Now its time to choose the right prescription










































- Slides: 43

Now it’s time to choose the right prescription drug plan. Your presenter today: Name, Title 600398. 1013 Y 0096_MRK_TMP_PDSALPRE 14 Approved 09092013

• Medicare Part D overview • Your 2014 Blue Cross Medicare. Rx (PDP)SM Plan Options • Enrolling in Blue Cross Medicare. Rx. SM • Questions 2

Medicare Part D Overview • Medicare Part D helps to pay for your covered prescription medications • Also referred to as prescription drug coverage or prescription drug plan (PDP) 3

• Must have Medicare Part A and/or Part B • Must live in the Part D plan’s service area • If you are covered by an employer or union: • Could affect your benefits • Call Benefits Administrator • Read plan communications 4

There are three enrollment periods: 1. Annual Enrollment Period (AEP) • October 15 to December 7 • Enroll for the first time or • switch plans Effective date: January 1 • Note: If you like what you have, there is no need to switch 5

2. Initial Enrollment Period (IEP) • Enroll when you first become eligible: • 7 -month period that starts 3 months before the month you turn 65, includes the month you turn 65, and ends 3 months after the month you turn 65 • Effective date: Generally, first of the month following enrollment, or first of birthday month 6

3. Special Enrollment Period (SEP) • Enroll or switch plans due to special circumstances • Moving to a new state • Enrolling in or disenrolling from a Part C Plan • Eligible for Low Income Subsidy assistance • Enrolling in both Medicare and Medicaid • Retiree losing group health coverage • Other situations that may be applicable • Effective date: Generally, first of the month following enrollment 7

• You may have higher premiums unless you had “creditable” coverage • You will be assessed 1% of the Medicare base beneficiary premium for every month in which you were eligible to enroll but did not enroll Note: You will not be charged a late enrollment penalty if your situation changes and you need to buy Part D, as long as you had creditable coverage and you apply within 63 days of the end of your creditable coverage. 8

• Some group health plans’ retiree coverage • State pharmacy assistance program • Veterans Affairs coverage • Military coverage, including TRICARE 9

10

Let’s look at the 2014 CMS designated plan design: • Annual Deductible: $310 This means you pay the first $310 in approved drug costs before your Part D benefits begin Deductible $310 Initial Limit $2, 970 $2, 930 The Gap $4, 700 $4, 750 Catastrophic 11

• Initial Limit: $2, 850 What counts toward the Initial Limit? • Once you have met your deductible, you typically pay a fixed amount (copay) to fill an approved prescription • Your Part D plan pays the balance of the drug cost for the prescription Deductible $310 Initial Limit $2, 850 The Gap $4, 700 $4, 750 Catastrophic 12

• Coverage Gap: $2, 850 to $4, 550 • You will reach the Coverage Gap after you and your plan have reached $2, 850 in drug costs • You will then be responsible for all costs while in the Coverage Gap, until you reach $4, 550 in True Out-Of-Pocket (Tr. OOP) costs • Note: During this time, you may be eligible for a 52. 5% discount on brand name drugs and a 28% discount on generic drugs at the time of purchase Deductible $310 Initial Limit $2, 850 Tr. OOP $4, 550 ( = Deductible + Catastrophic Initial Limit + Out. Of-Pocket Costs ) 13

• Catastrophic Coverage: $4, 550 • Medicare pays 95% of your approved drug costs once you reach the True Out-Of-Pocket (Tr. OOP) maximum at $4, 550 Deductible $310 Initial Limit $2, 850 Tr. OOP $4, 550 Catastrophic 14

• The Tr. OOP maximum amount is the amount of money you need to spend to reach Catastrophic Coverage • Thereafter you pay a minimum cost share of $2. 55 for generic or $6. 35 for brand name drugs, and 5% for specialty drugs for the remainder of 2014 • Tr. OOP consists of: • Deductible = $310 in 2014 • Copays or coinsurance you pay in 2014 • Once you reach $4, 550 out of your own pocket, the Medicare Catastrophic Coverage benefit begins 15

During the gap, all plans offer a manufacturer discount on brand name drugs* Your cost share for generics is decreasing each year* • 79% in 2013, 72% in 2014 Brand Drug A = $60 Generic Drug B = $20 Gap Coverage = None, but 28% discount applies Member Pays $28. 50 Plan’s payment responsibility: $1. 50 Member Pays $14. 40 Manufacturer Discount $30 (72% of the $20 generic Rx cost) Discount $5. 60 (28% of the $20 Generic Rx cost) Amount toward Tr. OOP: $58. 50 Amount toward Tr. OOP: $14. 40 *Discounts during the gap are available to members who do not receive extra help. Members who receive extra help have limited income and qualify for up to 100% of drug costs including monthly premium, annual deductibles and copays/coinsurance. 16

• Medicare prescription drug plan premiums • Most third-party payment arrangements • Drugs purchased outside the U. S. • Over-the-counter drugs • Drugs not on the plan’s formulary 17

• Part D-IRMAA stands for Part D income-related monthly adjustment amount • Effective January 1, 2011 • An additional amount for Medicare Part D drug coverage • Pay your Part D-IRMAA directly to Medicare, not to your plan • Required by law to pay the Part D-IRMAA based on your income, even if you have drug benefits through a union or employer-sponsored Medicare drug plan 18

• List of prescription drugs covered by a health insurance company • Varies between health insurance companies 19

• Under certain conditions, a Part D plan can make changes during the year by: • Adding or removing drugs based on safety concerns • Moving a drug to a higher or lower cost sharing tier (usually only when a brand goes off its patent) • Adding utilization management (step therapy, prior authorization, quantity limits, etc. ) • Ask your doctor to switch you to a drug on the formulary or ask for an exception 20

• The Exception Process ensures access to medically necessary Medicare-covered prescription drugs • Enrollees can request an exception if: • The enrollee is using a drug that • • • has been removed from the formulary A non-formulary drug is prescribed and medically necessary The cost-sharing tier of a drug an enrollee is using changes A drug covered under a more expensive cost-sharing tier is prescribed because the less expensive drug is medically inappropriate 21

22

23

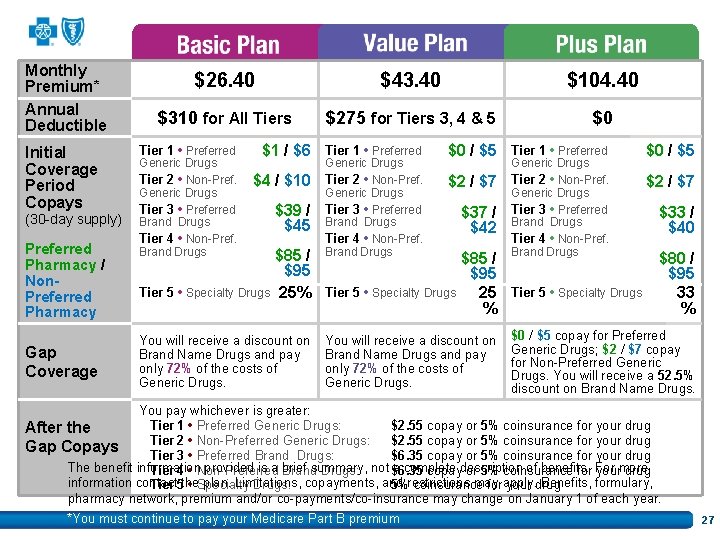
Monthly Premium* Annual Deductible Initial Coverage Period Copays (30 -day supply) Preferred Pharmacy / Non. Preferred Pharmacy Gap Coverage $26. 40 $39. 80 $101. 10 $310 for All Tiers $275 for Tiers 3, 4 & 5 $0 Tier 1 • Preferred Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $1 / $6 Tier 1 • Preferred $4 / $10 Tier 5 • Specialty Drugs $39 / $45 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $0 / $5 Tier 1 • Preferred $0 / $5 $2 / $7 $37 / $42 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $85 / $95 25% Tier 5 • Specialty Drugs 25 Tier 5 • Specialty Drugs % You will receive a discount on Brand Name Drugs and pay only 72% of the costs of Generic Drugs. $33 / $40 $80 / $95 33 % $0 / $5 copay for Preferred Generic Drugs; $2 / $7 copay for Non-Preferred Generic Drugs. You will receive a 47. 5% discount on Brand Name Drugs. You pay whichever is greater: Tier 1 • Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug After the *You must continue to pay your Medicare Part B premium Tier 2 • Non-Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug Gap Copays Tier 3 • Preferred Brand Drugs: $6. 35 copay or 5% coinsurance for your drug The benefit information provided is a brief summary, not a complete of benefits. Tier 4 • Non-Preferred Brand Drugs: $6. 35 copaydescription or 5% coinsurance for For yourmore drug information contact the plan. Limitations, copayments, and restrictions may apply. Benefits, formulary, Tier 5 • Specialty Drugs: 5% coinsurance for your drug pharmacy network, premium and/or co-payments/co-insurance may change on January 1 of each year. 24

Monthly Premium* Annual Deductible Initial Coverage Period Copays (30 -day supply) Preferred Pharmacy / Non. Preferred Pharmacy Gap Coverage $26. 40 $43. 40 $101. 10 $310 for All Tiers $275 for Tiers 3, 4 & 5 $0 Tier 1 • Preferred Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $1 / $6 Tier 1 • Preferred $4 / $10 Tier 5 • Specialty Drugs $39 / $45 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $0 / $5 Tier 1 • Preferred $0 / $5 $2 / $7 $37 / $42 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $85 / $95 25% Tier 5 • Specialty Drugs 25 Tier 5 • Specialty Drugs % You will receive a discount on Brand Name Drugs and pay only 72% of the costs of Generic Drugs. $33 / $40 $80 / $95 33 % $0 / $5 copay for Preferred Generic Drugs; $2 / $7 copay for Non-Preferred Generic Drugs. You will receive a 47. 5% discount on Brand Name Drugs. You pay whichever is greater: Tier 1 • Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug After the *You must continue to pay your Medicare Part B premium Tier 2 • Non-Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug Gap Copays Tier 3 • Preferred Brand Drugs: $6. 35 copay or 5% coinsurance for your drug The benefit information provided is a brief summary, not a complete of benefits. Tier 4 • Non-Preferred Brand Drugs: $6. 35 copaydescription or 5% coinsurance for For yourmore drug information contact the plan. Limitations, copayments, and restrictions may apply. Benefits, formulary, Tier 5 • Specialty Drugs: 5% coinsurance for your drug pharmacy network, premium and/or co-payments/co-insurance may change on January 1 of each year. 25

Monthly Premium* Annual Deductible Initial Coverage Period Copays (30 -day supply) Preferred Pharmacy / Non. Preferred Pharmacy Gap Coverage $26. 40 $43. 40 $104. 40 $310 for All Tiers $275 for Tiers 3, 4 & 5 $0 Tier 1 • Preferred Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $1 / $6 Tier 1 • Preferred $4 / $10 Tier 5 • Specialty Drugs $39 / $45 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $0 / $5 Tier 1 • Preferred $0 / $5 $2 / $7 $37 / $42 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $85 / $95 25% Tier 5 • Specialty Drugs 25 Tier 5 • Specialty Drugs % You will receive a discount on Brand Name Drugs and pay only 72% of the costs of Generic Drugs. $33 / $40 $80 / $95 33 % $0 / $5 copay for Preferred Generic Drugs; $2 / $7 copay for Non-Preferred Generic Drugs. You will receive a 52. 5% discount on Brand Name Drugs. You pay whichever is greater: Tier 1 • Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug After the *You must continue to pay your Medicare Part B premium Tier 2 • Non-Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug Gap Copays Tier 3 • Preferred Brand Drugs: $6. 35 copay or 5% coinsurance for your drug The benefit information provided is a brief summary, not a complete of benefits. Tier 4 • Non-Preferred Brand Drugs: $6. 35 copaydescription or 5% coinsurance for For yourmore drug information contact the plan. Limitations, copayments, and restrictions may apply. Benefits, formulary, Tier 5 • Specialty Drugs: 5% coinsurance for your drug pharmacy network, premium and/or co-payments/co-insurance may change on January 1 of each year. 26

Monthly Premium* Annual Deductible Initial Coverage Period Copays (30 -day supply) Preferred Pharmacy / Non. Preferred Pharmacy Gap Coverage $26. 40 $43. 40 $104. 40 $310 for All Tiers $275 for Tiers 3, 4 & 5 $0 Tier 1 • Preferred Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $1 / $6 Tier 1 • Preferred $4 / $10 Tier 5 • Specialty Drugs $39 / $45 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $0 / $5 Tier 1 • Preferred $0 / $5 $2 / $7 $37 / $42 Generic Drugs Tier 2 • Non-Pref. Generic Drugs Tier 3 • Preferred Brand Drugs Tier 4 • Non-Pref. Brand Drugs $85 / $95 25% Tier 5 • Specialty Drugs 25 Tier 5 • Specialty Drugs % You will receive a discount on Brand Name Drugs and pay only 72% of the costs of Generic Drugs. $33 / $40 $80 / $95 33 % $0 / $5 copay for Preferred Generic Drugs; $2 / $7 copay for Non-Preferred Generic Drugs. You will receive a 52. 5% discount on Brand Name Drugs. You pay whichever is greater: Tier 1 • Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug After the Tier 2 • Non-Preferred Generic Drugs: $2. 55 copay or 5% coinsurance for your drug Gap Copays Tier 3 • Preferred Brand Drugs: $6. 35 copay or 5% coinsurance for your drug The benefit information provided is a brief summary, not a complete of benefits. Tier 4 • Non-Preferred Brand Drugs: $6. 35 copaydescription or 5% coinsurance for For yourmore drug information contact the plan. Limitations, copayments, and restrictions may apply. Benefits, formulary, Tier 5 • Specialty Drugs: 5% coinsurance for your drug pharmacy network, premium and/or co-payments/co-insurance may change on January 1 of each year. *You must continue to pay your Medicare Part B premium 27

• Save money by switching to a generic • Talk to your doctor or pharmacist • To receive benefits, use Blue Cross Medicare. Rx network pharmacies or mail-order service except in an emergency • With preferred network pharmacies and mail-order, you may purchase a 90 -day supply of an eligible prescription drug and pay only two and a half months of copays instead of three • Some network pharmacies are NOT preferred; they do not offer lower copays for a 90 -day supply 28

• Save at any one of these or other preferred network pharmacies and their affiliates: • CVS, Sam’s Club, Walmart, and PPOK • Other pharmacies are available in our network • Eligible beneficiaries must use network pharmacies to access their prescription drug benefit, except under non-routine circumstances. Limitations, copayments, and restrictions may apply. • Pharmacies nationwide • Peace of mind while traveling 29

www. mybluepartd. com/selectplan/ok 30

31

• New to Medicare • Explore your options and consider enrolling in a plan, even if you do not take medications today • Health changes can be sudden • Protect yourself now • Peace of mind • Know that you are covered 32

• Your Medicare card • Other insurance information • Bank information if you choose automatic deduction 33

Over the phone 1 -866 -910 -9945 TTY/TTD: 711 8 a. m. – 8 p. m. , local time 7 days a week On the Web www. mybluepartd. com/enroll/ok By mail With agent www. bcbsok. com/medicareag ents 34

When we receive your enrollment application, the following steps will take place: 35

36

CMS requires we share the following information with you: • You must continue to pay your Medicare Part B premium. • The benefit information provided is a brief summary, not a complete description of benefits. For more information, contact the plan. • Limitations, copayments, and restrictions may apply. • All Medicare prescription drug plans agree to stay in the program for a full year at a time. Each year, the plans decide whether to continue for another year. Even if a Medicare prescription drug plan leaves the program, you will not lose Medicare coverage. • If a plan decides not to continue, it must send you a letter at least 90 days before your coverage will end. The letter will explain your options for Medicare coverage in your area. • Benefits, formulary, pharmacy network, provider network, premium and/or copayments/co-insurance may change on January 1 of each year. • Members may enroll in the plan only during specific times of the year. For more information, contact the plan. 37

• Banking information cannot be accepted over the phone. • Medicare beneficiaries may also enroll in Blue Cross Medicare. Rx through the CMS Medicare Online Enrollment Center located at www. medicare. gov • This information is available for free in other languages. Please call our customer service number at 1 -888 -285 -2249 for additional information. We are open between 8 a. m. and 8 p. m. , local time, 7 days a week. If you are calling from February 15 through September 30, alternate technologies (for example, voicemail) will be used on the weekends and holidays. TTY/TDD: 711. • Esta información está disponible en otros idiomas de forma gratuita. Comuníquese a nuestro número de Servicio al Cliente llamando al 1 -888 -2852249 para obtener información adicional. (Los usuarios de TTY/TDD deberán llamar al 711). Estamos a su disposición de 8: 00 a. m. a 8: 00 p. m. , los siete días de la semana. Si llama del 15 de febrero al 30 de septiembre, se utilizarán tecnologías alternas (por ejemplo, correo de voz) durante los fines de semana y días feriado. TTY/TDD: 711. 38

No one working with Medicare Part D is allowed to: Ñ Come to your home uninvited to sell or endorse any Medicare-related product Ñ Seek premium payments up front or before you have been billed Ñ Call you after you have asked not to receive additional calls Blue Cross and Blue Shield of Oklahoma Ñ Call before 8 a. m. or after 9 p. m. Ñ Offer a gift or a cash payment • Available 24/7 • to entice you to enroll Fraud Hotline 1 -800 -543 -0867 39

Medicare • • Phone: 1 -800 -MEDICARE (1 -800 -633 -4227) TTY 1 -877 -486 -2048 24 hours a day / 7 days a week Web: www. medicare. gov Social Security • • Phone 1 -800 -772 -1213 TTY 1 -800 -325 -0778 Between 7 a. m. and 7 p. m. , Monday – Friday Web: www. ssa. gov 40

Prescription drug plan provided by Blue Cross and Blue Shield of Oklahoma, which refers to HCSC Insurance Services Company (HISC), an independent licensee of the Blue Cross and Blue Shield Association. A Medicare-approved Part D sponsor. Enrollment in HISC’s plan depends on contract renewal. 41

42
