Noncommunicable Diseases Epidemiology and Pubic Health Dr Nick

Noncommunicable Diseases: Epidemiology and Pubic Health Dr Nick Banatvala Sixth International WHO IUMSP NCD Managers Seminar May 2012
Global Status

Structure of the presentation • Mortality • Morbidity • Risk factors – Behavioral – Metabolic/physical – Chronic infections • Public health impact and reducing the burden of NCDs • What do we need to do to tackle the problem?
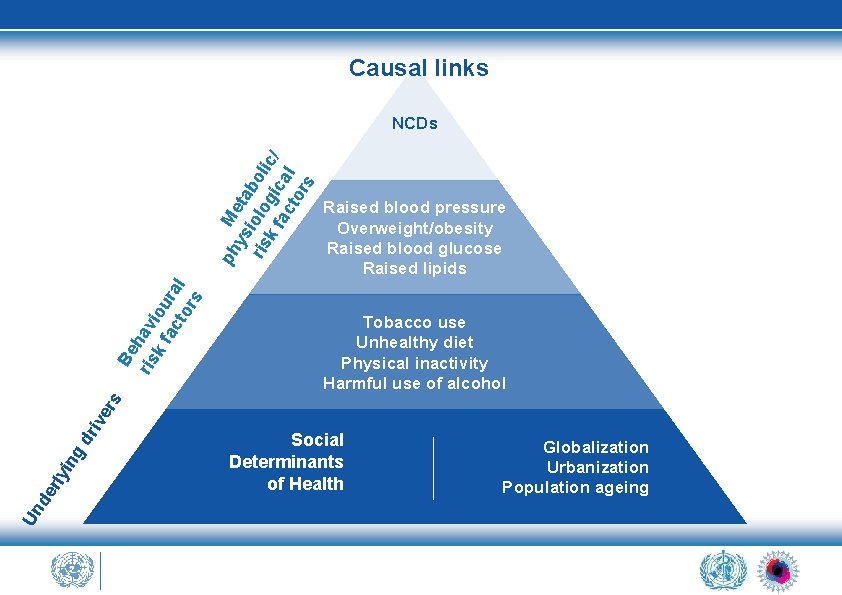
Causal links Raised blood pressure Overweight/obesity Raised blood glucose Raised lipids Tobacco use Unhealthy diet Physical inactivity Harmful use of alcohol Un de rly i ng dr ive rs Be ris hav k f iou ac ra to l rs ph M ys eta ris iolo boli k f gic c/ ac al to rs NCDs Social Determinants of Health Globalization Urbanization Population ageing

1. Mortality

• 57 million deaths in 2008 • 36 million (63%) were NCDs – principally CVD, diabetes, cancer and chronic respiratory diseases • 80% of these deaths in LMICs • 44% NCD deaths before the age of 70 (48% LMIC, 26% HIC) • Women are affected

Low-income countries Middle-income countries 1. 2. 3. 4. 5. 1. Stroke and cerebrovascular disease 2. Coronary heart disease 3. Chronic pulmonary disease 4. Lower respiratory infection 5. Trachea, bronchus, lung cancers 6. Road traffic accidents 7. Hypertensive heart disease 8. Stomach cancer 9. Tuberculosis 10. Diabetes mellitus 6. 7. 8. 9. 10. Lower respiratory infections Coronary heart disease Diarrhoeal diseases HIV/AIDS Stroke and cerebrovascular disease Chronic pulmonary disease Tuberculosis Neonatal infections Malaria Premature and low birth weight Source: The top-10 leading causes of death
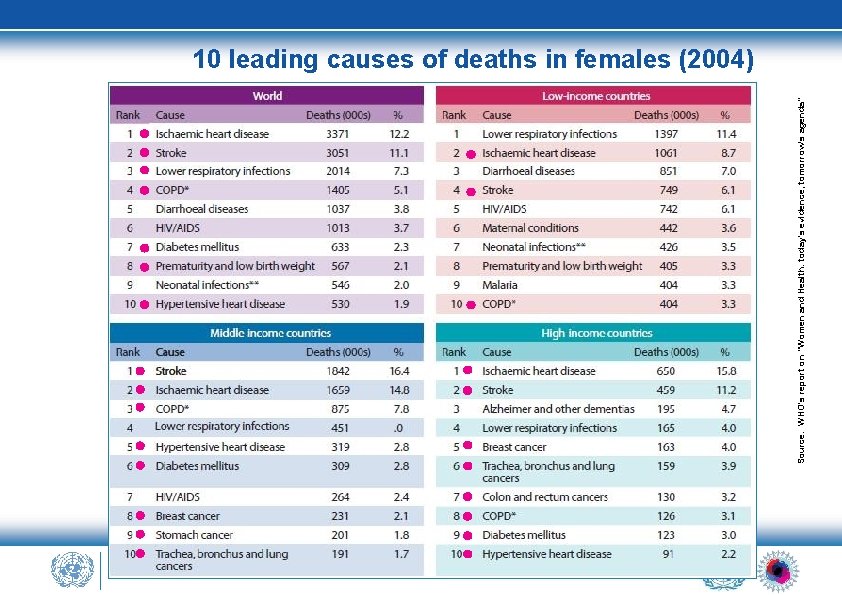
Source: WHO's report on "Women and Health: today's evidence, tomorrow's agenda" 10 leading causes of deaths in females (2004)
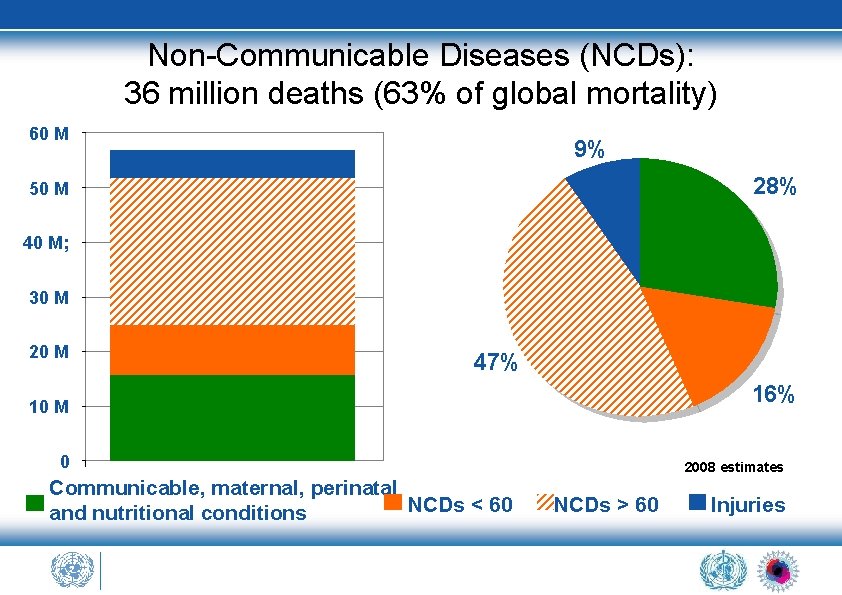
Non-Communicable Diseases (NCDs): 36 million deaths (63% of global mortality) 60 M 9% 28% 50 M 40 M; 30 M 20 M 47% 16% 10 M 0 Communicable, maternal, perinatal NCDs < 60 and nutritional conditions 2008 estimates NCDs > 60 Injuries
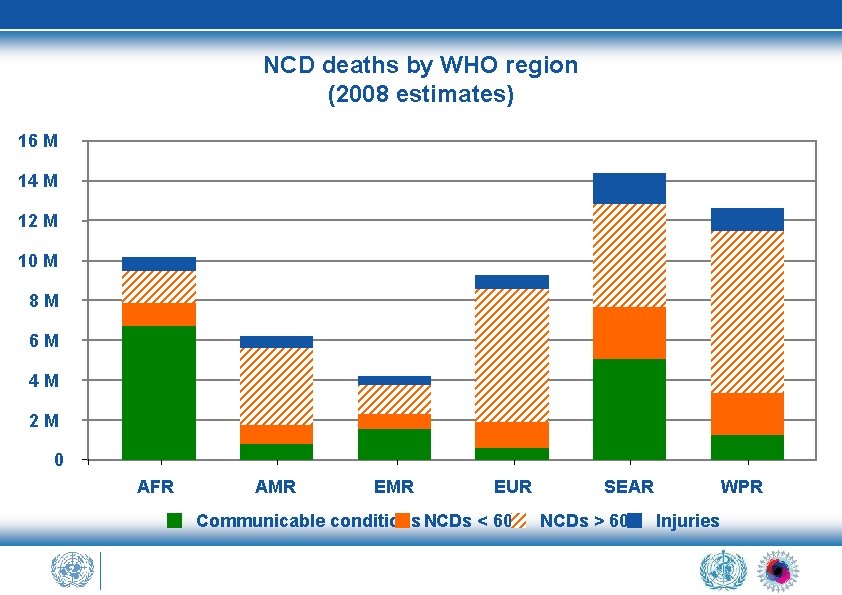
NCD deaths by WHO region (2008 estimates) 16 M 14 M 12 M 10 M 8 M 6 M 4 M 2 M 0 AFR AMR EUR Communicable conditions NCDs < 60 SEAR NCDs > 60 WPR Injuries
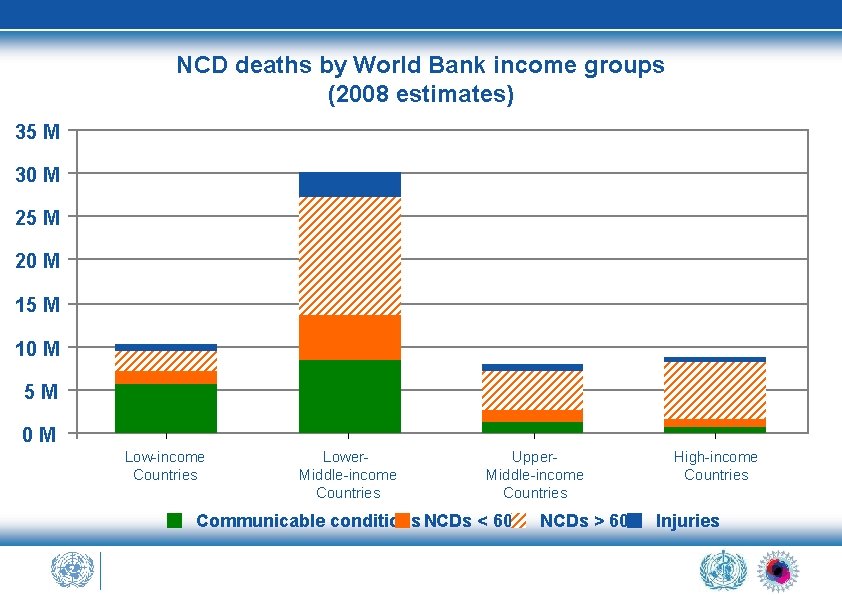
NCD deaths by World Bank income groups (2008 estimates) 35 M 30 M 25 M 20 M 15 M 10 M 5 M 0 M Low-income Countries Lower. Middle-income Countries Upper. Middle-income Countries Communicable conditions NCDs < 60 NCDs > 60 High-income Countries Injuries
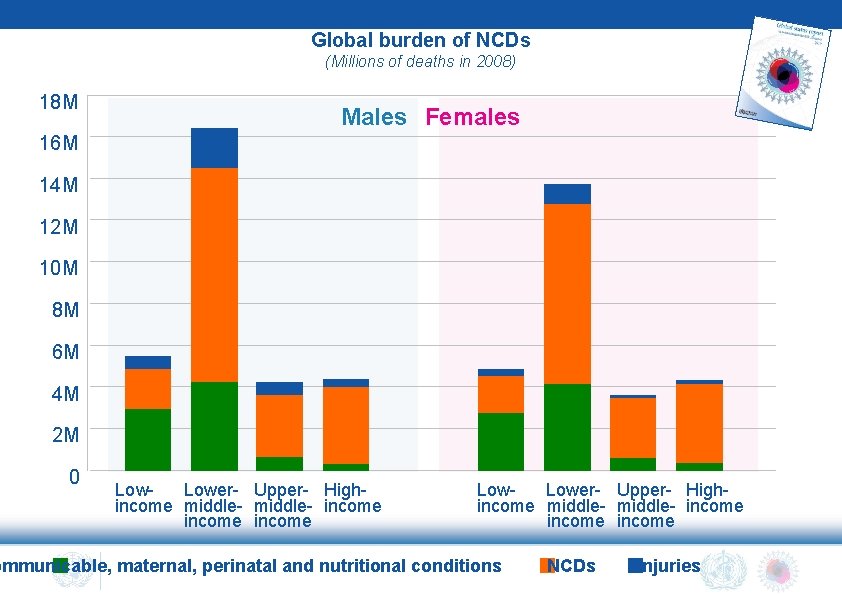
Global burden of NCDs (Millions of deaths in 2008) 18 M Males Females 16 M 14 M 12 M 10 M 8 M 6 M 4 M 2 M 0 Lower- Upper- Highincome middle- income income ommunicable, maternal, perinatal and nutritional conditions NCDs Injuries
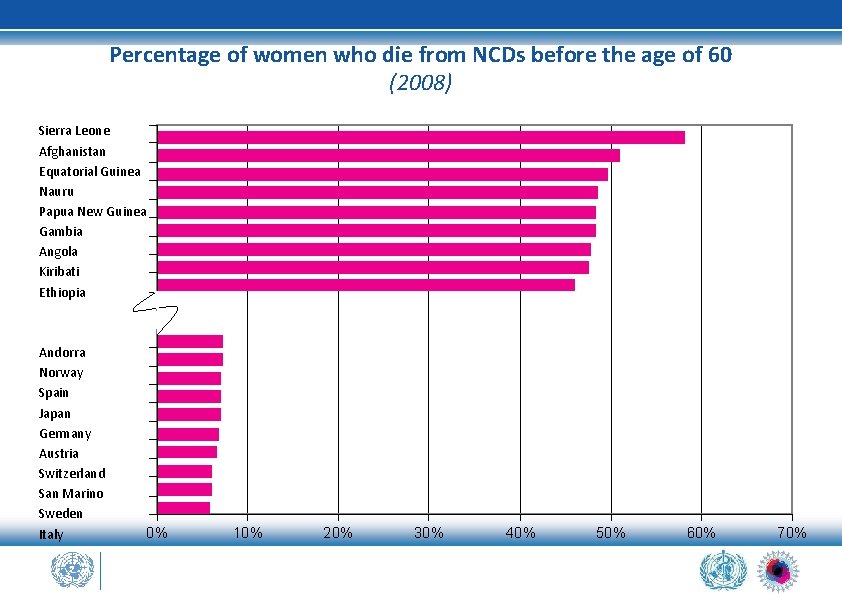
Percentage of women who die from NCDs before the age of 60 (2008) Sierra Leone Afghanistan Equatorial Guinea Nauru Papua New Guinea Gambia Angola Kiribati Ethiopia Andorra Norway Spain Japan Germany Austria Switzerland San Marino Sweden Italy 0% 10% 20% 30% 40% 50% 60% 70%
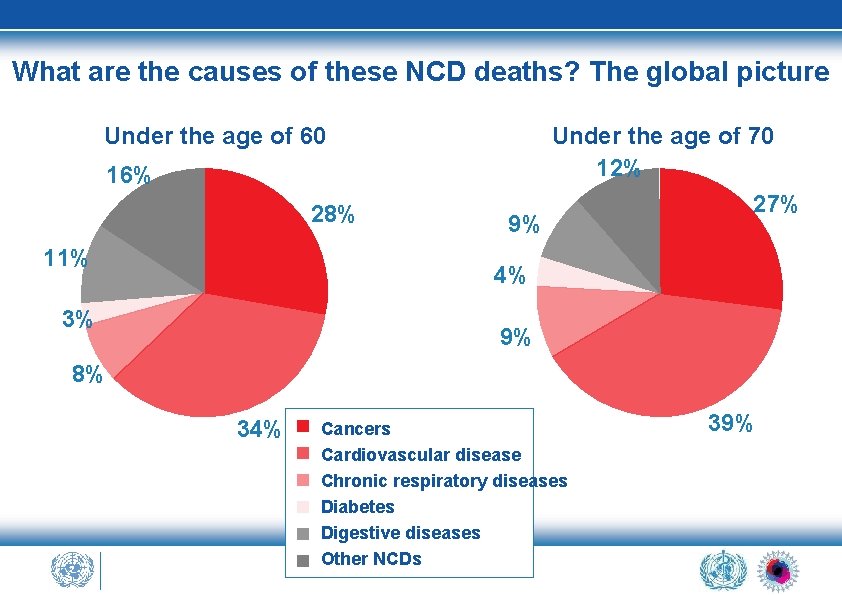
What are the causes of these NCD deaths? The global picture Under the age of 60 16% 28% 11% 9% Under the age of 70 12% 27% 4% 3% 9% 8% 34% Cancers Cardiovascular disease Chronic respiratory diseases Diabetes Digestive diseases Other NCDs 39%

2. Morbidity
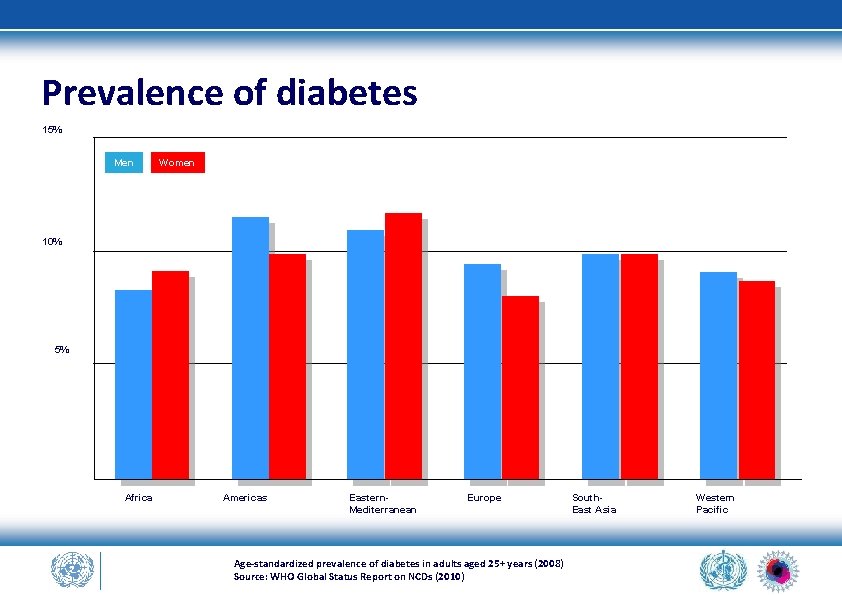
Prevalence of diabetes 15% Men Women 10% 5% Africa Americas Eastern. Mediterranean Europe Age-standardized prevalence of diabetes in adults aged 25+ years (2008) Source: WHO Global Status Report on NCDs (2010) South. East Asia Western Pacific
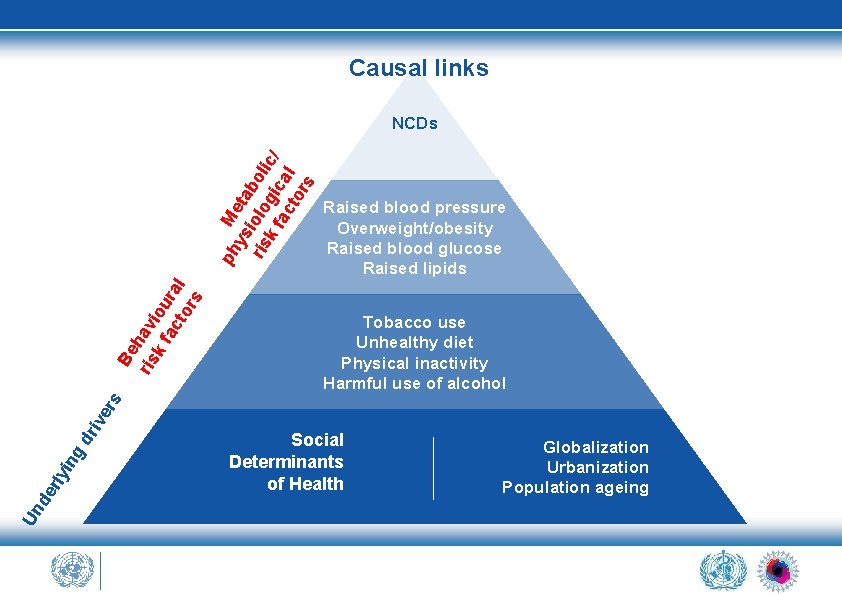
Causal links Raised blood pressure Overweight/obesity Raised blood glucose Raised lipids Tobacco use Unhealthy diet Physical inactivity Harmful use of alcohol Un de rly i ng dr ive rs Be ris hav k f iou ac ra to l rs ph M ys eta ris iolo boli k f gic c/ ac al to rs NCDs Social Determinants of Health Globalization Urbanization Population ageing

3. Metabolic/physical risk factors

Metabolic/physical risk factors a) Raised blood pressure – – – – ≥ 140 mm. Hg and/or ≥ 90 mm. Hg 40% adults over 25 have raised BP Causes 7. 5 million (13%) all deaths 3. 7% total DALYs Major risk factor for CHD, ischaemic and hemorrhagic stroke CVD risk doubles for each increase of 20/10 mm. Hg Other complications: heart failure, PVD, renal disease, retinal hemorrhage
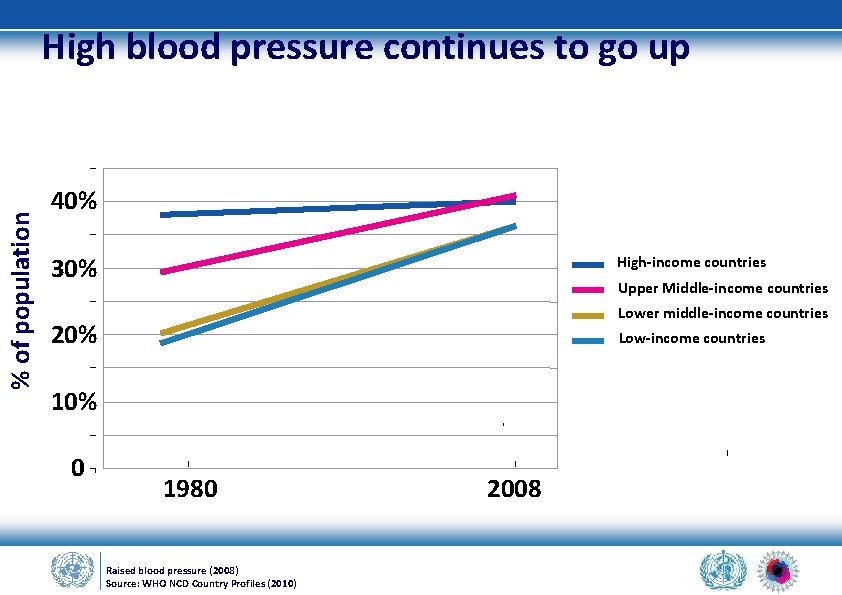
% of population High blood pressure continues to go up 40% 30% High-income countries Upper Middle-income countries Lower middle-income countries 20% Low-income countries 10% 0 1980 Raised blood pressure (2008) Source: WHO NCD Country Profiles (2010) 2008
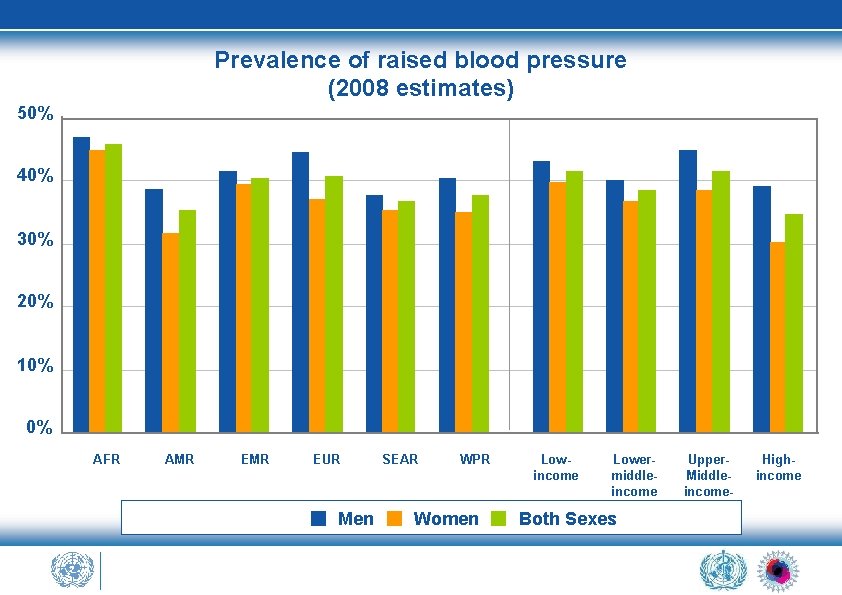
Prevalence of raised blood pressure (2008 estimates) 50% 40% 30% 20% 10% 0% AFR AMR EUR Men SEAR WPR Women Lowincome Lowermiddleincome Both Sexes Upper. Middleincome- Highincome

Metabolic/physical risk factors b) Overweight and obesity – BMI ≥ 25 kg/m 2, BMI >= 30 kg/m 2 – Population goal: 21 -23 kg/m 2 – Individual goal: 18. 5 to 24. 9 kg/m 2 – 35% adults aged 20+ overweight – Worldwide prevalence doubled over the last 30 y
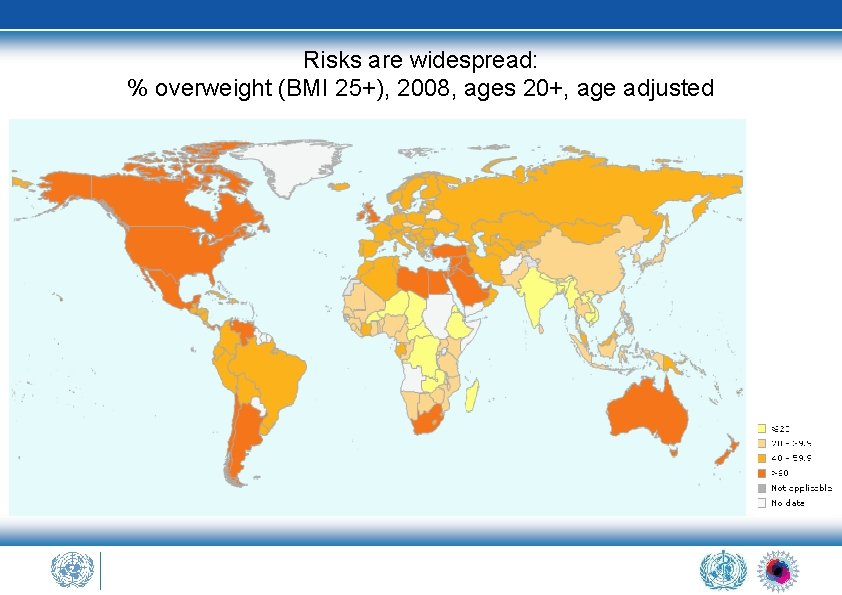
Risks are widespread: % overweight (BMI 25+), 2008, ages 20+, age adjusted
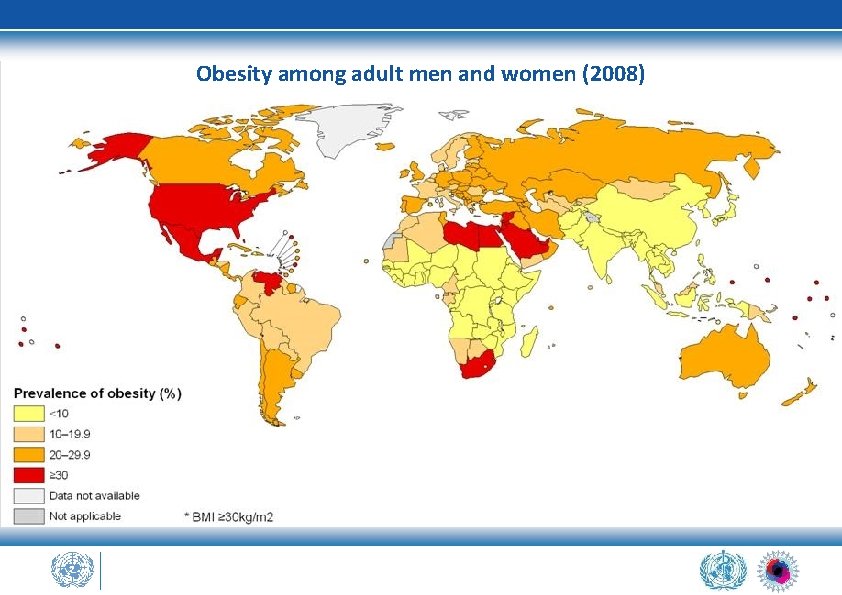
Obesity among adult men and women (2008)
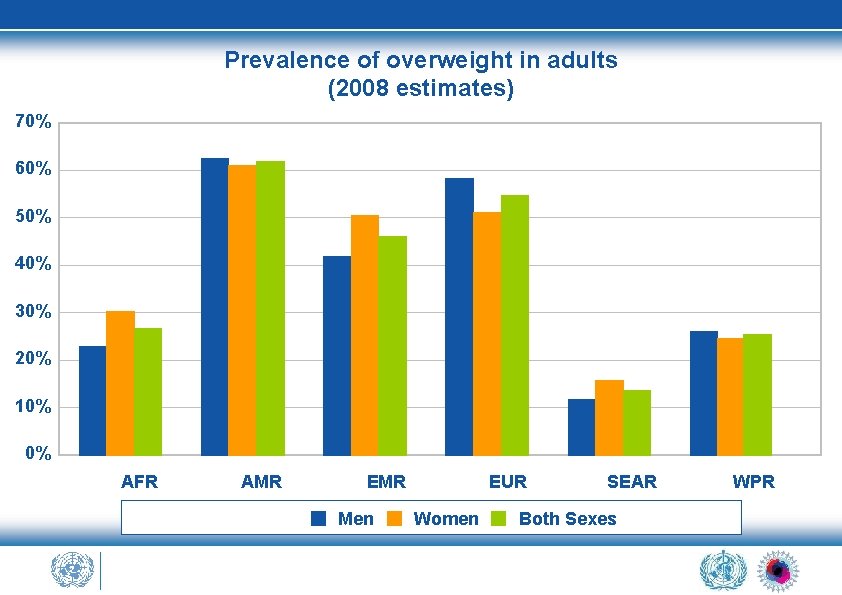
Prevalence of overweight in adults (2008 estimates) 70% 60% 50% 40% 30% 20% 10% 0% AFR AMR EMR Men EUR Women SEAR Both Sexes WPR
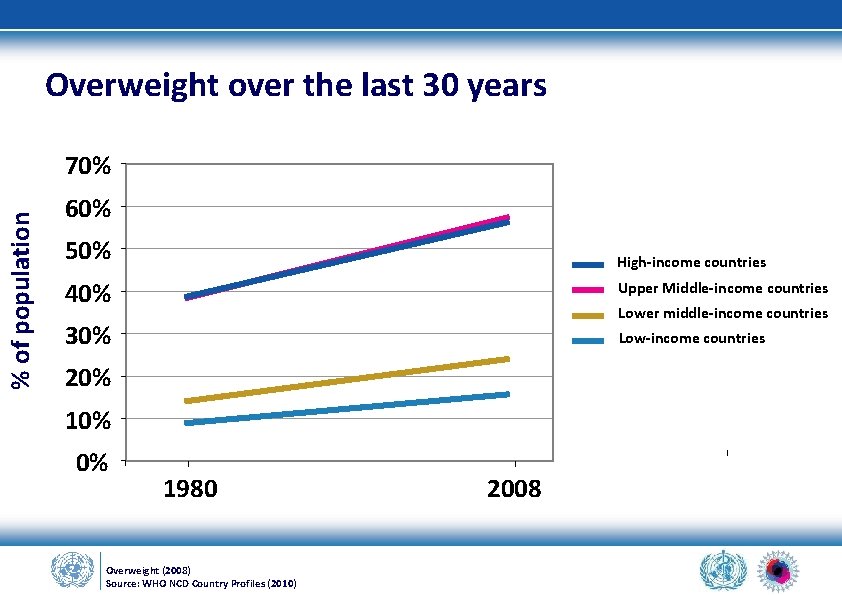
Overweight over the last 30 years % of population 70% 60% 50% High-income countries 40% Upper Middle-income countries 30% Low-income countries Lower middle-income countries 20% 10% 0% 1980 Overweight (2008) Source: WHO NCD Country Profiles (2010) 2008

Metabolic/physical risk factors c) Raised cholesterol – – – 5. 0 mmol/l or 190 mg/dl or higher Increases the risk of heart disease and stroke Third of IHD attributible to high cholesterol Cause of 2. 6 million deaths (4. 5% of the total) 10% reduction in men aged 40 would result in 50% reduction in heart disease over 5 years (and at age 70, 20% over 5 y – Global prevalence of raised total cholesterol 39%
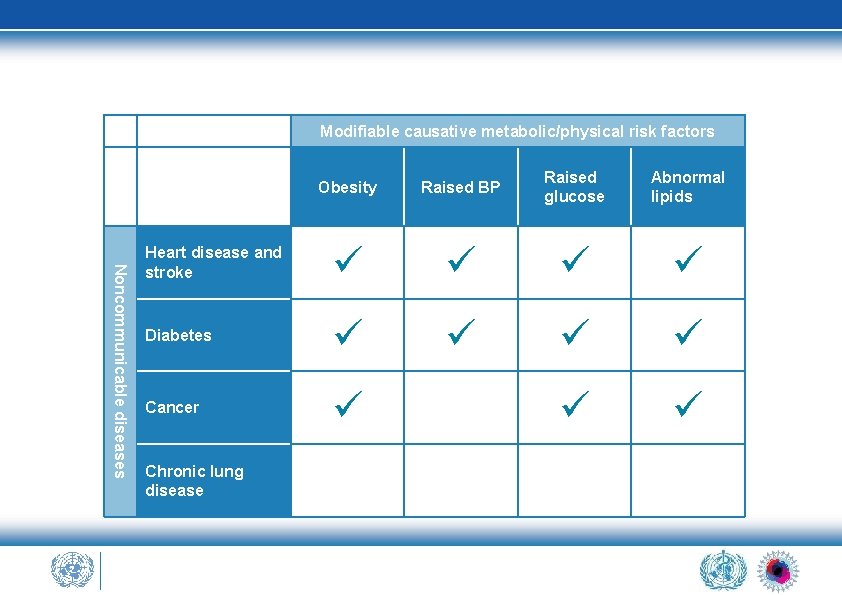
Modifiable causative metabolic/physical risk factors Noncommunicable diseases Obesity Raised BP Raised glucose Abnormal lipids Heart disease and stroke Diabetes Cancer Chronic lung disease

4. Behavioral risk factors

Behavioral risk factors a) Tobacco – 1 billion smokers – 4000 chemicals, 50 carcinogenic – Smoked and unsmoked forms – 6 million die from tobacco use and exposure • 6% all female deaths, 12% male • 10% deaths attributable to second-hand smoke • Causes 71% lung cancer deaths, 42% chronic respiratory deaths, 10% CVD deaths – 7. 5 million deaths by 2020
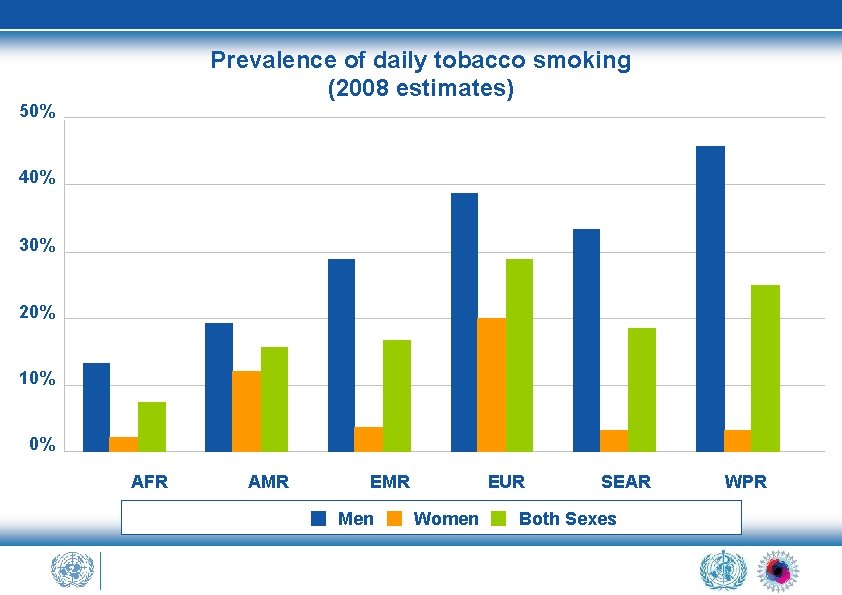
Prevalence of daily tobacco smoking (2008 estimates) 50% 40% 30% 20% 10% 0% AFR AMR EMR Men EUR Women SEAR Both Sexes WPR

Behavioral risk factors b) Insufficient physical activity • Less than x 5 30 min moderate activity per week (or x 3 20 min vigorous activity) • Globally, 31% those 15 y+ insufficiently active • 3. 2 million deaths • 20 -30% increased risk all-cause mortality • Adequate activity reduces risk of IHD by 30%, diabetes 27%, breast and colon cancer by 21 -25%
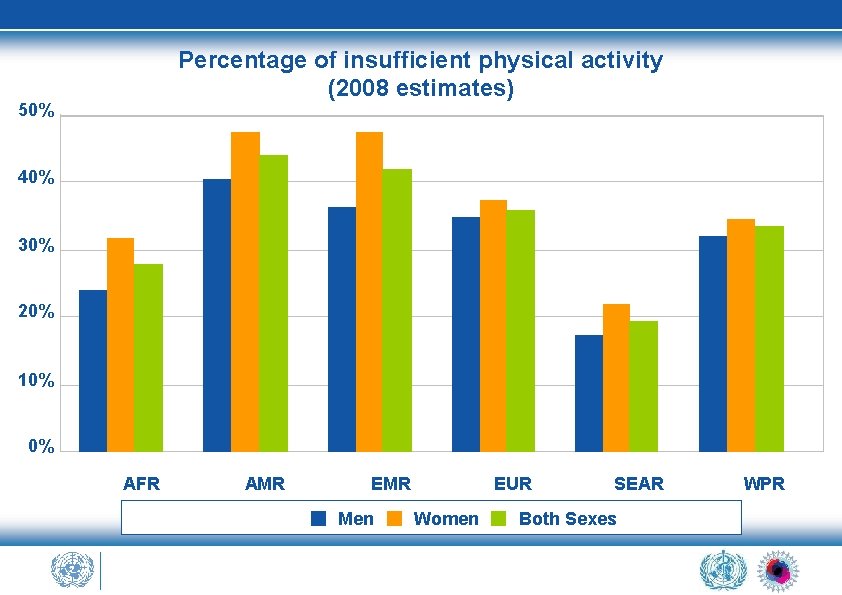
Percentage of insufficient physical activity (2008 estimates) 50% 40% 30% 20% 10% 0% AFR AMR EMR Men EUR Women SEAR Both Sexes WPR

Behavioral risk factors c) Harmful use of alcohol – Responsible 2. 3 million deaths and disabilities – 3. 8% of all deaths – 50% from NCDs – Low-risk patterns of consumption may have a beneficial effect – 45% global population never consumed alcohol

Behavioral risk factors d) Unhealthy diet – Overall estimates of unhealthy diet not possible – But 1. 7 million deaths (2. 8% of the total) attributable to low fruit and low vegetable consumption • Adequate fruit and vegetable intake reduces risk of CVD, stomach and colorectal cancer – Salt consumption important determinant of blood pressure and CVD risk • Recommendation is less than 5 g person – Saturated and trans-fat increase risk of CHD and type 2 diabetes. • Poly-unsaturated fat from vegetables is protective
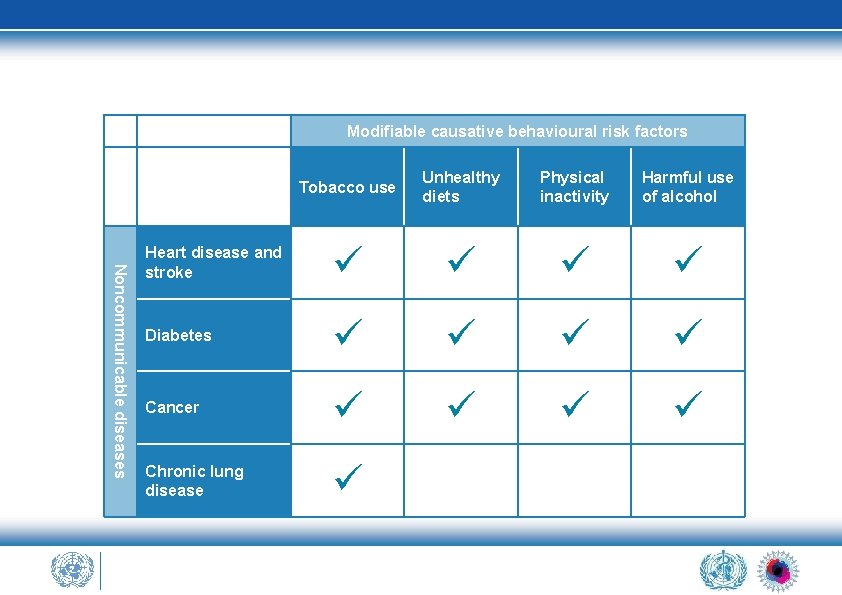
Modifiable causative behavioural risk factors Noncommunicable diseases Tobacco use Unhealthy diets Physical inactivity Harmful use of alcohol Heart disease and stroke Diabetes Cancer Chronic lung disease

Chronic infection as a risk factor • Cervical, liver and stomach cancers all have greatest incidence in LMICs • All caused predominately by chronic infections • 2 million cancer cases (18% global cancer burden) attributable to a few specific chronic infections – HPV: 100% cancer cervix, majority of anogenital tract, 20 -60% oro-pharyngeal – HBV and HBC: 50 -80% primary liver cancer – H. pylori: 80% noncardia carcinomas stomach
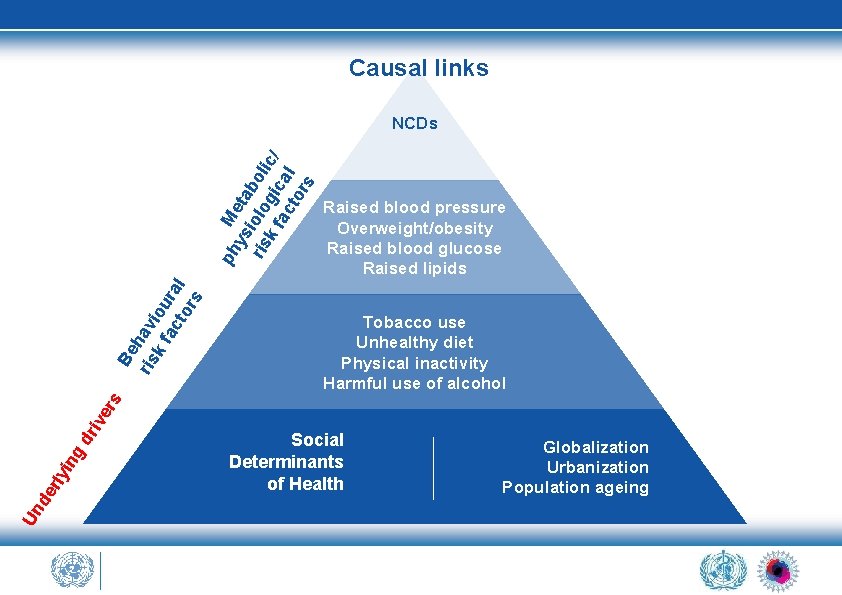
Causal links Raised blood pressure Overweight/obesity Raised blood glucose Raised lipids Tobacco use Unhealthy diet Physical inactivity Harmful use of alcohol Un de rly i ng dr ive rs Be ris hav k f iou ac ra to l rs ph M ys eta ris iolo boli k f gic c/ ac al to rs NCDs Social Determinants of Health Globalization Urbanization Population ageing

5. Public health impact of NCDs

Public health impact of NCDs • Premature mortality, significant morbidity • Quality of life of affected individuals and families • Socioeconomic impact on individuals, families, communities and societies
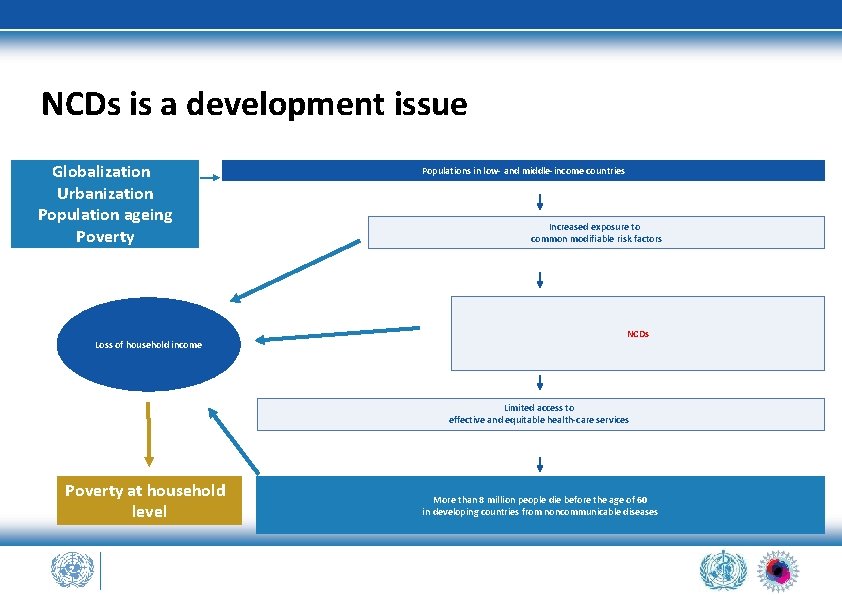
NCDs is a development issue Globalization Urbanization Population ageing Poverty Loss of household income Populations in low- and middle-income countries Increased exposure to common modifiable risk factors NCDs Limited access to effective and equitable health-care services Poverty at household level More than 8 million people die before the age of 60 in developing countries from noncommunicable diseases
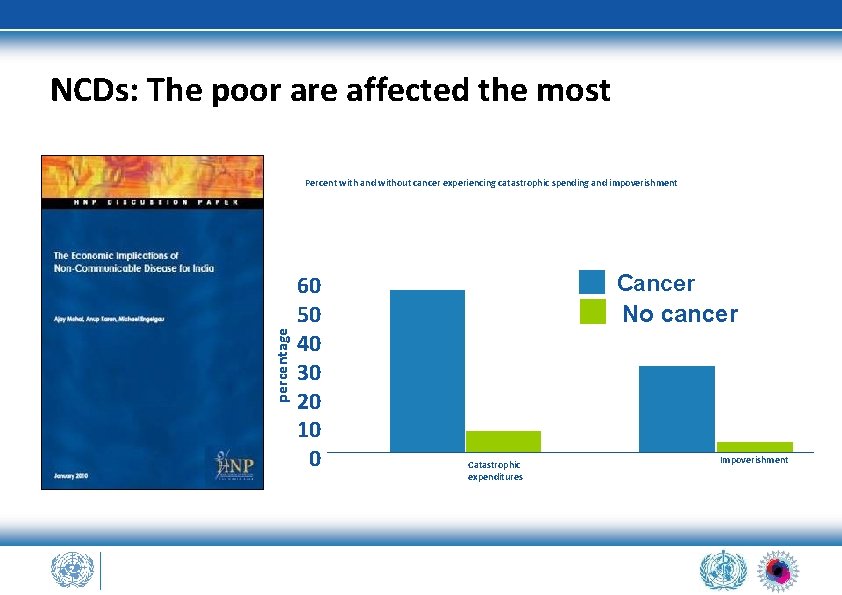
NCDs: The poor are affected the most p e r c e n t a ge Percent with and without cancer experiencing catastrophic spending and impoverishment 60 50 40 30 20 10 0 Cancer No cancer Catastrophic expenditures Impoverishment
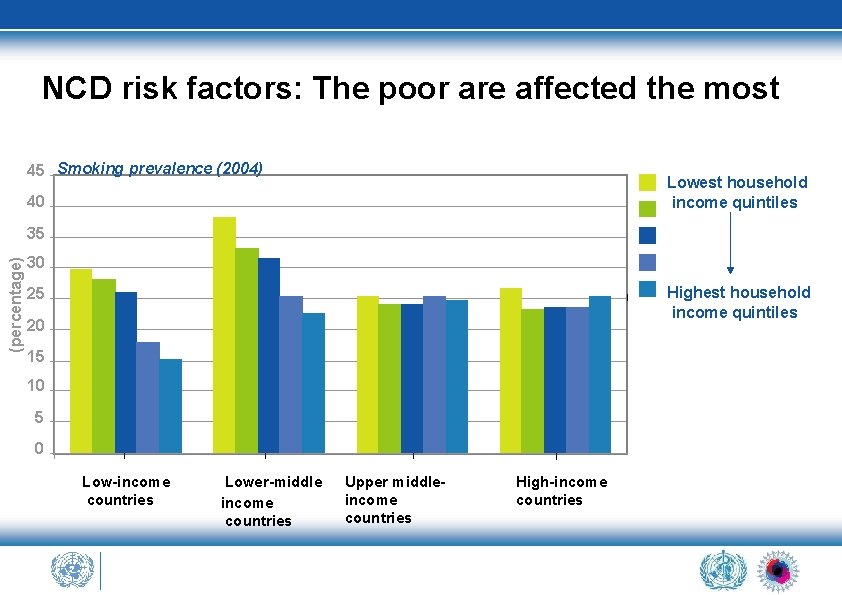
NCD risk factors: The poor are affected the most 45 Smoking prevalence (2004) Lowest household income quintiles 40 (percentage) 35 30 Highest household income quintiles 25 20 15 10 5 0 Low-income countries Lower-middle income countries Upper middleincome countries High-income countries
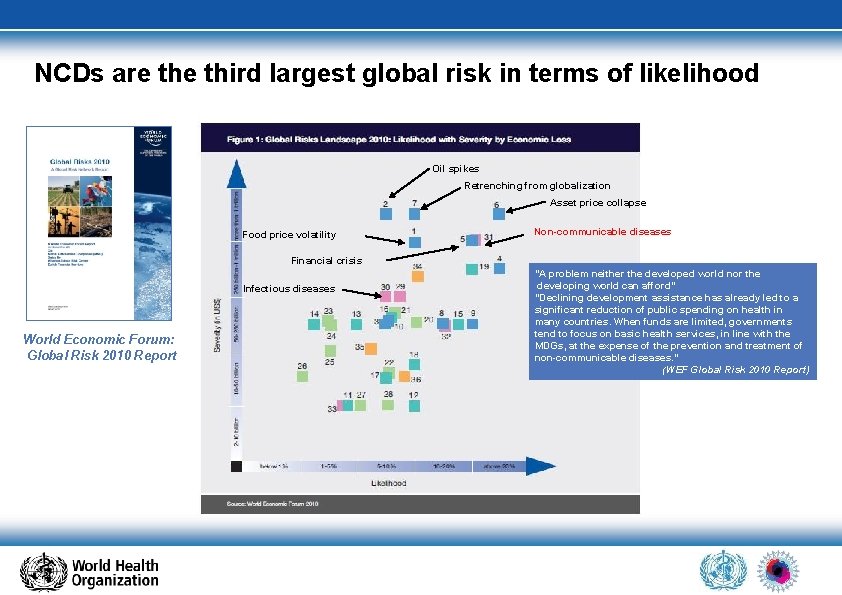
NCDs are third largest global risk in terms of likelihood Oil spikes Retrenching from globalization Asset price collapse Food price volatility Non-communicable diseases Financial crisis Infectious diseases World Economic Forum: Global Risk 2010 Report "A problem neither the developed world nor the developing world can afford" "Declining development assistance has already led to a significant reduction of public spending on health in many countries. When funds are limited, governments tend to focus on basic health services, in line with the MDGs, at the expense of the prevention and treatment of non-communicable diseases. " (WEF Global Risk 2010 Report)

US$ 7 T US$ 11 B is the cumulative lost output in developing countries associated with NCDs between 2011 -2025 is the average yearly cost for all developing countries to scale up action by implementing a combined set of "best buy" priority NCD interventions identified by WHO
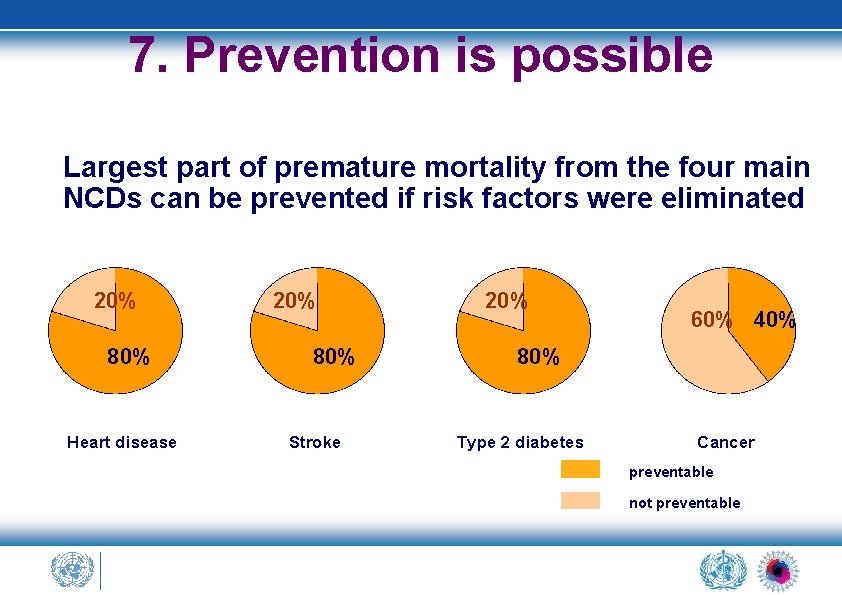
7. Prevention is possible Largest part of premature mortality from the four main NCDs can be prevented if risk factors were eliminated 20% 80% Heart disease 20% 80% Stroke 20% 60% 40% 80% Type 2 diabetes Cancer preventable not preventable

8. What is needed to tackle this public health problem?
- Slides: 47