Non leukemic myeloproliferative disorders polycythemia veraPV Non leukemic


















- Slides: 21

Non leukemic myeloproliferative disorders polycythemia vera(PV) Non leukemic Ess ential thrombocythemia (ET) My elofibrosis(MF)

myeloproliferative disorders(MPD) a group of conditions characterized by clonal proliferation of one or more haemopoietic components in the BM & in many cases in the liver & spleen. These disorders are closely related to each other , transitional forms occur & in many cases an evolution from one entity into other occurs during the course of disease.

polycythemia vera(PV), polycythemia rubra vera(PRV) blood changes includes an increased haemoglobin above 17. 5 g/dl in adult males & 15. 5 g/dl in females usually with increased red cell count above 6× 109 /l in male & 5. 5× 109 /l in females & haematocrit above 55% in males & 47% in females. The increased in red cell volume is caused by endogenous myeloproliferation due to stem cell defect, so in many patients overproduction of granulocytes & platelets occur as well as of red cells.

Causes of polycythemia:

Clinical features: This disease is of old subjects with equal sex incidence & the clinical features are the result of hyperviscosity, hypervolaemia or hypermetabolism. 1 -Headach, pruritis (especially after hot path) , dyspnoea, blurred vision & night sweat. 2 - Plethoric appearance – ruddy cyanosis. 3 - Splenomegaly in 2/3 of patients. 4 -Haemorrhage or thrombosis ( either arterial or venous ). 5 - Hypertension in 1/3 of patients. 6 - Gout due to raised uric acid production 7 - Peptic ulceration in 5 -10%.

Lab. Findings: 1 -The haemoglobin, haematocrit, red cell count & total red cell volume are increased. 2 -Neutrophil leucocytosis is seen in 1/2 0 f cases. 3 -Raised platelets count in 1/2 of cases. 4 - The neutrophil alkaline phosphatase score is high. 5 - Increased serum B 12 & B 12 binding capacity because of increased transcobalamin 1 6 - BM: is hypercellular with prominent megakaryocytes. 7 -Blood viscosity is increased. 8 - Plasma urate is often increased. 9 - Circulating erythroid progenitors are increased & grow in vitro independently of erythropoietin.

Essential thrombocythaemia (ET), primary thrombocythaemia Megakaryocyte proliferation & overproduction of platelets count above normal , this condition is closely related to PRV. Some cases show patchy fibrosis.

Criteria for diagnosis of ET: Platelets >600× 109 /L No evidence or indication of raised red cell mass No Philadelphia chromosome or bcr-abl rearrangement No support for a diagnosis of MF No demonstrated cause for reactive thrombocytosis

Clinical features: 1 -Recurrent hemorrhage & thrombosis 2 - splenic enlargement in early phase but splenic atrophy due to platelets blocking the splenic microcirculation 3 - There may be anemia (due to iron deficiency anemia from chronic bleeding) or polycythaemia Lab. Findings: 1 -Abnormal large platelets & megakaryocyte fragments may be seen in peripheral blood film 2 -The BM is similar to that in PRV 3 -Cytogenetic are analyzed to exclude CML 4 -Platelet function tests are constantly abnormal ( Failure of aggregation with adrenaline)

Myelofibrosis(MF) Pathogenesis: Generalized haemopoietic stem cells proliferation with splenic & hepatic involvement in which there is extramedullary haemopoiesis , there is reactive fibrosis in BM secondary to hyperplasia of abnormal megakaryocytes. There is stimulation of fibroblast probably by platelet-derived growth factor secreted by megakaryocytes & platelets & inhibition of collagenase by platelet factor IV.

Clinical features 1 - 1/3 of patients has previous history of PRV & some times present with features of both disorders. 2 - An insidious onset in older people is usual with symptoms of anemia 3 -Symptoms due to massive splenomegaly 4 - loss of weight, anorexia & night sweats are common. Bleeding problems, bone pain, gout occur in minority of patients.

Lab. Findings: 1 -Anemia is usual but normal or increased hemoglobin may be found in some patients. 2 - The WBCs & platelets count are frequently high at the time of presentation, later in disease leucopenia & thrombocytopenia are common 3 - A leuco-erythroblastic blood film is found. The red cells show characteristic tear drop shape. 4 - BM is usually not obtainable by aspiration. Trephine biopsy may show hyper cellular marrow with increased reticulin-fiber pattern.

Other causes of marrow fibrosis: 1 -CML 6 - Metastatic carcinoma 2 - AML FAB 7 7 - Non-Hodgkin's lymphoma 3 -MDS 8 --Hodgkin's disease 4 - myeloma 9 - Tuberculosis 5 - Hairy cell leukemia 10 - Leishmaniasis

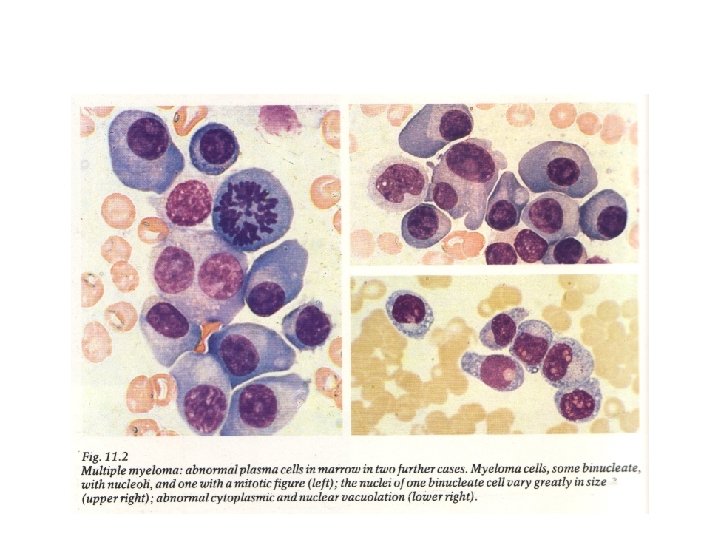
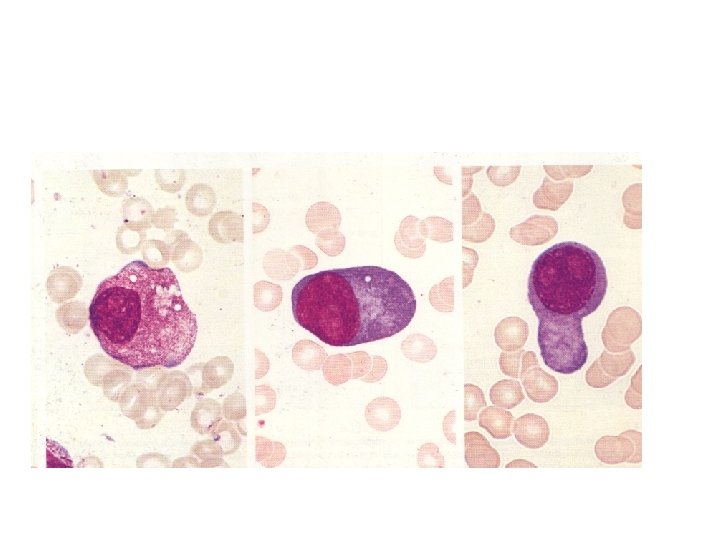
Multiple myeloma(MM) Is neoplastic monoclonal proliferation of BM plasma cells. Characterized by lytic bone lesion, plasma cell , accumulation in BM & presence of monoclonal protein in serum & urine. 98% of cases over the age of 40, with peak incidence in the 7 th decade

Clinical features 1 - Bone pain, pathological fracture. 2 - Features of anemia. 3 - Repeated infections because of deficient Ab & later on because neutropenia. 4 -features of renal failure & /or hypercalcaemia. 5 - Abnormal bleeding tendency because myeloma protein interfere with platelets function & coagulation factors & later on because of thrombocytopenia. 6 - Occasionally macroglossia , carpal tunnel syndrome, diarrhea due to amyloid disease 7 - In 2% hyperviscosity syndrome.

Diagnosis ( Lab. Findings) : This depends on 3 principle findings 1 - In 98% of patients monoclonal protein occurs in the serum or urine or both. The serum paraprotein is Ig. G in 2/3 of cases. The urine contain Bence-Jones protein in 2/3 of cases which is free light chains ( κ or λ) of the same type of serum paraprotein 2 - BM shows increased plasma cells > 4% & usually > 30% often with abnormal form ( myeloma cells) , these cells are monoclonal B cells & express the same Ig heavy & light chain of serum monoclonal protein


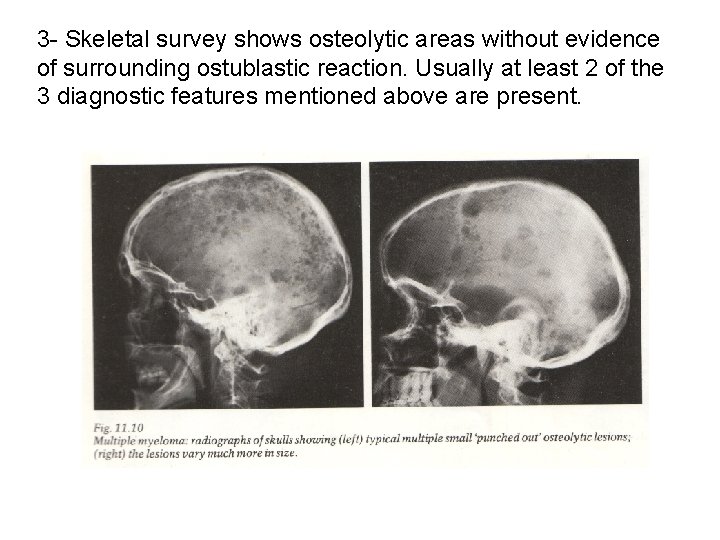
3 - Skeletal survey shows osteolytic areas without evidence of surrounding ostublastic reaction. Usually at least 2 of the 3 diagnostic features mentioned above are present.

Other lab. Findings: 1 -Normochromic , normocytic anemia. Rouleaux formation is marked in most cases. Neutropenia & Thrombocytopenia in advanced cases. Plasma cell seen in blood film in 15 % of cases. Leucoerythroblastic picture occasionally seen. 2 - High ESR( Erythrocyte sedimentation rate. ) 3 - Serum calcium increased in 45% of patients. 4 -Blood urea & serum creatinine increased in 20% if cases. 5 - Low serum albumin occurs in advanced disease.


Plasma cell leukaemia: This occurs either as a late complication of myeloma disease or often in younger patients as a primary disease characterized by the presence of 20% or more plasma cells in the blood, with an absolute count of>2× 109/L. There is more liver & spleen involvement than in myeloma, the paraprotein concentration in serum is often low. The results therapy is poor.