Nonspecific Host Defenses Physical barriers Cellular defense Processes
Non-specific Host Defenses • Physical barriers • Cellular defense • Processes: – Phagocytosis – Inflammation • Chemical defenses 1
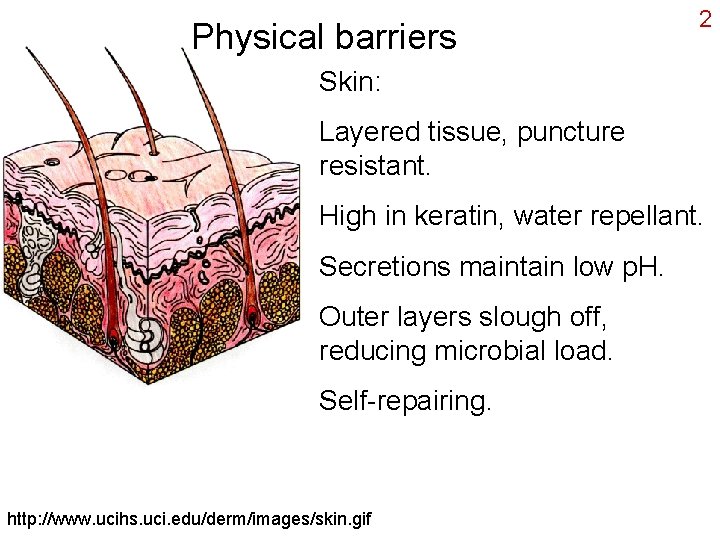
Physical barriers 2 Skin: Layered tissue, puncture resistant. High in keratin, water repellant. Secretions maintain low p. H. Outer layers slough off, reducing microbial load. Self-repairing. http: //www. ucihs. uci. edu/derm/images/skin. gif

Mucous membranes 3 Tissues lining openings to the outside: Mouth, genito-urinary tract, etc (anything pink). Easier for microbes to invade, but coated with mucus which traps microbes; this combined with some type of movement removes microbes from area: Flushing action: tears, urine, saliva, other secretions. Action of cilia: propel mucus & microbes toward GI tract or to where they can be coughed out. http: //www. ich. ucl. ac. uk/factsheets/test_procedure_operations/tonsils_adenoids_remove d/mouth. gif
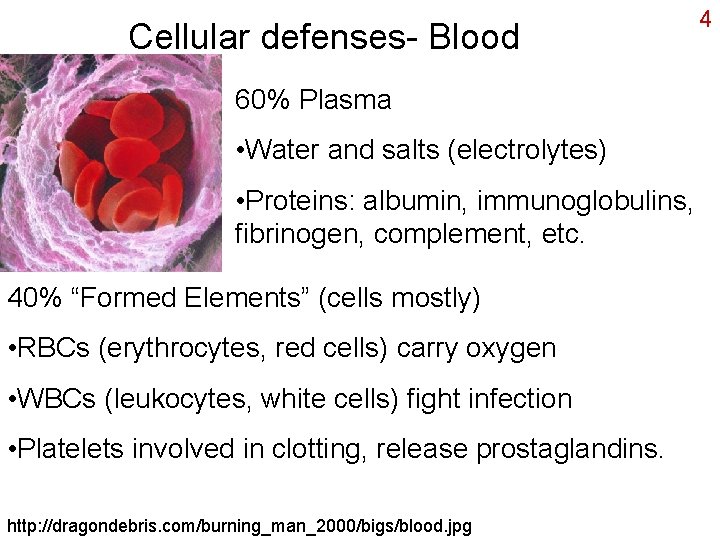
Cellular defenses- Blood 60% Plasma • Water and salts (electrolytes) • Proteins: albumin, immunoglobulins, fibrinogen, complement, etc. 40% “Formed Elements” (cells mostly) • RBCs (erythrocytes, red cells) carry oxygen • WBCs (leukocytes, white cells) fight infection • Platelets involved in clotting, release prostaglandins. http: //dragondebris. com/burning_man_2000/bigs/blood. jpg 4
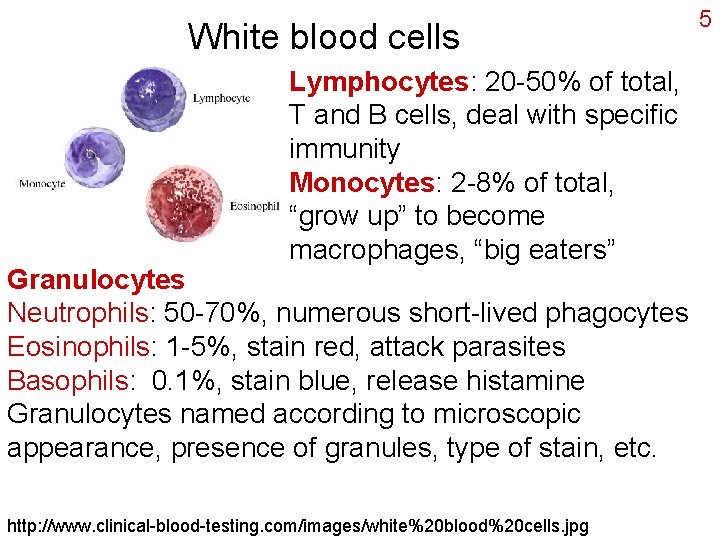
White blood cells Lymphocytes: 20 -50% of total, T and B cells, deal with specific immunity Monocytes: 2 -8% of total, “grow up” to become macrophages, “big eaters” Granulocytes Neutrophils: 50 -70%, numerous short-lived phagocytes Eosinophils: 1 -5%, stain red, attack parasites Basophils: 0. 1%, stain blue, release histamine Granulocytes named according to microscopic appearance, presence of granules, type of stain, etc. http: //www. clinical-blood-testing. com/images/white%20 blood%20 cells. jpg 5

Blood clotting 6 • Complicated pathway featuring inactive proteins becoming activated. – Prothrombin to thrombin; Fibrinogen to fibrin • Platelets respond to physical roughness, release factors that lead to clotting. • Response to endotoxin results in blood clotting within the vessels: intravascular coagulation. • Definition: Serum is plasma without the clotting factors. Allow blood to clot, result is serum. Clotting factors are used up, gone.

More about Macrophages 7 • Large and mean, clean up debris as well as microbes. • Important link between non-specific immunity and specific immunity • Wandering vs. fixed macrophages – Wandering macrophages patrol bloodstream, stepping into tissues when “called” – Fixed reside in specific organs, get fancy names like Kupffer cells, histiocytes, osteoclasts, neuroglia, depending on home.

Phagocytosis-1 8 • What and who – Cell-eating, a process by which cells engulf and destroy microbial invaders, debris, foreign material. – Neutrophils (PMNs) and macrophages are the major phagocytic cells in the body. • Steps in the Process – Chemotaxis: phagocytes respond to (move toward) various chemicals (cytokines) released by host cells and by microbes. – Attachment: cell binds to material/microbe.
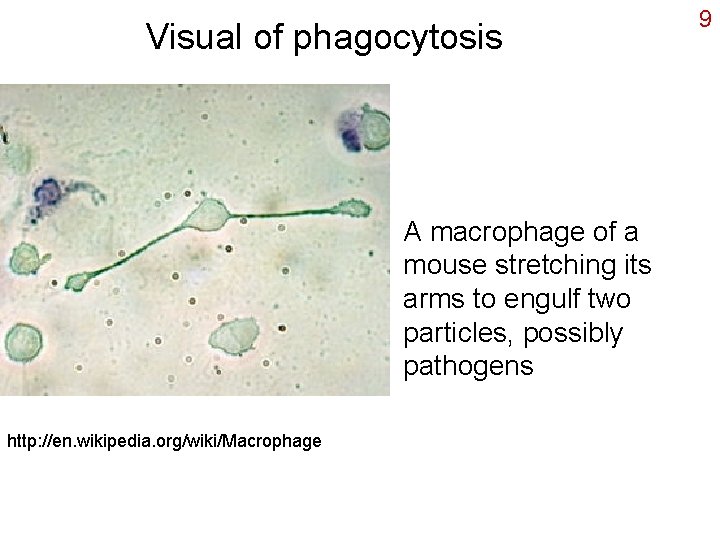
Visual of phagocytosis A macrophage of a mouse stretching its arms to engulf two particles, possibly pathogens http: //en. wikipedia. org/wiki/Macrophage 9

Phagocytosis-2 10 • Process continued – Engulfment: target brought into cell by endocytosis. Now in cytoplasm in a vesicle. – Digestion: vesicle (phagosome) containing microbe fuses with lysosome. Microbe is subjected to: • Hydrolytic enzymes, hydrogen peroxide, bleach, superoxide… • Residual, undigested material is tossed out.
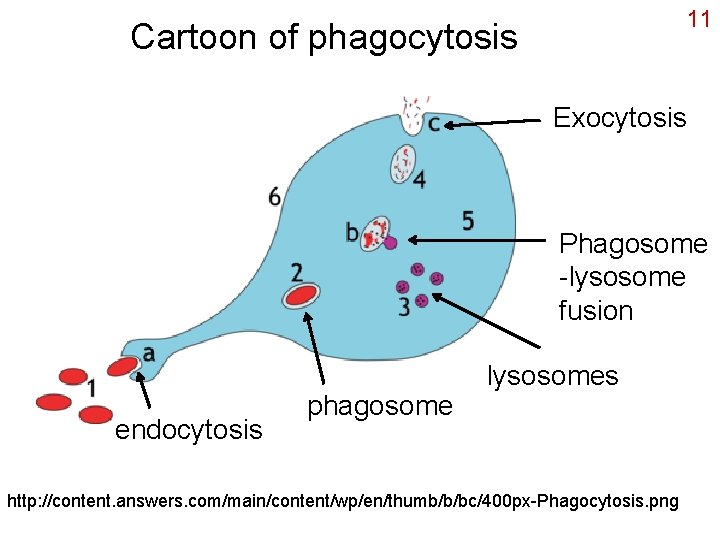
11 Cartoon of phagocytosis Exocytosis Phagosome -lysosome fusion endocytosis phagosome lysosomes http: //content. answers. com/main/content/wp/en/thumb/b/bc/400 px-Phagocytosis. png

For every step in the process, some microbe has found a way to interfere and save itself!! • Anti-phagocytic coatings – Capsules, M-protein; aren’t grabbed and engulfed • Prevent phagosome-lysosome fusion • Prevention of destruction in phago-lysosome • Hide from phagocytes by entering “nonprofessional” phagocytes. • Kill phagocytic cells – leukocidins medlib. med. utah. edu/. . . / AIDS/AIDS 030. html 12

Extracellular killing 13 • Eosinophils – Attach to parasites (protozoa, worms) larger than they are, release enzymes that attack pest. • Natural killer cells – Non-specific lymphocytes (different from T and B cells) which attack virus-infected cells and kill them. • Death of virus-infected host cells is a major way of fighting a viral infection; T cells do the same. • Also attack tumor cells

The Lymph system 14 • Parallel circulatory system – Series of vessels and nodes – Drains off excess body fluids from tissues, returns fluids to cardiovascular system – Lymph nodes filter out microbes • Nodes filled with macrophages and lymphocytes • Fluid flows thru slowly, maximizes contact • Other lymphoid tissue – Spleen, thymus, MALT/GALT, tonsils http: //www. acm. uiuc. edu/sigbio/project/updated-lymphatic/lymph_node. gif
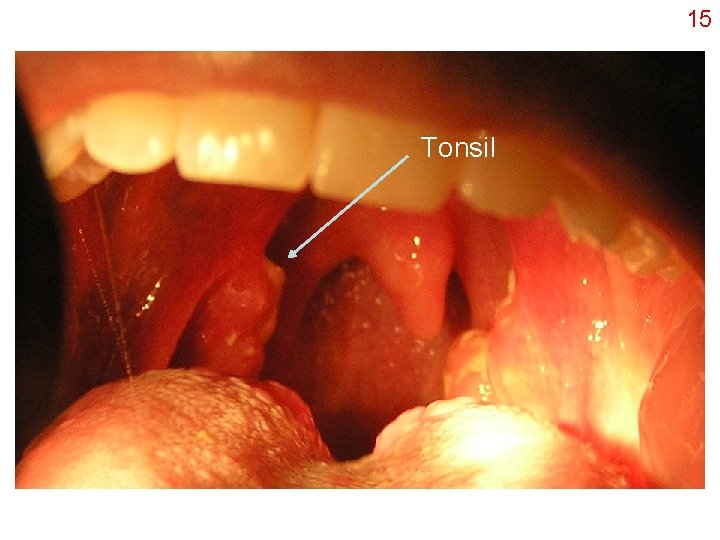
15 Tonsil

Inflammation 16 • Rubor, calor, tumor, dolor: redness, local heat, swelling, and pain. (and loss of function). • Largely all explained by increased blood flow and vessel permeability in area of injury. • Inflammation is a host response to tissue injury! – Injury doesn’t have to be accompanied by microbes, but often is in real life. – Process limits spread of microbes, brings antimicrobial factors to the area.
Inflammation-2 17 • Tissue damage activates mast cells – Mast cells release histamine, a substance that • Contracts smooth muscle • Dilates capillaries and venules – Fluid leaks into tissue, WBC line up and pass through vessel was into tissue (diapedesis) • WBCs = neutrophils THEN macrophages, move into area, carry out phagocytosis • Fibrinogen activates to fibrin, produces inflammatory barrier. Walls off microbes. – Coagulase increases; streptokinase breaks down
Inflammation-3 18 • Pus: accumulation of fluid, live and dead cells. – A pyogen promotes pus formation • Usually, pus released to outside or absorbed. • Repair: fibroblast multiply to create a patch – With minor damage, normal cells repair wound. – Too much damage, fibroblasts and fibers make up granulation tissue, leave scar. – A granuloma is a pocket of scar tissue • Chronic inflammation – Normal tissue gradually replaced by non-functional scar tissue; can eventually lead to organ failure.
Inflammation-4 19 • The signs and symptoms of inflammation are mostly explained by the vasodilation and increased permeability of blood vessels – Increased redness: more blood in area. – Edema: leakage and accumulation of fluid. – Increased heat: more blood flow from warm interior. – Pain: pressure from swelling, also chemical mediators of pain like prostaglandins, bradykinin • Inflammation is separate from Fever

Fever 20 • Pyrogen: a substance that causes fever – Exogenous pyrogen: external substance that activates the body’s temperature setting systems • LPS – Endogenous pyrogen: Interleukin-1, substance produced by macrophages – Il-1 travels to hypothalamus, changes body thermostat • Chills result from body’s attempt to warm itself to reach the new “correct temperature”.

Fever-2 21 • Fever is good for you – Raises temperature above what’s optimal for pathogen, allows host defense more time. – May inactivate toxins or enzymes. – Speeds up host metabolic rate, faster response. – Makes patient feel ill so you’ll stay home and rest! • Leukocyte-endogenous mediator (LEM) – Causes fever and hides iron. – Battle over Fe; hemolysins and siderophores vs. transferrin and LEM; you hide it, germs try to find it. • Too high a fever is dangerous, though.

Chemical defenses 22 • Secretions: – Fatty acids in sebum on skin, low p. H and are toxic – Lysozyme in tears, saliva, other fluids • Blood and fluid proteins – Complement: collection of >20 blood proteins that work in cascade fashion. • Stimulate inflammation, act as opsonins, lyse cells; work together with antibodies. – Interferon: several types, warn neighboring cells of local viral infection, induce anti-viral state. • Function also as interleukins

Microbial Antagonism • Normal Microbiota aids host defenses by – Competing w/ pathogens for nutrients – Occupying host surfaces – Killing invaders with bacteriocins – Changing conditions, e. g. p. H – Stimulating host defenses • Leaking into body, keeping defenses on alert – Producing vitamins benefiting overall host health 23
- Slides: 23