Noninvasive Pacing What You Should Know Hey Maybe

Noninvasive Pacing – What You Should Know

Hey! Maybe we should try pacing!

Evidence Based Medicine What articles or literature support the use of pacing in the Pre-hospital arena?

The Original Pacing Study!

Other Important Papers on Pacing • “Prehospital TCP for symptomatic bradycardia” • Pacing and Clinical Electrophysiology, 1991 • 51 pts tot. , 27 paced • Survival to dischg if palpable pulse on paramedic arrival? 80% in TCP vs 0% (p=0. 02) • TCP clearly benefits the bradycardic pt with pulse • “The Benefits of Electricity: TCP in EMS” • Emerg. Med. Svcs, 2002 • Informational article supporting the use of TCP in the bradycardic patient and now also in children

ACLS Guidelines • Last revised in 2005 • Emphasis on early pacing for symptomatic bradycardia • Initial pacing method of choice in emergency cardiac care • Quickly initiated and least invasive
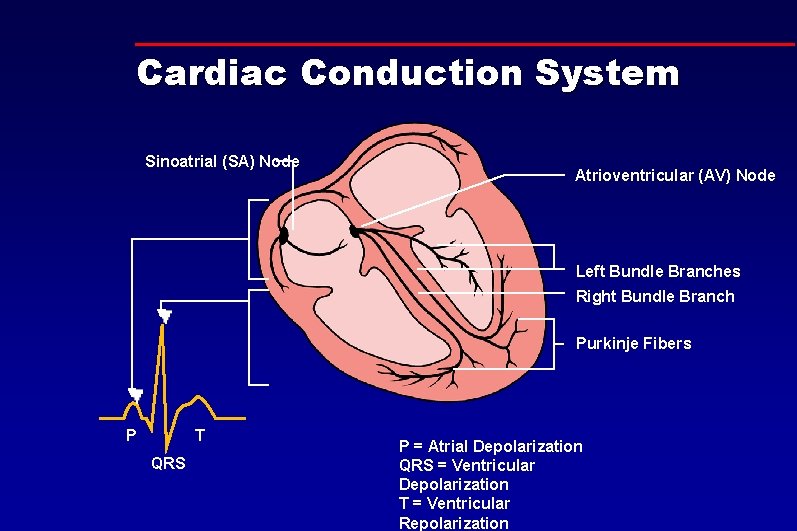
Cardiac Conduction System Sinoatrial (SA) Node Atrioventricular (AV) Node Left Bundle Branches Right Bundle Branch Purkinje Fibers P T QRS P = Atrial Depolarization QRS = Ventricular Depolarization T = Ventricular Repolarization

Failure of the Conduction System • May occur anywhere in the system • The farther down the system – the slower the heart rate • Multiple causes • Results – bradycardia – asystole

Treatment of Symptomatic Bradycardia • Atropine • Noninvasive pacing (Class 1 intervention) • Dopamine • Epinephrine

Asystole • Pacing is no longer recommended for aystole

MVEMSA Pacing Protocol • INDICATIONS: – Symptomatic Bradycardia – 3 rd degree Complete Heart Block or 2 nd degree Mobitz type 2 • RELATIVE CONTRAINDICATIONS: – Hypothermia – Hemodynamically stable awake patients. – Non-intact skin at the site of the electrode placement

Temporary Pacing Techniques üEpicardial üTransesophageal üTrancutaneous

Noninvasive Pacing • Self-adhesive electrodes applied to the skin • Advantages – easily initiated by nurse, paramedic and MD – not invasive/cost effective – used when invasive pacing is contraindicated / undesirable • Disadvantages – discomfort

Applications for Noninvasive Pacing • Emergency Use • Alternative to invasive pacing • Standby Use

Emergency Use of Noninvasive Pacing • Therapeutic bridge to stabilize the patient and plan further care – symptomatic bradycardia unresponsive to drugs – cardiac arrest

Standby Use of Noninvasive Pacing • Patient is clinically stable but may decompensate – cardiac patient undergoing surgery – acute MI with heart block – permanent pacemaker surgery – cardiac catheterization/angioplasty – post cardioversion bradycardias • We WILL NOT be using Pacing for these purposes!

Pacing Procedure • Preparing the patient and family • ECG electrode placement • Pacing electrode placement • Selecting the rate, mode and current • Assessing for capture

Preparing the Patient and Family • Explain procedure – discomfort with cutaneous nerve and skeletal muscle stimulation • Sedation or analgesia often needed

ECG Electrodes • Skin prep – remove excessive chest hair – clean, dry, and gently abrade skin • Place ECG electrodes away from pacing electrodes • Use quality ECG electrodes

Pacing Electrodes • Skin prep important – clip excessive chest hair – clean skin with soap and water – dry skin and gently abrade • Place pacing electrodes on clean, dry skin
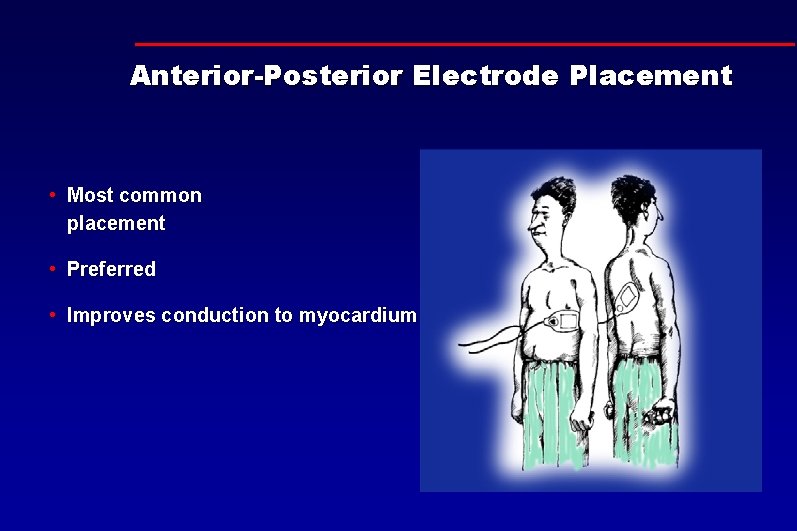
Anterior-Posterior Electrode Placement • Most common placement • Preferred • Improves conduction to myocardium
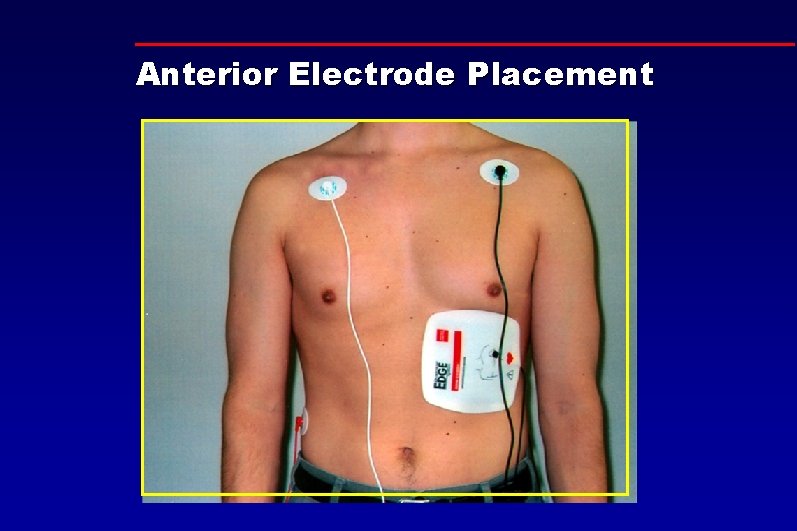
Anterior Electrode Placement
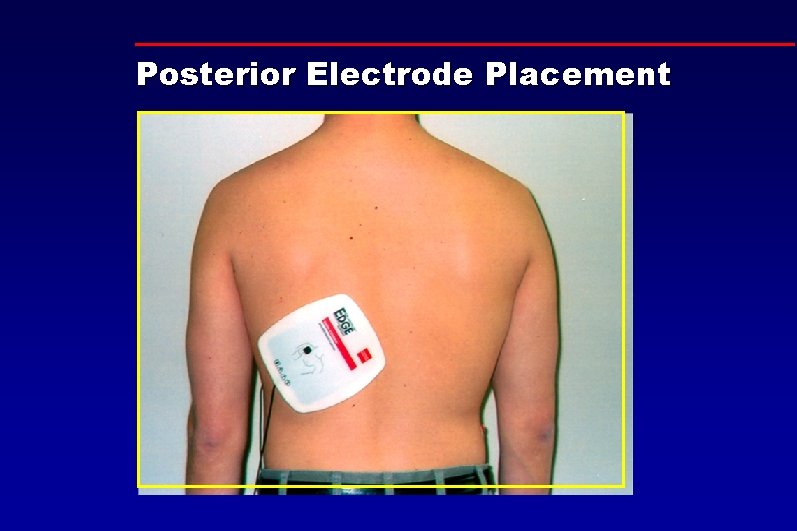
Posterior Electrode Placement
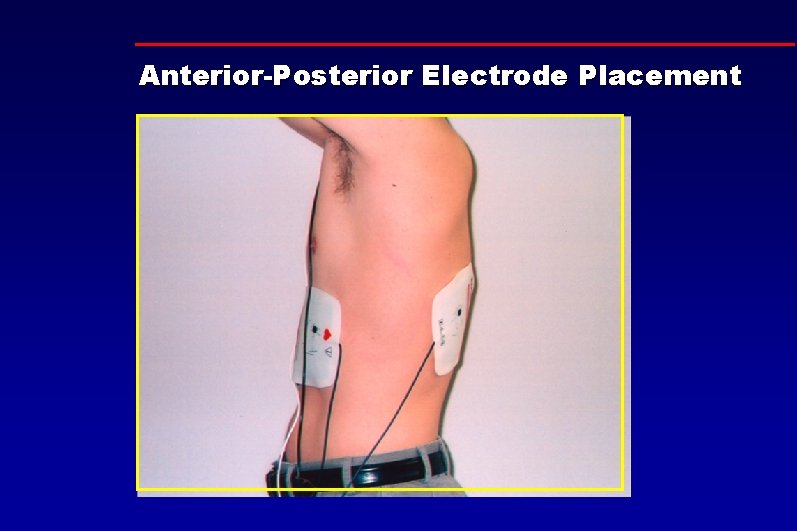
Anterior-Posterior Electrode Placement
Anterior-Lateral Electrode Placement • Alternate placement • Convenient placement in cardiac arrest • Usually the SECOND choice
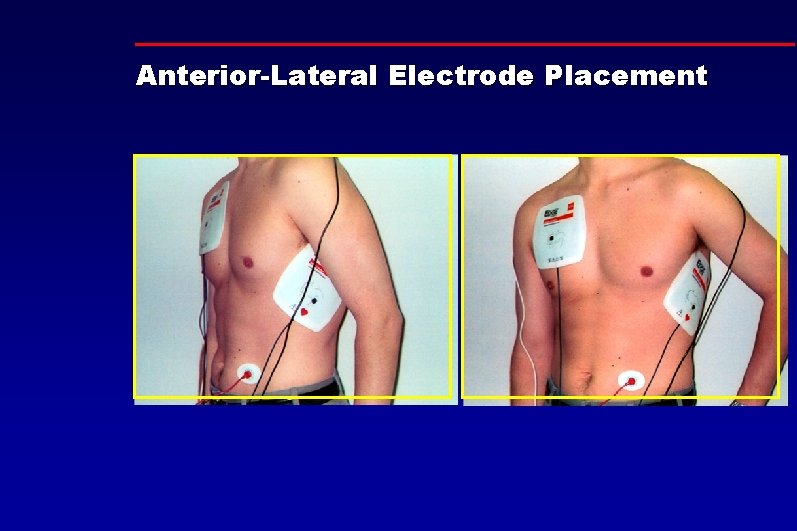
Anterior-Lateral Electrode Placement

Noninvasive Pacing Modes • Demand • Non-demand (asynchronous or fixed)

MVEMSA Protocol • Assemble the required equipment. • Explain the procedure to the patient. • Connect the patient to a cardiac monitor and obtain a rhythm strip. • Obtain baseline vital signs.

MVEMSA Protocol • Provide for patient sedation using Versed 2 mg slow IV push, titrate in 1 mg increments, to a maximum of 6 mg. DO NOT delay pacing to give sedation if the patient is critically ill and such delay may cause a detriment in patient’s care. • Apply pacing electrodes (avoid large muscle masses) and attach the pacing cable and pacing device, per manufacturer’s recommendations. • Select the pacing mode to demand or non-demand mode, if applicable. • Set the pacing rate to 80 BPM. • Set the milliamps (m. A) at zero.

MVEMSA Protocol • Activate the pacing device and increase the milliamps as tolerated (observe the patient and ECG) until capture is achieved (capture is the point when the pacemaker produces a pulse with each QRS complex). • Obtain rhythm strips as appropriate. • Continue monitoring the patient and anticipate furtherapy.
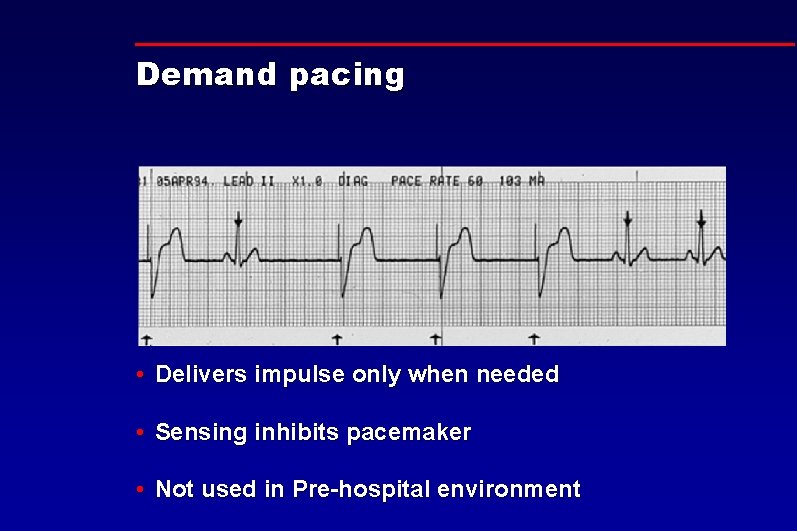
Demand pacing • Delivers impulse only when needed • Sensing inhibits pacemaker • Not used in Pre-hospital environment
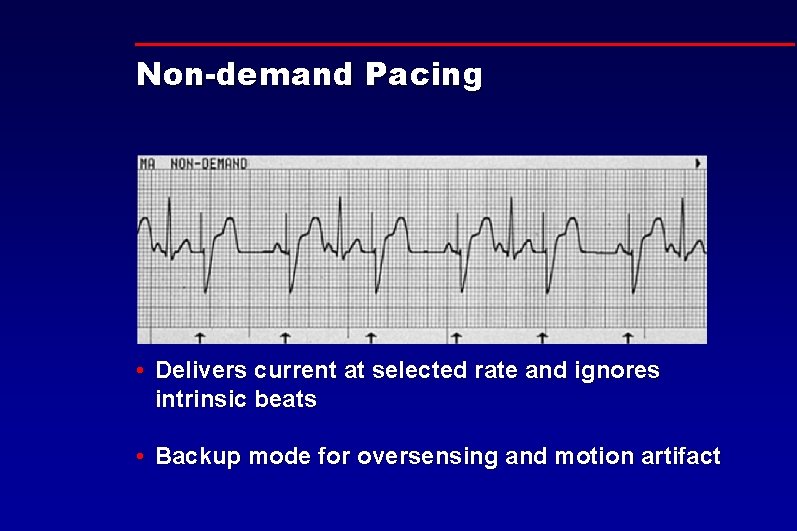
Non-demand Pacing • Delivers current at selected rate and ignores intrinsic beats • Backup mode for oversensing and motion artifact

Selecting Rate and Current • Assure proper QRS sensing • Set pace rate high enough for adequate perfusion • Increase current (m. A) until electrical capture

Access Pacer (Green) mode (Zoll) The Pacer (Green) mode is accessed by turning the Selector Switch counterclockwise Milliamps are the type of current which are utilized in this mode No AED capability or ANALYZE button can be used in this mode

Pacer Mode: Rate Dial • Pacer markers (PPM) indicate the rate set to attempt to capture the ventricle • Default settings of 70 PPM and 0 m. A are displayed upon access of Pacer Mode • To increase or decrease pacer marker (PPM) turn the Pacer Rate Dial

Pacer Mode: Output Dial • Turn the Pacer Output dial to adjust the level of discharged milliamps. • If capture is achieved, the PPM will have a wide complex reflecting ventricular contraction following the thin PPM rate marker

Assessing for Capture • Electrical capture – depolarization of the ventricles – confirmed by ECG display • Mechanical capture – contraction of the myocardium – confirmed by pulse and improved cardiac output • Both must occur to benefit the patient
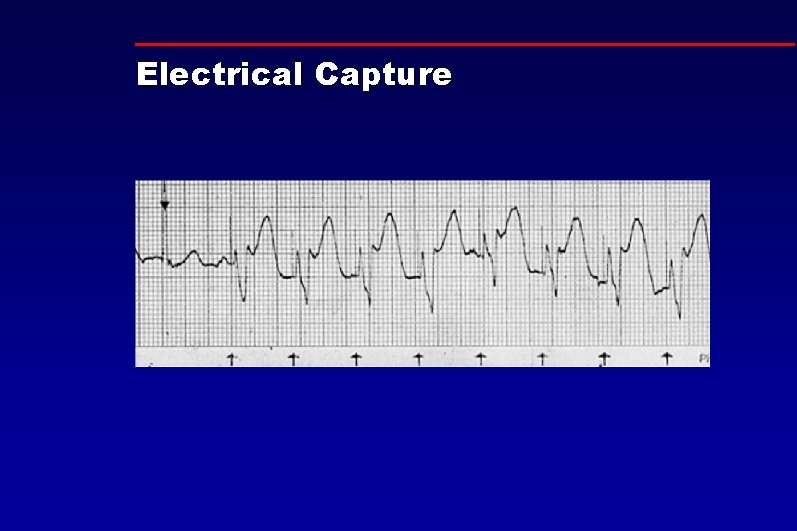
Electrical Capture
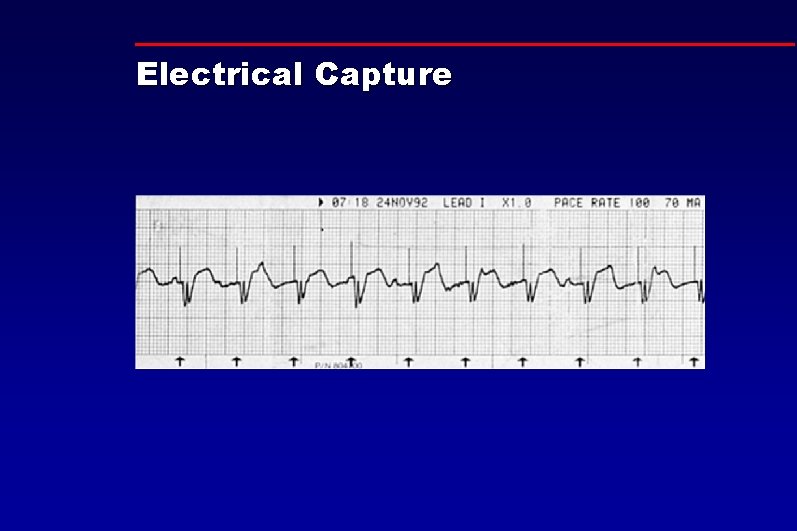
Electrical Capture
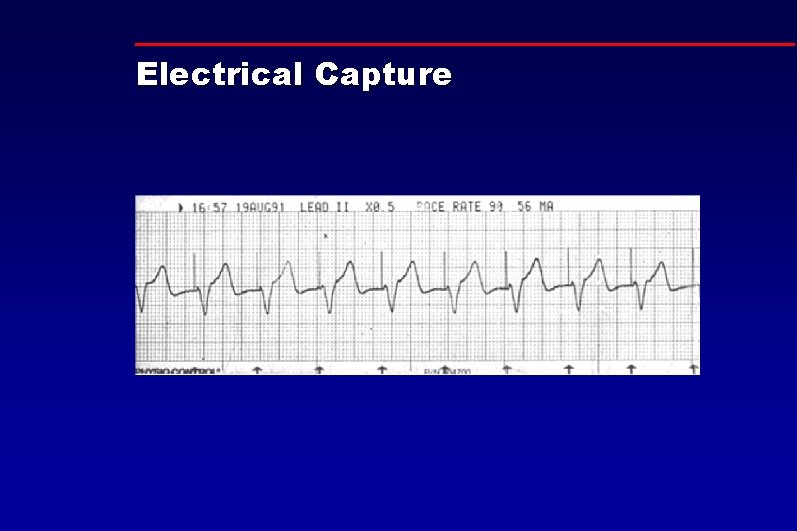
Electrical Capture
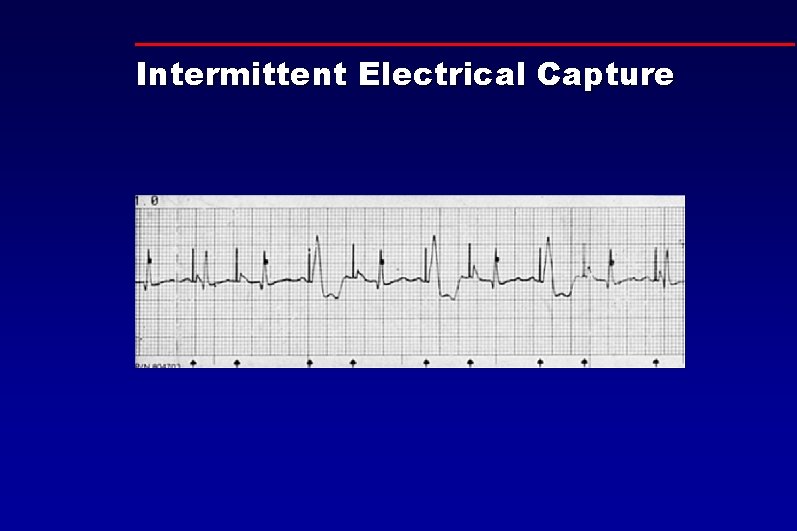
Intermittent Electrical Capture
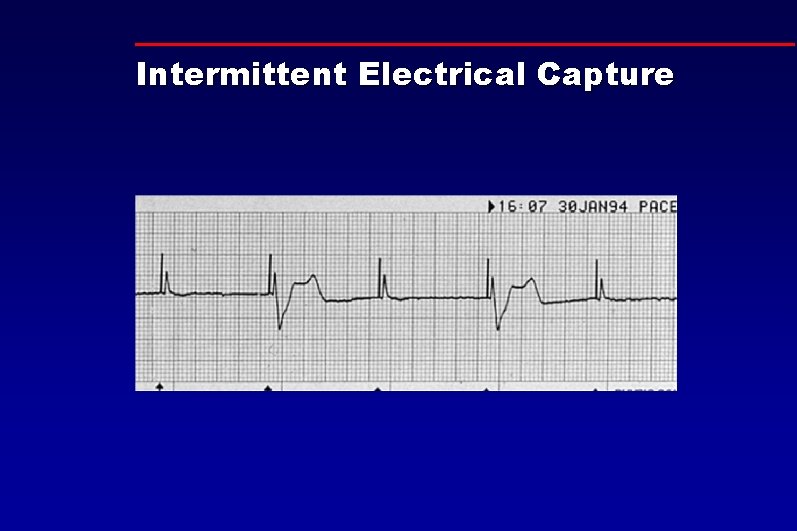
Intermittent Electrical Capture
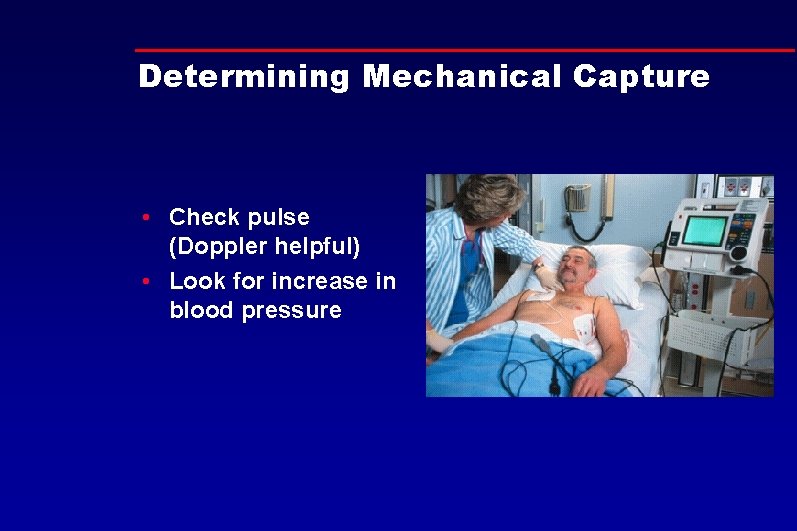
Determining Mechanical Capture • Check pulse (Doppler helpful) • Look for increase in blood pressure

Determining Mechanical Capture • Use of pulse oximetry during pacing may assist in determining capture • PLEASE DON’T FORGET THIS IMPORTANT POINT!
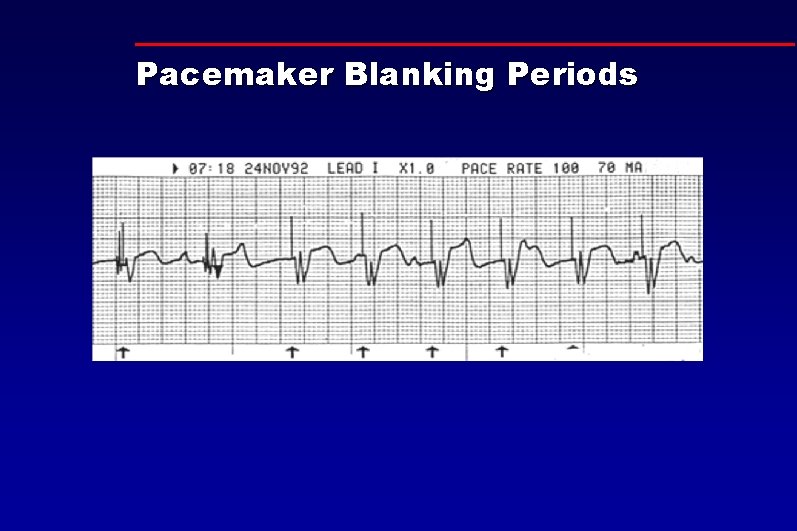
Pacemaker Blanking Periods

Artifact During Pacing • Artifact may mimic electrical capture
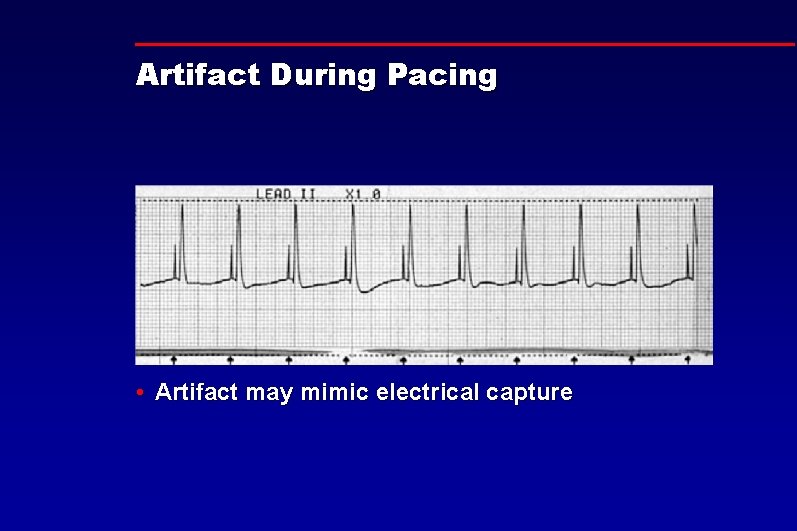
Artifact During Pacing • Artifact may mimic electrical capture

Artifact During Pacing • ECG electrodes pick up artifact from pacing current • Artifact is sometimes displayed on monitor • May mask VF and distort response to pacing • Blanking period attempts to filter out artifact and limit distortion of ECG signal

Troubleshooting • Discomfort • Failure to capture • Undersensing • Oversensing

Discomfort • Explain procedure • Reposition anterior electrode • Use sedation or analgesia

Failure to Capture • Increase current • Reposition electrode across precordium • Correct metabolic acidosis, hypoxia • Check pacemaker function

Factors Possibly Leading To High Capture Thresholds • Hypoxia • Acidosis • Air, fluid in the chest • Emphysema, pericardial effusion • Positive pressure ventilation • Ischemia • Mild Hypothermia
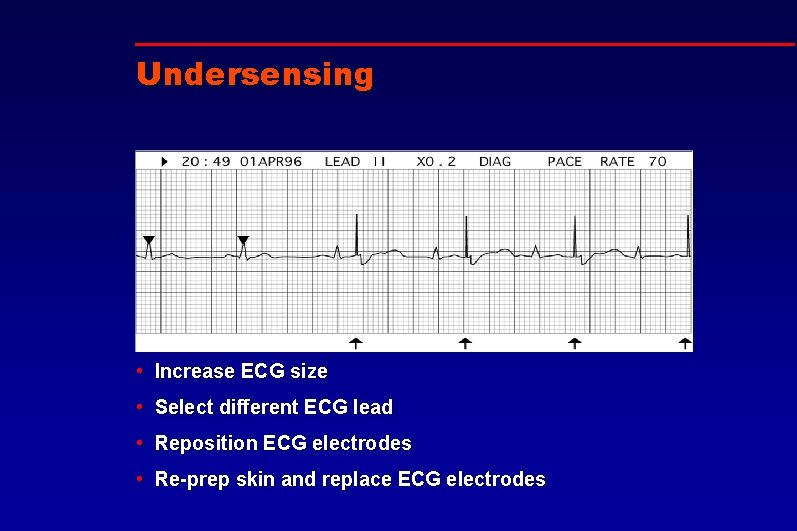
Undersensing • Increase ECG size • Select different ECG lead • Reposition ECG electrodes • Re-prep skin and replace ECG electrodes
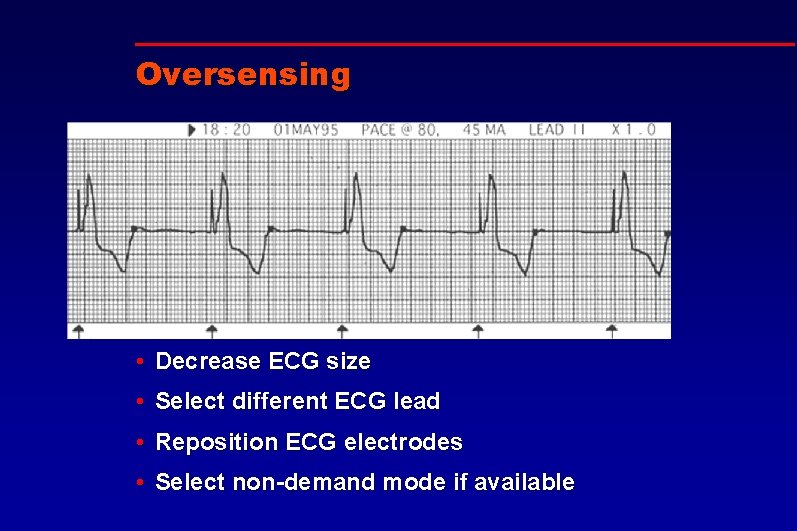
Oversensing • Decrease ECG size • Select different ECG lead • Reposition ECG electrodes • Select non-demand mode if available

Pacing Success

Summary - Noninvasive Pacing • Valued and respected technique in emergency cardiac care • Basic principles of invasive pacing apply to noninvasive pacing • Allows rapid initiation of emergency pacing

“Buying Time”
- Slides: 57