Northeast Regional Epilepsy Group Christos Lambrakis M D

Northeast Regional Epilepsy Group Christos Lambrakis M. D. 1

October 29 th, 2016 How is Epilepsy Diagnosed Recognizing Types of Seizures and Imitators of Epilepsy 2
3

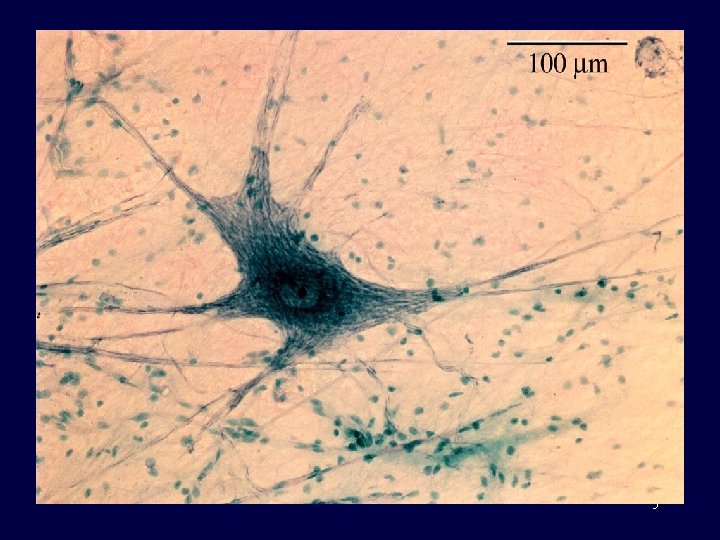
Brain *Weight: 3 lbs *Made of 75% water * 2% of body weight * 20% of energy requirements *Contains 100 billion neurons *Each neuron has 1000 to 10, 000 synapses *100, 000 miles of blood vessels *Likes: Oxygen, Glucose, Cute cat videos
5
6
7

8

What is a Seizure? • A seizure is caused by abnormal electrical activity between cells of the brain (neurons) • A seizure can temporarily disturb many of the brains normal functions. • This abnormal electrical activity results in the clinical manifestations of the seizure. 9

What is a Seizure? • The clinical manifestations of the seizure are determined by the region of the brain where the abnormal electrical activity is located. • Clinical manifestations of a seizure are varied depending on the region of the brain involved. Examples include changes in movement, sensation, behavior or awareness. 10
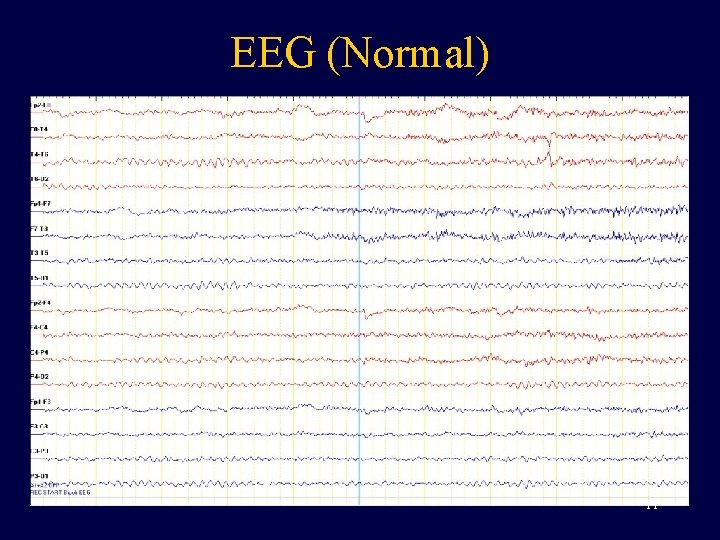
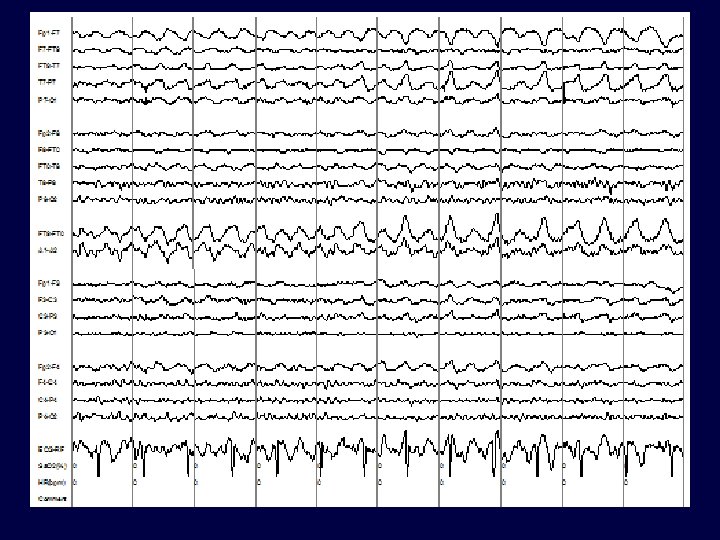
EEG (Normal) 11
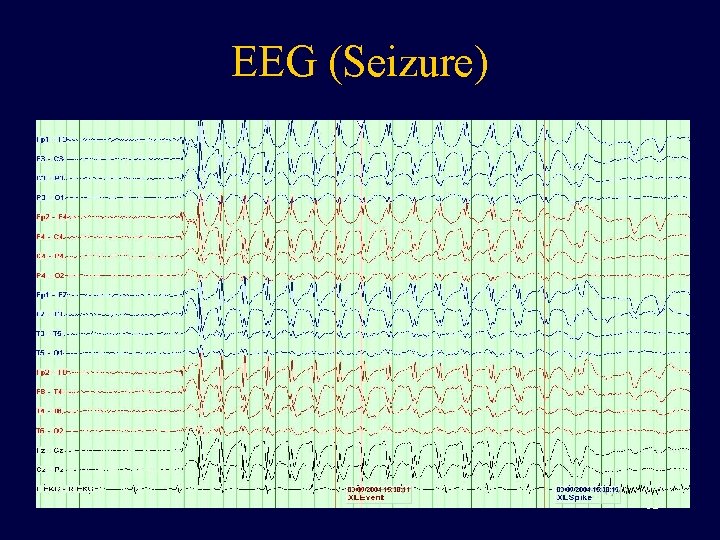
EEG (Seizure) 12

What is Epilepsy? • Epilepsy is the term applied to the state of recurrent seizures. • Epilepsy is a condition of the brain, of various causes, which predisposes the patient to recurrent epileptic seizures. • Epilepsy is a tremendously variable condition in terms of its cause, seizure types and response to treatment. 13

How is Epilepsy Diagnosed? 14

Epilepsy Diagnosis • Clinical description of the seizure events provides very important information. – What was seen? (Confusion, Loss of consciousness, Body movements, Head turning, Eye deviation, Right side/Left side or both) – What was felt by the patient? (At the start of the seizure (Aura) or as seizure evolves) • **Helps us to localize the seizure (where in the brain did it originate from).

Epilepsy Diagnosis • Precipitating factors: – Lack of sleep, fever, current illness, medications, flashing lights, hyperventilation. • Predisposing factors: – Past medical history (head trauma, stroke), Family history • **Helps us to better understand why the seizures occurred (Etiology). 16

Epilepsy Diagnosis • Physical Examination – Vitals (Fever) – General (Head size, dysmorphic features, skin lesions, stiff neck). – Neurologic Examination (Confusion, memory loss, speech difficulty, motor weakness, sensory loss) 17

Epilepsy Diagnosis • Acute Symptomatic Seizures • Chronic Symptomatic Seizures • Idiopathic Seizures 18

Epilepsy Diagnosis-Etiology • Acute Symptomatic Seizures (Seizures caused by a suspected acute reason). – Trauma (Head injury) – Metabolic (Electrolyte imbalance, Uremia) – Toxic (Ingestion, Medication) – Infectious (Meningitis, Encephalitis, Sepsis) – Vascular (Stroke, Hemorrhage) 19

Epilepsy Diagnosis-Etiology • Chronic Symptomatic Seizures (Seizures caused by preexisting conditions which favor the development of seizures). – Remote injury (Past head injury, Birth trauma) – Developmental (Cortical dysplasia) – Degenerative Disorders (Alzheimer’s) – Metabolic (Amino and organic acid disorders) 20

Epilepsy Diagnosis-Etiology • Idiopathic Seizures (Etiology is unclear) – The cause of the seizures cannot be determined from our current knowledge or conventional testing. – Approximately 50% of patients will fall under this category. 21

Epilepsy Diagnosis Diagnostic Studies • Blood work (Electrolytes such as Sodium, Potassium, Calcium; Glucose, Kidney and Liver function) • Electro-diagnostic (EEG) • Imaging (CT, MRI, SPECT, PET and MEG) 22

Electroencephalogram (EEG) 23

Electroencephalogram EEG • Represents a record of the small shifting brain electrical potentials from the surface of the brain recorded over the scalp. • As seizures are caused by a disturbance of electrical activity, the EEG is uniquely suited to further our understanding of a patients seizures.

Goals of Video-EEG Monitoring • Is it really an epileptic seizure? (Epilepsy vs. non-epileptic events) • What type of seizure is it? (Characterize epilepsy type) • Where does the seizure originate from? Is it focal? (i. e. does it come from one specific region? )

Electrodes 26
27
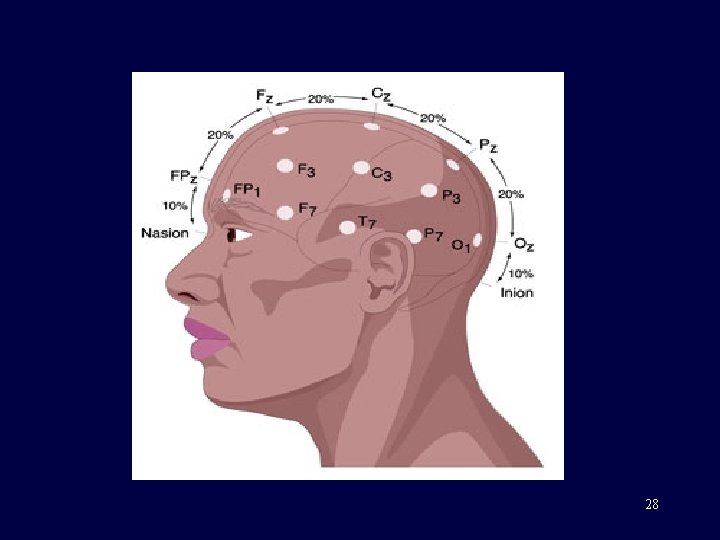
28
29
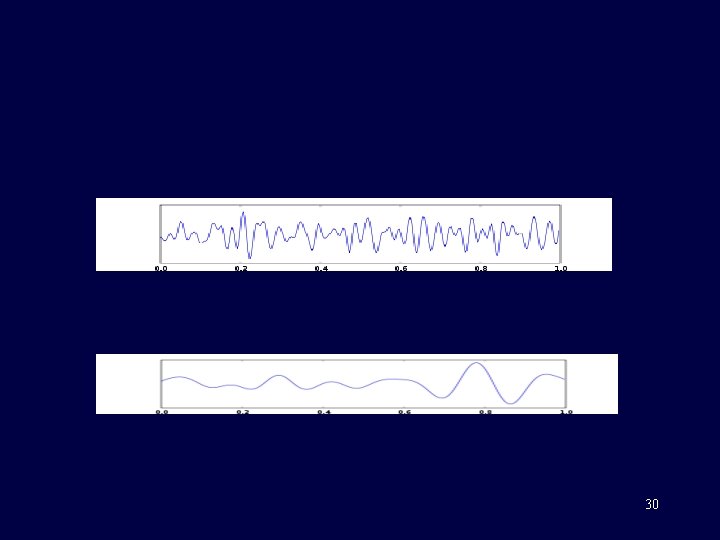
30
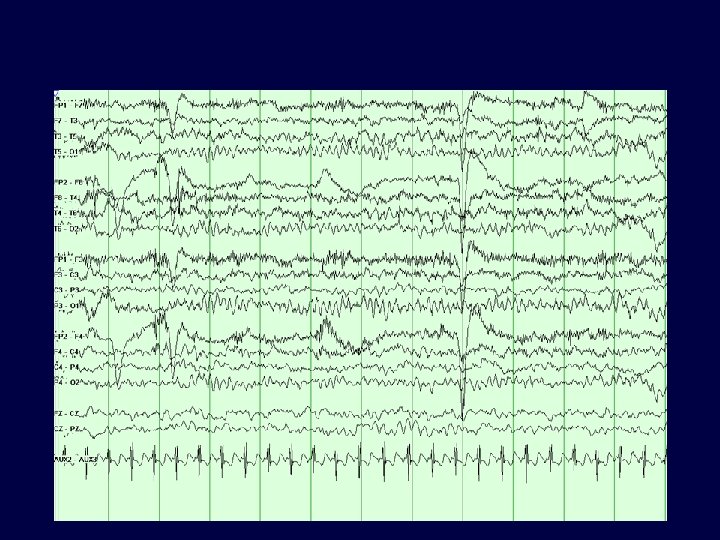
31

Video-EEG Monitoring • Long term inpatient monitoring allows for recording of seizure events. • Clinical and electroencephalographic features can be reviewed aiding in seizure characterization and localization. • Baseline EEG may be helpful in determining risk of future seizures.

Inpatient Video-EEG 33
Outpatient Ambulatory Video. EEG 34

Brain MRI • Provides a structural assessment of the brain. • We look for developmental abnormalities, strokes, tumors or scar tissue that could be focus for electrical irritation that could cause a seizure.
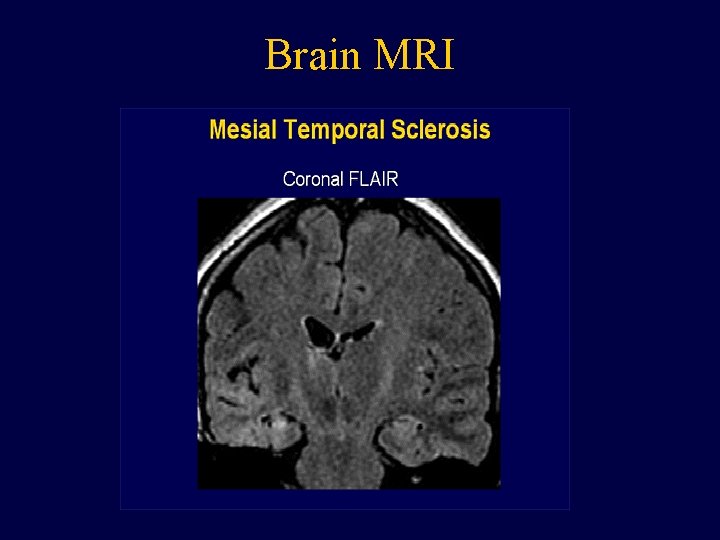
Brain MRI

Recognizing Types of Seizures 37

Seizure Classification • Two major categories: – Generalized – Partial 38
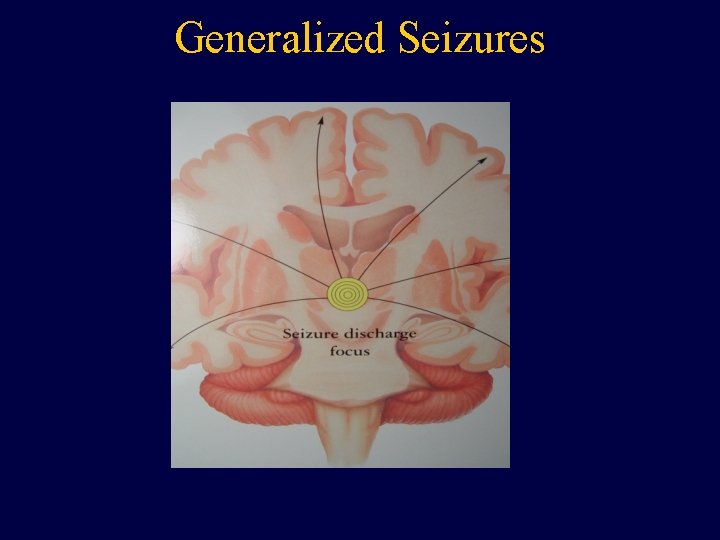
Generalized Seizures
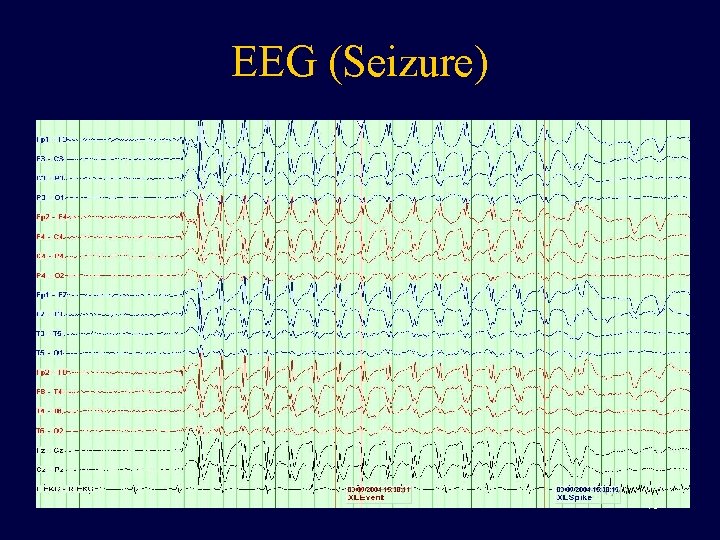
EEG (Seizure) 40

Seizure Classification • Generalized Seizures Tonic/Clonic Absence Myoclonic Atonic Tonic

Generalized Seizures Tonic/Clonic • Electrically the entire brain is affected all at once. • Patients loses consciousness at the onset of the seizure. • Stiffening (tonic) and rhythmic jerking movements (clonic) follow. • Cyanosis, tongue biting and loss of bladder control are common.

Generalized Seizures Absence • Results in a brief period of staring (5 -10 sec). • Patient is usually unaware of his surroundings. • Sometimes accompanied by eye blinking or chewing movements. • Prompt recovery. • Commonly seen in childhood and may be mistaken for day-dreaming.

Generalized Seizures Other Less Frequent • Myoclonic seizure: Brief jerk like contractions which can be localized or generalized. • Atonic seizure: Drop attacks 44
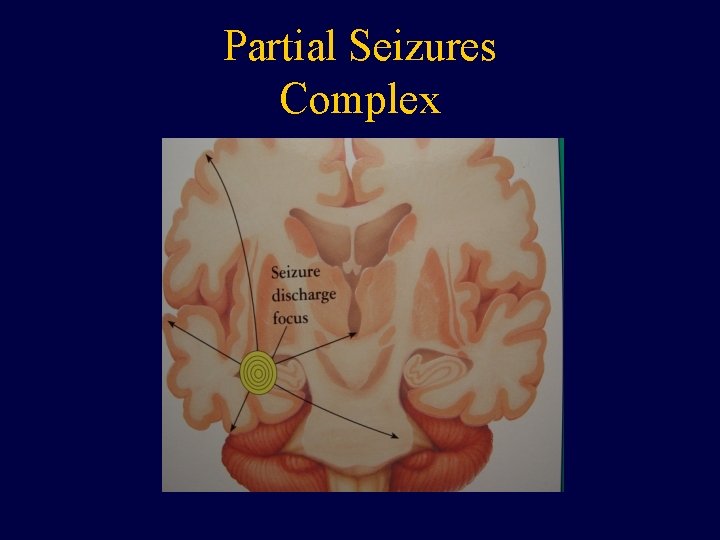
Partial Seizures Complex

Partial Seizures • Seizures originate from a specific (focal) region of the brain. Depending on what area of the brain is stimulated a variety of clinical presentations can occur. • Seizures are often stereotypic to the patient. • Examples include changes in awareness, sensation, rhythmic jerking or stiffening of a specific limb, visual hallucinations.

Partial Seizures • Can progress to a Generalized Tonic/Clonic seizure ‘Secondary Generalization’. • Often associated with aura. • Often associated with automatisms (coordinated involuntary, non-purposeful movements). Examples would include lip smacking, picking, rubbing etc. 48

Partial Seizures • Two Types: Simple and Complex • Simple Partial: No impairment of consciousness. • Complex Partial: Impairment of consciousness.
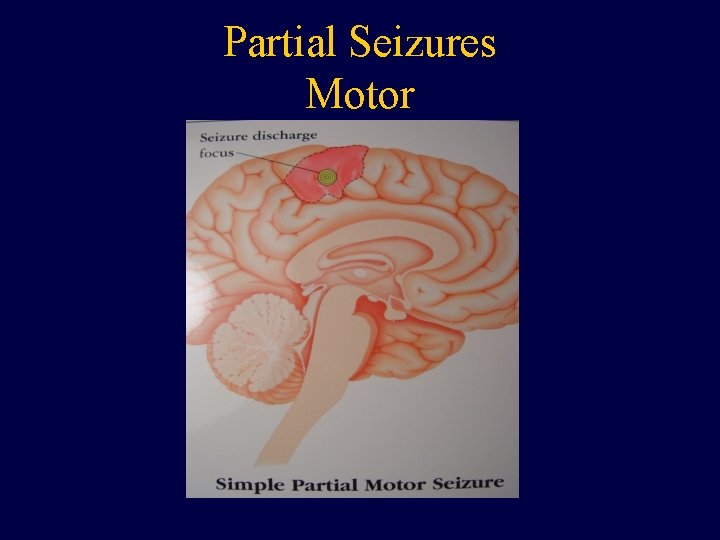
Partial Seizures Motor
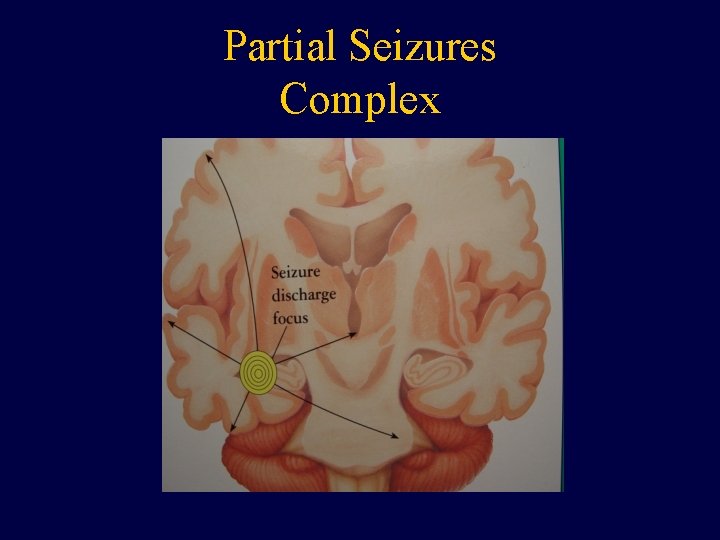
Partial Seizures Complex

Generalized vs Partial Seizures • Sudden onset with no warning/aura • Symmetrical movements • Loss of consciousness • May begin with aura (subjective symptoms experienced by the patient) • Asymmetric or focal motor movements • Alteration of awareness. 52

Imitators of Epilepsy 53

Differential Diagnosis • Seizures can produce sudden neurologic symptoms. • Many diseases can produce sudden neurologic symptoms. • ** Many neurologic diseases can be mistaken for epilepsy and vice-versa. 54

Differential Diagnosis • Non-Epileptogenic events can be secondary to organic or psychogenic etiologies 55

Differential Diagnosis • How do we differentiate between events that are seizure related and those that are caused by a non-epileptic medical or psychiatric condition? • ** Capturing an episode on EEG and demonstrating abnormal electrical activity during the event. 56

Differential Diagnosis • In general episodes stemming from nonepileptic neurologic issues are NOT associated with EEG changes. • Caveats – Some partial seizures can remain electrical silent (i. e. not obvious on EEG). – Some neurologic diseases can cause changes on the EEG (Migraine, Syncope) 57

Seizure Imitators Loss of Consciousness • • • Cardiac (heart failure, heart attack, arrhythmias) Hypoglycemia (fasting, excess insulin) Hypovolemia (dehydration) Hypoxia (lung disease) Panic attack (vasovagal response) Syncope (orthostatic) 58

Syncope • Decreased delivery of oxygenated blood to the brain resulting in loss of consciousness. – Very common with many etiologies – Sudden and unpredictable – Recurrent – Stereotypic – Premonitory symptoms (nausea, sweating) – ‘Convulsive’-type movements 59

Syncope Work-Up • Video-EEG monitoring – Ictal (during event) – Inter-Ictal (between episodes) • EKG/ Holter Monitor • Carotid Ultrasound • Tilt Table Testing 60

Seizure Imitators Confusion • Cerebrovascular (TIA, Stroke, TGA) • Endocrine (Hypo/Hyperglycemia, Thyroid Disease) • Migraine Headaches (complicated) • Metabolic (hepatic or renal encephalopathy 61

Seizure Imitators Motoric or Behavioral Change • Movement Disorders (Tics, Tremors, RLS) • Panic Attacks • Sleep Disorders (Night terrors/ Sleep walking, Benign myoclonus, Sleep apnea) • Psychogenic Non-Epileptic Seizures (PNES) 62

Psychogenic Non-epileptic Seizures • Resemble epileptic seizures but lack EEG correlate. • Can mimic any type of epileptic seizures. • Very common (~25% of patients referred to Video-EEG monitoring for evaluation of intractable epilepsy). 63

Psychogenic Non-epileptic Seizures • Psychiatric manifestation – Somatoform/Conversion Disorder (most common) • Unconscious production of physical symptoms due to psychological factors. A psychological defense mechanism to keep internal stress out of conscious awareness. – Factitious Disorder • Consciously determined symptoms driven by a powerful unconsciously determined need. – Malingering • Willful production of symptoms for a specific external 64 incentive.

Psychogenic Non-epileptic Seizures • Often difficult to distinguish clinically from epileptic seizures. • Clues: – Resistance to AEDs – Emotional Triggers (stress) – Bilateral clonic movements without loss of consciousness – Absence of post-event confusion/lethargy. • Video-EEG is very helpful in diagnosis. 65

Psychogenic Non-epileptic Seizures • Many clinical patterns: – Migratory motor activity (most common) – Generalized motor activity – Unilateral (less common) – Alteration of awareness (Common) ** Can be difficult to distinguish from frontal lobe seizures. 66

Psychogenic Non-epileptic Seizures • Characteristics of PNES – Variable responsiveness or preserved awareness. – Out of phase movements of extremities. – Discontinuous motor activity – Pelvic thrusting. – Side to side head movements. – Eye closure/eye flutter 67

Psychogenic Non-epileptic Seizures • Characteristics of PNES – Varied character of events – Suggestibility – Emotional triggers – Prompt recovery (Absence of post-ictal state) – Poor response to anti-epileptic medications 68

Psychogenic Non-epileptic Seizures • Although such findings as urinary incontinence, tongue biting and injuries are often attributed to epileptic seizures they can also be seen in PNES. 69

Psychogenic Non-epileptic Seizures • ~20 % of patients with PNES will also have coexistent epileptic seizures. • Latency between manifestation of PNES and diagnosis is ~ 7 years. • Prompt diagnosis is crucial to avoid iatrogenic morbidity (Exposure to unnecessary medication ~80%, Intubation ~50%). 70
- Slides: 70