation Peptic ulceration Anemia Pruritus Abnormal hemostasis

Treatment 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. low protein, phos, & potassium diet Daily fluid intake restriction Low sodium intake such as ( chips) Calcium supplement anti- hypertension blood transfusion Human erythropoietin Growth hormone may be given in some children Dialysis kidney transplant

Dialysis • • • Patients with CRF eventually require dialysis Diffuse harmful waste out of body Control BP Keep safe level of chemicals in body 2 types – Hemodialysis – Peritoneal dialysis

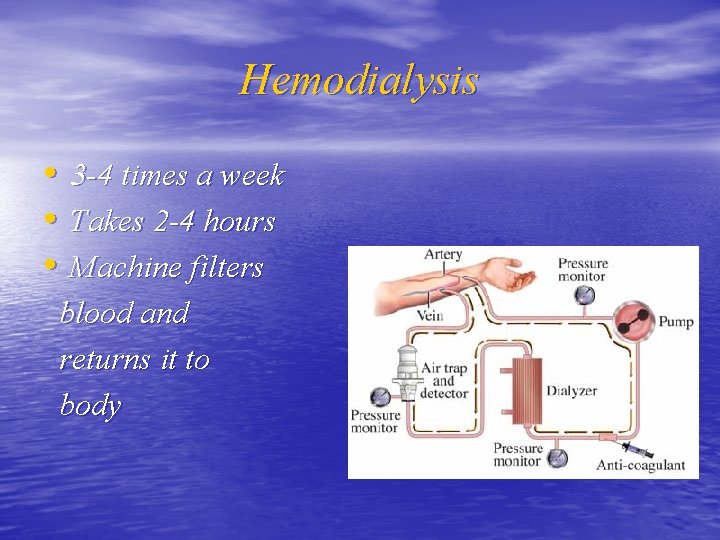
Hemodialysis • 3 -4 times a week • Takes 2 -4 hours • Machine filters blood and returns it to body

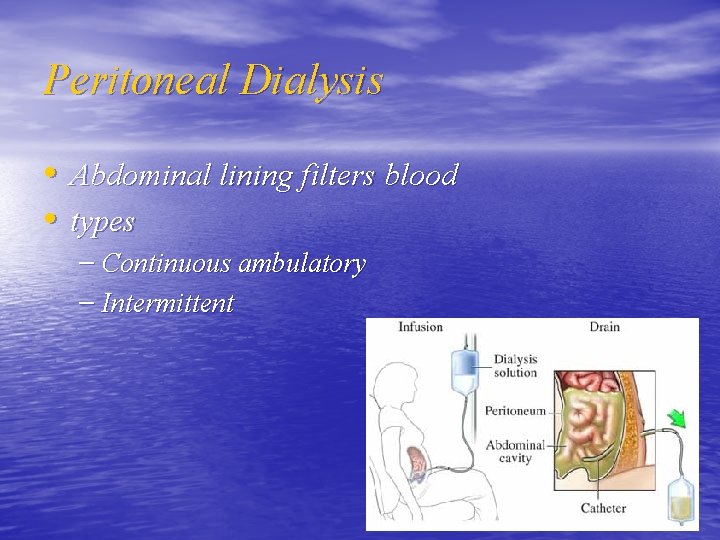
Peritoneal Dialysis • Abdominal lining filters blood • types – Continuous ambulatory – Intermittent

Thank you