NONMALIGNANT DISORDERS OF WBCs APLASTIC ANEMIA Dr KSHEERA

NON-MALIGNANT DISORDERS OF WBCs & APLASTIC ANEMIA Dr. KSHEERA CARIAPPA ASSISTANT PROFESSOR 1

CONTENT • • • INTRODUCTION FUNCTIONS OF WBCs LEUCOCYTOSIS LEUKEMOID REACTIONS LEUCOPENIA APLASTIC ANEMIA 2
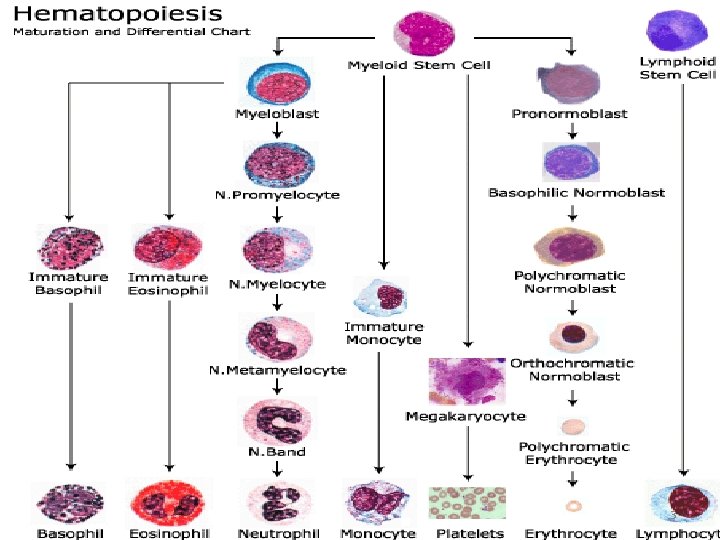
3

• FUNCTION OF WBCs NORMAL COUNT- 4000 TO 11, 000 cells/cubic mm 4

• GRANULOCYTES- 3 TYPES: - NEUTROPHILS BASOPHILS EOSINOPHILS • AGRANULOCYTES- 2 TYPES : - LYMPHOCYTES MONOCYTES 6

WBC’s 7
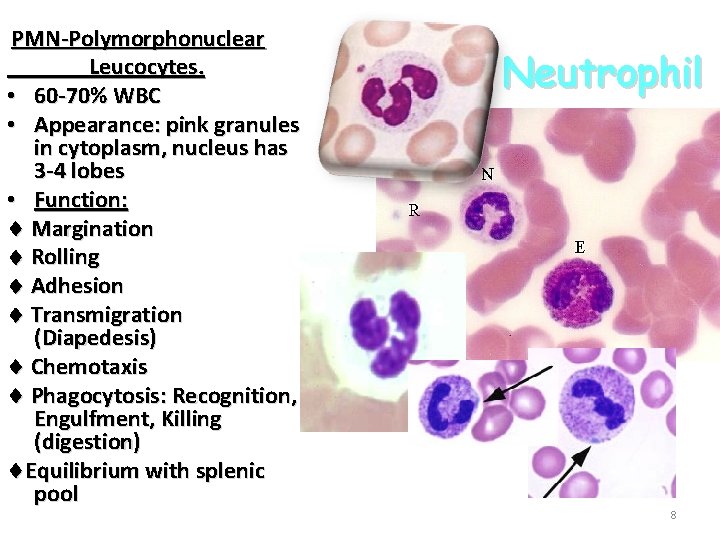
PMN-Polymorphonuclear Leucocytes. • 60 -70% WBC • Appearance: pink granules in cytoplasm, nucleus has 3 -4 lobes • Function: Margination Rolling Adhesion Transmigration (Diapedesis) Chemotaxis Phagocytosis: Recognition, Engulfment, Killing (digestion) Equilibrium with splenic pool Neutrophil 8
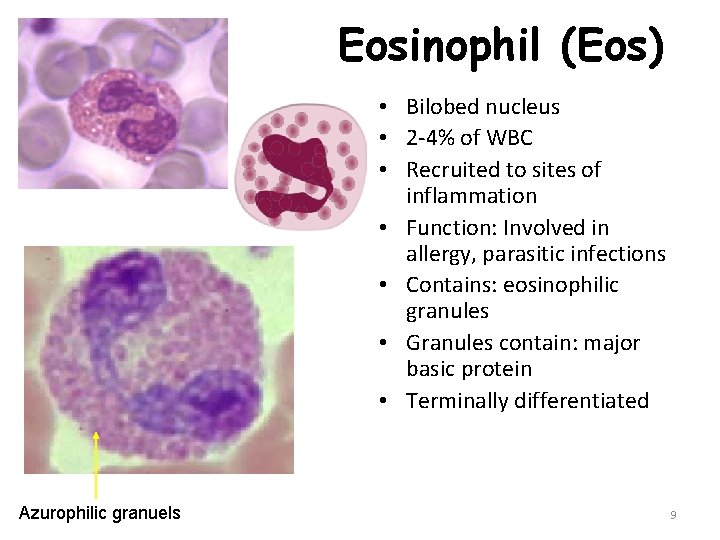
Eosinophil (Eos) • Bilobed nucleus • 2 -4% of WBC • Recruited to sites of inflammation • Function: Involved in allergy, parasitic infections • Contains: eosinophilic granules • Granules contain: major basic protein • Terminally differentiated Azurophilic granuels 9
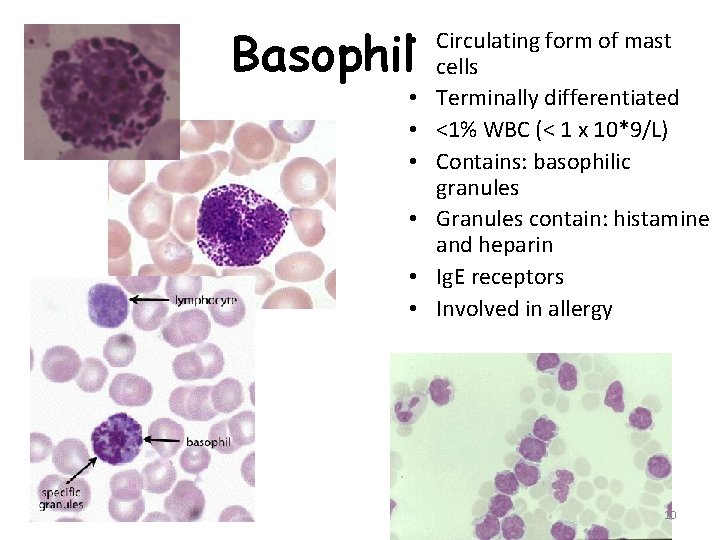
Basophil • Circulating form of mast cells • Terminally differentiated • <1% WBC (< 1 x 10*9/L) • Contains: basophilic granules • Granules contain: histamine and heparin • Ig. E receptors • Involved in allergy 10
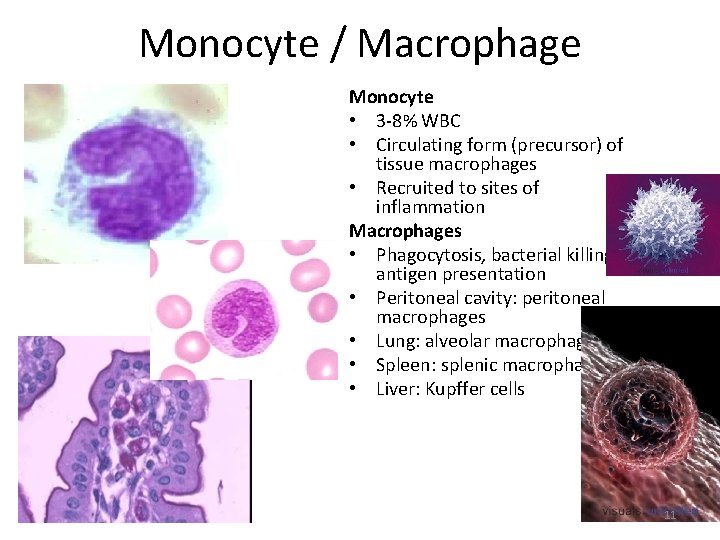
Monocyte / Macrophage Monocyte • 3 -8% WBC • Circulating form (precursor) of tissue macrophages • Recruited to sites of inflammation Macrophages • Phagocytosis, bacterial killing, antigen presentation • Peritoneal cavity: peritoneal macrophages • Lung: alveolar macrophages • Spleen: splenic macrophages • Liver: Kupffer cells 11
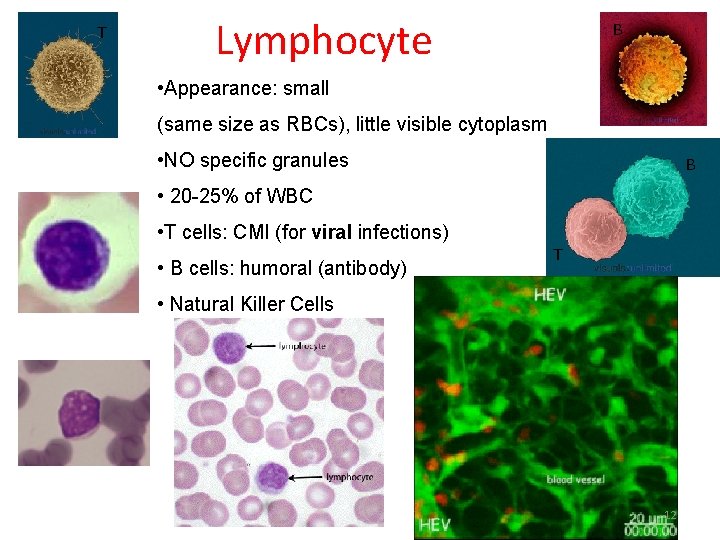
T Lymphocyte B • Appearance: small (same size as RBCs), little visible cytoplasm • NO specific granules B • 20 -25% of WBC • T cells: CMI (for viral infections) • B cells: humoral (antibody) T • Natural Killer Cells 12
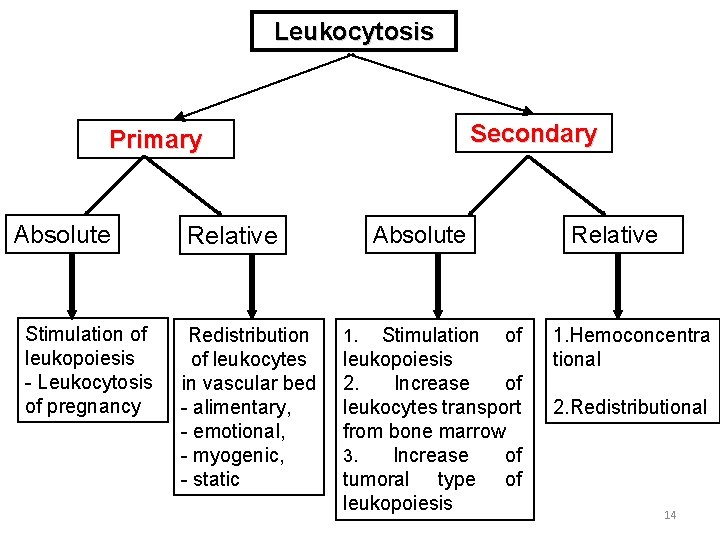
Leukocytosis Secondary Primary Absolute Stimulation of leukopoiesis - Leukocytosis of pregnancy Absolute Relative Redistribution of leukocytes in vascular bed - alimentary, - emotional, - myogenic, - static Stimulation of leukopoiesis 2. Increase of leukocytes transport from bone marrow 3. Increase of tumoral type of leukopoiesis 1. Relative 1. Hemoconcentra tional 2. Redistributional 14
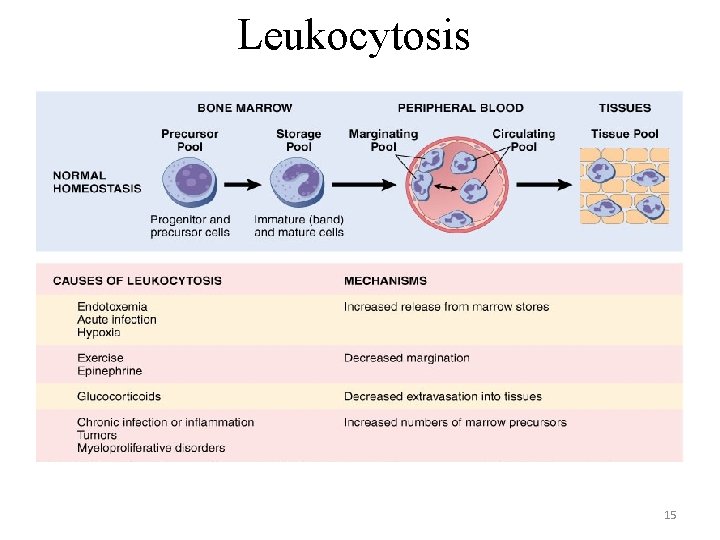
Leukocytosis 15

Leukocytosis • Neutrophilia – Acute bacterial infection, sterile inflammation • Eosinophilia – Allergy (allergic rhinitis, other hypersensitivity reactions, including drug reactions), parasites (ascaris, hookworm, strongiloides), certain skin diseases, cancer (adenocarcinoma) • Basophilia – rare (leukemia) – CML • Monocytosis – chronic infections, bacterial endocarditis, rickettsiosis, malaria, collagen vascular disorders, inflammatory bowel diseases • Lymphocytosis – some viral infections (infectious mononucleosis, hepatitis, measles), tuberculosis, CLL 16

NEUTROPHILIC LEUKEMOID REACTION Extreme neutrophilic reaction to severe infections or necrotising tissue may produce a leukemoid reaction It is a benign leucocytic proliferation. Produces a picture similar to CML. 17

LYMPHOCYTIC LEUKEMOID REACTION • Characterised by increased lymphocyte count • There is presence of immature appearing lymphocytes relative 18
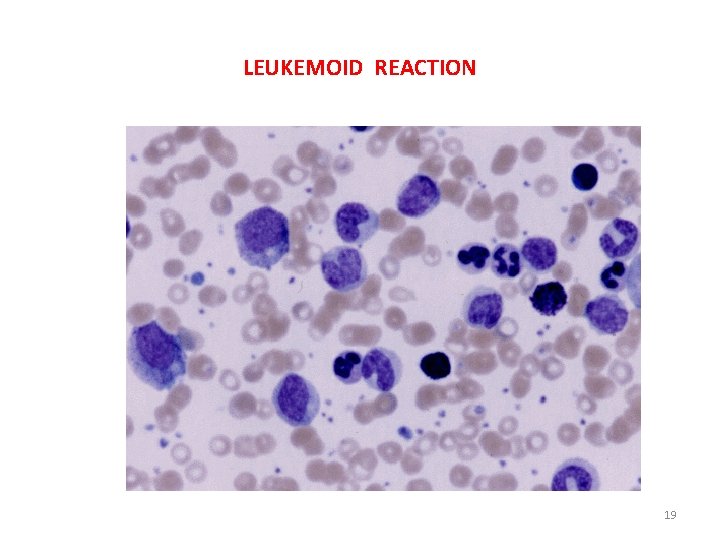
LEUKEMOID REACTION 19
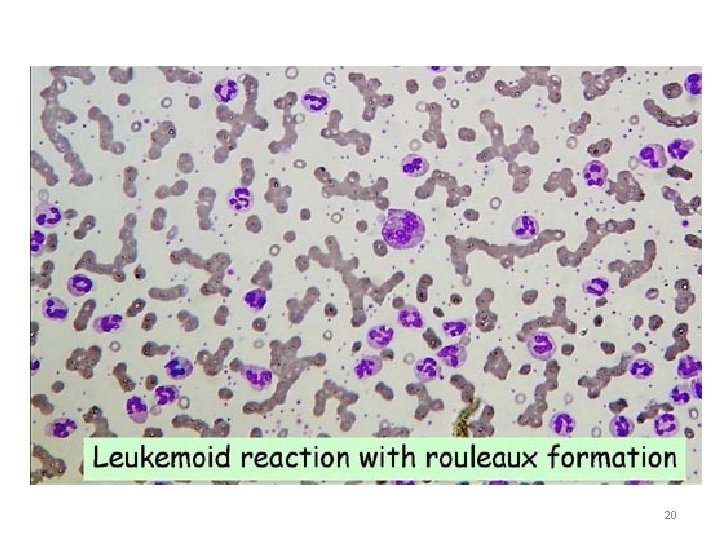
20
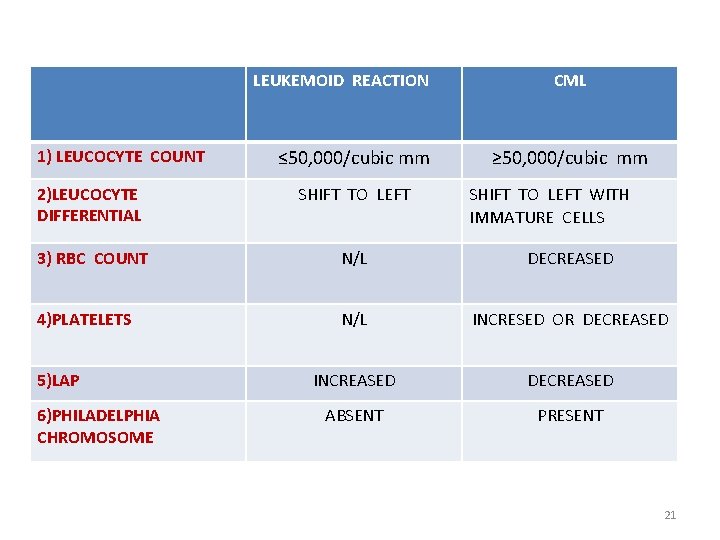
LEUKEMOID REACTION 1) LEUCOCYTE COUNT ≤ 50, 000/cubic mm CML ≥ 50, 000/cubic mm 2)LEUCOCYTE DIFFERENTIAL SHIFT TO LEFT 3) RBC COUNT N/L DECREASED 4)PLATELETS N/L INCRESED OR DECREASED INCREASED DECREASED ABSENT PRESENT 5)LAP 6)PHILADELPHIA CHROMOSOME SHIFT TO LEFT WITH IMMATURE CELLS 21

LEUKOERYTHROBLASTIC REACTION • Presence of n. RBC & neutrophilic shift to left. • Total count may be increased , decreased or normal • Associated with myelofibrosis , myelophthisis, & severe hemolytic anaemia 22
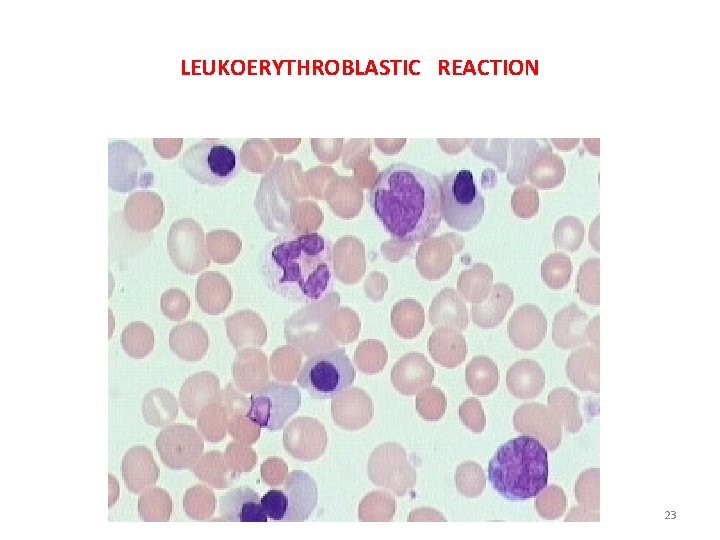
LEUKOERYTHROBLASTIC REACTION 23

Leukopenias Primary (hereditary) 1. Deficit of maturity factors - constant hereditary neutropenia -periodic hereditary neutropenia 2. Deficit of myeloperoxidase, G-6 -PD - hereditary monocytopenia with phagocytic insufficiency (disease of Chediak-Higashi) Secondary (Acquired) Absolute 1. Inhibition of leukopoiesis 2. Increase of leukodieresis 3. Increase of leukocyte destruction 4. Decrease of leukocyte emigration from bone morrow Relative 1. Redistributional e. g. shock, severe muscular workout etc. 2. Hemodilutional e. g. blood plasma, transfusion of blood substitutes etc. 24

Causes of Neutropenia Cause Mechanism Accelerated removal (e. g. , inflammation and infection) Removal of neutrophils from the circulation exceeds production Drug-induced granulocytopenia - Defective production Anticancer drugs • Phenothiazine, thiouracil, chloramphenicol, phenylbutazone - Immune destruction Aminopyrine and others • • • Predictable damage to precursor cells, usually dose dependent Idiosyncratic depression of bone marrow function Intramedullary destruction of granulocytes Immunologic mechanisms with cytolysis or leukoagglutination Periodic or cyclic neutropenia (occurs during infancy and later) Unknown Neoplasms involving bone marrow (e. g. , leukemias and lymphomas) Overgrowth of neoplastic cells, which crowd out granulopoietic precursors Idiopathic neutropenia that occurs in the absence of other disease or provoking influence Autoimmune reaction Felty’s syndrome Intrasplenic destruction of neutrophils 25

AUTOIMMUNE NEUTROPENIA(AIN) • 2 types: Primary AIN- Not associated with any other disease - Develops as antibody- coated neutrophils are destroyed by spleen Seen in young children 26

SECONDARY AIN • Seen in older patients diagonosed with other autoimmune disorders as SLE, Rheumatoid arthritis • Confirmed by testing antineutrophil antibodies or neutrophil surface antigens 27

ALLOIMMUNE NEUTROPENIA • • Occurs when there is transplacental transmission of maternal alloantibodies against infants neutrophils Also seen as a result of transfusion reaction 28

CONGENITAL NEUTROPENIA • Begins in infancy or childhood • Periodic or cyclic neutropenia occurs in regular 21 -30 days cycle. • Severe neutropenic period is marked by frequent infections 29

PSEUDONEUTROPENIA • Produced by alterations in circulating and marginating pools of neutrophils • Characteristic of infections with endotoxin production & hypersensitivity 30

SPURIOUS OR FALSE NEUTROPENIA CAUSES: - • • • Neutrophils may rarely adhere to RBCs when blood is drawn in EDTA Neutrophils disintegrate over time faster than other leucocytes. Delay in testing can lead to neutropenia Clump formation 31
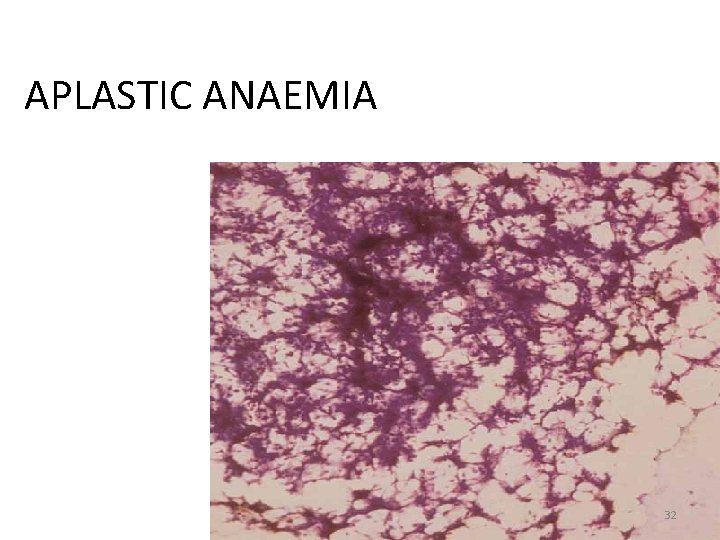
APLASTIC ANAEMIA 32

DEFINITION • Apastic anaemia is a group of disorders in which haemopoietic cells of the marrow get replaced by fat resulting in progessive cytopenias; deficiency of neutrophils and platelets may result in fatal infections or bleeding episodes. 33
• Bone marrow failure. • Decreased / absent production of normal blood cells. • Manifests as: • Decreased red cells -Anemia • White blood cells -Infections • Platelets -Bleeding complications 34

CAUSES: • CONGENITAL - Fanconi’s anaemia • ACQUIRED - Idiopathic - Drugs and chemicals: - Dose-dependent: - cytotoxic drugs, benzene - Idiosyncratic: - chloramphenicol, nonsteroidal anti-inflammatory drugs(NSAID) - Radiation 35

- Viruses: - such as hepatitis virus, Epstein. Barr virus, cytomegalovirus, parvovirus B 19, and HIV - Paroxysmal nocturnal haemoglobinuria (PNH). 36
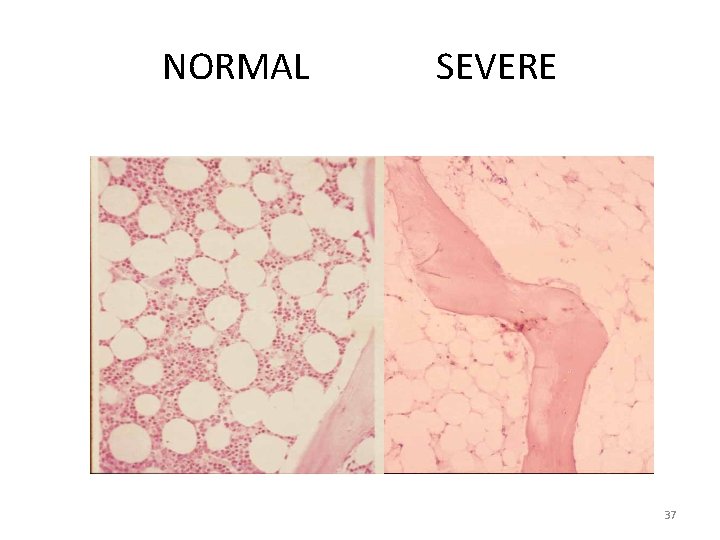
NORMAL SEVERE 37
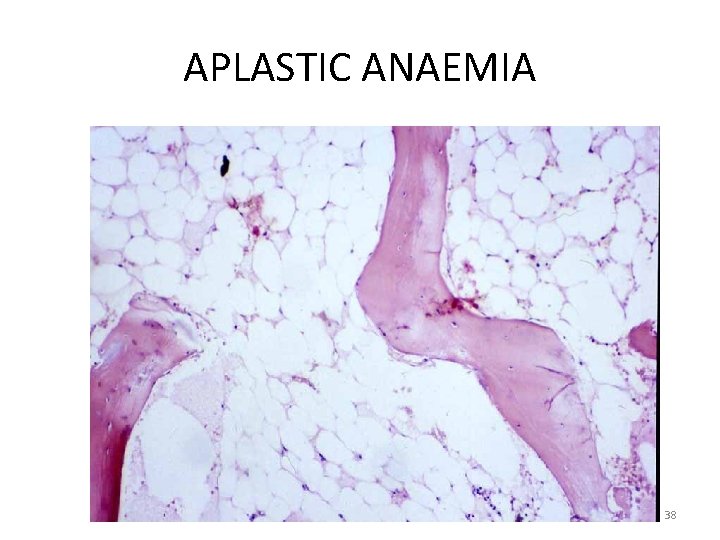
APLASTIC ANAEMIA 38

ETIOLOGY: • Aplastic anaemias may occur spontaneously or appear following exposure to viruses or drugs. • However, in about 2/3 rd of cases no etiological agent can be identified and are grouped as idiopathic type. 39

PATHOGENESIS • The mechanisms by which various agents produce aplastic anaemia are unknown. • Haematopoietic failure can result from various mechanisms: 1. Reduction in the number of stem cells in bone marrow; 2. Defective stem cells: - The causative agents affects the capacity of self-renewal, proliferation, and differentiation of stem cells; 40

3. Defective haematopoietic microenvironment that is not able to sustain normal haematopoiesis; 4. Deficiency of factors stimulating haematopoiesis; 5. Inhibition of hematopoiesis by immunological mechanisms: - Immune mediated suppression of haematopoiesis is thought to underlie majority of cases of aplastic anaemia. 41

• Response to immunosuppressive therapy supports this concept. • Activated T lymphocytes produce cytokines such as ginterferon and TNF-beta, which have been shown to suppress the growth of haematopoietic stem cells in vitro. 42

CLINICAL FEATURES • Clinical features of these patients are due to thrombocytopenia, anaemia or neutropenia. . 1. Bleeding manifestations: - thrombocytopenia results in petechial haemorrhages/ bruises/ bleeding from gums or trauma. 2. Infections: - Because of neutropenia, these patients are prone to infections of respiratory tract, and skin. 3. Progressive pallor, lassitude and feeling of tiredness from anaemia. 43

Haematological findings • Blood and bone marrow picture is similar in idiopathic and secondary aplastic anaemia. 1. Pancytopaenia: - Peripheral blood demonstrate paucity of neutrophils, platelets and red cells. • Few lymphocytes are present. • In early stages there may be single or bicytopaenia. 44

• • • The haematological findings are: Decreased Hb Decreased PCV Decreased TLC Decreased Platelet count DLC: - Neutrophils are markedly diminished and neutropenia is a reflection of severity of Aplasia. 45

2. Reticulocytopaenia: • Reticulocyte count decreased. • Reticulocyte count is markedly diminished. • It varies from 0. 05% to 1%. 46

SEVERE APLASTIC ANAEMIA • At least 2 of the following 4 criteria should be present: • Granulocytes < 0. 5 x 10^9/litre. • Platelets < 20 x 10^9/litre. • Reticulocytes <1% (corrected). • Marrow cellularity <25%. 47

• Red blood cells are normocytic normochromic. • Lymphocyte count: - In initial stages lymphocyte is normal but as the disease progresses lymphocyte count also falls. 48
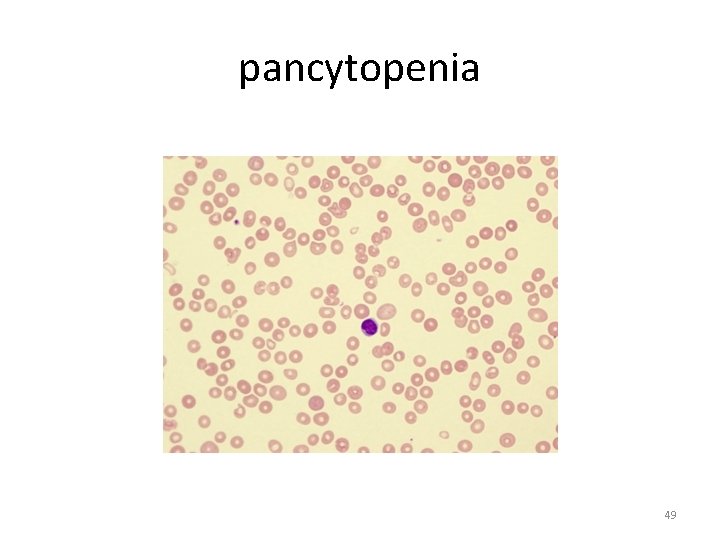
pancytopenia 49

Bone marrow • BONE MARROW ASPIRATE • Bone marrow is usually a dry tap or sometimes marrow fragments are obtained which demonstrate: • - Marked hypocellularity with replacement of marrow cells by fat in >75% of the marrow. • - Paucity of erythroid, myeloid and megakaryocytic precursors. • - Focal areas of haemopoiesis are present in initial stages. • - Lymphocytes and plasma cells are the preponderant cells in the marrow. 50

• BONE MARROW TREPHINE BIOPSY • BMB is required in cases of dry tap and also to assess the exact cellularity. The features are: • - Marked reduction in cellularity with replacement of marrow by fat. • - Infiltration of fat by lymphocytes and plasma cells. • - Increase in mast cells. • - Increased bone marrow iron. 51

Aplastic anaemia bone marrow biopsy 52

Other tests • - Urine for haemosiderin. • - Ham’s test for paroxysmal noctural hemoglobinuria(PNH). • - These tests are carried out to rule out associated PNH, both acquired aplastic anaemia and PNH being stem cell disorders. 53

Hereditary AA - Fanconi’s anaemia • Fanconi’s anemia is a genetic disease that affects children and adults from all ethnic backgrounds. - It is rare, with an overall incidence of 1 per 3, 50, 000 births. - The disease is named after the Swiss pediatrician who originally described this disorder, Guido Fanconi. - It should not be confused with Fanconi syndrome, a kidney disorder also named after Fanconi. 54

• FA is characterized by short stature, skeletal anomalies, increased incidence of solid tumors and leukemias, bone marrow failure (aplastic anemia), and cellular sensitivity to DNA damaging agents such as mitomycin C. 55

• The features of this rare disorder are: • - Inheritance as an autosomal recessive character; • - Onset of pancytopenia between the ages of 5 and 10 years; • - Frequent association with other congenital abnormalities (ex- skin pigmentation, short stature, microcephaly, skeletal defects, genital hypoplasia and renal abnormalities); 56

- Various chromosomal abnormalities (breaks, rearrangements, exchanges and endoreduplications) in cultured lymphocytes and skin fibroblasts; • - Increased number of chromosome breaks per cell culture with alkylating agents, and increased incidence of acute leukamia and solid tumours. 57

• There is usually some response to treatment with androgens and cortico-steroids. • Allogenic bone marrow tranplantation may cure the aplastic anaemia but does not prevent the appearance of solid tumours. 58

Principles of treatment • Since these patients have pancytopenia therefore the management consists of: • 1. Supportive measures • 2. Attempts to Restore marrow haemopoiesis 59

1. Supportive measures • • - Packed red cells for anaemia. - Platelets for thrombocytopenia. - G-CSF/GM-CSF to raise the neutrophil count. - Antibiotics to be used prophylactically in patients with severe neutropenia (<0. 2 x 10^9/litre). 60

2. Attempts to restore marrow activity (i). Immunosuppressive therapy: - The following drugs have been used in severe aplastic anaemia cases: • Anti-lymphocyte globulin (ALG) • Cyclosporin • Antithymocyte globulin (ATG). (ii). Androgens/anabolic steroids: • These are quite effective in some cases and preferred as a first drug to be tried in aplastic anaemia. (iii). Allogeneic bone marrow transplantation (BMT): • BMT or peripheral blood stem cell (PBSC) transfusion is the preferred treatment for young age patients. 61

Erythropoietin • - Recently, administration of recombinant human erythropoietin (r. Hu. Epo) has been reported to be an effective treatment for patients with aplastic anaemia. • - A primary AA patient complicated with end-stage renal disease, usually show marked improvement in erythropoietic cell-line as well as megakaryocytes with administration of a low dose of r. Hu. Epo after initiation of HD. 62

THANK YOU!! 63
- Slides: 61