Normal Bacterial Flora Host Defense Mechanisms Nonspecific Immunity
















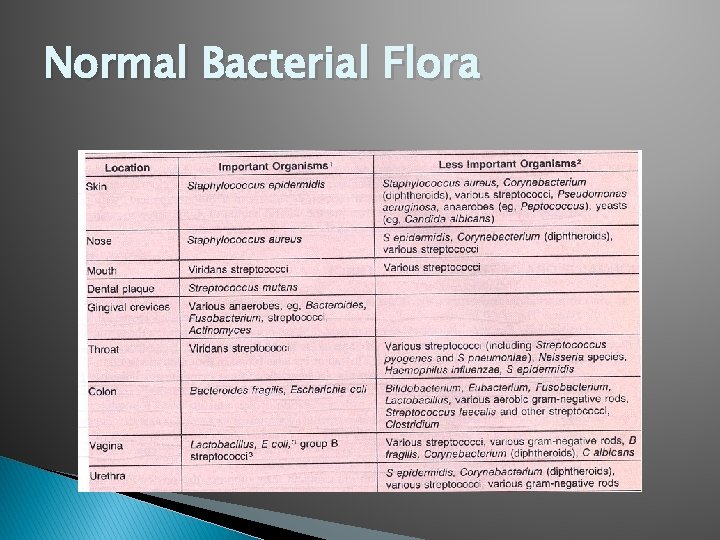
Normal Bacterial Flora

Host Defense Mechanisms � Nonspecific Immunity ◦ barriers ◦ inflammatory response � Specific ◦ Passive ◦ Active Immunity �humoral �cell-mediated

Clinical Microbiology � Gram Positive Cocci � Gram Positive Bacilli � Gram Negative Cocci � Gram Negative Bacilli � Anaerobes � Spirochetes � Mycobacteria

Gram Positive Cocci � Staphylococcus � Streptococcus

Staphylococcus � S. aureus, S. epidermidis, S. saprophyticus � S. aureus

Streptococcus � S. viridans ◦ oral flora ◦ infective endocarditis

S. pyogenes � Group A, beta hemolytic strep � pharyngitis, cellulitis � rheumatic fever �migrating polyarthritis �carditis �immunologic cross reactivity � acute glomerulonephritis �edema, hypertension, hematuria �antigen-antibody complex deposition
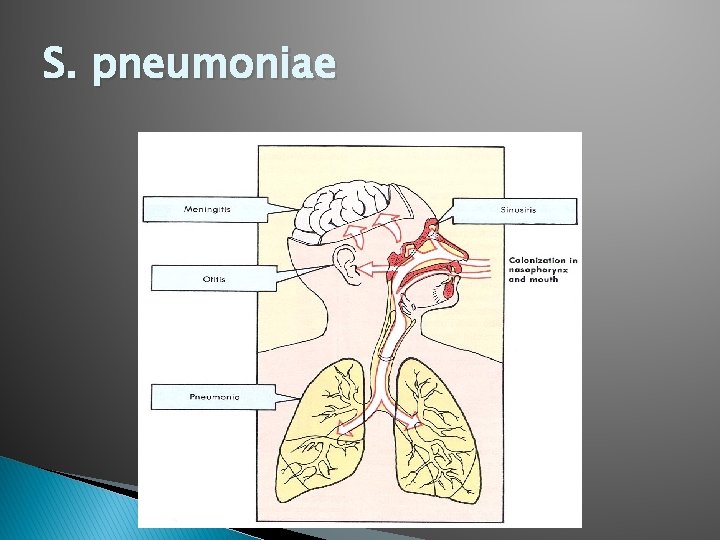
S. pneumoniae

Gram Negative Cocci � Neisseria ◦ meningitidis ◦ gonorrhea � Moraxella catarrhalis

Gram Positive Bacilli � Clostridium Bacillus � Corynebacterium � Listeria � Actinomyces � Nocardia �
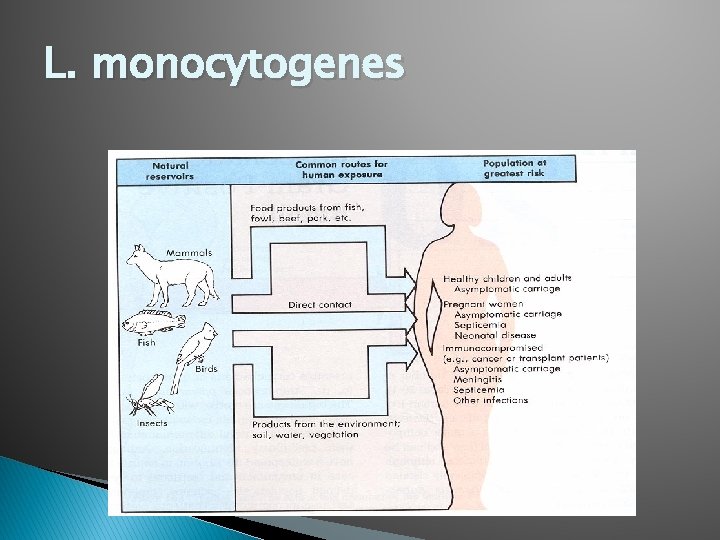
L. monocytogenes
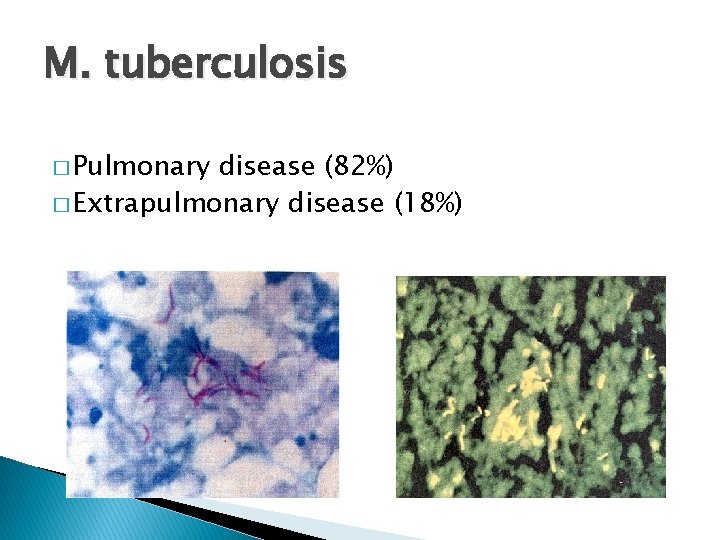
M. tuberculosis � Pulmonary disease (82%) � Extrapulmonary disease (18%)
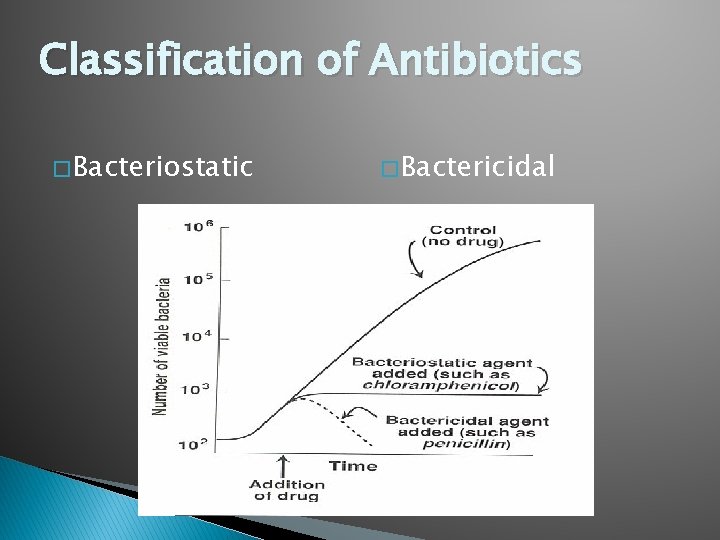
Classification of Antibiotics � Bacteriostatic � Bactericidal

Classification of Antibiotics � Chemical Structure � Spectrum of Activity � Mechanism of Action
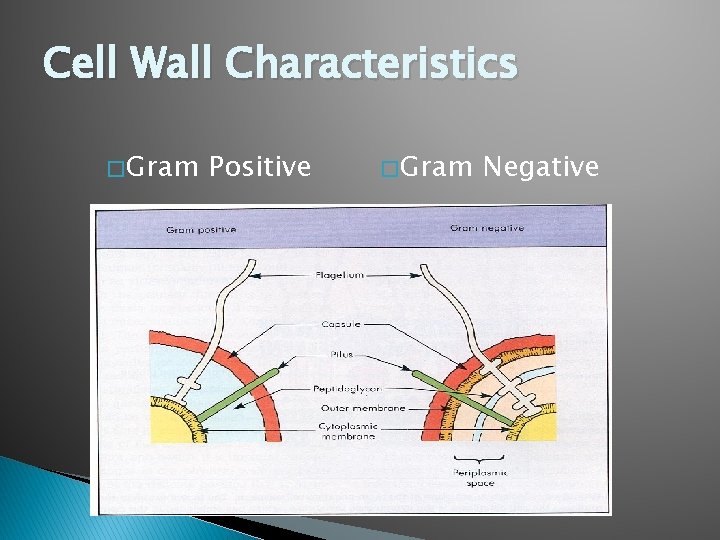
Cell Wall Characteristics � Gram Positive � Gram Negative

Mechanism of Action

Inhibitors of Cell Wall Synthesis

Beta Lactam Antibiotics � Penicillins � Cephalosporins � Carbapenems � Monobactams

Penicllins � Derived from the fungus Penicillium � Therapeutic concentration in most tissues � Poor CSF penetration � Renal excretion � Side effects: hypersensitivity, nephritis, neruotoxicity, platelet dysfunction

Natural Penicillins � Penicillin G, Penicillin V

Antistaphylococcal Penicillins � Methicillin � Nafcillin � Oxacillin � Dicloxacillin

Aminopenicillins � Amoxicillin � Ampicillin +/- clavulanate +/- sulbactam

Antipseudomonal Penicillins � Carbenicillin � Ticarcillin +/- clavulanate � Piperacillin +/- tazobactam



Cephalosporins ◦ Structurally similar to penicillins ◦ Therapeutic concentration in many tissues, 3 rd and 4 th generation into CSF ◦ Renal Excretion ◦ Side Effects �allergy �disulfiram-like effect �anti-Vitamin K

Generations of Cephalosporins

ﺳﻔﺎﻟﻮﺳپﻮﺭﻳﻦ ﻫﺎ : ﻧﺴﻞ ﺍﻭﻝ � cephalotin, cephradin, cephapirin, cephalexin, cephadroxil, cephradin : ﻧﺴﻞ ﺩﻭﻡ � � Cephazolin, � Cephamandol, cefonicid, cefuroxime, cephachlor, ceforoxim axetil, lora carbef,

: ﻧﺴﻞ ﺳﻮﻡ � ceftriaxon, ceftizoxime, cefixim, cefdinir, cefditoren ﺧﻮﺭﺍکی , cefpodoxim ﺧﻮﺭﺍﻛﻲ : ﻧﺴﻞ چﻬﺎﺭﻡ � � Cefoprazon, � Cefepime, cefpirom, cefpiramid
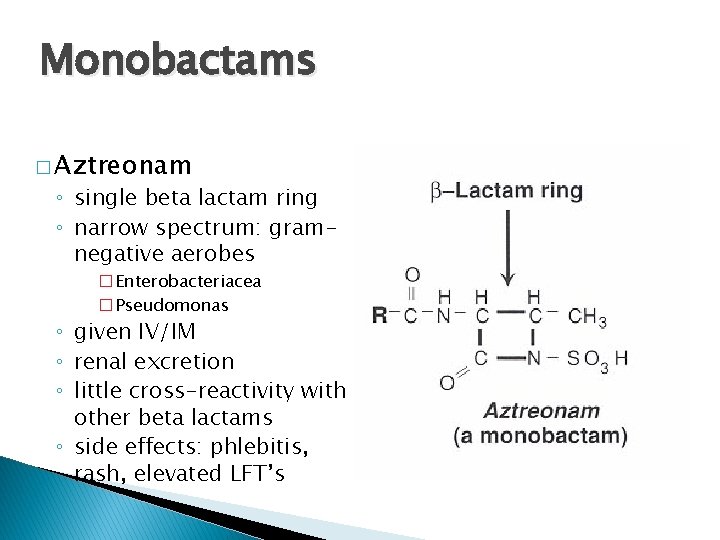
Monobactams � Aztreonam ◦ single beta lactam ring ◦ narrow spectrum: gramnegative aerobes �Enterobacteriacea �Pseudomonas ◦ given IV/IM ◦ renal excretion ◦ little cross-reactivity with other beta lactams ◦ side effects: phlebitis, rash, elevated LFT’s
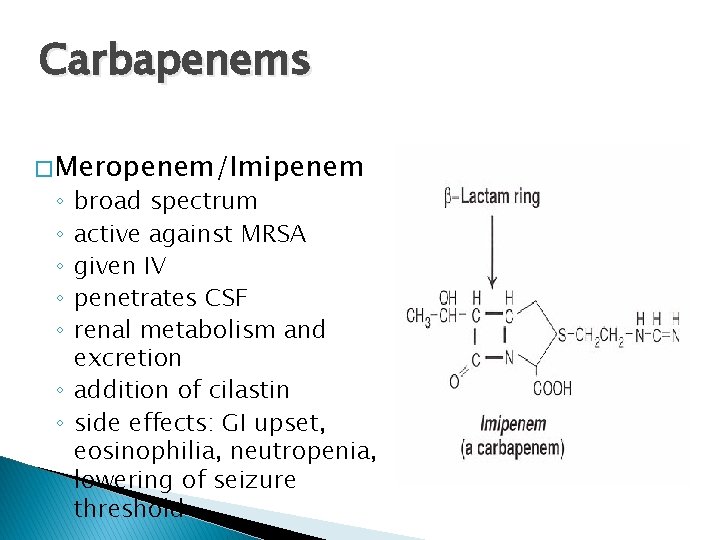
Carbapenems � Meropenem/Imipenem broad spectrum active against MRSA given IV penetrates CSF renal metabolism and excretion ◦ addition of cilastin ◦ side effects: GI upset, eosinophilia, neutropenia, lowering of seizure threshold ◦ ◦ ◦



Adverse Effects of ß-Lactams Penicillin hypersensitivity – 0. 4% to 10 % ◦ Mild: rash ◦ Severe: anaphylaxis & death � There is cross-reactivity among all Penicillins � Penicillins and cephalosporins ~5 -15% � Penicillins and carbapenems~1% (may be higher) ◦ Desensitization is possible for mild hypersensitivity � Aztreonam does not display cross-reactivity with Penicillins and can be used in penicillin-allergic patients




Vancomycin � Tricyclic glycopeptide � Inhibits synthesis of phospholipids and cross -linking of peptidoglycans � Activity against gram-positive organisms � Useful for beta lactam resistant infections � Widely distributed, penetrates CSF � Renal elimination, follows creatinine cl. � Side effects: phlebitis, red man syndrome, ototoxicity, nephrotoxicity


Adverse Effects of Glycopeptides � Oesophageal ulceration � Photosensitivity reaction

Adverse Effects of Vancomycin � Red-Man Syndrome ◦ Erythema multiforme-like reaction with intense pruritus, tachycardia, hypotension, rash involving face, neck, upper trunk, back and upper arms �Related to infusion rate �Resolves spontaneously after discontinuation �Lengthen infusion (over 2 - 3 hr) � Hematological ◦ Neutropaenia ◦ Eosinophilia

Protein Synthesis Inhibitors � Human ◦ 80 S � 40 S � 60 S Ribosome � Bacterial ◦ 70 S � 30 S � 50 S Ribosome

Tetracyclines � Isolated from Streptomyces aureofaciens � Reversibly bind 30 S ribosomal subunit � Penetrate sinus mucosa, saliva and tears � Metabolized in liver-->excreted in bile--> reabsorbed-->eliminated in urine � Side effects: GI upset, hepatotoxicity, photosensitivity, bony deposition � Contraindicated in pregnant or breast feeding women, children under 8 y/o
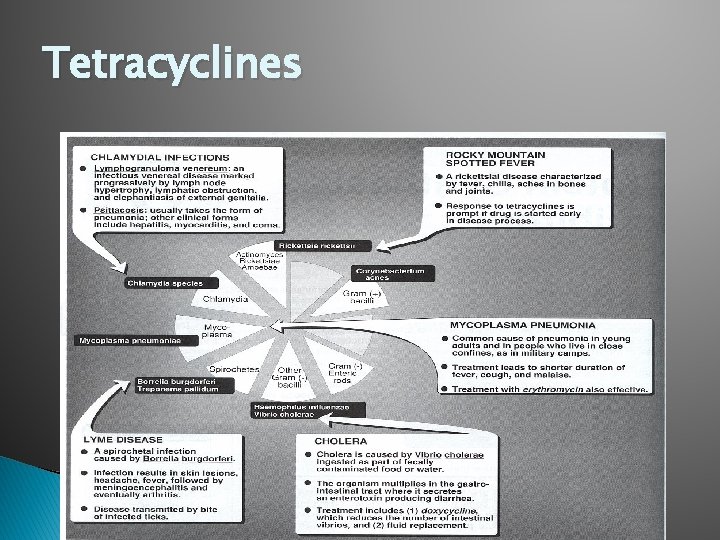
Tetracyclines

Aminoglycosides � Derived from Streptomyces and Micormonospora � Irreversible binding to 30 S subunit � Actively transported into bacterial cells � Variable tissue penetration, unreliable CSF levels � Concentrate within perilymph � Renal elimination � Nephrotoxicity, ototoxicity, neurotoxicity

Aminoglycosides


Adverse Effects of Aminoglycosides � � � Nephrotoxicity ◦ Direct proximal tubular damage - reversible if caught early ◦ Risk factors: High troughs, prolonged duration of therapy, underlying renal dysfunction, concomitant nephrotoxins Ototoxicity ◦ 8 th cranial nerve damage – irreversible vestibular and auditory toxicity �Vestibular: dizziness, vertigo, ataxia �Auditory: tinnitus, decreased hearing ◦ Risk factors: as for nephrotoxicity Neuromuscular paralysis ◦ Can occur after rapid IV infusion especially with; �Myasthenia gravis �Concurrent use of succinylcholine during anaesthesia

Macrolides � Macrocyclic lactone structure � Irreversible binding to 50 S subunit � Therapeutic concentrations in oropharyngeal and respiratory secretions � No CSF penetration � Metabolized in liver, excreted in feces and urine � Side effects: GI upset, ototoxicity, hepatotoxicity

Erythromycin

Alternate Macrolides � Clarithromycin � Azithromycin


Adverse Effects of �Gastrointestinal (up to 33 %) (especially �Erythromycin) • Nausea • Vomiting • Diarrhoea • Dyspepsia � Thrombophlebitis: IV Erythromycin & Azithromycin � QTc prolongation, ventricular arrhythmias � ototoxicity with high dose erythromycin in renal impairment � Haematological changes Eosinophilia Leucocytosis

Chloramphenicol � Isolated from Streptomyces � Reversible binding to 50 S subunit � Broad spectrum of activity � Indicated for severe anaerobic infections or unresponsive life-threatening infections � Widely distributed, enters CSF � Metabolized in liver (inhibits P-450), eliminated in urine � Toxicities: reversible anemia, hemolytic anemia, aplastic anemia, gray baby syndrome

Adverse Reactions of Chloramphenicol Central nervous system: Confusion, delirium, depression, fever, headache Dermatologic: Angioedema, rash, urticaria Gastrointestinal: Diarrhea, enterocolitis, glossitis, nausea, stomatitis, vomiting Hematologic: Aplastic anemia, bone marrow suppression, granulocytopenia, hypoplastic anemia, pancytopenia, thrombocytopenia Ocular: Optic neuritis

Clindamycin � Semisynthetic derivative of Lincomycin � Irreversible binding to 50 S subunit � Covers anaerobes and gram + aerobes � Widely useful for head and neck infections � Penetrates saliva, sputum, pleural fluid, and bone, but not CSF � Metabolized in liver-->reabsorbed->eliminated in urine � Side effects: rash, neutropenia/thrombocytopenia, pseudomembranous colitis

Adverse Reactions of clindamycin � Gastrointestinal antibiotic-associated diarrhea due to Clostridium difficile ( Pseudomembranous colitis )caused by overgrowth of C. difficile. � Allergic reactions

Inhibitors of Metabolism � Sulfonamides � Trimethoprim � Interfere with the production of folic acid coenzymes that are required for purine and pyrimidine synthesis
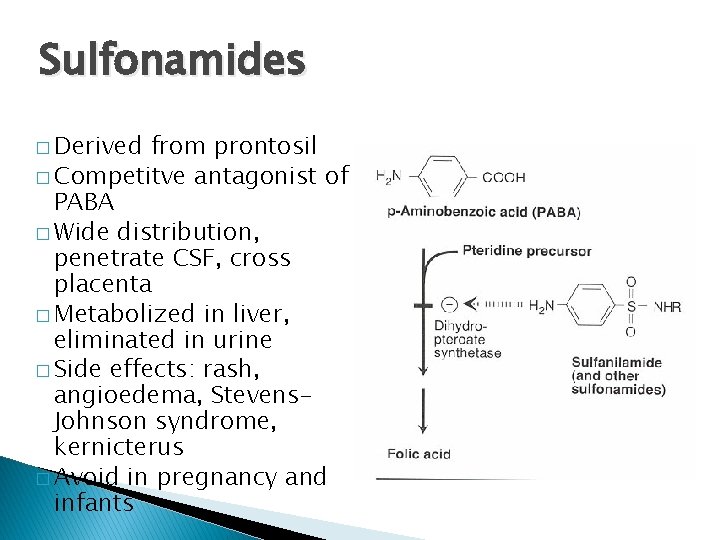
Sulfonamides � Derived from prontosil � Competitve antagonist of PABA � Wide distribution, penetrate CSF, cross placenta � Metabolized in liver, eliminated in urine � Side effects: rash, angioedema, Stevens. Johnson syndrome, kernicterus � Avoid in pregnancy and infants

Sulfonamides

Trimethoprim � Inhibits dihydrofolate reductase � 1000 x higher affinity for bacterial enzyme than human enzyme � Similar spectrum and pharmacokinetic profile as sulfas � Side effects: folate deficiency anemia, leukopenia, granulocytopenia

Major adverse effects of Trimethoprim_Sulfamethoxazole � � � � Systemic allergic reactions: Anaphylaxis , Serum sickness Cutaneous reactions: Rash, Stevens-Johnson syndrome , Erythema muliforme, Toxic epidermal necrolysis , Photodermatis Gastrointestinal and hepatic reactions: Nausea and vomiting, Diarrhea Hepatotoxicity Hematologic reactions: Pancytopenia , Agranulocytosis , Anemia Thrombocytopenia Renal disorders: Transient rise in creatinine due to impaired secretion by trimethoprim, Acute interstitial nephritis, Crystalluria due to precipitation of sulfamethoxazole, Hyperkalemia due to trimethoprim -induced blockade of collecting tubule sodium channel Central nervous system : headache, confusion, aseptic meningitis, Fever Phlebitis
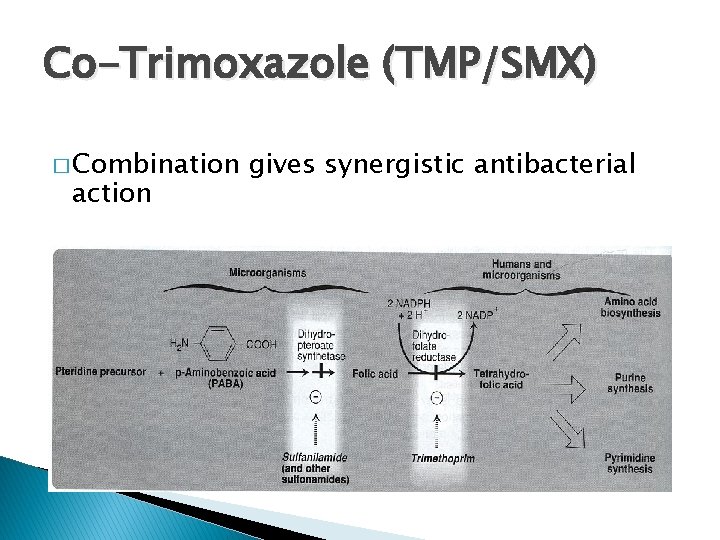
Co-Trimoxazole (TMP/SMX) � Combination action gives synergistic antibacterial

Co-Trimoxazole (TMP/SMX)

Inhibitors of Nucleic Acid Function/Synthesis � Fluoroquinolones ◦ Bind bacteria DNA gyrase (topoisomerase II) ◦ Concentrate in sinus and middle ear mucosa, penetrate cartilage and bone ◦ Partially metabolized in liver-->GI or renal excretion ◦ Side effects: nausea, dizziness, phototoxicity, nephrotoxicity ◦ Avoid in pregnant or nursing women ◦ ? Use in children--possible effect on articular cartilage
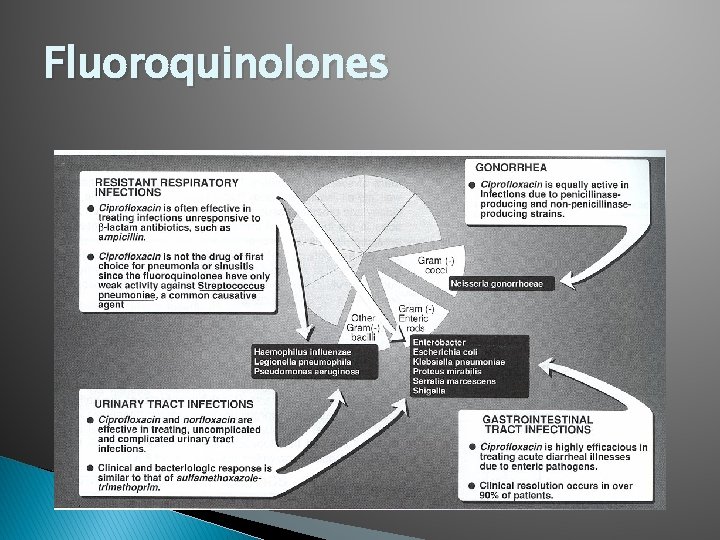
Fluoroquinolones


Adverse Effects of Fluoroquinolones � Cardiac • Prolongation QTc interval • Assumed to be class effect � Articular Damage • Cartilage damage • Induced in animals with large doses

- Slides: 85