Noon Report CC Bleeding Dr Catherine Murphree 3302020

Noon Report CC: Bleeding Dr. Catherine Murphree 3/30/2020 Chief facilitator: Dr. Riana Wurzburger

HPI What do you suspect this is? • 79 y/o male • History of BCC, melanoma s/p Moh’s, PTSD, alcohol use disorder in remission • Evaluated in interim clinic (on a Monday) for a rash- present three days • 1 week ago- placed CPAP on face which caused intra-nasal cyst to rupturetwo days later had lesion on his head that bled uncontrollably • Next day- gingival bleeding while cleaning teeth, and “dark spots” in back of his throat- later same day had epistaxis and noticed diffuse rash on arms (Saturday) • We saw him on Monday night after sent in from clinic

HPI/ROS • Other symptoms patient endorsed was cold like symptoms for past YEAR including cough, rhinorrhea, chills, with increased fatigue • 15 lb weight loss over past year- intentional • No new medications • No joint swelling • No sick contacts recently • No sexual contacts recently • Denies fevers, dizziness, confusion, focal weakness, headache, blood in urine or bowel movements

Past Medical History: Medications: • chronic sinusitis • HTN • OSA with CPAP • Melanoma • Actinic keratosis • Seborrheic keratoses • PTSD • H/o alcohol abuse • Albuterol as needed (doesn’t use) • Budesonide/formoterol (rarely uses) • Eye drops • No new medications or OTCs in the last month

Social History: Family History: • Tobacco- 11 years of age to 45 years of age 1 PPD • Tried MDMA 6 times over a period of 10 years- no other illicit drugs • 2 -3 beers +- 4 glasses of wine daily for many years- quit six years ago • No family history of bleeding disorders that he knows of- no family history of clotting disorders that he knows of • Lives in 2 bedroom apartment NO PETS

What is your differential diagnosis? What’s most likely? What can’t you miss?

DDX: Bleeding Disorders Start broadly: is this a problem with Primary vs Secondary hemostasis? Primary: thrombocytopenia (production, sequestration, destruction), platelet dysfunction, VWD, others Secondary: factor deficiencies (acquired vs hereditary), vitamin K deficiencies, liver disease, DIC, others This case sounds like a problem with primary Vascular: Scurvy, others hemostasis: epistaxis, gingival bleeding, “rash” Ma, A. (2019). Approach to the adult with a suspected bleeding disorder. In J. A. Melin (Ed. ), Up. To. Date. Retrieved March 30, 2020, from https: //www-uptodatecom. liboff. ohsu. edu/contents/approach-to-the-adult-with-a-suspected-bleeding-disorder

Based on the HPI and history, what do you want to look for on exam? Why?

Exam: Vitals: afebrile, pulse 74, RR 23, blood pressure 142/88, weight 226. 4 lbs, Sp. O 2 99% on room air Gen: resting comfortably HEENT: scattered red/purple macules throughout face and scalp in addition to buccal mucosa + hard palate- one dark nodular tongue lesion noted- few scabs on the scalp CV: RRR, no MRG Lungs: clear to auscultation, no accessory muscle use, no wheezes Abd: scattered petechiae throughout, no tenderness, no distension Ext: warm well perfused no LE edema Skin: scattered red/purple macules as described above Neuro: non focal
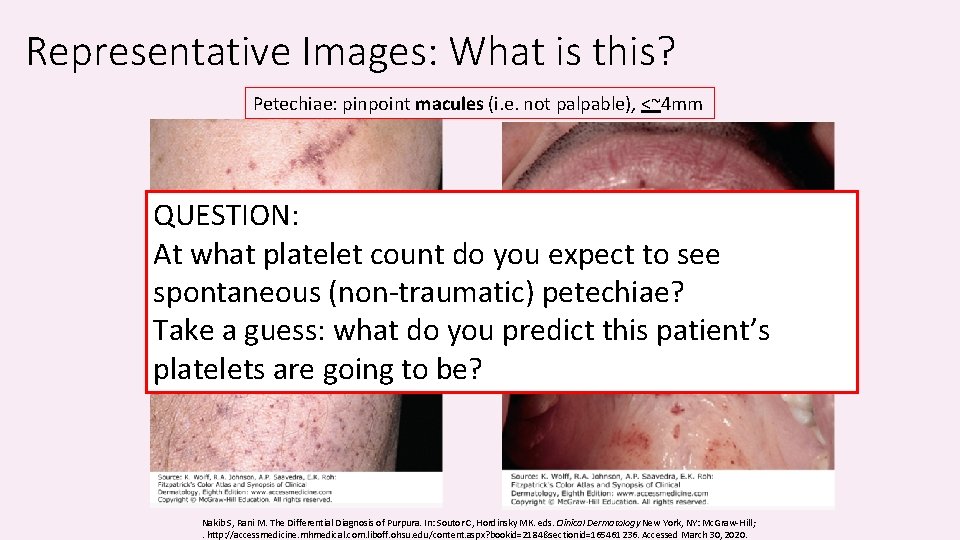
Representative Images: What is this? Petechiae: pinpoint macules (i. e. not palpable), <~4 mm QUESTION: At what platelet count do you expect to see spontaneous (non-traumatic) petechiae? Take a guess: what do you predict this patient’s platelets are going to be? Nakib S, Rani M. The Differential Diagnosis of Purpura. In: Soutor C, Hordinsky MK. eds. Clinical Dermatology New York, NY: Mc. Graw-Hill; . http: //accessmedicine. mhmedical. com. liboff. ohsu. edu/content. aspx? bookid=2184§ionid=165461236. Accessed March 30, 2020.

How has your differential changed with the exam?

Resident’s differential diagnoses: • Blood/immune disorders such as ITP, TTP, DIC, leukemia, etc. • Vasculitis, etc • Viral (CMV, EBV, hep C, VZV, etc) vs. bacterial infection (hemorrhagic fevers, RMSF, endocarditis, strep pharyngitis, etc) • Less likely medication reaction (patient without any new medication exposures and doesn’t take them at baseline) • Physical trauma (less likely not endorsed in history)

What’s your summary statement thus far?

Resident’s summary statement: • 79 y/o male who is presenting with acute onset epistaxis, gingival bleeding, and diffuse petechial rash in the setting of a year of cough, rhinorrhea, malaise without significant family history who is currently hemodynamically stable undergoing further workup.

Basic diagnostic studies Spontaneous petechiae (and mucosal bleeding) typically occurs at plts <10, 000 Wbc 5. 5, rbc 4. 07, hgb 12. 7, hct 40. 1, platelets less than 5 (confirmed) AST 19 ALT 14 alk phos 71 bilirubin 1. 0 Calcium 9. 2 total protein 7. 9 Cr. 1. 1 BUN 13

Based on your differential, what other studies do you want? Why?

More laboratory studies Peripheral blood smear: no schistocytes!! Haptoglobin 38, LDH 288 Vitamin b-12 839, Folate 14. 2, Ferritin 733 PT 14. 8, PTT 42. 7, INR 1. 2 TSH 2. 83 Flu negative, COVID negative, + for Human rhinovirus/enterovirus group PCR Hep B negative, Hep C negative, CMV not detected, HIV negative, H. pylori negative Resident Thoughts: Pretty extensive lab work up- only other thing I would have considered would be a bone marrow biopsy vs. maybe Flow cytometry vs. FISH which they eventually got later

Imaging studies None- none needed

What is your leading diagnosis now? Can we streamline the summary statement more with this data?

DDX: Thrombocytopenia From Dr. Deloughery’s lecture on 01/14/2020: BROAD CATEGORIES INCLUDE • • • Production Defects (RARE to cause isolated thrombocytopenia) Sequestration (hypersplenism) Immune Destruction Non-immune destruction Liver disease (a little bit of everything…sequestration, production) You can break your DDX down further based on the severity of the thrombocytopenia. The DDX for SEVERE thrombocytopenia isn’t actually that long… Our Patient… - Drug-induced

A few more questions to help your DDX… NO

Resident’s modified summary statement: • 79 y/o male who is presenting with acute onset epistaxis, gingival bleeding, and diffuse petechial rash found to have platelets less than 5, 000 without shistocytes on smear, + for rhino/enterovirus suggestive of…

Generally not recommended for diagnosis

ITP…but why? PAUSE. What are some causes of secondary ITP? What do you think was the cause here?

Hospital course/more info: • Started dexamethasone initially • Started IVIG after this • Didn’t respond so tried po steroids • Eventually started ritux and Eltrombopag • Bone marrow biopsy showed slightly hypercellular marrow with maturing trilineage hematopoiesis, megakaryotic hyperplasia with no evidence of dysplasia, lymphoproliferative disorder, plasma cell neoplasm, no increase in blasts

Take us home: - Followed up with hematology as an outpatient Determined most likely was ITP 2/2 viral etiology Continued on Eltrombopag and rituximab last I saw Platelets last checked were 23, 000

Resident Teaching Points • ITP- immune thrombocytopenic purpura- autoimmune disorder where there is antibody mediated platelet destruction and decreased platelet production (thought to be from Ig. G antibody targeting glycoproteins IIb-IIIa on the platelet) • Usually a dx of exclusion • DDx- TTP, HUS, DIC, PNH, MDS, lymphoproliferative disorders, HIV, hepatitis C, and drug induced thrombocytopenia • Treatment- aimed at reducing amount of antibody mediated destructioncan use steroids, IVIG and anti-Rh. D immunoglobulin • Splenectomy is usually a second line treatment therapy • Auto-antibodies also interfere with megakaryocyte maturation and platelet production, so using things like thrombopoietin receptor mimetic drugs (Eltrombopag) have shown efficacy in increasing platelet number!

References Karen A. Kinnaman, William D. Binder, Eric S. Nadel, David F. M. Brown, Petechiae, Anemia, and Thrombocytopenia, The Journal of Emergency Medicine, Volume 48, Issue 4, 2015, Pages 461 -465, ISSN 0736 -4679, Khan M, Mikhael J. A review of immune thrombocytopenic purpura: focus on the novel thrombopoietin agonists. J Blood Med. 2010; 1: 21– 31. doi: 10. 2147/JBM. S 6803 Zainal A, Salama A, Alweis R. Immune thrombocytopenic purpura. J Community Hosp Intern Med Perspect. 2019; 9(1): 59– 61. Published 2019 Feb 11. doi: 10. 1080/20009666. 2019. 1565884

Chief References Ma, A. (2019). Approach to the adult with a suspected bleeding disorder. In J. A. Melin (Ed. ), Up. To. Date. Retrieved March 30, 2020, from https: //www-uptodate-com. liboff. ohsu. edu/contents/approachto-the-adult-with-a-suspected-bleeding-disorder Nakib S, Rani M. The Differential Diagnosis of Purpura. In: Soutor C, Hordinsky MK. eds. Clinical Dermatology New York, NY: Mc. Graw-Hill; . http: //accessmedicine. mhmedical. com. liboff. ohsu. edu/content. aspx? bookid=2184§ionid=165461236. Accessed March 30, 2020. Deloughery, T. Thrombocytopenia. OHSU IM Noon Conference Lecture, 01/14/2020; https: //ohsu. medhub. com/index. mh

Bath time


Dinner time

BEFORE YOU GO! PLEASE take a moment to list ONE take away point from this case on the comments section for this blog post. It’s a small way for us to stay connected and hear each other’s thoughts with virtual reports. Thank you!
- Slides: 33