NUR 941943 AcidBase and Metabolic Acidosis Review Melanie

NUR 941/943 Acid-Base and Metabolic Acidosis Review Melanie Hardin-Pierce, DNP, APRN, ACNP-BC University of Kentucky College of Nursing

Scenario #1 • A 29 year old female is brought in via the emergency department unresponsive. She is currently intubated and on a D 5 NS gtt at 100 ml/hr. Her initial lab work is: Na 142 WBC 6. 9 Ph 7. 12 K 5. 1 Hgb 9. 8 Pa. O 2 106 Cl 106 Hct 30. 1 Pa. CO 2 31 CO 2 13 Platelets 187 K O 2 Sat 94% BUN 32 Creat 1. 8 Glu 104 Bicarb 12

Scenario #1: What can you learn from her blood work? Na 142 WBC 6. 9 Ph 7. 12 K 5. 1 Hgb 9. 8 Pa. O 2 106 Cl 106 Hct 30. 1 Pa. CO 2 31 CO 2 13 Platelets 187 K O 2 Sat 94% BUN 32 Creat 1. 8 Glu 104 Bicarb 12

B. What are possible causes for her unresponsiveness and her acid-base disturbance?

C. What additional lab work do you order and why?

High Anion Gap Metabolic Acidosis • p. H < 7. 35 is acidemia • Occurs due to 1. increased acid 2. loss of bicarb or 3. diminished renal acid excretion • High anion gap vs normal anion gap acidosis

Causes of Metabolic acidosis Mechanism of acidosis Increase AG Increased acid production Lactic acidosis Normal AG Ketoacidosis – DM Starvation, ETOH Ingestions – methanol, Toluene ingestion if late ethylene glycol, ASA and if renal fx is preserved (salicylate), Toluene, other glycols Loss of Bicarbonate Diarrhea, other GI fluid loss Type 2 (prox) renal tubular acidosis (RTA) Post DKA Ureteral diversion (ileal loop) Carbonic anhydrase inhibitors Decreased renal acid excretion Chronic kidney disease Type 1 RTA or Type 4 RTA (aldosteronism)

Serum anion gap • Na – (Cl+ HCO 3) • Measured cations – measured anions • Nl is 7 -13 meq/L however, this can vary based on lab instruments and methods. Should consider pts baseline if known. i. e is baseline is 4, and it is now 12, then the elevation is significant despite still being in the “normal range”

Treatment of High AG Metabolic Acidosis (controversial) • IV Bicarbonate therapy (50 meq/50 ml) or THAM (Tromethamine) for p. H < 7. 0 for acute metabolic High AG acidosis. One amp Na. Bicarb will generally raise the HCO 3 level by 1. 3 -1. 5 meq/L in a 70 kg pt, so 1 -2 amps IVP or as a gtt. • THAM dose = kg X desired HCO 3 – actual HCO 3) X 1. 1

Scenario #2 • A 42 year old male is admitted to your service fro the ED. He was brought to the Ed by his family after he passed out at home. On his initial work-up in the ED his vitals and labs were: Next slide…. .
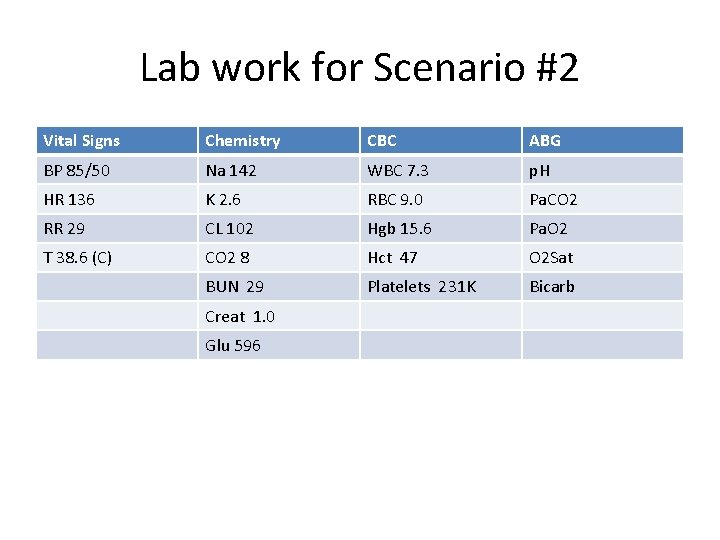
Lab work for Scenario #2 Vital Signs Chemistry CBC ABG BP 85/50 Na 142 WBC 7. 3 p. H HR 136 K 2. 6 RBC 9. 0 Pa. CO 2 RR 29 CL 102 Hgb 15. 6 Pa. O 2 T 38. 6 (C) CO 2 8 Hct 47 O 2 Sat BUN 29 Platelets 231 K Bicarb Creat 1. 0 Glu 596

A. What is the probably cause for this patient's problems and what test would confirm your diagnosis?

Outline your initial treatment plan for this patient

IV Fluids for DKA • Determine hydration status • Severe dehydration – give 0. 9 %Na. Cl (1. 0 L/hr) • Mild dehydration – Evaluate corrected serum Na, if normal or high give 0. 45% Na. Cl (250 -500 Ml/hr); If low give 0. 9%Na. Cl (250 -500 m. L/hr) • When serum glucose is 200, change to D 5% + 0. 45% Na. Cl at 150 -200 m. L/hr • Check e-lytes, BUN, creat, venous p. H q 2 -4 hours until stable; q 1 hour glucose while on insulin gtt

Insulin • IV route for critically ill pt. Can do SC for uncomplicated pts using rapid acting insulin (0. 3 U/kg, then 0. 2 U/kg one hr later, then 0. 2 U/kg SC q 2 hrs) • Insulin - regular 0. 1 U/kg IV bolus then, • 0. 1 U/kg/hr IV gtt • If glu does not fall by 50 -70 mg/d. L in the first hour, re-bolus with double the IV bolus dose • When glu is 200, reduce insulin IV gtt rate to 0. 02 -0. 05 U/kg/hr. Keep glu between 150 and 200 until anion gap normalizes. • After resolution of DKA and when patient is able to eat, initiate SC multi-dose insulin regimen. Continue the IV insulin for 1 -2 hr after SC insulin is begun to ensure adequate plasma insulin levels. Can start SC insulin at 0. 5 U/kg to 0. 8 U/kg per day and adjust as needed. • Be sure precipitating causes are addressed i. e. infection

Potassium • Establish adequate renal fx and UOP • If < 3. 3 hold insulin and give 20 -30 m. Eq KCL/hr until K > 3. 3 • If > 5. 3 do not give KCL but check serum K level q 2 hrs • If > 3. 3 but < 5. 3 give 20 -30 m. Eq KVL in each liter of IV fluids to keep serum K level between 4 -5.

Bicarbonate • If p. H < 6. 9 dilute Na. CO 3 (100 mmol) in 400 m. L saline with 20 m. Eq KCL and infuse over 2 hours. • Repeat q 2 hr until p. H > 7. 0 • Monitor serum K level q 2 • If p. H > 7. 0, hold HCO 3

Scenario #3 • A 26 year old female is admitted with a 3 day history of nausea, vomiting and diarrhea. Her vital signs on admission are: BP 90/42; HR 121; RR 21; T 38. 20 C Her initial labs show a Na+ 156; K+ 3. 1; Cl- 108; CO 2 18; BUN 29; Creat 1. 6; Gluc 102; WBC 10. 2; Hgb 15. 1; Hct 45; plt 132

What are the problems that this patient has by evaluation of her lab work ?

What are the problems that this patient has by evaluation of her lab work ? • Hypernatremia (hypovolemic type), • Hypokalemia, • Slight hyperchloremia, • acidosis, • elevated Creatinine & BUN, • acute renal failure (unsure if its acute on chronic, need PMH); • she can also have an underlying metabolic alkalosis because of her vomiting • and loss of HCl.

What acid/base abnormalities could this patient have based upon both her history and her lab values ?

What acid/base abnormalities could this patient have based upon both her history and her lab values ? Patient has an Anion Gap Metabolic Acidosis with AG of 30. (Na –(Cl + CO 2)= AG) and most likely has a nongap metabolic acidosis as well. Need ABG to determine more fully. Patient has had 3 day h/o nausea, vomiting, diarrhea, and an elevated BUN and Creatinine. The Non gap metabolic acidosis is most likely a result of the loss of bicarbonate from the large Gi losses. The Anion Gap metabolic acidosis can be from infection (pt with low grade fever, lactic acidosis, rhabdomyolysis which can happen in pts with long h/o N/V/D, as well as certain medications such as metformin, ASA (need to check med history. ) She probably has a combination of both since with both vomiting (loss of acid leading to alkalosis) and diarrhea leading to loss of bicarb and acidosis.

The patient’s weight is 59 kg. What is her fluid deficit? • at her free water deficit is calculated at 4 liters 0. 6(59) x ([156/140] - 1)

What would your treatment plan be for this patient ?

What would your treatment plan be for this patient ? • Do a Complete H&P including, medication history and neurological exam. Labs: ABG, Renal Function Panel, Mg, i. Ca, Urine Na, K, urine Eosinophil, urine glucose, UA, Urine Culture, serum osmo, urine osmo, lactate. C-diff, stool O & P; Treat hypotension and tachycardia (hypervolemia) first with isotonic sodium chloride prior to free water administration. Correct serum sodium at a rate of 2 to 3 m. Eq/L/h or 12 m. Eq/L/d. Check serum and urine electrolytes every 2 hours, complete serial neurologic exams

Scenario #4 • A 26 year old is admitted to your ICU after ingesting ½ bottle of extra strength Tylenol. He is currently arousable to verbal stimuli, is oriented x 4 and is able to follow commands. Outline your treatment plan.

Plan • Assess and monitor ABC’s. Patient may need to be intubated to protect airway, patients often con’t to have declining neurological status and are at high risk for vomiting, placing them at increasing risk for aspiration. • Monitor pt closely: cardiac monitor, frequent VS, strict I&O • Check Tylenol level, aspirin level, UDS, CMP, Hemogram, ABG, CXR, UPT, bilirubin • Draw 4 hour post ingestion level • Give activated charcoal (if with in one to 2 hours of acute ingestion) • If 4 hour post ingestion level is greater than 150 start IV N-acetylcysteine 150 mg/kg over 60 minutes, then 50 mg/kg over 4 hours, then 100 mg/kg over 16 hours (can de-escalate as Tylenol level returns) • Treat N/V with Zofran PRN
- Slides: 27