Non Thermal Non Tumescent Ablation How and When

Non Thermal, Non Tumescent Ablation: How and When To Cool It Down Steve Elias MD Director, Center for Vein Disease Englewood Hospital and Medical Center NJ

Disclosures • Medtronic Inc. – Scientific Advisory Board • Vascular Insights LLC – Scientific Advisory Board • Le. Maitre Vascular – Consultant • Hancock-Jaffe Labs - Consultant

“SO WE BEAT ON, BOATS AGAINST THE CURRENT, BORNE BACK CEASELESSLY INTO THE PAST” F. SCOTT FITZGERALD “THE GREAT GATSBY”

How and When • How has been discussed many times • How can be learned at our hands-on workshops • When is more important now • When to consider NTNT or TT?

EVA: Categories* • TT (Thermal, Tumescent) • NTNT (Non Thermal, Non Tumescent) • TNT (Thermal Non Tumescent) - new • NTT (Non Thermal Tumescent) - new *Elias S. Emerging Endovenous Technologies. Endovasc Today. March 2014.

Thermal Tumescent: TT • Laser – HSLW, WSLW, radial/jacketed • Radiofrequency – Closurefast, RFITT • Steam – SVS, Veneti

Non Thermal, Non Tumescent: NTNT • Mechanical Occlusion Chemical Assisted – Vascular Insights LLC • Cyanoacrylate glue – Medtronic Inc • Polidocanol Injectable Microfoam – BTG • V Block – VVT Medical
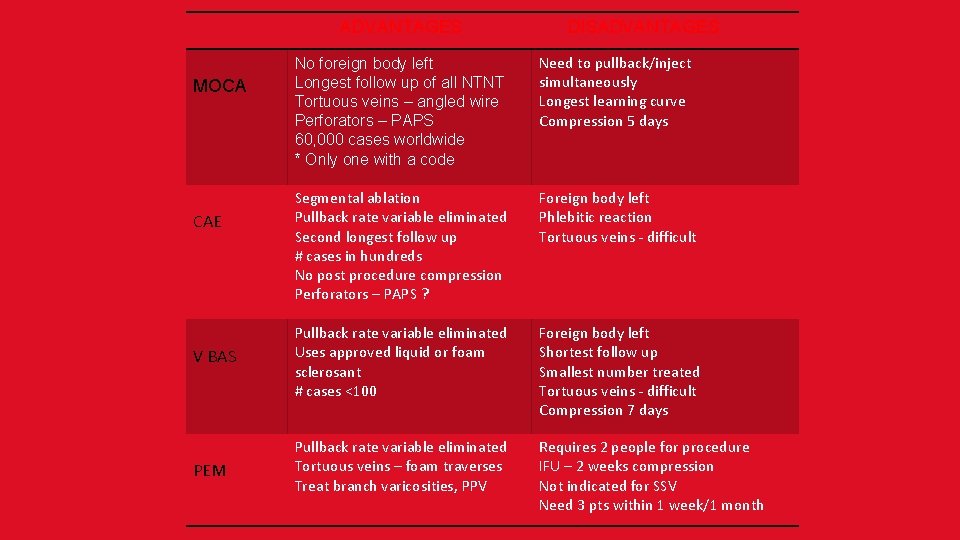
ADVANTAGES DISADVANTAGES No foreign body left Longest follow up of all NTNT Tortuous veins – angled wire Perforators – PAPS 60, 000 cases worldwide * Only one with a code Need to pullback/inject simultaneously Longest learning curve Compression 5 days Segmental ablation Pullback rate variable eliminated Second longest follow up # cases in hundreds No post procedure compression Perforators – PAPS ? Foreign body left Phlebitic reaction Tortuous veins - difficult V BAS Pullback rate variable eliminated Uses approved liquid or foam sclerosant # cases <100 Foreign body left Shortest follow up Smallest number treated Tortuous veins - difficult Compression 7 days PEM Pullback rate variable eliminated Tortuous veins – foam traverses Treat branch varicosities, PPV Requires 2 people for procedure IFU – 2 weeks compression Not indicated for SSV Need 3 pts within 1 week/1 month MOCA CAE

NTNT – Recent Literature • • They all work with similar safety/efficacy They all improve Qo. L NTNT non inferior to TT NTNT probably less discomfort during/after MOCA – Dedicated code and valuation PEM – some carriers have on policy (not Medicare) CAE – self pay currently Successful EVA helps patients

Should We Do This? • SVS/AVF Guidelines – 1 B recommendation for EVA, compression if not a candidate for EVA • NICE Guidelines (UK): EVA Foam Surgery Stockings • Good data based on: efficacy, safety and Qo. L • A closed/ablated superficial axial vein is good no matter how it is accomplished

What’s In A Name? It is not really about the name of the vein Technique and technology choices depends on: • • Size – small, medium, large Length – short, long Location – AK, BK, Suprafascial The Neighbors – nerves, skin, LDS or ulcer Disease state – C 5, C 6, SVT Patient type – fat, thin, anxious Special – MD, MD spouse, friend, foe, barrister

Rules To Live By: When Deciding What To Use When • Treat to lowest point of incompetence • Use whatever is “safest” to achieve above • Consider cost – to patient and health care system • Tailor technique/technology to the clinical setting • Need to have TT and NTNT in armamentarium

Size, Length, Tortuosity • Size – Large >12 mm, Medium 5 -10 mm, Small <5 mm – Large – TT before NTNT – Medium – NTNT before TT or dealers choice – Small – NTNT or Should you be doing this? • Length – Long – anything, Short – cost CAE, PEM - expensive MOCA/RF/Laser - good • Tortuosity – PEM, MOCA then others (guidewires)

Location: AK or BK (Nerves) • AK – GSV, AAGSV, Intersaphenous (Giacomini) • BK – GSV, SSV, PPV, VV • AK – anything as long as it is in fascia and straight • BK – GSV/SSV – NTNT>TT, VV – PEM, Phlebec • PPV – Laser>MOCA> Foam (artery) CAE?
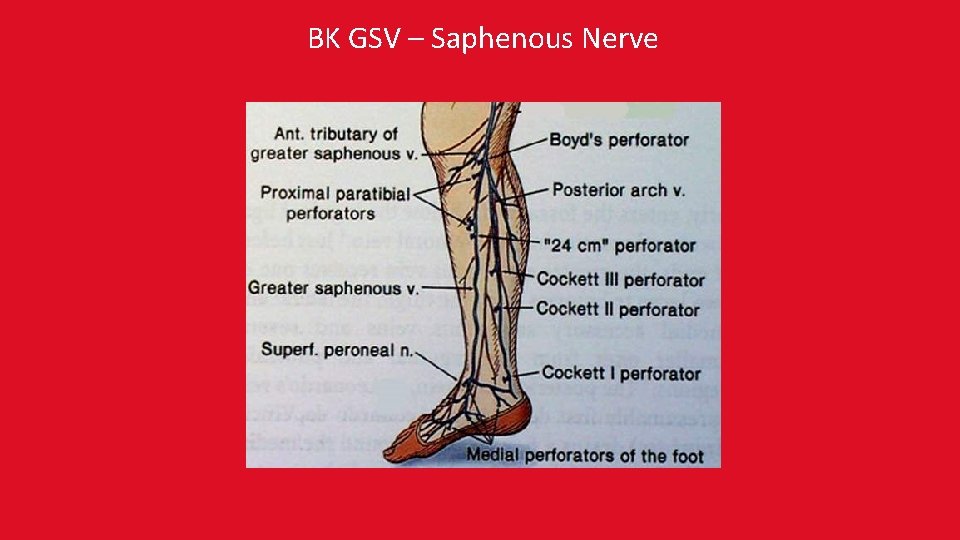
BK GSV – Saphenous Nerve
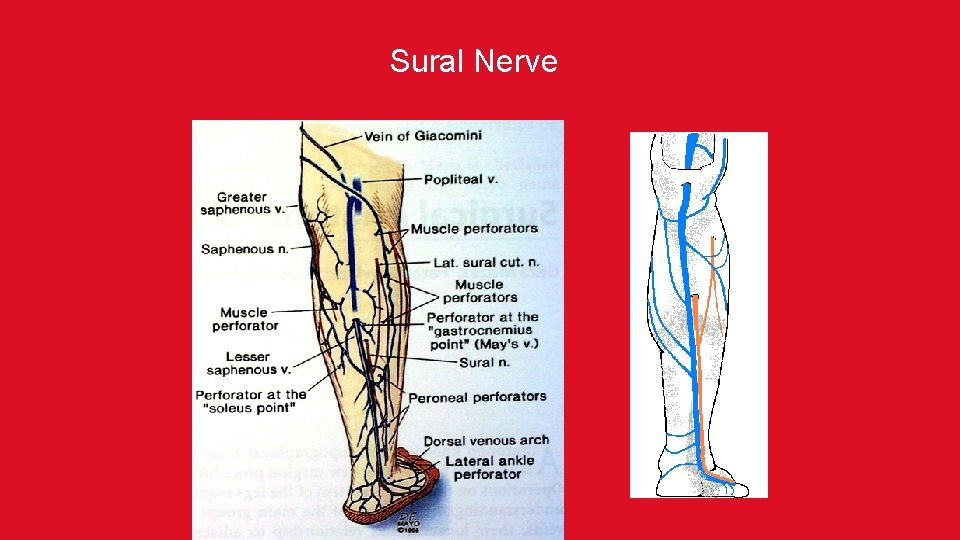
Sural Nerve
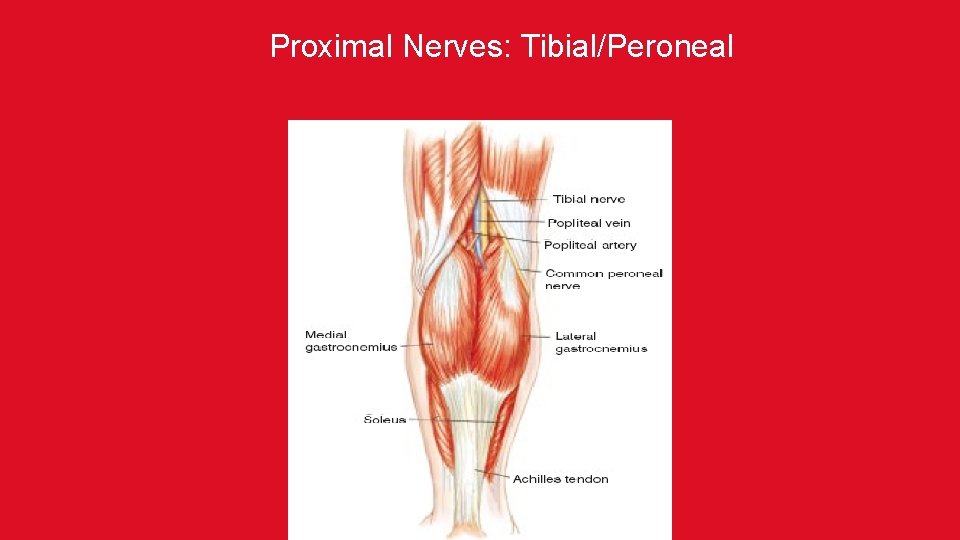
Proximal Nerves: Tibial/Peroneal

LOCATION: Fascial/Suprafascial • AK Fascial – anything • BK GSV and SSV – NTNT (MOCA>PEM>CAE) before TT • Suprafascial – MOCA> Inversion stripping> PEM> TT (skin/cord, hyperpig)>CAE(phlebitis)

ADVANCED DISEASE STATE: C 4 -6 • C 5, C 6 – AK GSV to mid calf – TT/NTNT • C 5, C 6 – GSV/SSV to ankle – NTNT (LDS or ulcer difficult tumescence) • C 5, C 6 – BK GSV residual – retrograde NTNT and foam ulcer bed (MOCA/PEM) • Previous SVT – TT – need more energy
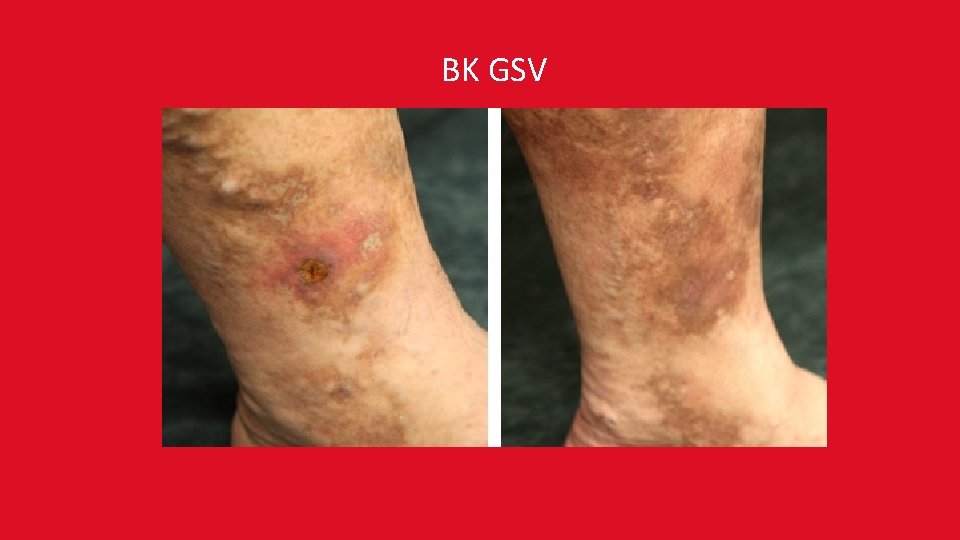
BK GSV
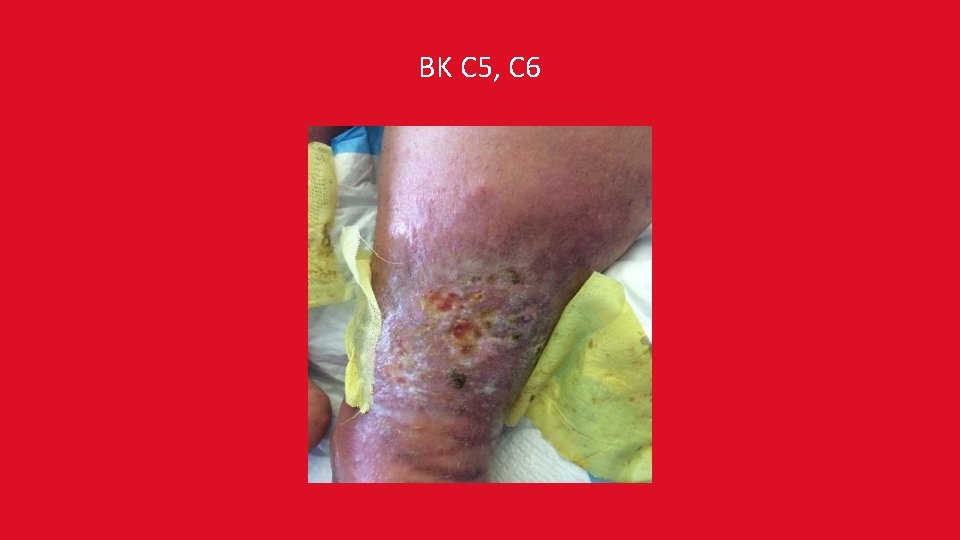
BK C 5, C 6

PATIENT TYPE • Fat – TT over NTNT • Thin – NTNT over TT • Anxious, Nervous – NTNT over TT

SPECIAL SCENARIOS • MD or Spouse – RF, MOCA • Friend – RF, WSLW (1470), MOCA • Foe – HSLW (810/980) or stripping • Attorney/Barrister – 810/980 with 150 joules/cm and no tumescence

ANTICOAGULATION • INR 2. 0 – 2. 5 – anything • INR > 2. 5 – TT • Rarely stop it

RETREATMENT AFTER FAILED EVA If used NTNT > use TT If used TT > use alternate TT If TT fails > inversion stripping with tumescence

CONCLUSIONS • Need one TT and one NTNT • More advanced disease, the lower to go -NTNT • Tailor the technique to the situation • All veins are not the same – either by name but more importantly by size, location, disease state

TREATMENT OF REFLUX IN THE SUPERFICIAL VEINS TREATMENT OF PATIENTS WITH REFLUX IN THEIR VEINS

“THE FUTURE OF NON THERMAL ABLATION: IS THE FUTURE OF ENDOVENOUS ABLATION”

Don’t Worry, Be Happy Vein Disease Is An Incurable Disease
- Slides: 29