Normal Anion Gap Acidoses Renal Tubular Acidosis Jai

Normal Anion Gap Acidoses Renal Tubular Acidosis Jai Radhakrishnan, MD, MS, MRCP, FACC, FASN Associate Professor of Clinical Medicine Columbia University

Disclosures • None

Objective • Physiology of renal acid handling • Diagnostic approach to Metabolic Acidosis with normal anion gap. • Case-based diagnostic workup of the RTA’s
![Chemistry: Carbonic Acid • Carbonic Acid. – [ H+ ] x [ HCO 3 Chemistry: Carbonic Acid • Carbonic Acid. – [ H+ ] x [ HCO 3](http://slidetodoc.com/presentation_image_h/fcb2c7d0a36a518ea029b3f4e1b9781d/image-4.jpg)
Chemistry: Carbonic Acid • Carbonic Acid. – [ H+ ] x [ HCO 3 - ] = k 1 x H 2 CO 3 = k 2 x [ CO 2 ] x [ H 2 O ] • Simplified – H 2 CO 3 is not of clinical interest – [H 2 O] is constant in-vivo – PCO 2 is more familiar than [CO 2]: • [ H+ ] x [ HCO 3 - ] = k x PCO 2 • [ Modified Henderson Equation. ] • Hasselbalch Modification 4
![Metabolic Acidosis: The “Anion Gap” [Na+] - ([Cl-] + [HCO 3 -]) ~ 10 Metabolic Acidosis: The “Anion Gap” [Na+] - ([Cl-] + [HCO 3 -]) ~ 10](http://slidetodoc.com/presentation_image_h/fcb2c7d0a36a518ea029b3f4e1b9781d/image-5.jpg)
Metabolic Acidosis: The “Anion Gap” [Na+] - ([Cl-] + [HCO 3 -]) ~ 10 -12 m. M/L Alb- Alb. HCO 3 - HCO 3 Na+ Cl- Nl Anion gap M acidosis

Etiology of “normal anion gap” (A. K. A. “hyperchloremic”) metabolic acidosis 1. GI bicarbonate loss (typically also with low K): diarrhea villous adenoma pancreatic, biliary, small bowel fistulae uretero-sigmoidostomy obstructed uretero-ileostomy
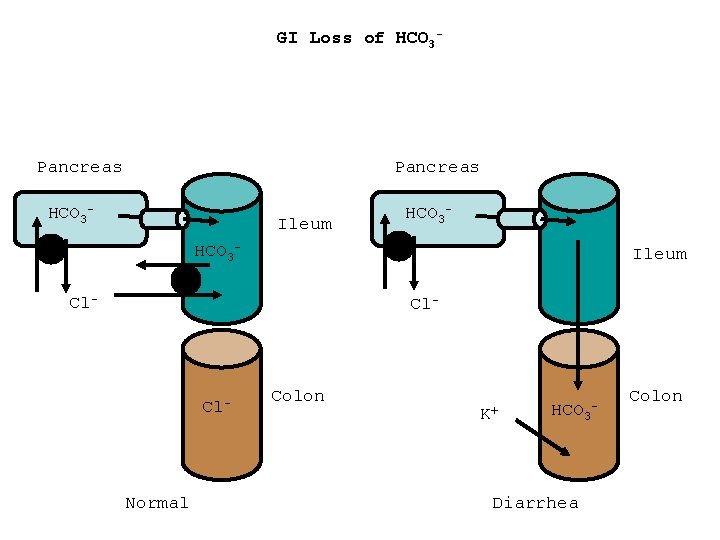
GI Loss of HCO 3 - Pancreas HCO 3 - Ileum Cl- Cl- Normal Colon K+ HCO 3 - Diarrhea Colon
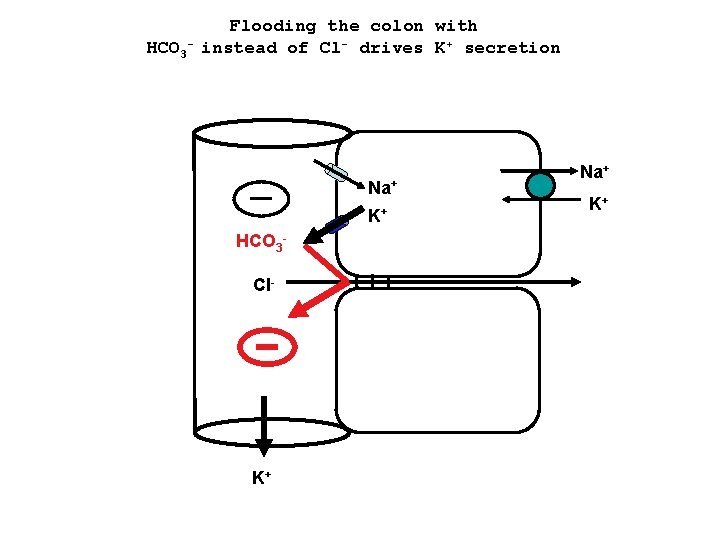
HCO 3 - Flooding the colon with instead of Cl- drives K+ secretion Na+ K+ HCO 3 Cl- K+ Na+ K+
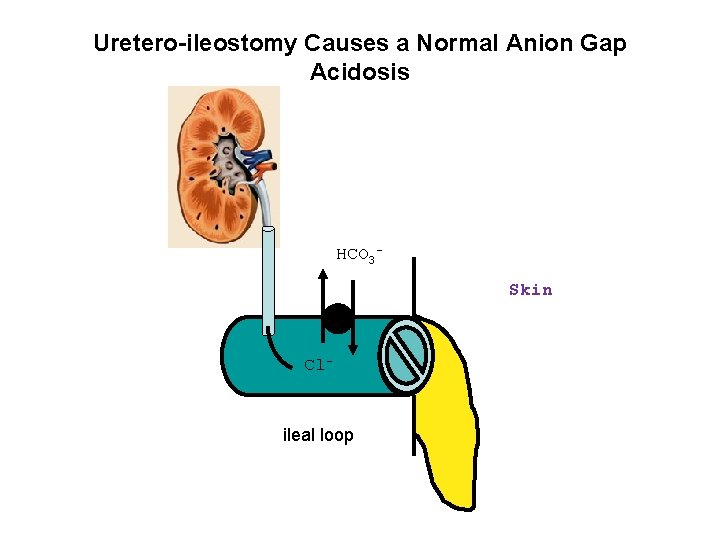
Uretero-ileostomy Causes a Normal Anion Gap Acidosis HCO 3 Skin Cl- ileal loop

Causes of a “normal anion gap” (A. K. A. “hyperchloremic”) metabolic acidosis 2. Ingestions & infusions ammonium chloride hyperalimentation (arginine/lysine-rich) 3. Renal bicarbonate (or equivalent) loss • proximal RTA • distal RTA • type IV RTA early renal failure acetazolamide hydrated DKA
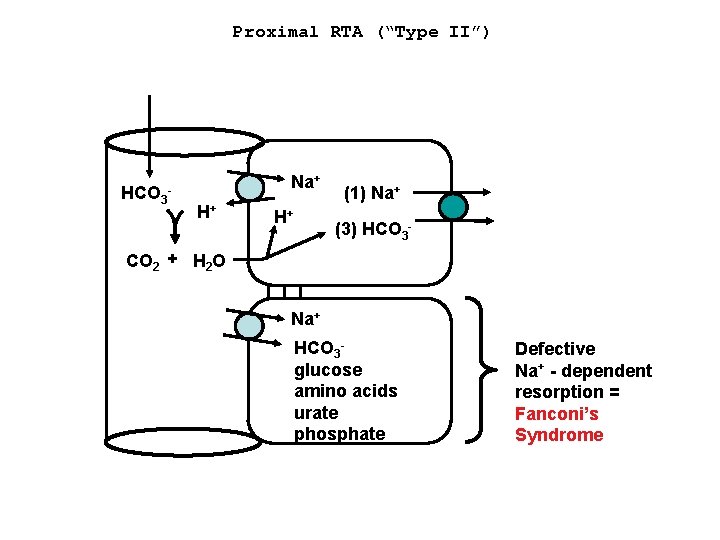
Proximal RTA (“Type II”) HCO 3 Na+ - H+ H+ (1) Na+ (3) HCO 3 - CO 2 + H 2 O Na+ HCO 3 glucose amino acids urate phosphate Defective Na+ - dependent resorption = Fanconi’s Syndrome
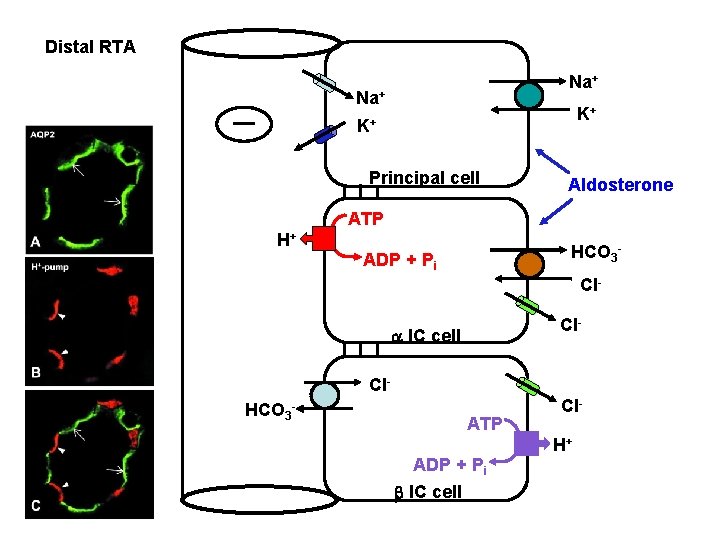
Distal RTA Na+ K+ K+ Principal cell Aldosterone ATP H+ HCO 3 - ADP + Pi Cl. Cl- a IC cell Cl. HCO 3 - ATP ADP + Pi b IC cell Cl. H+
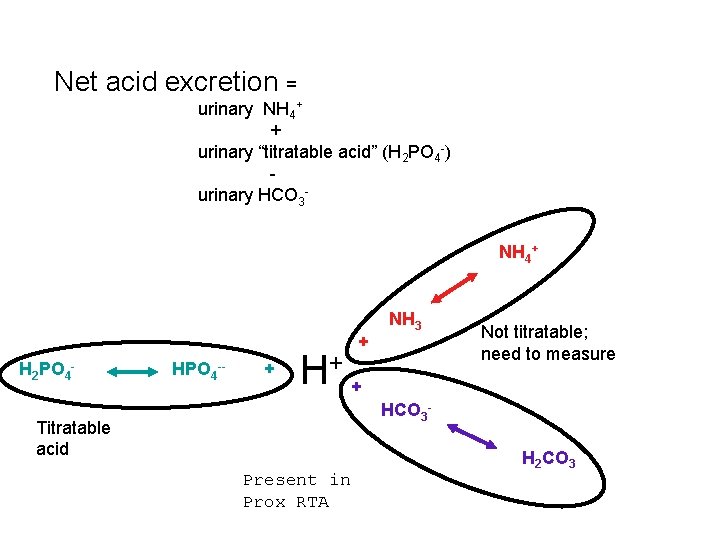
Net acid excretion = urinary NH 4+ + urinary “titratable acid” (H 2 PO 4 -) urinary HCO 3 - NH 4+ + H 2 PO 4 - HPO 4 -- + NH 3 H+ + Not titratable; need to measure HCO 3 - Titratable acid Present in Prox RTA H 2 CO 3
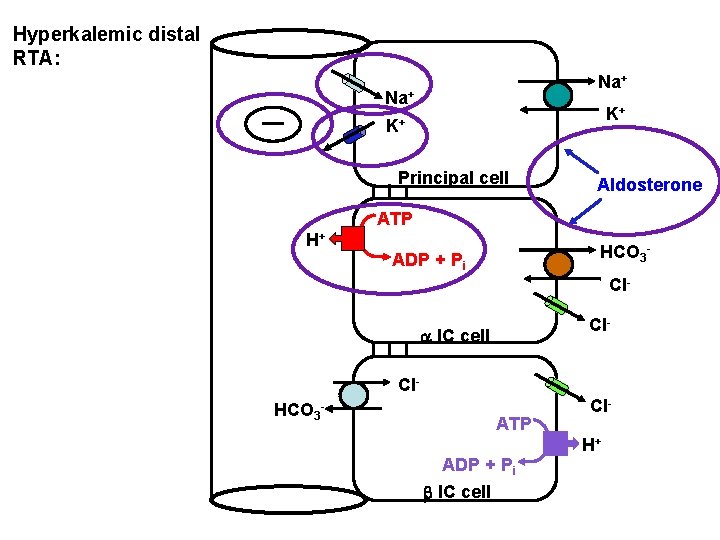
Hyperkalemic distal RTA: Na+ K+ K+ Principal cell Aldosterone ATP H+ HCO 3 - ADP + Pi Cl. Cl- a IC cell Cl. HCO 3 - ATP ADP + Pi b IC cell Cl. H+
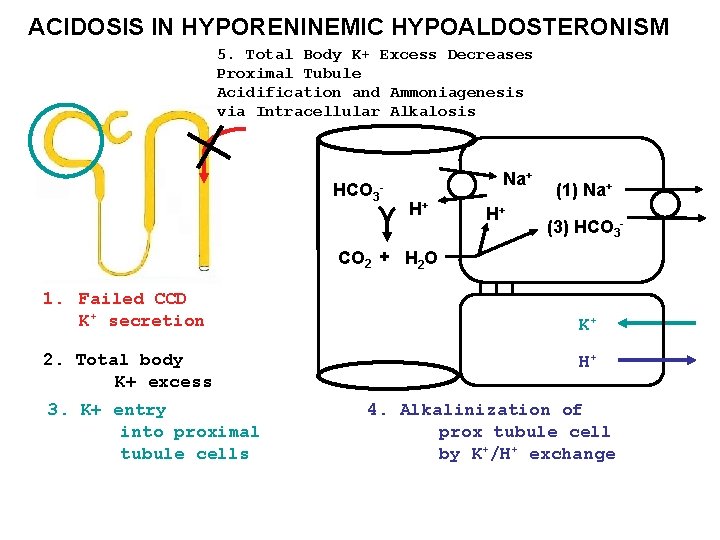
ACIDOSIS IN HYPORENINEMIC HYPOALDOSTERONISM 5. Total Body K+ Excess Decreases Proximal Tubule Acidification and Ammoniagenesis via Intracellular Alkalosis HCO 3 Na+ - H+ H+ (1) Na+ (3) HCO 3 - CO 2 + H 2 O 1. Failed CCD K+ secretion 2. Total body K+ excess 3. K+ entry into proximal tubule cells K+ H+ 4. Alkalinization of prox tubule cell by K+/H+ exchange

DIAGNOSTIC APPROACH Minimum Urine p. H Urinary Anion Gap Plasma potassium Renal stones or Nephrocalcinosis Prox. Tubular dysfunction FEHCO 3 Daily bicarbonate replacement needs
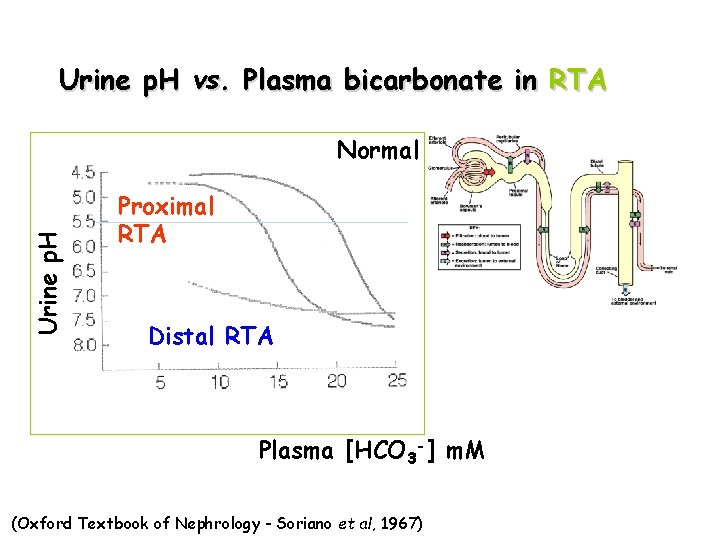
Urine p. H vs. Plasma bicarbonate in RTA Urine p. H Normal Proximal RTA Distal RTA Plasma [HCO 3 -] m. M (Oxford Textbook of Nephrology - Soriano et al, 1967)

Urinary Anion Gap • Urine (Na+K) – Cl Unmeasured anions-unmeasured cations • Proton is partially excreted as NH 4 (unmeasured cation) • The gap is usually Zero or Negative • In d. RTA the anion gap will remain zero or positive • In other acidoses, the gap will become more negative. 19
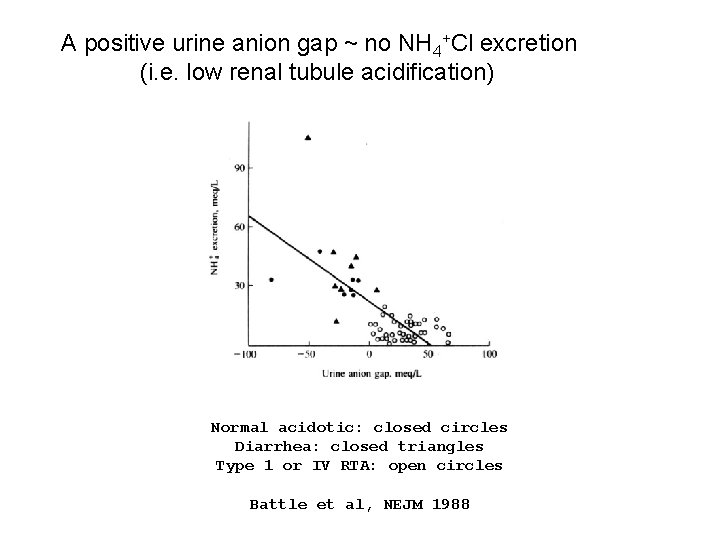
A positive urine anion gap ~ no NH 4+Cl excretion (i. e. low renal tubule acidification) Normal acidotic: closed circles Diarrhea: closed triangles Type 1 or IV RTA: open circles Battle et al, NEJM 1988
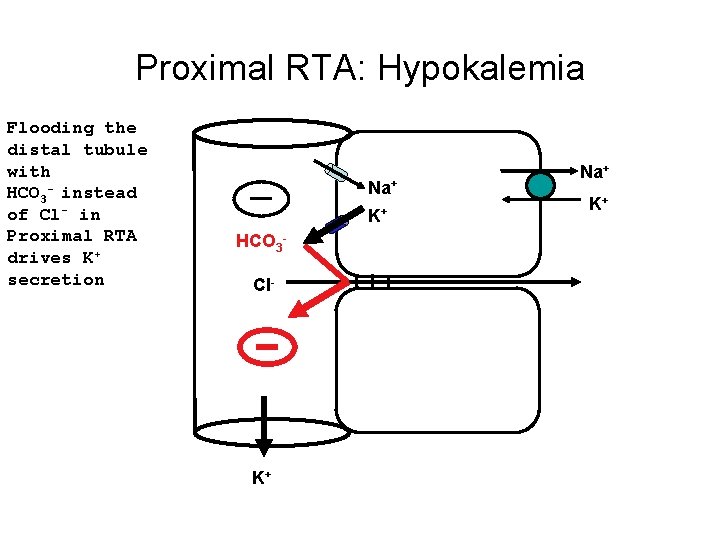
Proximal RTA: Hypokalemia Flooding the distal tubule with HCO 3 - instead of Cl- in Proximal RTA drives K+ secretion Na+ K+ HCO 3 Cl- K+ Na+ K+
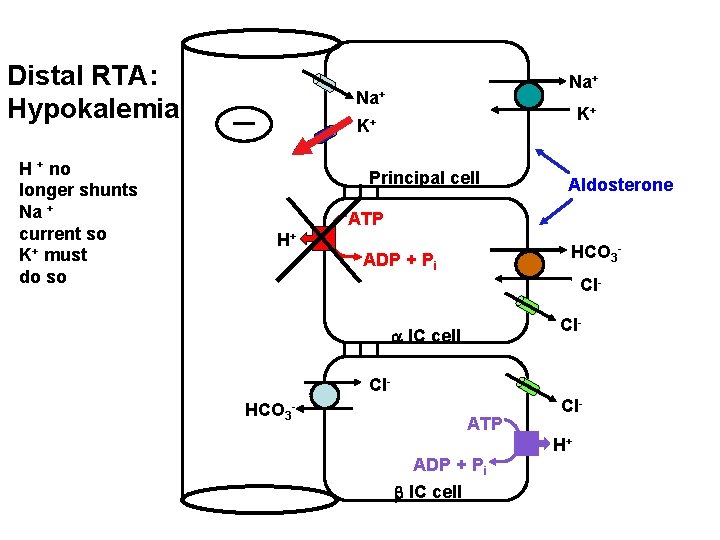
Distal RTA: Hypokalemia H + no longer shunts Na + current so K+ must do so Na+ K+ K+ Principal cell Aldosterone ATP H+ HCO 3 - ADP + Pi Cl. Cl- a IC cell Cl. HCO 3 - ATP ADP + Pi b IC cell Cl. H+
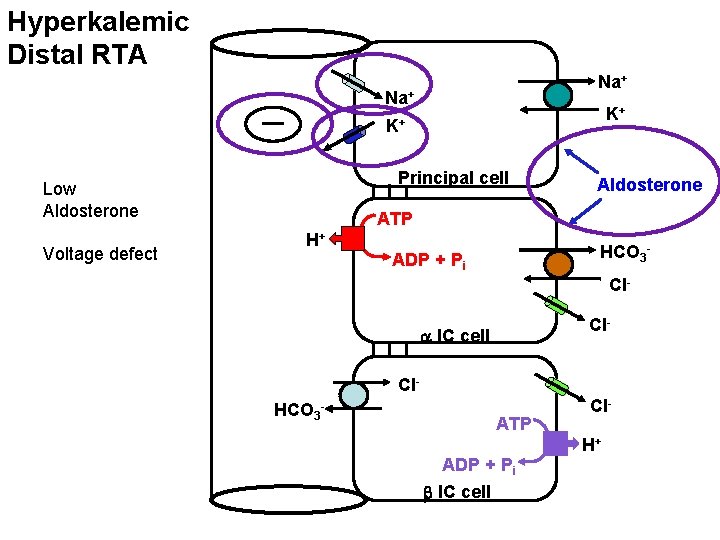
Hyperkalemic Distal RTA Na+ K+ K+ Principal cell Low Aldosterone Voltage defect Aldosterone ATP H+ HCO 3 - ADP + Pi Cl. Cl- a IC cell Cl. HCO 3 - ATP ADP + Pi b IC cell Cl. H+
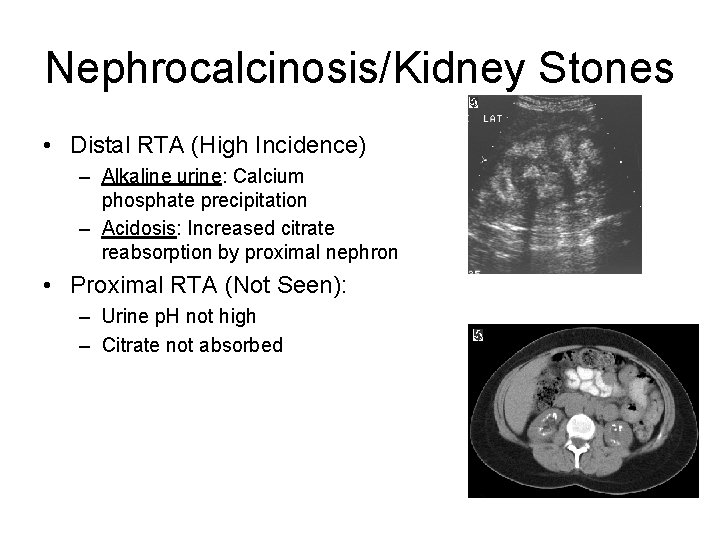
Nephrocalcinosis/Kidney Stones • Distal RTA (High Incidence) – Alkaline urine: Calcium phosphate precipitation – Acidosis: Increased citrate reabsorption by proximal nephron • Proximal RTA (Not Seen): – Urine p. H not high – Citrate not absorbed
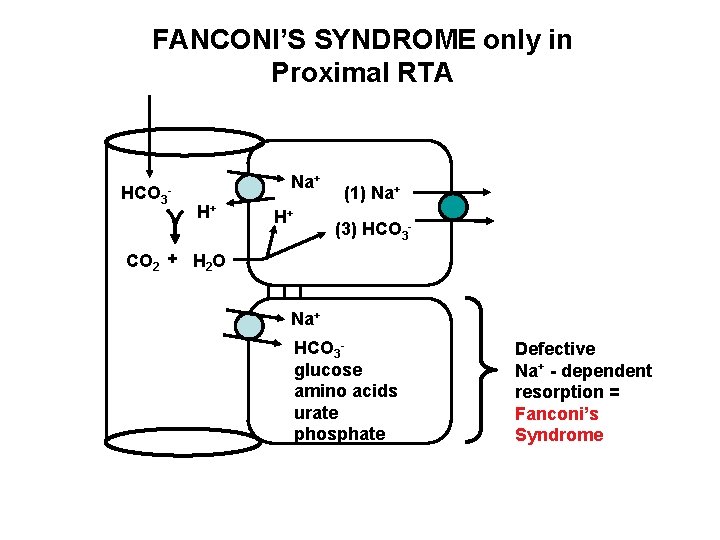
FANCONI’S SYNDROME only in Proximal RTA HCO 3 Na+ - H+ H+ (1) Na+ (3) HCO 3 - CO 2 + H 2 O Na+ HCO 3 glucose amino acids urate phosphate Defective Na+ - dependent resorption = Fanconi’s Syndrome
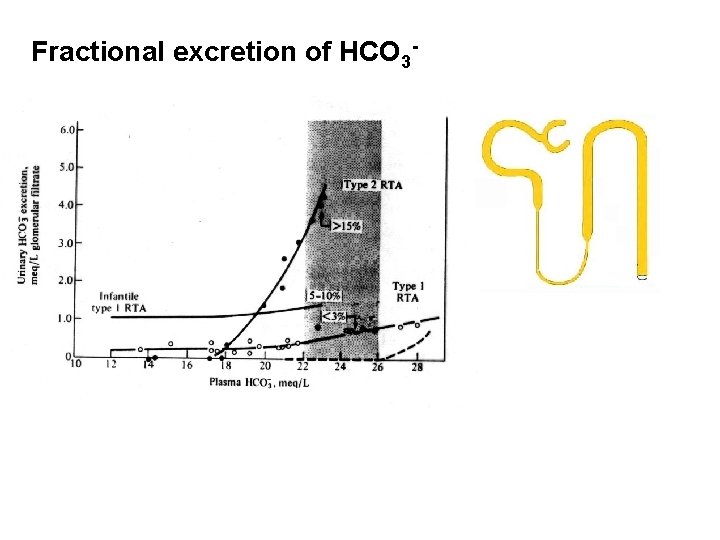
Fractional excretion of HCO 3 -
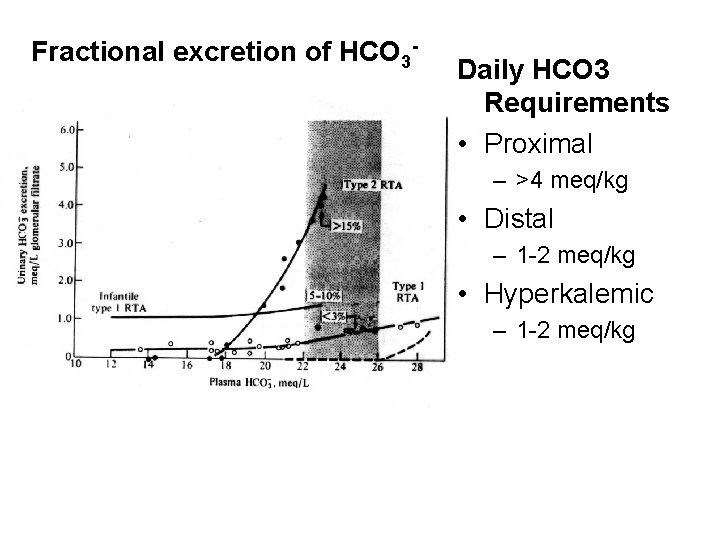
Fractional excretion of HCO 3 - Daily HCO 3 Requirements • Proximal – >4 meq/kg • Distal – 1 -2 meq/kg • Hyperkalemic – 1 -2 meq/kg
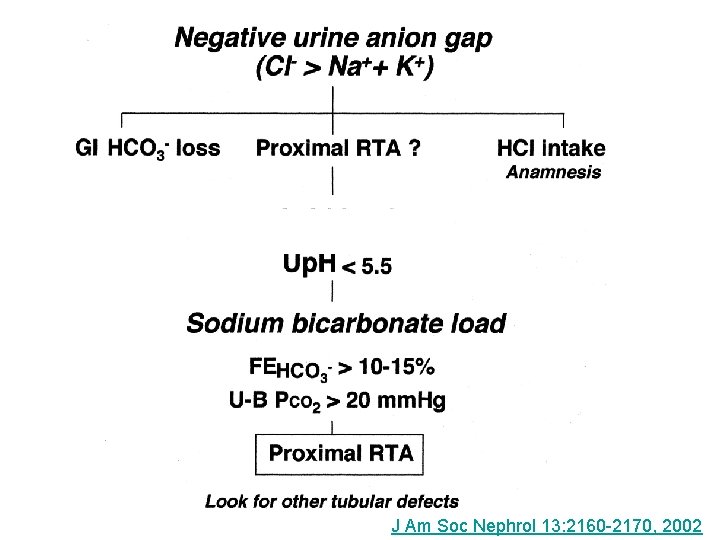
J Am Soc Nephrol 13: 2160 -2170, 2002
![Positive Urinary anion gap Urine p. H & plasma [K+] Urine p. H < Positive Urinary anion gap Urine p. H & plasma [K+] Urine p. H <](http://slidetodoc.com/presentation_image_h/fcb2c7d0a36a518ea029b3f4e1b9781d/image-29.jpg)
Positive Urinary anion gap Urine p. H & plasma [K+] Urine p. H < 5. 5 & high[K+] Hypoaldosteronism RTA(type IV) Urine p. H > 5. 5 & low/nl[K+] Distal RTA (“Type I”): secretory or gradient defect


Case 1 • • • A 55 -year-old woman presents with complaints of lethargy, thirst, muscle weakness and generalized body pains. Previous ED visits with hypokalemia. Her serum potassium level was 2. 6 mmol/l. Other Electrolytes: Proximal RTA – – – • • sodium 138 mmol/l chloride 116 mmol/l HCO 3 17 mmol/l BUN/Creatinine normal Glucose 75 mg/d. L Urine analysis: p. H 5. 4, 2+ glucose Urine anion gap: -20 ABG: p. H 7. 25 p. CO 2 28 p. O 2 100 total bicarbonate 15. 1 mmol/l base excess – 13. 7 mmol/l
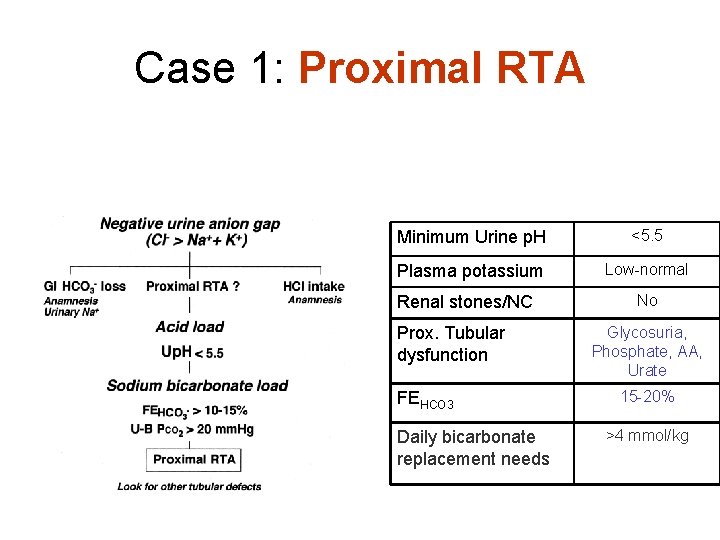

Case 1: Proximal RTA Minimum Urine p. H <5. 5 Plasma potassium Low-normal Renal stones/NC Prox. Tubular dysfunction FEHCO 3 Daily bicarbonate replacement needs No Glycosuria, Phosphate, AA, Urate 15 -20% >4 mmol/kg

FEHCO 3 • Intravenous infusion of sodium bicarbonate at a rate of 0. 5 to 1. 0 meq/kg per hour • UHCO 3 x PCr FEHCO 3 = —————— x 100 PHCO 3 x UCr • Proximal RTA: FE HCO 3>15 -20%

Clinical Features of Proximal RTA • Urine p. H depends on plasma [HCO 3 -] • Fractional HCO 3 - excretion high (15 -20%) at nl plasma [HCO 3 -] • Plasma [K+] reduced, worsens with HCO 3 - therapy • Dose of daily HCO 3 - required: 10 -15 m. Eq/kg/d • Non-renal: rickets or osteomalacia

Causes of Proximal RTA • Primary isolated proximal RTA – hereditary (persistent) • a. autosomal dominant • b. autosomal recessive associated with mental retardation and ocular abnormalities – Sporadic (transient in infancy) • Secondary proximal RTA – in the context of Fanconi syndrome (cystinosis, galactosemia, fructose intolerance, tyrosinemia, Wilson disease, Lowe syndrome, metachromatic leukodystrophy, multiple myeloma, light chain disease) – drugs and toxins (acetazolamide, outdated tetracycline, aminoglycoside antibiotics, valproate, 6 -mercaptopurine, streptozotocin, iphosphamide, lead, cadmium, mercury) – other clinical entities (vitamin D deficiency, hyperparathyroidism, chronic hypocapnia, Leigh syndrome, cyanotic congenital heart disease, medullary cystic disease, Alport syndrome, corticoresistant nephrotic syndrome, renal transplantation, amyloidosis, recurrent nephrolithiasis) J Am Soc Nephrol 13: 2160 -2170, 2002
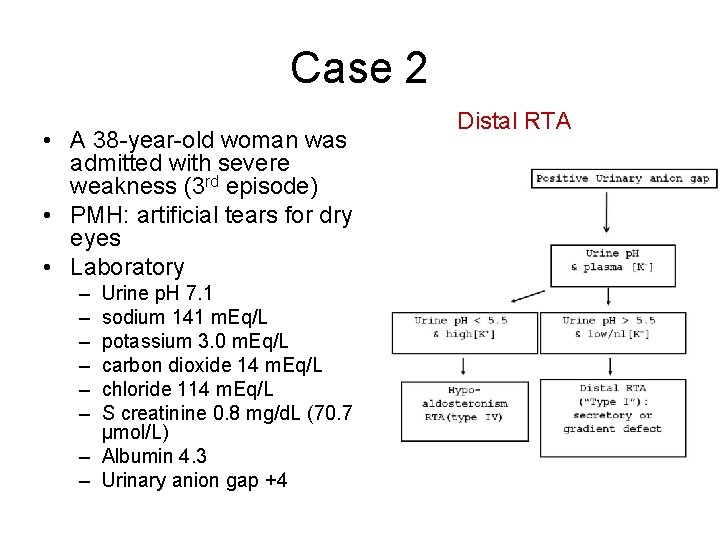
Case 2 • A 38 -year-old woman was admitted with severe weakness (3 rd episode) • PMH: artificial tears for dry eyes • Laboratory Distal RTA – – – Urine p. H 7. 1 sodium 141 m. Eq/L potassium 3. 0 m. Eq/L carbon dioxide 14 m. Eq/L chloride 114 m. Eq/L S creatinine 0. 8 mg/d. L (70. 7 µmol/L) – Albumin 4. 3 – Urinary anion gap +4 Arch Intern Med. 2004; 164: 905 -909
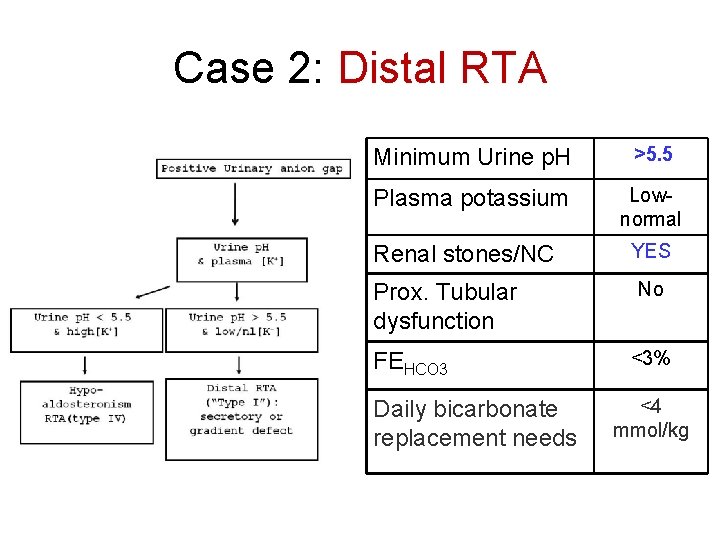
Case 2: Distal RTA Minimum Urine p. H >5. 5 Plasma potassium Lownormal Renal stones/NC Prox. Tubular dysfunction FEHCO 3 Daily bicarbonate replacement needs YES No <3% <4 mmol/kg Arch Intern Med. 2004; 164: 905 -909
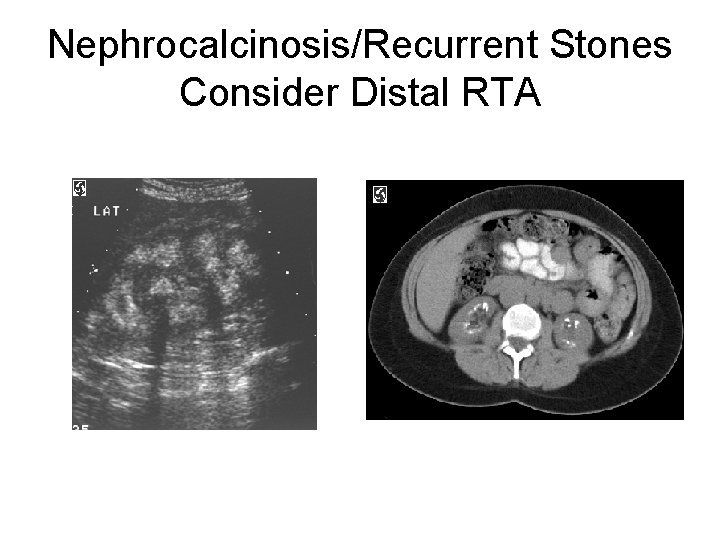
Nephrocalcinosis/Recurrent Stones Consider Distal RTA

Furosemide/Fludrocortisone Test • Baseline urine sample • Oral administration of furosemide (40 mg) and fludrocortisone (1 mg). • Fluid intake ad libitum. • Urine q 1 h x 6 h after the baseline sample. • Failed to acidify their urine to p. H<5. 3 Kidney International (2007) 71, 1310– 1316

• Schirmer’s test positive • antibodies to the Ro/SSA and La/SSB + • Cryocrit +

Causes of distal RTA J Am Soc Nephrol 13: 2160 -2170, 2002
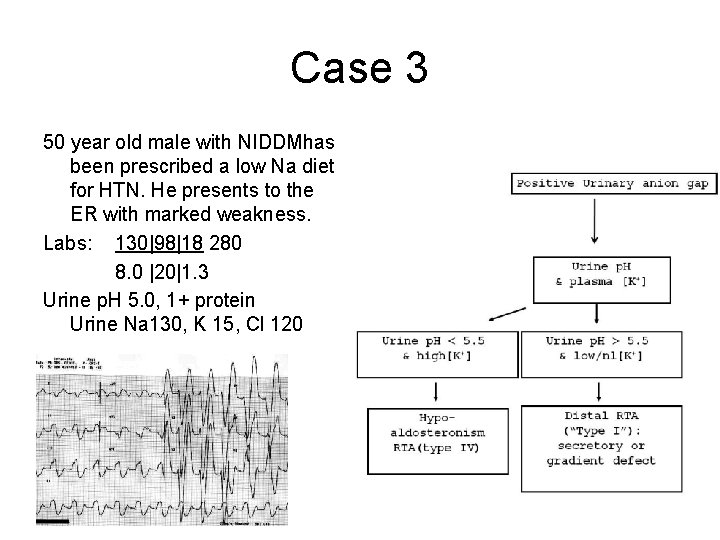
Case 3 50 year old male with NIDDMhas been prescribed a low Na diet for HTN. He presents to the ER with marked weakness. Labs: 130|98|18 280 8. 0 |20|1. 3 Urine p. H 5. 0, 1+ protein Urine Na 130, K 15, Cl 120

Case 3 50 year old male with NIDDMhas been prescribed a low Na diet for HTN. He presents to the ER with marked weakness. Labs: 130|98|50 280 8. 0 |20|1. 3 Urine p. H 5. 0, 1+ protein Hyperkalemic Minimum Urine p. H <5. 5 Plasma potassium High Renal stones/NC No Prox. Tubular dysfunction No FEHCO 3 Daily bicarbonate replacement needs <3% <4 mmol/kg

Type IV RTA: Etiology • Aldosterone – Hyporenin/hypoaldo (CKD) – Addison – Congenital : enzymes • Voltage – PHA – Drugs: TMP, K-sparing, pentamidine CNI (Na-K ATPas) • Multiple: Tubulointerstitial disease
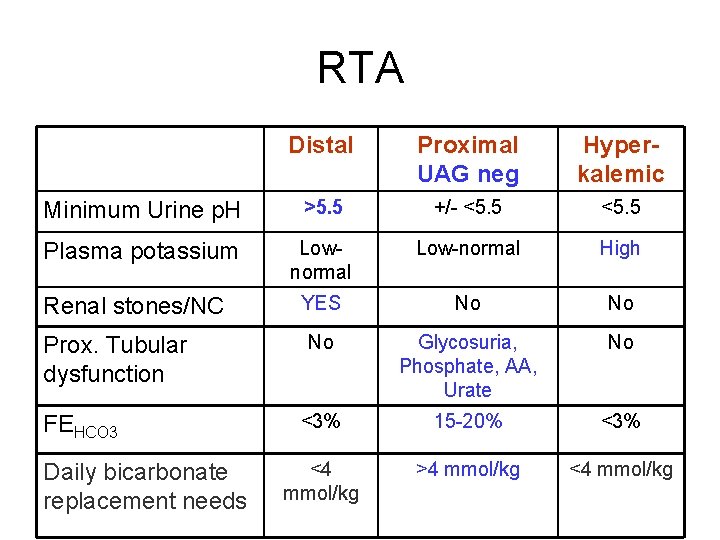
RTA Distal Proximal UAG neg Hyperkalemic Minimum Urine p. H >5. 5 +/- <5. 5 Plasma potassium Lownormal Low-normal High YES No No Glycosuria, Phosphate, AA, Urate No <3% 15 -20% <3% <4 mmol/kg >4 mmol/kg <4 mmol/kg Renal stones/NC Prox. Tubular dysfunction FEHCO 3 Daily bicarbonate replacement needs
- Slides: 45