Normal Heart VT Syndromes Long QT Short QT




























- Slides: 50

Normal Heart VT

Syndromes • • Long QT Short QT Brugada Catecholaminergic Polymorphic VT-CPVT Idiopathic VF Short coupled Td. P Lev-Lenegre Syndrome

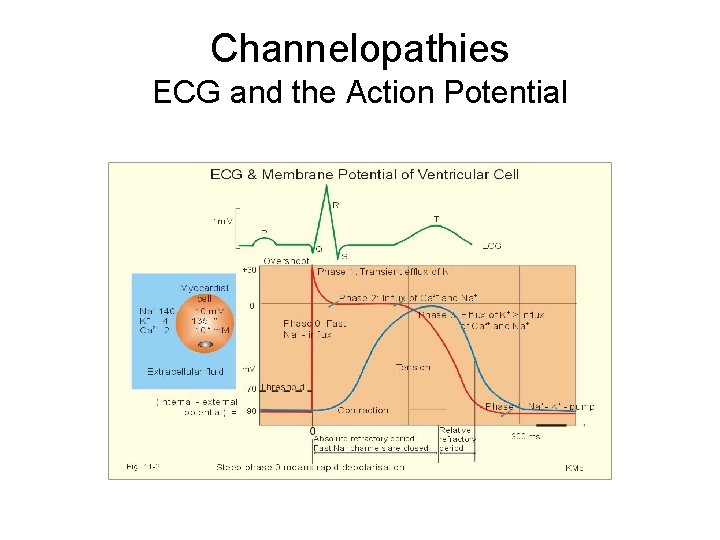
Channelopathies ECG and the Action Potential

Case 1 • 13 yo girl presents with syncope while swimming – QTc ≥ 500 msec – ß-blocker initiated with no further events – Presents five years later inquiring about stopping medications • Do you stop ß-blocker? • Is an ICD indicated?

Long QT Syndrome History • • 1957 1963 -1964 1958 -1970 1971 • 1979 • 1991 -2007 • • 1 st LQTS family reported Romano-Ward Syndrome 25 LQTS cases reported 1 st treatment – left stellate ganglionectomy • LQTS registry started • 10 LQTS genes identified

Long QT Syndrome Overview • Incidence: 1/7, 000 • Presentation: mean age 8 -14 years • Symptoms: – Syncope, palpitations, seizures, sudden death – Syncope in pediatric population should be considered malignant until proven otherwise • Arrhythmia: Torsades pointes

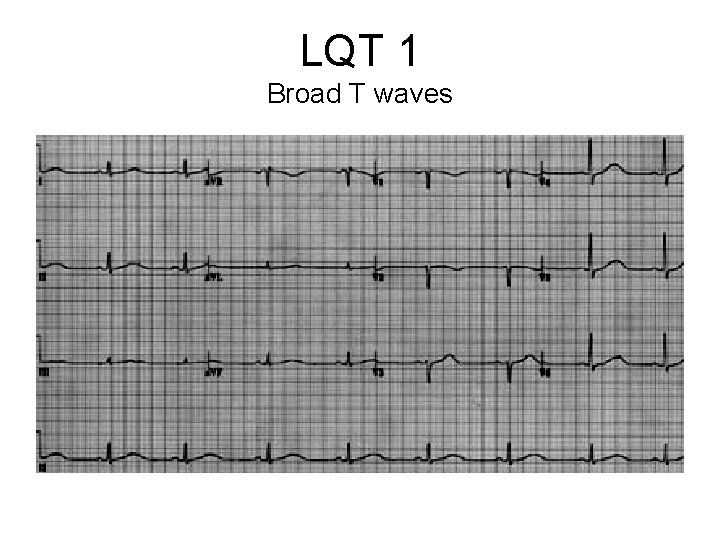
LQT 1 Broad T waves

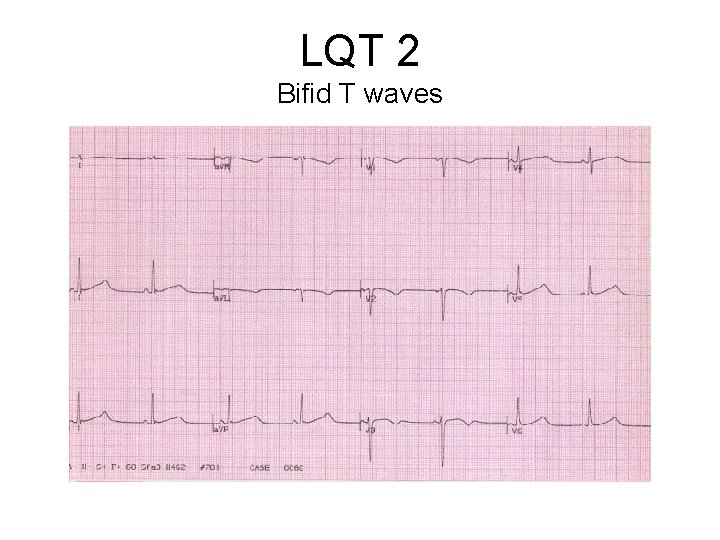
LQT 2 Bifid T waves

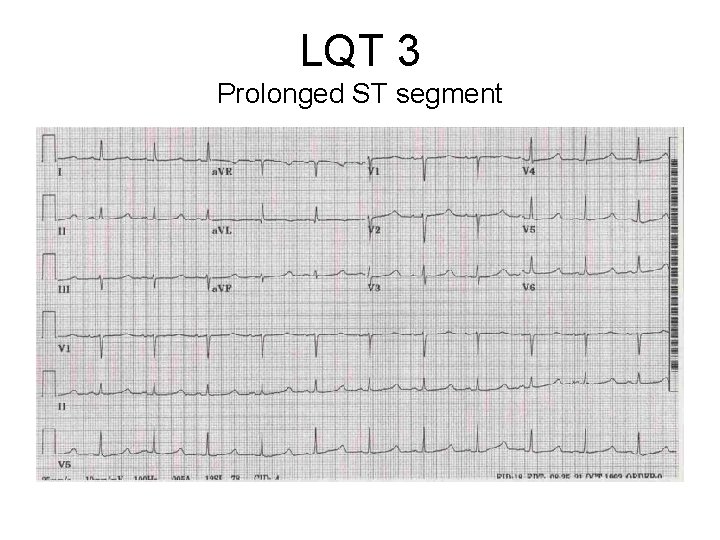
LQT 3 Prolonged ST segment

Long QT Syndrome Diagnosis • ECG definition – QTc > 460 females – QTc > 450 males • Challenges – 25 to 50% of LQT 1, 2, & 3 individuals will have QTc ≤ 460 msec – Genetic testing has 3 to 5% false (+) rate • Epinepherine challenge – Useful in evaluating LQT 1 (∆QT 30 msec) • Iks response to epinepherine in LQT 1 impaired • NPV 93%, PPV 76%, Sens 92%, Spec 86% • Less useful when on beta-blockers

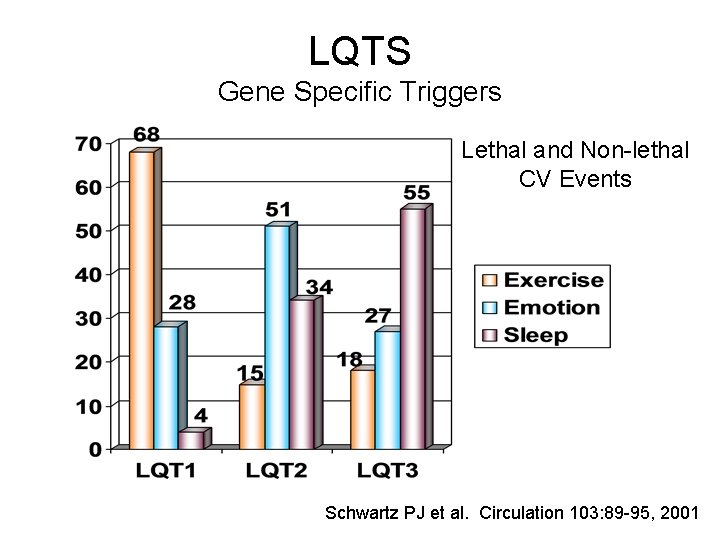
LQTS Gene Specific Triggers Lethal and Non-lethal CV Events Schwartz PJ et al. Circulation 103: 89 -95, 2001

Long QT Syndrome High Risk Features • Aborted cardiac arrest • Family history (< 50 y) of cardiac arrest or unexplained syncope • History of “seizures” or congenital deafness • Prolonged QTc ≥ 500 msec on ECG • Positive genetic test

LQTS Risk of Cardiac Event (syncope, cardiac arrest, or sudden death) • Risk > 50% – QTc ≥ 500 msec: LQT 1, LQT 2, Male LQT 3 • Risk 30 -50% – QTc ≥ 500 msec: Female LQT 3 – QTc < 500 msec: Female LQT 2/3, Male LQT 3 • Risk < 30% – QTc < 500 msec: LQT 1, Male LQT 2

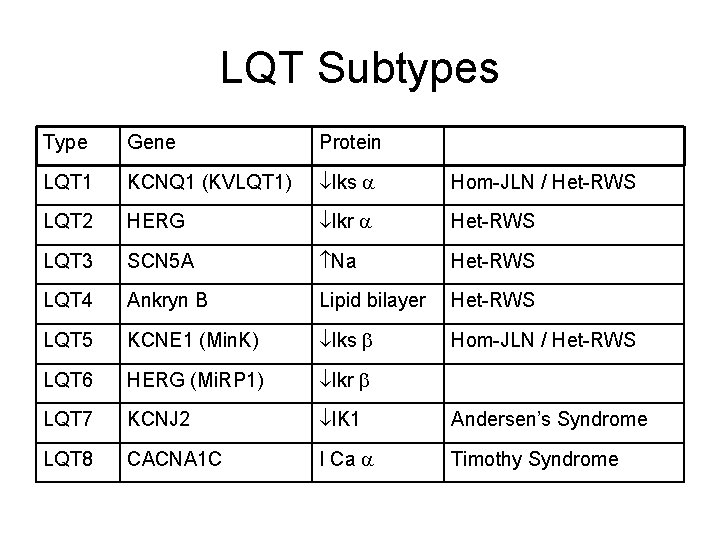
LQT Subtypes Type Gene Protein LQT 1 KCNQ 1 (KVLQT 1) Iks Hom-JLN / Het-RWS LQT 2 HERG Ikr Het-RWS LQT 3 SCN 5 A Na Het-RWS LQT 4 Ankryn B Lipid bilayer Het-RWS LQT 5 KCNE 1 (Min. K) Iks Hom-JLN / Het-RWS LQT 6 HERG (Mi. RP 1) Ikr LQT 7 KCNJ 2 IK 1 Andersen’s Syndrome LQT 8 CACNA 1 C I Ca Timothy Syndrome

LQTS Management Options • Lifestyle modification (IB) • Beta-blockers (IB) – Very effective LQT 1, Moderate LQT 2 – Minimal effect LQT 3 • ICD plus BB – Cardiac arrest (IA) – Syncope / VT (IB) – Prophylactic in LQT 2 or LQT 3 (IIB) • Left stellate ganglionectomy (IIB)

LQT Resources • Cardiac Arrhythmias Research & Education (CARE) – www. longqt. org • Cardiac Arrest Survivors Network (CASN) – www. casn-network. org • International Registry for Drug Induced Arrhythmias – www. qtdrugs. com

Case 1 Review • 13 yo girl with syncope during swimming and QTc ≥ 500 msec – – Asymptomatic for 5 y on BB Swimming…suggests LQT 1 High risk subgroup based LQT 1 and QTc ≥ 500 msec Recommendation • Continue BB given very effective in LQT 1 • Consider ICD if has arrest, syncope, or VT

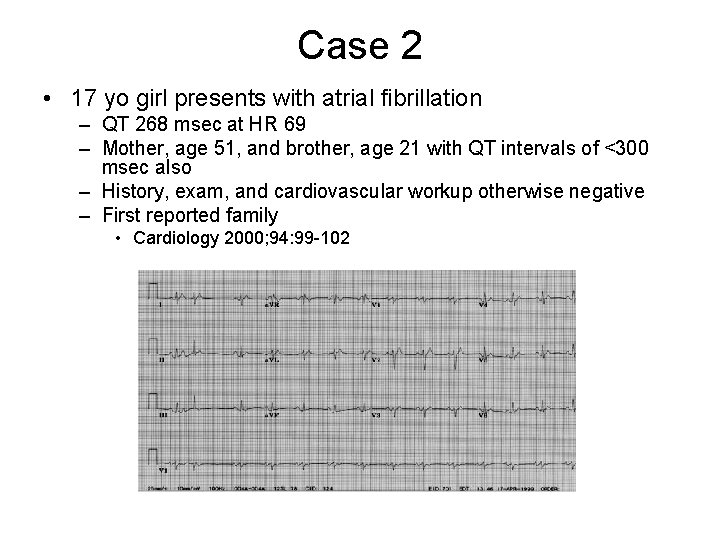
Case 2 • 17 yo girl presents with atrial fibrillation – QT 268 msec at HR 69 – Mother, age 51, and brother, age 21 with QT intervals of <300 msec also – History, exam, and cardiovascular workup otherwise negative – First reported family • Cardiology 2000; 94: 99 -102

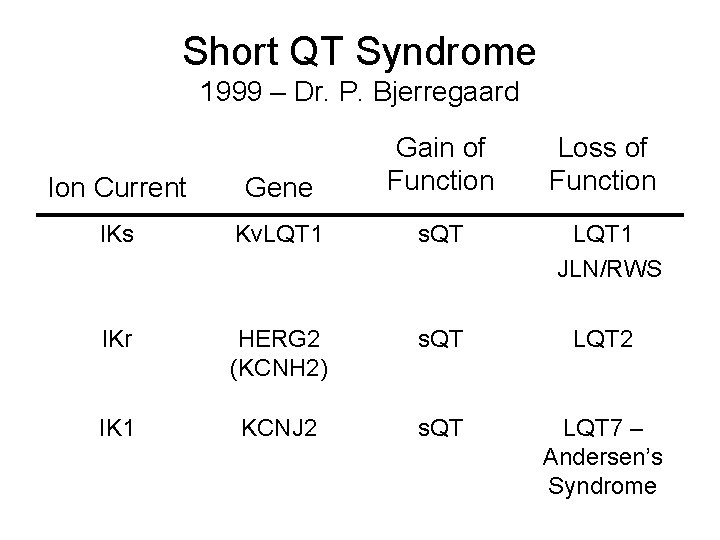
Short QT Syndrome 1999 – Dr. P. Bjerregaard Ion Current Gene Gain of Function Loss of Function IKs Kv. LQT 1 s. QT LQT 1 JLN/RWS IKr HERG 2 (KCNH 2) s. QT LQT 2 IK 1 KCNJ 2 s. QT LQT 7 – Andersen’s Syndrome

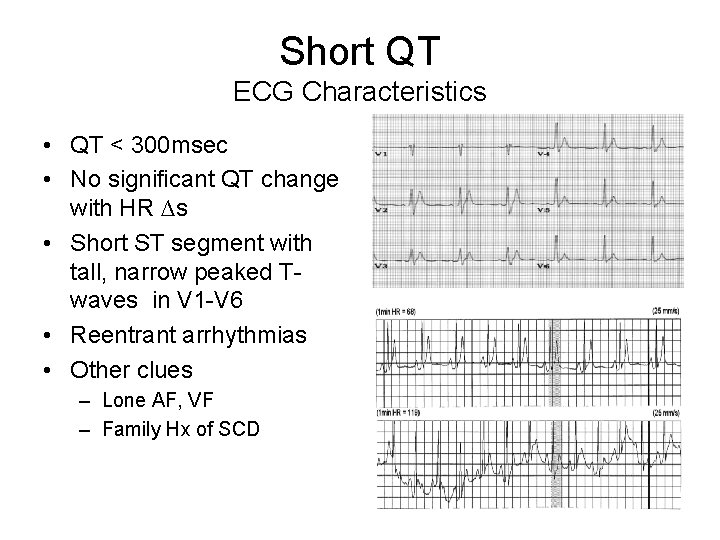
Short QT ECG Characteristics • QT < 300 msec • No significant QT change with HR ∆s • Short ST segment with tall, narrow peaked Twaves in V 1 -V 6 • Reentrant arrhythmias • Other clues – Lone AF, VF – Family Hx of SCD

Short QT • EP testing – Short atrial and ventricular refractory periods • Management – Pharmacological (small studies) • Only hydroquinidine effective in increasing QT • Fleicanide, sotalol, ibutilide ineffective – ICD experience (limited) • T wave oversensing/inappropriate shocks • Device selection (St. Jude – delay/decay)

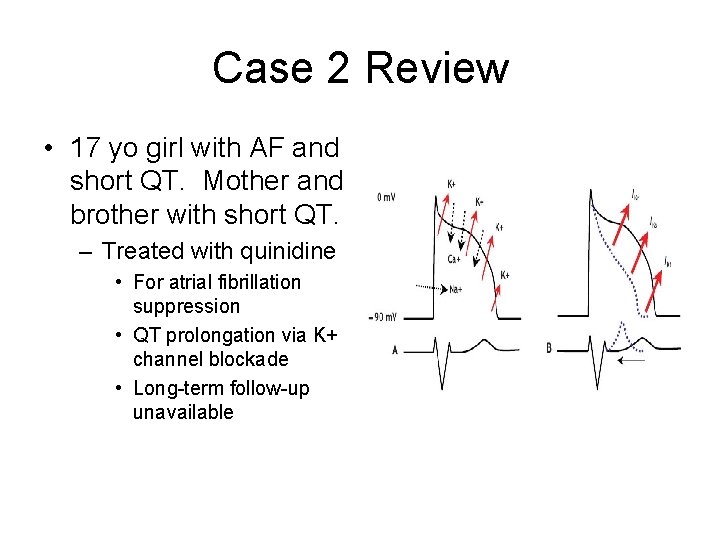
Case 2 Review • 17 yo girl with AF and short QT. Mother and brother with short QT. – Treated with quinidine • For atrial fibrillation suppression • QT prolongation via K+ channel blockade • Long-term follow-up unavailable

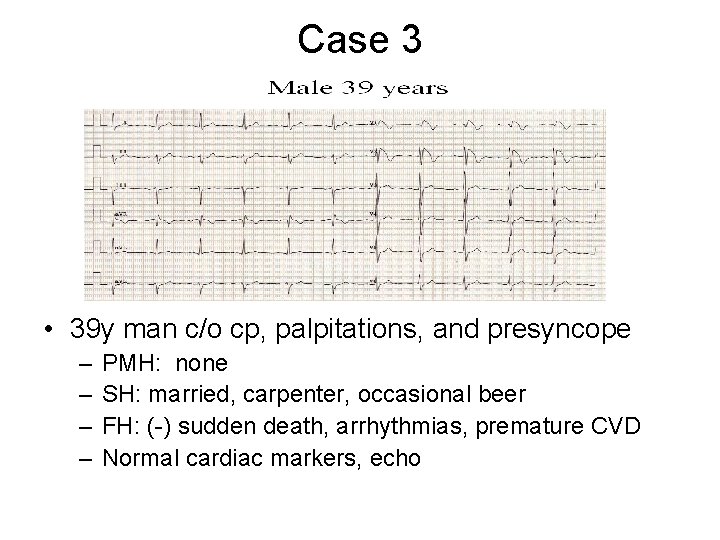
Case 3 • 39 y man c/o cp, palpitations, and presyncope – – PMH: none SH: married, carpenter, occasional beer FH: (-) sudden death, arrhythmias, premature CVD Normal cardiac markers, echo

Brugada Syndrome Overview • • • Identified 1992 Age spectrum - 2 d to 84 y Mean age sudden death 40 ± 15 y Men > 5 x risk of arrhythmic events Prevalence – 5/10, 000 - overall – #2 cause of death SE Asian men <40 y • Dynamic but characteristic ECG changes • 1 in 5 have Na channel mutation (SCN 5 A)

Brugada Syndrome Definition • Type 1 pattern ECG in V 1 -V 3 plus 1 of following: – Pharm conversion to Type 1 from Type 2/3 ECG • Na channel blocker (procainamide, fleicanide, ajmaline) – – – Documented VF/polymorphic VT Family history of SCD < 45 y Inducible VT at EP study Syncope Nocturnal agonal respirations • ECG pattern only = Brugada pattern ECG but not Brugada Syndrome • Exclude other heart conditions

Brugada pattern ECG ST elevation V 1 -V 3 • Type 1 (DIAGNOSTIC) – Coved ST elevation ≥ 2 mm with negative T wave – sensitivity by moving V 2/V 3 from 4 th to 2 nd/3 rd intercostal space • Type 2 – Saddleback ST elevation ≥ 2 mm w/ ST trough ≥ 1 mm – Positive/biphasic T wave • Type 3 – Coved/saddle ST elevation ≥ 2 mm w/ ST trough < 1 mm • Also reported in inferior leads and left precordial leads – Some individuals also had SCN 5 A mutation

Brugada Syndrome • Other conduction abnormalities – QT prolongation (R > L precordial) • Prolonged action potential duration in RV epicardium – P, PR, & QRS • PR prolongation associated with Hispurkinje delay • Utility of EP study – Controversial – 6 -9% of healthy individuals of induced VF at EPS – Brugada, +EPS associated w/ 8 x risk

Brugada Consensus Conference Spontaneous Type 1 ECG

Brugada Consensus Conference Sodium Channel Blocker Induced Type 1 ECG

Case 3 Review • 39 y man c/o cp, palpitations, and presyncope – – Spontaneous type 1 ECG “Asymptomatic” Negative family hx EP study (IIA indication) • Sustained VT with DES at 500 from RVA • No supraventricular arrhythmias induced • Normal AV node and His-Purkinje function – ICD was implanted (IIA indication) • Asymptomatic without events at 32 mo f/u • ** Most events occur at night - autonomic role? – Other tx options: ablation, quinidine

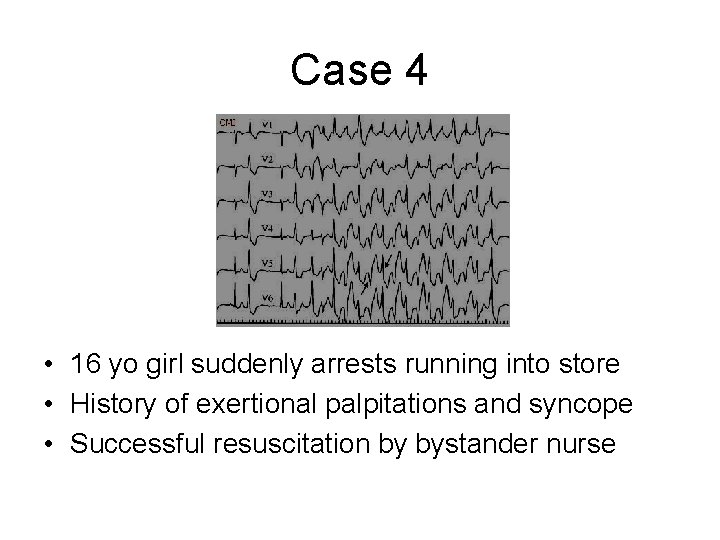
Case 4 • 16 yo girl suddenly arrests running into store • History of exertional palpitations and syncope • Successful resuscitation by bystander nurse

Catecholaminergic Polymorphic Ventricular Tachycardia (CPVT) • Clinical Features – Direct correlation with adrenergic stimulation (physical/emotional) • Threshold heart rate 120 -130 bpm • Abnormal automaticity or triggered activity – Bidirectional VT – Symptom onset in childhood – Genetic mutations – Ryanodine / Calsequestrin

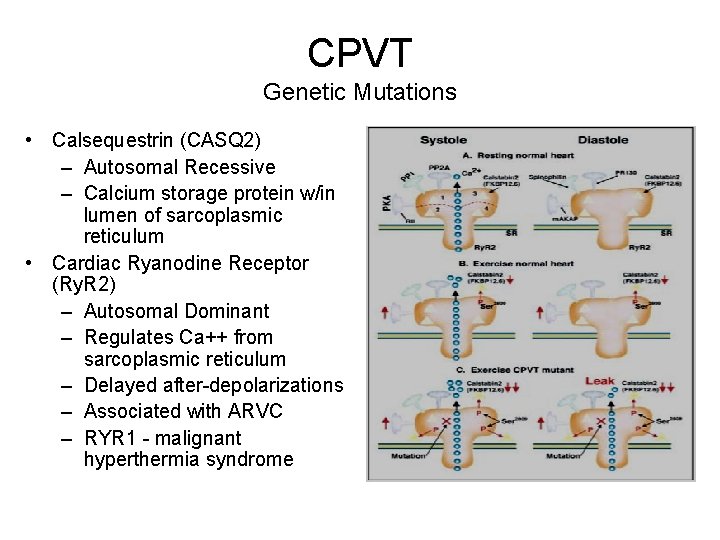
CPVT Genetic Mutations • Calsequestrin (CASQ 2) – Autosomal Recessive – Calcium storage protein w/in lumen of sarcoplasmic reticulum • Cardiac Ryanodine Receptor (Ry. R 2) – Autosomal Dominant – Regulates Ca++ from sarcoplasmic reticulum – Delayed after-depolarizations – Associated with ARVC – RYR 1 - malignant hyperthermia syndrome

CPVT Management • Anti-adrenergic treatment – Beta blockers are the mainstay of treatment • ICDs – B-blockers not always effective

Case 4 Review • 16 yo with history of palpitations and syncope who collapses in store – Arrested 3 times en route to hospital – ICD implanted and atenolol started • 3 ICD revision procedures • 2 lead dislodgements resulting in inappropriate ICD therapies

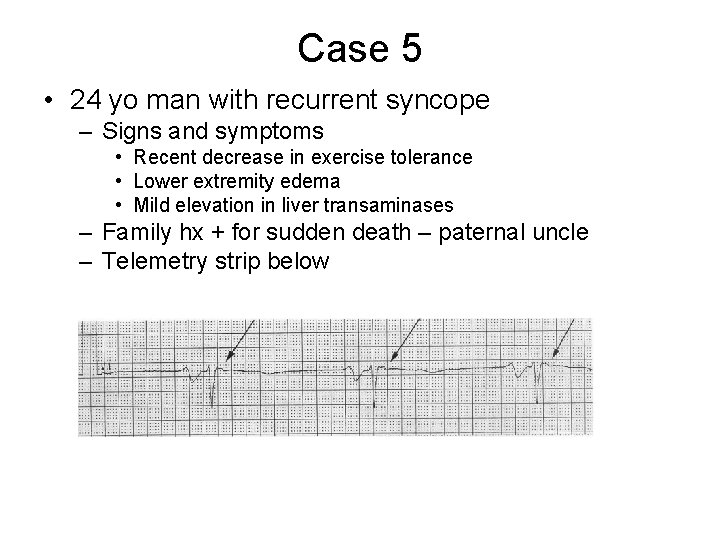
Case 5 • 24 yo man with recurrent syncope – Signs and symptoms • Recent decrease in exercise tolerance • Lower extremity edema • Mild elevation in liver transaminases – Family hx + for sudden death – paternal uncle – Telemetry strip below

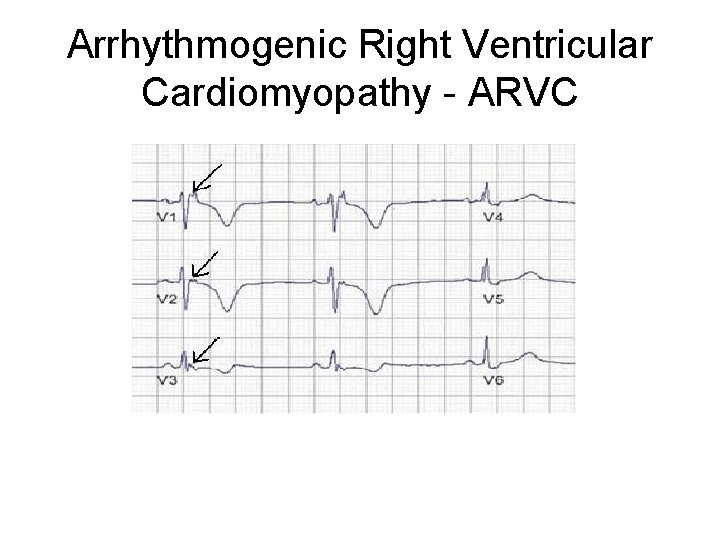
Arrhythmogenic Right Ventricular Cardiomyopathy - ARVC

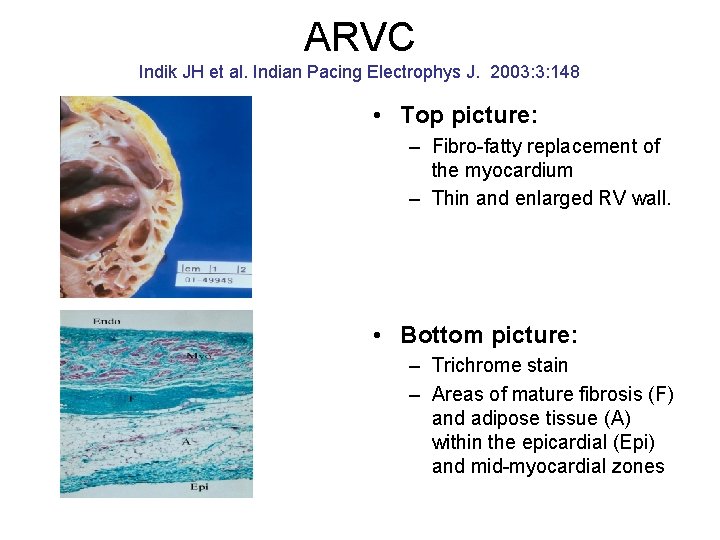
ARVC Indik JH et al. Indian Pacing Electrophys J. 2003: 3: 148 • Top picture: – Fibro-fatty replacement of the myocardium – Thin and enlarged RV wall. • Bottom picture: – Trichrome stain – Areas of mature fibrosis (F) and adipose tissue (A) within the epicardial (Epi) and mid-myocardial zones

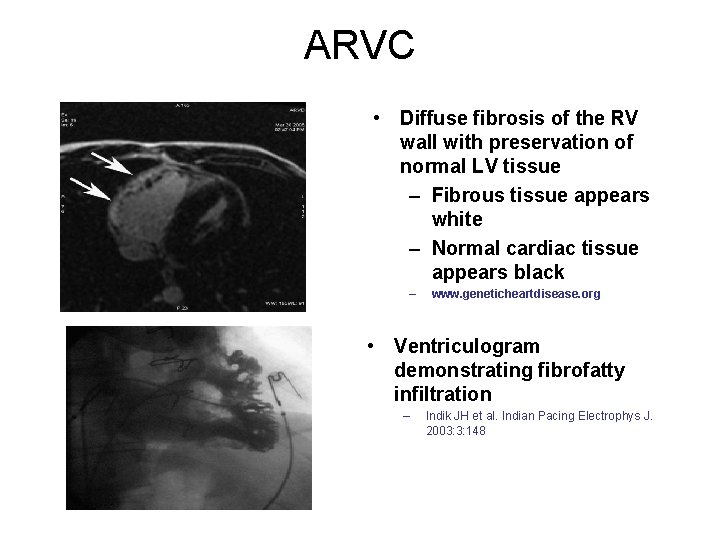
ARVC • Diffuse fibrosis of the RV wall with preservation of normal LV tissue – Fibrous tissue appears white – Normal cardiac tissue appears black – www. geneticheartdisease. org • Ventriculogram demonstrating fibrofatty infiltration – Indik JH et al. Indian Pacing Electrophys J. 2003: 3: 148

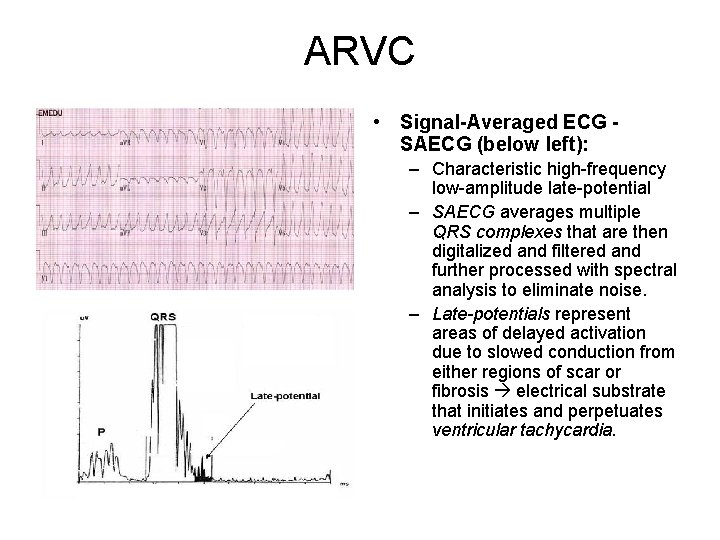
ARVC • Signal-Averaged ECG SAECG (below left): – Characteristic high-frequency low-amplitude late-potential – SAECG averages multiple QRS complexes that are then digitalized and filtered and further processed with spectral analysis to eliminate noise. – Late-potentials represent areas of delayed activation due to slowed conduction from either regions of scar or fibrosis electrical substrate that initiates and perpetuates ventricular tachycardia.

ARVC High Risk Features • • • Younger patients Recurrent syncope History of cardiac arrest or sustained VT Clinical signs of RV failure or LV involvement Patients with or having a family member with the high risk ARVD gene (ARVD 2) • Increase in QRS dispersion ≥ 40 msec – QRS dispersion = max measured QRS minus min measured QRS • Naxos disease

Case 5 Review • Diagnosis – Rhythm strip and ECG notable for epsilon waves and T wave inversion in right precordial leads • Risk – High risk features present – young age, recurrent syncope, signs of RV failure, family history of sudden cardiac arrest • Management – ICD implantation

• Idiopathic Ventricular Fibrillation – Sodium channel mutation • Short-coupled Torsades Pointes – Normal QT interval with coupling interval of 1 st ectopic beat < 300 msec – Prognosis poor with unproven tx (BB or CCB); ablation? • Lev-Lenegre Syndrome – Progressive cardiac conduction defect associated with bradyarrhythmias although tachyarrhythmias may also occur – Sodium channel defect

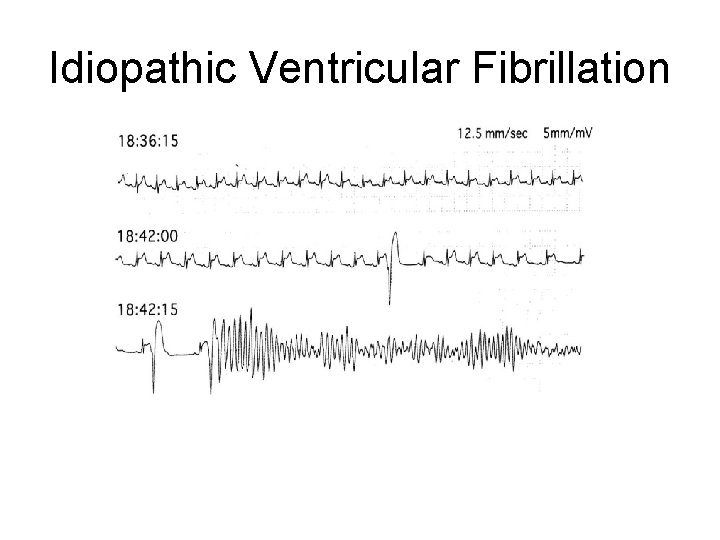
Idiopathic Ventricular Fibrillation

Lev-Lenegre Syndrome • Progressive Cardiac Conduction Defect – Acquired complete heart block – Idiopathic fibrosis and calcification of cardiac conduction system • Very rare • Sodium channel mutations (subtype-SCN 5 A) • Often result in bradyarrhythmias although tachyarrhythmias may also result • • Lev M. Anatomic basis for atrioventricular block. Am J Med 1964; 37: 742 -8. Lenegre J. Etiology and pathology of bilateral bundle branch block in relation to complete heart block. Prog Cardiovasc Dis 1964; 6: 409 -444

Hypertrophic Cardiomyopathy • #1 cause of SCA in athletes – > 1/3 of deaths – Often associated with physical activity – 60% high school age – >90% males • Genetic disorder left ventricular hypertrophy • First symptom often sudden death

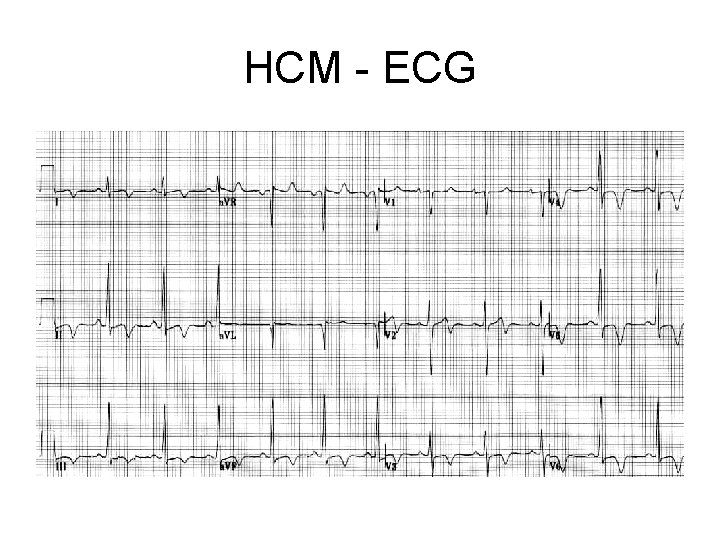
HCM - ECG

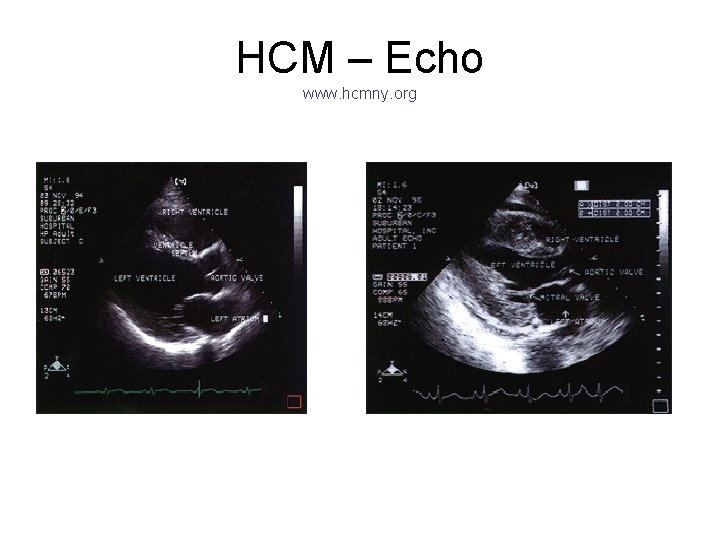
HCM – Echo www. hcmny. org

HCM vs. Athletic Heart • HCM – Septum > 15 mm – Assymetrical (septum: posterior wall thickness > 1. 5: 1) – Occasional family history – No change with deconditioning • Athletic Heart – – Septum < 15 mm Symmetrical thickening No family history Resolves with deconditioning – 3 mo

Thank You Questions?