NonInvasive Prenatal Testing NIPT Developed by Dr Judith

Non-Invasive Prenatal Testing (NIPT) Developed by Dr. Judith Allanson, Ms. Shawna Morrison and Dr. June Carroll Last updated November 2015

Disclaimer • This presentation is for educational purposes only and should not be used as a substitute for clinical judgement. GEC-KO aims to aid the practicing clinician by providing informed opinions regarding genetic services that have been developed in a rigorous and evidence-based manner. Physicians must use their own clinical judgement in addition to published articles and the information presented herein. GEC-KO assumes no responsibility or liability resulting from the use of information contained herein.

Objectives • Following this session the learner will be able to: – Refer to their local genetics centre and/or order genetic testing appropriately regarding non-invasive prenatal testing (NIPT) – Discuss and address patient concerns regarding NIPT – Find high quality genomics educational resources appropriate for primary care

Typical Prenatal Testing Algorithm Offer PN screening to all pregnant women FTS/IPS/SIPS NIPT for AMA and for women willing to pay Family history Ethnicity-based screening AMA – Advanced Maternal Age, ≥ 40 y@EDB If negative or decline 18 -20 week fetal morphology scan If positive* Refer to Genetics If indicated (e. g. fetal anomalies ) *for ethnicity-based screening, if both members of the couple are carriers of the same condition

Prenatal Testing Algorithm for Women at Increased Risk Indication Advanced maternal age, multiple soft markers on ultrasound, ultrasound anomaly, positive prenatal screen, etc. Genetic counselling with testing options Screening Test e. g. NIPT Invasive Testing (diagnostic) No further testing QF-PCR If positive Detects common aneuploidies: Down syndrome, Trisomy 18, Trisomy 13 and sex chromosome aneuploidies If positive Karyotype If negative No further testing Additional Testing e. g. Chromosomal microarray If negative Depending on indication: • No further testing • Consider additional testing

Case 1 A 32 year old woman has had a positive Integrated Prenatal Screening Test (IPS) result for Down syndrome. She is about 17 weeks gestation. – Is NIPT a good option?

Case 2 A 40 year old G 1 woman is about 9 weeks gestation. She is in your office to discuss prenatal testing options in this pregnancy conceived by IVF. – Is NIPT a good option?

Case 3 • A 29 year old patient had a nuchal translucency (NT) of 4. 4 mm at 12+5 weeks gestation • You offered NIPT and she accepted • NIPT results were normal. She is now 14+2 weeks gestation • What are the next steps?

What is Non-Invasive Prenatal Testing? • Screening test to prenatally detect Down syndrome and other aneuploidies (extra or missing chromosomes) – trisomy 21, 18, 13 – trisomy of sex chromosomes (XXX, XXY, XYY) – Turner syndrome (monosomy X) – triploidy (extra copy of all chromosomes)

What is Non-Invasive Prenatal Testing? • NIPT measures circulating cell-free DNA (cf. DNA) from placenta present in maternal blood • ‘fetal’ cf. DNA comprises ~3 -10% of DNA in maternal blood • Increases with gestational age • Companies offering NIPT use various technologies to analyze cf. DNA and determine chromosome quantities • Performed on maternal blood sample • As early as 9 weeks gestation (company specific) • Prior U/S preferable– viability, accurate GA, exclude multiples
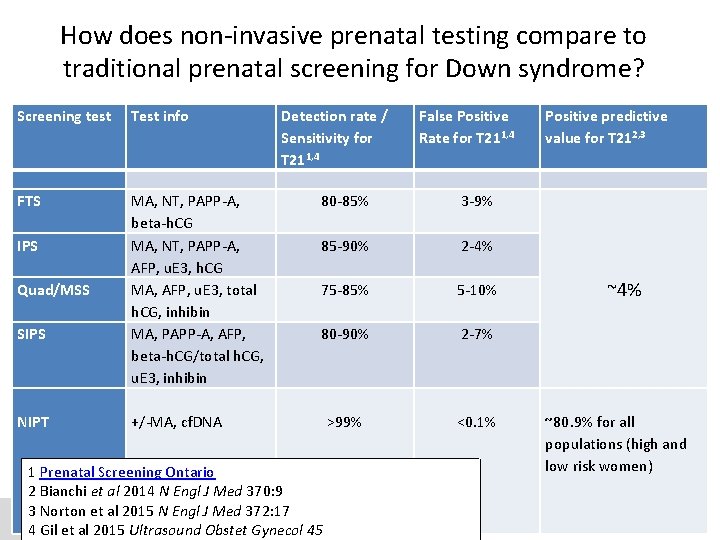
How does non-invasive prenatal testing compare to traditional prenatal screening for Down syndrome? Screening test Test info FTS MA, NT, PAPP-A, beta-h. CG MA, NT, PAPP-A, AFP, u. E 3, h. CG MA, AFP, u. E 3, total h. CG, inhibin MA, PAPP-A, AFP, beta-h. CG/total h. CG, u. E 3, inhibin +/-MA, cf. DNA IPS Quad/MSS SIPS NIPT Detection rate / Sensitivity for T 211, 4 False Positive Rate for T 211, 4 80 -85% 3 -9% 85 -90% 2 -4% 75 -85% 5 -10% 80 -90% 2 -7% >99% <0. 1% 1 Prenatal Screening Ontario 2 Bianchi et al 2014 N Engl J Med 370: 9 3 Norton et al 2015 N Engl J Med 372: 17 4 Gil et al 2015 Ultrasound Obstet Gynecol 45 Positive predictive value for T 212, 3 ~4% ~80. 9% for all populations (high and low risk women)

How does non-invasive prenatal testing perform for other common aneuploidies? Aneuploidy Trisomy 18 Trisomy 13 Monosomy X (Turner syndrome) Other sex chromosome aneuploidies Gil et al 2015 Ultrasound Obstet Gynecol 45 Detection Rate 96. 3% 91. 0% 90. 3% 93. 0% False Positive Rate 0. 13% 0. 14%

Non-Invasive Prenatal Testing (NIPT) Landscape • Offered at genetics centres all over Canada – To all vs. high risk varies • Increasing demand uptake by women • 3 separate companies, 3 separate technologies (available in Canada) • Costs about 500$ • 8 -10 days for result

Recommendations • Offer to all women: – Conventional prenatal screening using either FTS, IPS or MSS (SIPS or Quad) – Fetal morphology scan at about 18 -20 weeks gestation • Consider NIPT as an option for women who have a high risk for having a baby with an aneuploidy

Women who have a high risk for having a baby with an aneuploidy Are of advanced maternal age, defined as 40 years of age or older at estimated date of birth Have an abnormal multiple marker screen i. e. FTS/IPS/MSS Have had a previous pregnancy or child with aneuploidy

Women who have a high risk for having a baby with an aneuploidy In consultation with genetics or maternal-fetal-medicine, consider NIPT for women where: Fetal nuchal translucency (NT) measures 3. 5 mm or greater Fetal congenital anomalies on ultrasound are highly suggestive of trisomy 13, 18 or 21 Soft markers on ultrasound are highly suggestive of aneuploidy [Refer to SOGC guidelines, 2005]. There is a risk of carrying a male fetus with an X-linked condition (NIPT would be used for sex determination)

Non-Invasive Prenatal Testing (NIPT) results • Results will be reported in various ways and may be worded as: – positive or negative – aneuploidy detected, no aneuploidy detected or aneuploidy suspected/borderline value – high risk or low risk • Labs that report the chance of aneuploidy commonly use “>99%” as indicative of high risk and “<1/10, 000” as indicative of low risk, intermediate results are also occasionally reported

Non-Invasive Prenatal Testing (NIPT) results Negative result: Low risk • Your patient should still be offered: – Fetal morphology scan at 18 -20 weeks’ gestation – Referral for genetic and/or maternal fetal medicine consultation, which may be indicated for additional counselling and testing, depending on the reason your patient qualified for NIPT (e. g. increased NT) – As per SOGC guidelines, MS-AFP should only be offered to pregnant women with a pre-pregnant body mass index ≥ 35 kg/m 2 or when geographical or clinical access factors limit timely and good quality ultrasound screening

Non-Invasive Prenatal Testing (NIPT) results Positive result: High risk • Genetic counselling • Confirmation by diagnostic testing • Consider the positive predictive value (PPV) – www. perinatalquality. org/Vendors/NSGC/NIPT/ • No irrevocable obstetrical decisions should be made in pregnancies based on abnormal NIPT results alone without confirmatory invasive testing (CVS or amniocentesis) - SOGC

NIPT and PPV www. perinatalquality. org/Vendors/NSGC/NIPT/
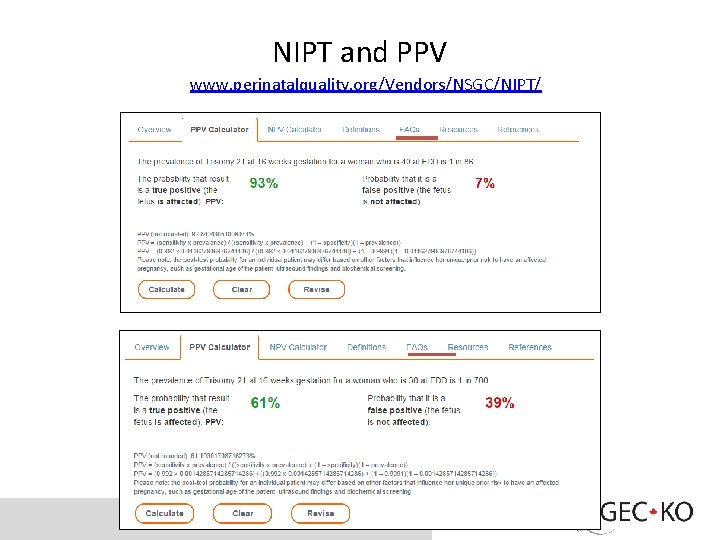

NIPT and PPV www. perinatalquality. org/Vendors/NSGC/NIPT/
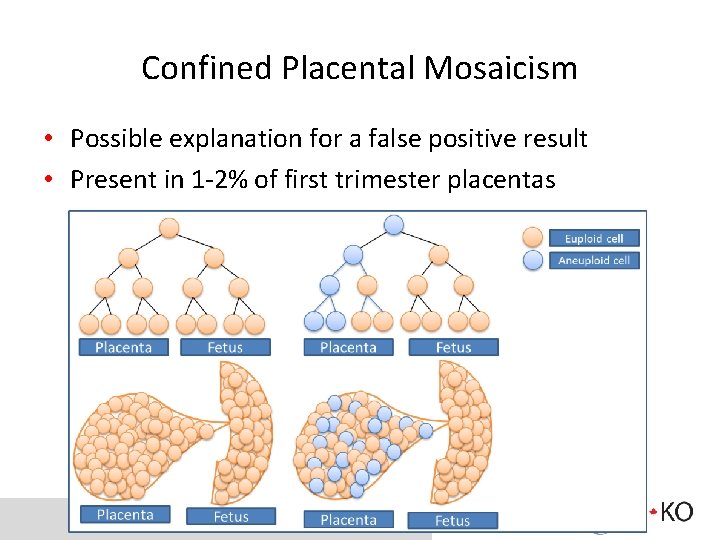
Confined Placental Mosaicism • Possible explanation for a false positive result • Present in 1 -2% of first trimester placentas

Benefits of Non-Invasive Prenatal Testing (NIPT) • Fewer women having diagnostic tests with associated risk of pregnancy loss • Increased access • Early test result (drawn at ≥ 9 -10 weeks at earliest) • No risk of miscarriage • Detects the most common chromosomal aneuploidies • Higher detection rates and lower false positive rates than IPS or MSS

Limitations of Non-Invasive Prenatal Testing (NIPT) • NIPT cannot: – Detect chromosome differences other than aneuploidy of chromosomes 13, 18, 21, X and Y • some companies are now adding screening for other trisomies and certain microdeletion syndromes – Completely rule out aneuploidy – Detect single gene conditions – Detect congenital anomalies • Possibility of no result (~6%) – 1/2 - 2/3 can be successfully resolved with redraw at later gestation – False positives and false negatives – Twins and IVF pregnancies

Non-Invasive Prenatal Testing (NIPT) and counselling • Pre- and post-test counselling is important – Invasive testing following positive results – Conditions tested for in addition to T 21 – Incidental findings • Consult genetics if unsure – www. Genetics. Education. ca has more information, links to companies and sample completed forms • Refer for genetic counselling when appropriate

Ordering Non-Invasive Prenatal Testing (NIPT) www. geneticseducation. ca Educational Resources > GECKO on the run > NIPT Harmony Prenatal Test™ by Ariosa Diagnostics through Dynacare Panorama™ by Natera through Lifelabs Genetics Verifi® Prenatal Test by Verinata through Mount Sinai Services Inc. and Medcan Clinic in Toronto

Expansion of non-invasive prenatal testing • In October 2013 one company expanded their NIPT test menu to include screening for microdeletion syndromes (e. g. 22 q deletion/Di. George) and trisomies associated with early pregnancy loss (e. g. trisomy 16) and in spring 2014 others followed suit 22 q. org – Teddy Bohan, 3 y

Expansion of non-invasive prenatal testing Arguments for NIPT with microdeletions now • Clinically relevant microdeletions and duplications occur in 11. 7% of all structurally normal pregnancies • Incidence is independent of maternal age • Cumulatively these disorders are common – The combined at-birth incidence of the 5 commonly offered microdeletion syndromes is approximately 1 in 1, 000 • Less women are expected to have invasive procedures and be offered microarray, so these conditions should be added to NIPT
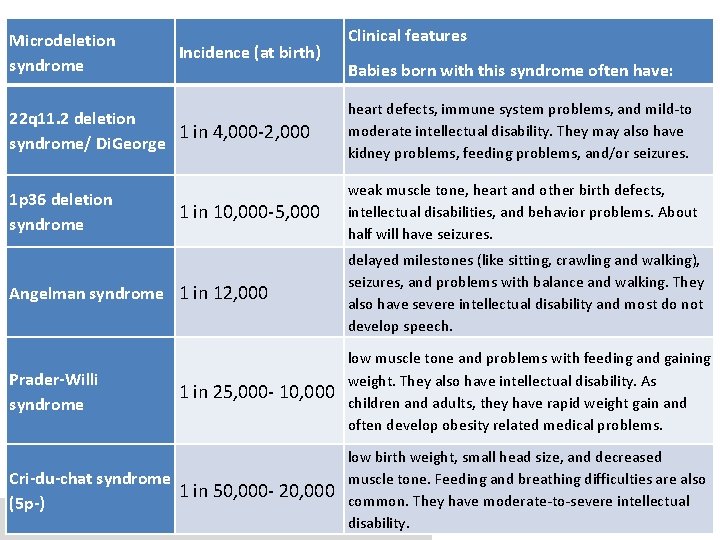
Microdeletion syndrome Incidence (at birth) Clinical features Babies born with this syndrome often have: 22 q 11. 2 deletion 1 in 4, 000 -2, 000 syndrome/ Di. George heart defects, immune system problems, and mild-to moderate intellectual disability. They may also have kidney problems, feeding problems, and/or seizures. 1 p 36 deletion syndrome weak muscle tone, heart and other birth defects, intellectual disabilities, and behavior problems. About half will have seizures. 1 in 10, 000 -5, 000 Angelman syndrome 1 in 12, 000 delayed milestones (like sitting, crawling and walking), seizures, and problems with balance and walking. They also have severe intellectual disability and most do not develop speech. Prader-Willi syndrome 1 in 25, 000 - 10, 000 low muscle tone and problems with feeding and gaining weight. They also have intellectual disability. As children and adults, they have rapid weight gain and often develop obesity related medical problems. Cri-du-chat syndrome 1 in 50, 000 - 20, 000 (5 p-) low birth weight, small head size, and decreased muscle tone. Feeding and breathing difficulties are also common. They have moderate-to-severe intellectual disability.

Expansion of non-invasive prenatal testing Arguments against NIPT with microdeletions now • There are no published clinical validation studies, only proof of concept • There are no guidelines – not considered standard of care • Because these are low-prevalence disorders, false positive results are inevitable and the positive predictive value will be low – Undermine benefit of NIPT reducing the number of women undergoing invasive testing – Uncertainty about the prenatal prevalence • Informed consent – Familiarity with rare conditions – Familiarity with testing limitations • E. g. 22 q - 85% of individuals with 22 qdeletion will have typical full deletion screened for by NIPT while 15% will have ‘nested’ deletions within the region; ~ 65 -70% of Angelman syndrome is caused by (maternal) deletions at 15 q 11. 2 screened for by NIPT while others will have various other genetic mechanisms • Provinces are not currently funding
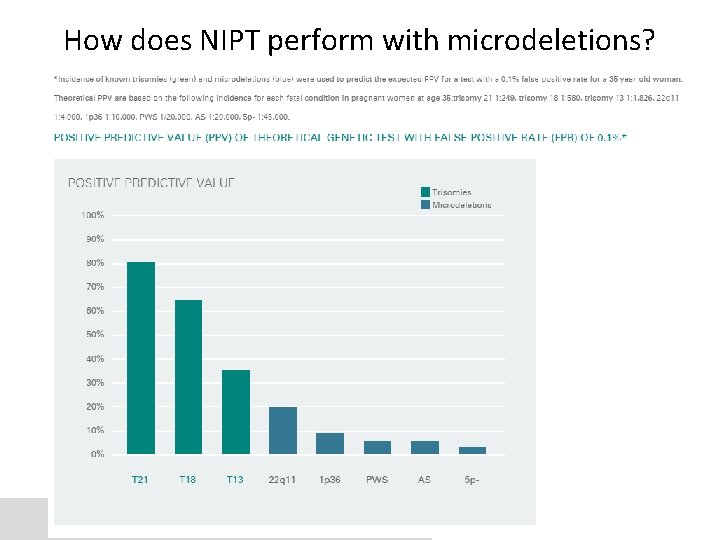
How does NIPT perform with microdeletions?

Back to case 1: IPS positive, 17 W GA Is NIPT a good option? • Yes – She is at high risk to have a baby with aneuploidy • May be eligible for provincial funding where applicable • But consider: – In the event of an abnormal result, is termination of pregnancy an option for the couple? – More rapid result from amniocentesis, consider GA • If NIPT is positive, guidelines recommend confirmatory diagnostic testing by amniocentesis – delays timing for diagnosis – What is her IPS risk? • 1 in 2 versus 1 in 120

Back to case 2: 40 yo G 1 Is NIPT a good option? • Yes – Advanced maternal age (greater than 40 years at EDB) is an appropriate indication for NIPT – Covered by some provincial health plans – Better screen than IPS – Earlier result – Decreased chance with NIPT that patient would receive screen positive result

Back to case 3: NT 4. 4 mm, low risk NIPT What are the next steps? • Genetic counselling is recommended • Patient likely to be offered: – – Chromosomal microarray Genetic testing for other single gene conditions Level II ultrasound Fetal echocardiogram

Non-Invasive Prenatal Testing Pearls • Consider offering NIPT to high risk women • Consider NIPT as a screen of higher sensitivity than current screening if your patient is willing to pay for the test • Not a diagnostic test, diagnostic testing should follow a positive result • Not an all purpose genetic test, only gives info on specific chromosomes, and so not indicated in all circumstances

Resources • See www. geneticseducation. ca for more details and how to connect to your local genetics centre and the GECKO on the run resource for more information • For a recent review on NIPT see Cuckle H, Benn P, Pergament E. Cell-free DNA screening for fetal aneuploidy as a clinical service. Clin Biochem 2015; [Epub ahead of print]
- Slides: 36