NonSquamous Laryngeal Neoplasms Patrick J Bradley MBA FRCS

“Non-Squamous Laryngeal Neoplasms” Patrick J. Bradley, MBA. , FRCS. , Nottingham 105 th Scientific Conference Taiwan Society of Otorhinolaryngology Head and Neck Surgery Taipei, Taiwan Sunday 4 rd November 2018

WHO Classification of tumours of the Larynx Epithelial Tumours Others Tumours Malignant Benign Neuro-endocrine Soft Tissue Haematolymphoid Bone and Cartilage Mucosal Melanoma Secondary

WHO Classification of tumours of the Larynx Epithelial Tumours Malignant: Squamous cell carcinoma Verucous Basaloid Papillary Spindle cell Acantholytic Adenosquamous Lymphoepithelial Giant cell Malignant salivary gland-type Mucoepidermoid Adenoid cystic Epithelial Tumours Benign: Papillomatosis Salivary gland-type adenomas Pleomoprhic adenoma Oncocytic papillary cystadenoma

WHO Classification of tumours of the Larynx Soft Tissue Tumours Malignant: Fibrosarcoma Malignant fibrous histeocytoma Liposarcoma Leiomyosarcoma Rhabdomyosarcoma Angiosarcoma Kaposi sarcoma Malignant peripheral nerve sheath Synovial sarcoma Soft Tissue Tumours Benign: Schwannoma Neurofibroma Lipoma Leiomyoma Rhabdomyoma Haemangioma Lymphangioma Granular cell tumour Borderline Tumours Inflammatory myofibroblastic

WHO Classification of tumours of the Larynx Neuroendocrine Tumours of Bone / Cartilage Typical carcinoid Atypical carcinoid Small cell carcinoma Combined small cell Chondrosarcoma Osteosarcoma Chondroma Giant cell tumour Haematolymphoid Lymphoma Non-Hodgkin Lymphoma

Malignant Tumour Location Epithelial Malignant >95% Supraglottis 35 – 45% Glottis 60 – 55% Subglottis < 10% Non-Epithelial Malignant <5% 70% 30%

Presenting Symptoms • • Dysphonia Airway restriction Dysphagia Haemoptysis Neck mass Neck pain Previous treatment – biopsy / excision

Investigation • • • Nasendoscopy Review previous biopsy material CT/MRI Angio +/- Selective angiography CT Chest / PET-CT Biopsy – Endoscopic, FNCB, Open biopsy

Treatment Approach Site Extent Histology Sensitivity of Adjuvant Therapy

Treatment • • • Biopsy and Non-Surgical Treatment (Lymphoma) TOLS / TORS Laryngofissue excision Partial laryngectomy Supra-cricoid laryngectomy Cricotracheal resection Total laryngectomy +/- Chemoradiotherapy Voice and swallow rehabilitation / TEP Follow-up

Selected Benign Neoplasms • Granular cell – arise from Schwann cells, 50% involve the true vocal cord, may be multiple lesions, excision is curative • Lipoma – complete or partially encapsulated, usually single lesions • Neurogenic – neurofibroma/schwannoma – arise form the internal branch of the superior laryngeal nerve, 80% aryepiglottic fold • Lymphatic/Vascular – haemangioma
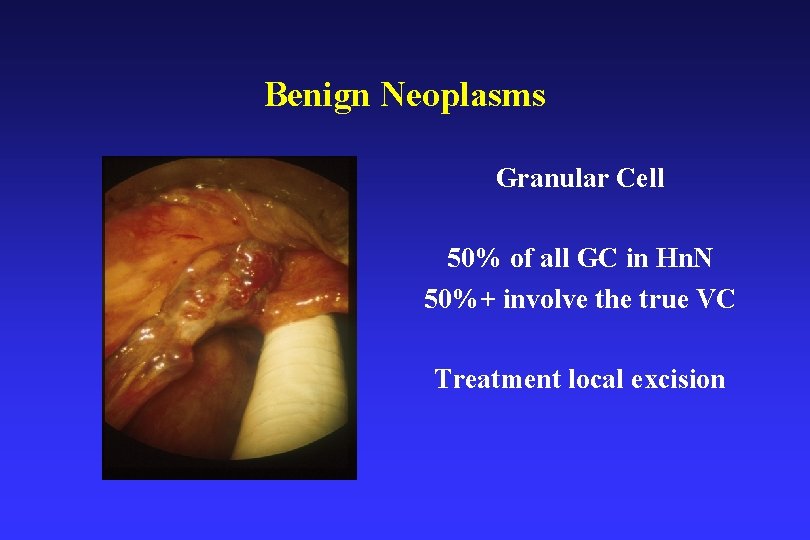
Benign Neoplasms Granular Cell 50% of all GC in Hn. N 50%+ involve the true VC Treatment local excision
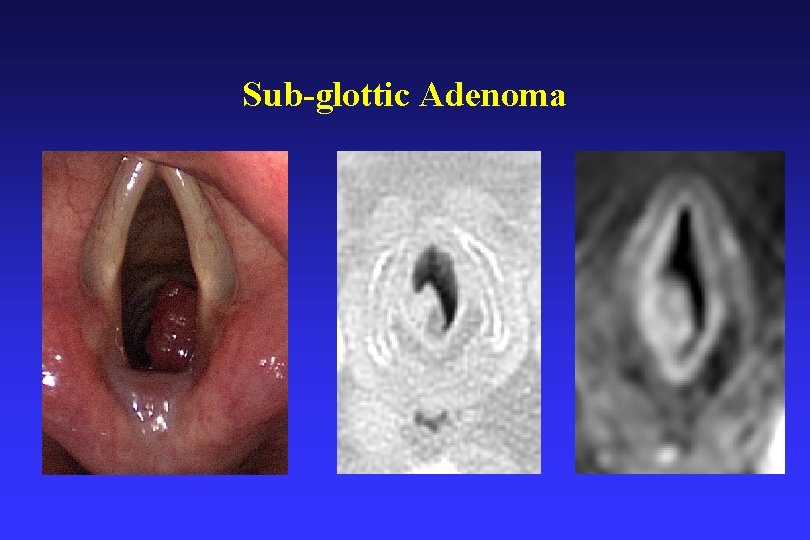
Sub-glottic Adenoma
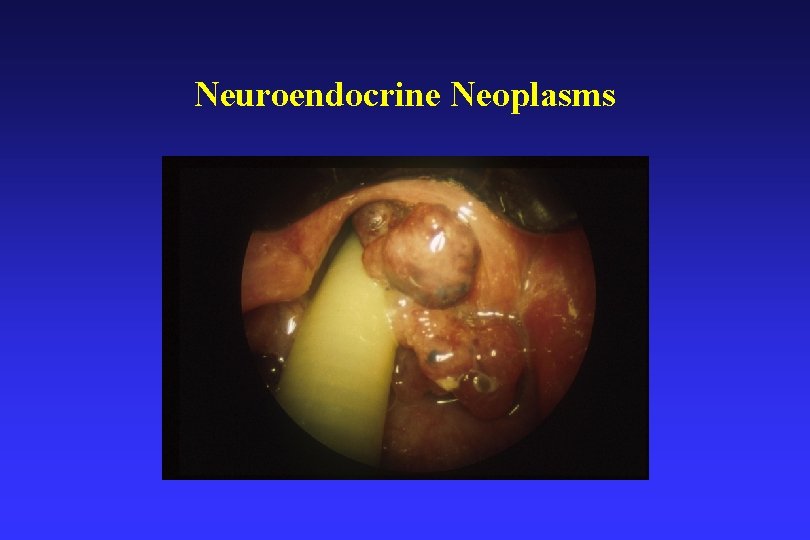
Neuroendocrine Neoplasms

Laryngeal Neuroendocrine Neoplasms • Neuroendocrine neoplasms of the larynx are a heterogeneous group of tumours (4 Subtypes). • Most common non-squamous neoplasm of the larynx • About 700+ reported • Atypical 54%, Small cell neuroendocrine type 34%, Paraganglioma 9%, and Typical 3%. • Presents as a submucosal mass or polyp • Supraglottic location – A/E fold and vicinity

Laryngeal Neuroendocrine Neoplasms Carcinoid / Small Cell Paraganglioma Epithelial Neoplasms Diagnosis: Micro, IHC/EM Neural Neoplasm Diagnosis: Micro, IHC/EM Rx: Typical Carcinoid (TC) --- Surgery + END 0 Atypical C (AC) --- Surgery + END + CRT Small Cell (SC) (M+) --- Surgery 0 CRT Rx: Wide local excision (Partial Lx or CO 2 laser) Outcome: TC – v rare, No survival figures AC -- 5 year survival > 50% SC -- 5 -year survival < 5% Outcome: Good, benign behaviour, excellent prognosis
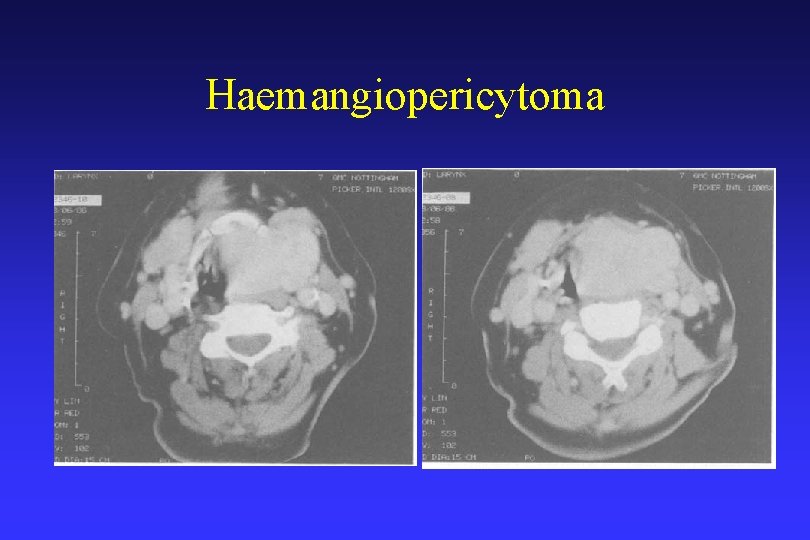
Haemangiopericytoma
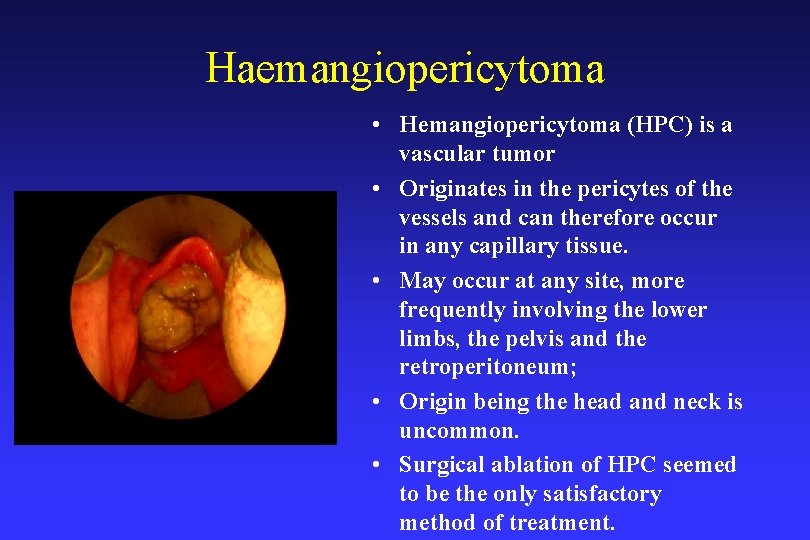
Haemangiopericytoma • Hemangiopericytoma (HPC) is a vascular tumor • Originates in the pericytes of the vessels and can therefore occur in any capillary tissue. • May occur at any site, more frequently involving the lower limbs, the pelvis and the retroperitoneum; • Origin being the head and neck is uncommon. • Surgical ablation of HPC seemed to be the only satisfactory method of treatment.
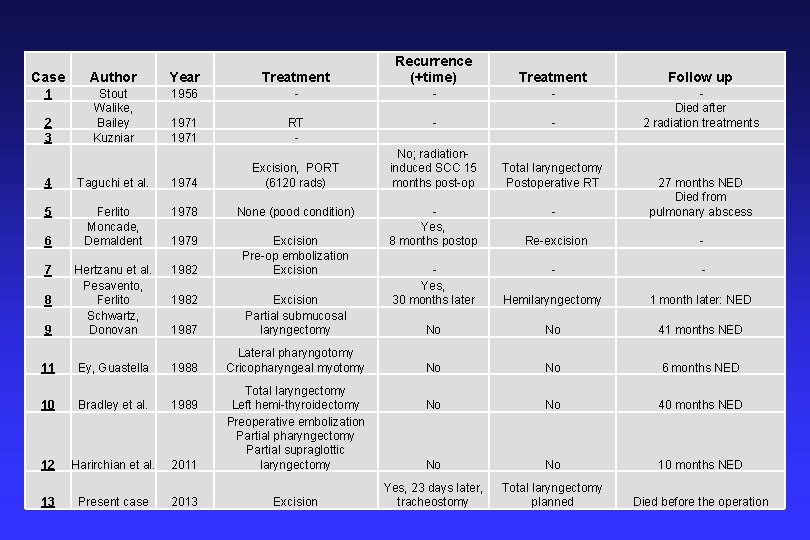
Case Author Year Treatment Recurrence (+time) 1 1956 - - - 2 3 Stout Walike, Bailey Kuzniar 1971 RT - 4 Taguchi et al. 1974 Excision, PORT (6120 rads) - No; radiationinduced SCC 15 months post-op 5 Ferlito Moncade, Demaldent 1978 None (pood condition) 1979 1982 9 Hertzanu et al. Pesavento, Ferlito Schwartz, Donovan Excision Pre-op embolization Excision 1987 Excision Partial submucosal laryngectomy 11 Ey, Guastella 1988 Lateral pharyngotomy Cricopharyngeal myotomy 6 7 8 1982 10 Bradley et al. 1989 12 Harirchian et al. 2011 13 Present case 2013 Total laryngectomy Left hemi-thyroidectomy Preoperative embolization Partial pharyngectomy Partial supraglottic laryngectomy Excision - Yes, 8 months postop Treatment Follow up - Died after 2 radiation treatments Total laryngectomy Postoperative RT - 27 months NED Died from pulmonary abscess Re-excision - - Yes, 30 months later - - Hemilaryngectomy 1 month later: NED No No 41 months NED No No 6 months NED No No 40 months NED No No 10 months NED Yes, 23 days later, tracheostomy Total laryngectomy planned Died before the operation

Salivary Gland Neoplasms • • Represent <1 % Laryngeal Tumours Usually present 4 th – 7 th Decade Benign PA Malignant ACC (32 – 69%) and MEC (15 – 35%), [80% Overall], Adenocarcinoma Most frequently located supraglottis Grade and location determine treatment choice [ACE, Age and Patient Preference] N+ -- ACC 18%, MEC ? Surgery +/- PORT

Salivary Gland Neoplasms Benign • Pleomorphic Adenoma • Supra-glottic>subglottis>g • Surgery – Endoscopic, CO 2, Open Surgery Malignant • ACC – Sub-glottic (64%), Supra -glottic (25%) MEC – Supra-glottic (57%), Glottic (30%), Sub-glottic (8%) • Sub-mucosal mass • CT and Biopsy Essential • Surgery – Laser/Partial Lx/TLx • Survival: ACC – 12 – 17% MEC – Depends G and N status
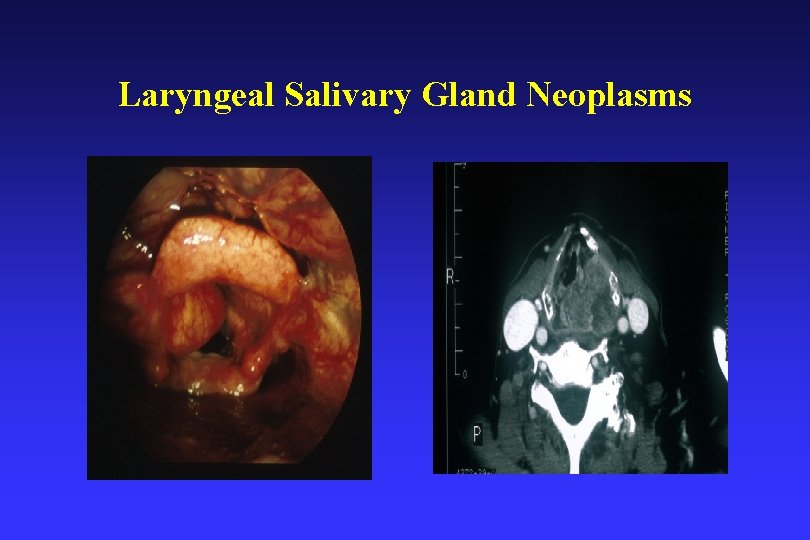
Laryngeal Salivary Gland Neoplasms
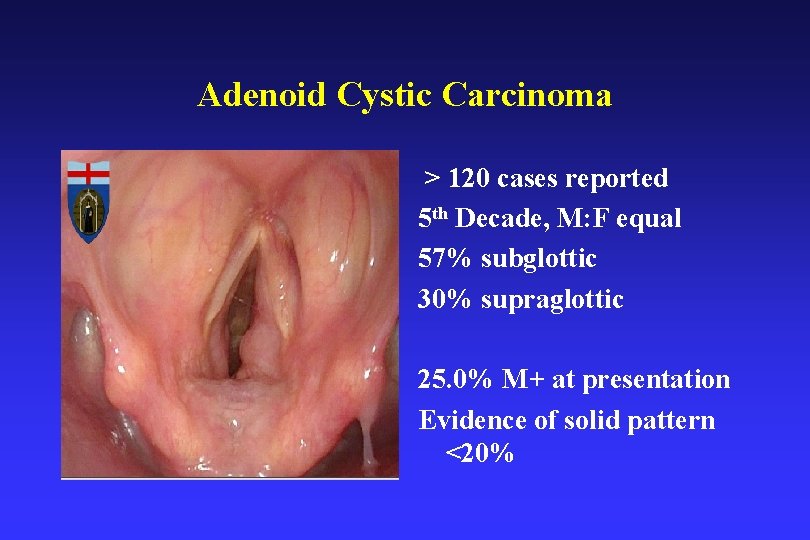
Adenoid Cystic Carcinoma > 120 cases reported 5 th Decade, M: F equal 57% subglottic 30% supraglottic 25. 0% M+ at presentation Evidence of solid pattern <20%

Chondrosarcoma (CS) • CS is the most frequent of malignant submucosal lesions • Most commonly involves the cricoid 70% +, thyroid 20%, arytenoids, epiglottis, corniculate • Presents 60 – 70 age, predominant male 3/4: 1 • Tumour differentiation (grading) – best predictor of clinical behaviour & allows treatment stratification (Well-differentiated – most common (WHO)) • The preservation of a single functioning cricoarytenoid joint will allow for reconstructive options STL - avoiding TL.
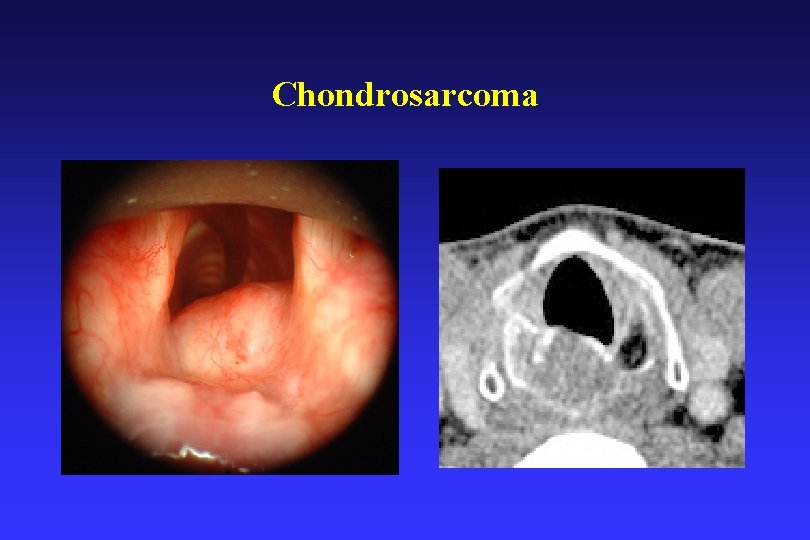
Chondrosarcoma

Other sarcomas • • • Liposarcoma – 10 M: 1 F Leiomysarcoma – Rhabdomyosarcoma – Angiosarcoma – Kaposi sarcoma – Synovial cell sarcoma – arise in the soft tissues of the thyrohyoid ligament area. • Malignant peripheral nerve sheath tumors
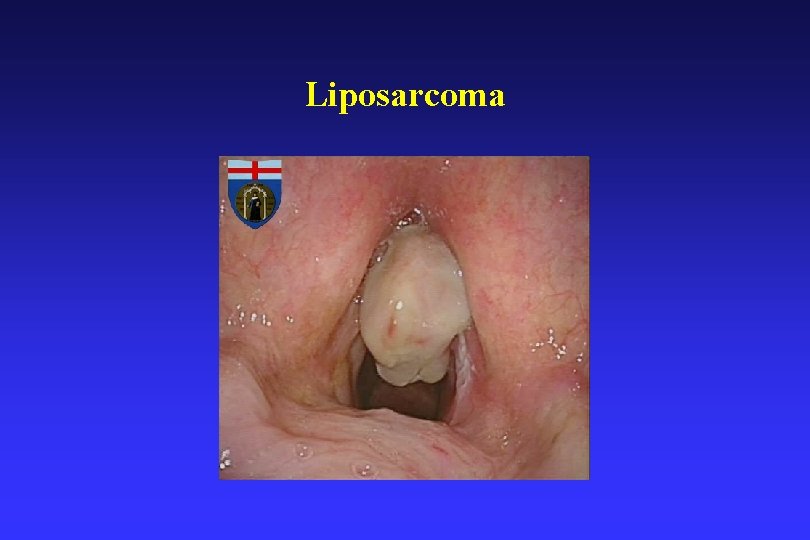
Liposarcoma
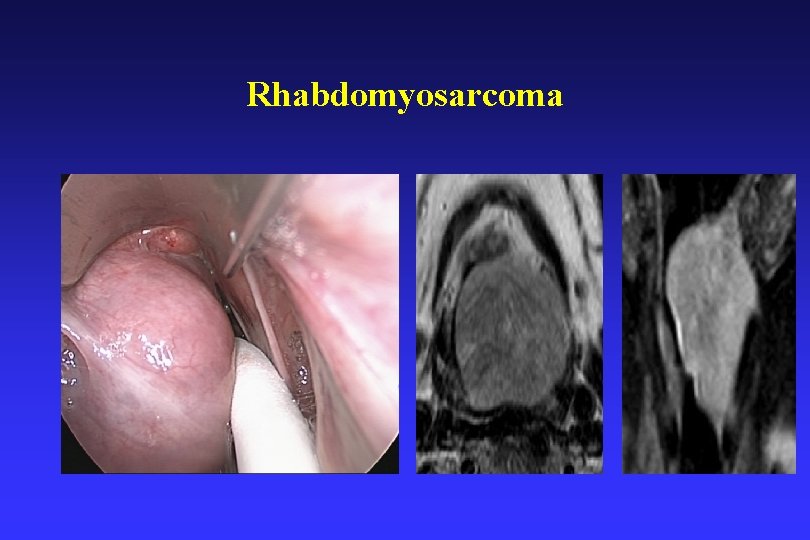
Rhabdomyosarcoma
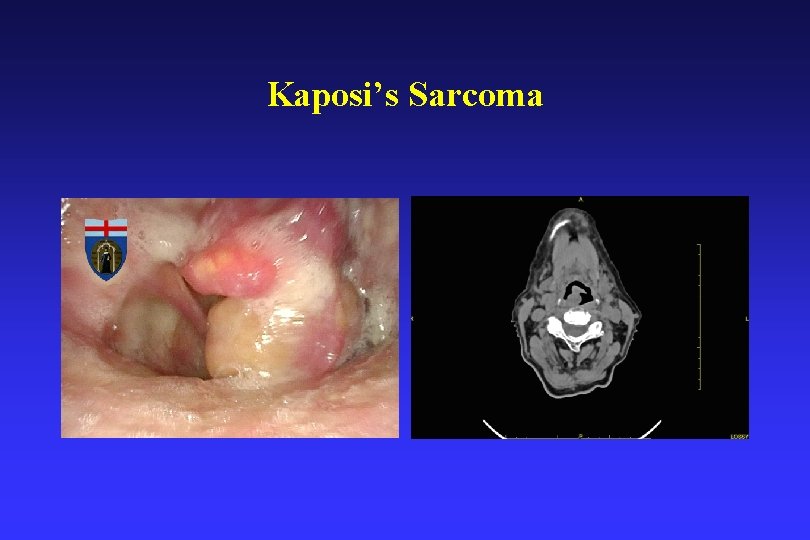
Kaposi’s Sarcoma
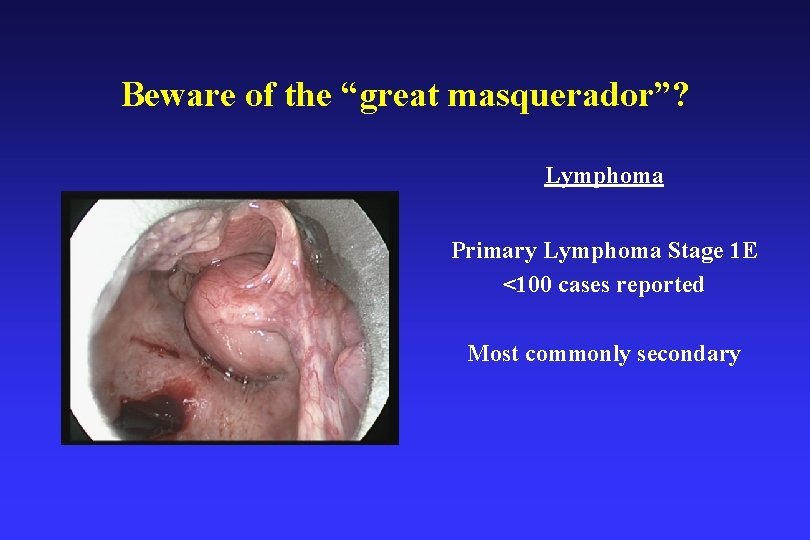
Beware of the “great masquerador”? Lymphoma Primary Lymphoma Stage 1 E <100 cases reported Most commonly secondary

SUMMARY Be suspicious if a laryngeal mass lesion presents as a submucosal mass Subepithelial lesions represent a broad spectrum of possible pathologies Histopathologists may express a reluctance to commit to an final diagnosis and may require a “bigger biopsy”

Non-Squamous Cell Tumours of the Head and Neck “Laryngeal Tumours” Patrick J. Bradley, MBA. , FRCS. , Emeritus Professor Head and Neck Oncologic Surgeon Nottingham University Hospitals United Kingdom Head and Neck Round Table 3 rd Congress of European ORL-HNS 2015
- Slides: 32