NonTraumatic Brachial Plexopathy All that radiates Disclosure I

Non-Traumatic Brachial Plexopathy All that radiates…. .

Disclosure I have NO RELEVANT financial disclosures.

Goals of lecture • Review common brachial plexopathies • Discuss key history and physical examination issues which differentiate plexus from radiculopathy • Discuss positives and pitfalls of major diagnostic studies

Brachial Plexopathy • Brachial Plexus Neuropathy (Neuralgic amyotrophy ) (Parsonage-Turner) • True neurogenic thoracic outlet syndrome • Diabetic cervical radiculoplexus neuropathy • Malignancy – Primary tumor – Malignant invasion – Radiation

Brachial plexopathy • • • Traumatic plexopathy Perioperative plexopathy Stinger/burner Hematoma/ false aneurysm Perioperative – Stretch neck/ shoulder – Medial sternotomy – Regional anesthesia – Local shoulder surgery – Brachial plexus neuropathy

Neuralgic Amyotrophy: Parsonage and Turner Syndrome • History – Sudden onset of severe pain, often nocturnal, followed by weakness – Pain presents in cervical spine or shoulder blade and upper arm – Pain often diminishes or resolves after weakness develops – Often preceded by infection, trauma, vaccination, surgical intervention, stress

Neuralgic Amyotrophy: Parsonage and Turner Syndrome • Physical examination – Patchy findings which are not dermatomal; may be a combination of radiculopathy, brachial plexopathy and peripheral nerve abnormalities – Presentation (in order of frequency) • Upper and/or middle plexus – Frequently with long thoracic nerve involvement • Pan plexus > middle plexus/ posterior cord • Lower plexus • Anterior interosseus nerve predominant • Van Alfen, 2006

NA: Diagnostic studies • EMG: patchy findings of root/ plexus/ nerve • Confounding factors include comorbidites or asymptomatic electrical findings • MRI brachial plexus and shoulder – Most common abnormalities supra/infraspinatus – Acute: increase in T 2 signal (muscular edema) – Subacute: T 2 changes persist, atrophy may develop – Subacute to chronic: increased T 1 signal due to fat infiltration • (Scalf, 2007)

Diagnostic studies • Cervical MRI: watch for “TBU” (true but unrelated) – Major “abnormality” in 19% of asymptomatic patients • 14% of patients < 40 • 28% of patients > 40 • Milder disc narrowing or degeneration in 60% of patients > 40 (Boden, 1990)

Neuralgic Amyotrophy: Differential diagnosis • Cervical radiculopathy • Brachial Plexopathy • Peripheral nerve
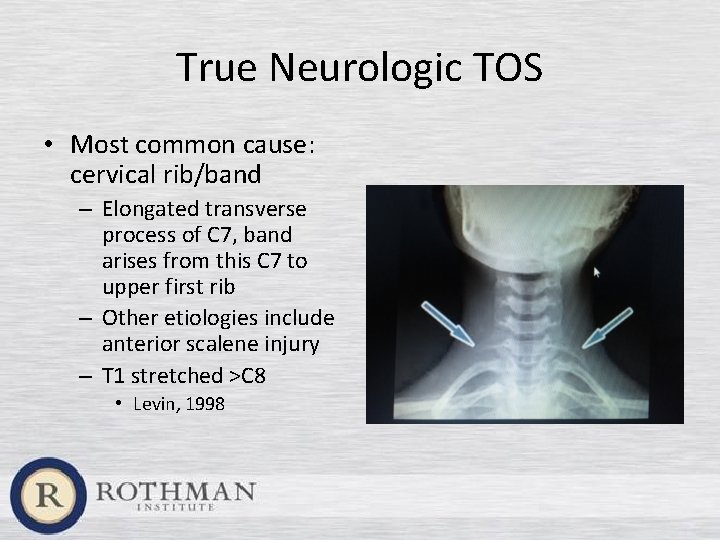
True Neurologic TOS • Most common cause: cervical rib/band – Elongated transverse process of C 7, band arises from this C 7 to upper first rib – Other etiologies include anterior scalene injury – T 1 stretched >C 8 • Levin, 1998

True Neurologic TOS • History – Gradual onset of wasting and weakness of hand – Paresthesias of ulnar forearm and small finger – May have achiness in forearm • Physical – Thenar weakness/ atrophy> than hypothenar muscles – Flexor forearm muscles weak – Sensory loss varies, may not split ring finger

True Neurologic TOS: Differential diagnosis • Cervical radiculopathy (C 8 or T 1) – T 1 results in more thenar weakness/ dermatomal findings (more T 1 in APB) – C 8 results in more hypothenar weakness/dermatomal findings • • • Peripheral nerve Spinal cord injury Other brachial plexopathies Syrinx Motor neuron disease

True Neurologic TOS: Studies • MRI/ Xray of cervical spine • MRI brachial plexus • Electrodiagnostic studies – Most sensitive findings: mabc snap often absent, ulnar snap low amplitude, median cmap low amplitude • mabc and median cmap share T 1 innervation • Few small fibs in thenar > hypothenar musculature • *Vs median sternotomy plexopathy in which ulnar snap and ulnar cmap have lower amplitudes and median cmap /mabc is less affected – Fibs in hypothenar>thenar musculature • Levin 1998

Diabetic cervical radiculoplexus neuropathy (Massie, 2012) • Median age: 62 years old(32 -83) • Pain initial symptom followed by subacute progression of weakness and numbness • Weakness is most common presenting complaint • Involves motor, sensory and autonomic fibres • Upper, middle and lower plexus equally involved • Greater than 50% of patients had at least one other body region affected (contralateral extremity, lumbosacral, thoracic)

Diabetic cervical radiculoplexus neuropathy • May precede or present simultaneously with lower extremity symptoms • Often improves over 2 -9 months • May recur

Diabetic cervical radiculoplexus neuropathy: studies • Electrodiagnosis – Axonal neuropathy, paraspinal denervation • Snaps/cmaps decreased, ncv normal • Fibs, polys and large amplitude potentials in distribution of clinical complaints – Abnormal sensory and autonomic testing frequent • MRI reveals brachial plexus abnormality • Plexus>peripheral nerve increased T 2 signal • Nerve hypertrophy>contrast enhancement • Muscle increased T 2(edema) subacutely increased T 1 (fat) chronically

Diabetic cervical radiculoplexus neuropathy: studies • CSF protein elevated • Pathology: ischemic injury secondary to microvasculitis

Diabetic cervical radiculoplexus neuropathy: Differential Diagnosis • • • Radiculopathy Neuralgic amyotrophy Peripheral nerve CIDP Myelopathy

Brachial plexus and Malignancy • Malignancy (78%) – Primary tumor – Malignant invasion • Radiation (22%) • Kori, 1981

Brachial plexus and tumors • Primary tumors (rarely malignant) – Primarily benign: peripheral nerve sheath tumors – Neurofibroma: Upper trunk, lateral cord • Present with pain, supraclavicular mass • Occasionally mild neurologic deficit – Schwannoma • Often arise in spinal nerves • Rare neurologic deficit – Intraneural perineurioma (rare) • Slow progressive neurologic deficit

Brachial Plexopathy: malignant invasion • Breast and lung (70%), followed by lymphoma • Multiple others metastasize to upper lung before spreading to plexus (sarcoma, larynx, melanoma, bladder, etc) • (Kori et al, 1981) • Initial pain in shoulder to medial forearm/ulnar 2 fingers, can be severe in metastatic disease • Followed by weakness, sensory deficit in C 7, 8 and T 1 distribution and medial cord distribution

Brachial plexopathy: Malignant invasion • Primary tumors from head and neck may invade superior plexus • Metastasis to lymph nodes may result in patch involvement of plexus, but frequently involve lower trunk due to proximity of lateral axillary lymph nodes • Significant number of patients have epidural extension of disease • (Jaeckle, 2010)

Pancoast syndrome • Superior pulmonary sulcus tumor – Tumor at apex of lung invades lower trunk/ medial cord – Pain along medial arm – Horner’s syndrome (2/3 of patients) • Paravertebral tumor near T 1, involves the sympathetic trunk or ganglia

Brachial Plexopathy post radiation treatment • Most commonly delayed after radiation; risk is for the patient’s entire lifetime (3 months – 26 years) • Risk factors include radiation dose (>6000 rads), treatment technique and concomitant use of chemotherapy • Rare complication of a radiation-induced nerve sheath tumor of the brachial plexus (can be delayed for many years) • Radiation-induced arteritis can result in ischemia in arm and hand • (Kori et al, 1981)(Stewart, 2010)(Jaeckle, 2010)

Brachial plexopathy post radiation • Most patients have sensory and motor abnormalities • Edema in arm possible, but also seen with metastasis • Presents with pain less commonly(18%) but can be severe and can develop later (65%) (Kori, 1981) • Distribution is most commonly in upper trunk and less common “pan plexus” • Horner’s syndrome less common than in direct metastatic spread – 14% with radiation vs 56% with metastasis (Kori, 1981) • Can be progressive

Studies • Radiation plexopathy: – Emg reveals fasciculations, myokymia, axonal damage – MRI/ CT scan chest and brachial plexus may need to repeated in 4 -6 weeks if mass not seen – MRI cervical and thoracic spine if epidural spread a consideration – PET scan
Case 1 • 53 year old female • 1 -2 years of numbness in right arm • 6 weeks ago patient wakes up with severe pain in the right upper extremity – Like a blood pressure cuff in upper arm radiating to the shoulder blade, no change in numbness

Case 1 • 3 days later patient receives cervical epidural. • 3 days later patient notes weakness in right hand • 1 week later patient has pronator teres injection and pain improves although no change in weakness or numbness
Case 1 • At time of evaluation (6 weeks after onset of symptoms), no pain in cervical spine or upper extremity • Arm is stiff from elbow to hand • No change in numbness in right hand

Physical examination Cervical and shoulder mobility full 4/5 shoulder abductors, external rotators 4/5 abductor pollicis brevis 0/5 flexor digitorum profundus (median distribution) flexor pollicis longus • DTR biceps 1/ 4 bilaterally • Sensation decreased over distal volar thumb • •

Studies • Cervical MRI: small noncompressive central disc herniation at C 56 • Ultrasound : pronator teres entrapment and median nerve entrapment at wrist

EMG/NCV 6 weeks post flare • EMG – Median FDP and FPL spontaneous activity – FDP repetitive fire – FPL no voluntary potentials – APB normal, as is rest of screen • NCV – Decreased amplitude right LAC – Right Median mixed motor sensory prolonged

Actual treatment • 1 month later: – Median nerve decompression at wrist – Median and anterior interosseus neurolysis – 5 months later “good” recovery of FDP, FPL • What do you think now?

Original case • Disputed – Surgeon says pronator syndrome/anterior interrosseus syndrome • Median nerve released at the pronator teres and carpal tunnel and patient ultimately improved – I say Neuralgic Amyotrophy • Patient would have improved with or without surgery Acute, proximal pain Patchy exam LAC involvement in addition to anterior interosseus

Conclusions • History and physical is critical • MRI/EDX may help to confirm diagnosis or be a trap • Diagnosis can not be made in isolation of the history and physical
- Slides: 36