Nocardiosis NOCARDIA SPECIES Nocardia Aerobic Grampositive bacilli of

Nocardiosis

NOCARDIA SPECIES • Nocardia – Aerobic Gram-positive bacilli of with branching filament. – Weakly acid fast • Common natural inhabitants of the soil • Rare among normal population, most infections occurring in immuno-compromised hosts. • Structural lung disease, pulmonary alveolar proteinosis (PAP), diabetes mellitus is also known risk factors.
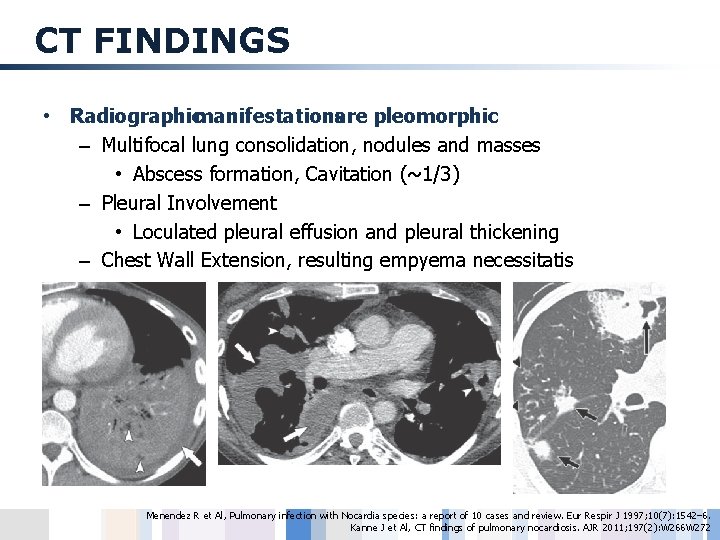
CT FINDINGS • Radiographicmanifestationsare pleomorphic – Multifocal lung consolidation, nodules and masses • Abscess formation, Cavitation (~1/3) – Pleural Involvement • Loculated pleural effusion and pleural thickening – Chest Wall Extension, resulting empyema necessitatis Menendez R et Al, Pulmonary infection with Nocardia species: a report of 10 cases and review. Eur Respir J 1997; 10(7): 1542– 6. Kanne J et Al, CT findings of pulmonary nocardiosis. AJR 2011; 197(2): W 266 W 272

DIFFERENTIAL DIAGNOSIS • Tuberculosis – Mediastinaland hilar lymphadenopathy is not a usual feature of pulmonary nocardiosis • Actinomycosis – Usually develops in patients with poor dentition – Immunocompromise does not appear to be a risk factor of actinomycosis • Septic lung • Vasculitis • Malignancy Menendez R et Al, Pulmonary infection with Nocardia species: a report of 10 cases and review. Eur Respir J 1997; 10(7): 1542– 6. Kanne J et Al, CT findings of pulmonary nocardiosis. AJR 2011; 197(2): W 266 W 272

TREATMENT • Long-term antibiotics – 1 st : TMP-SMX – 2 nd : amikacin, imipenem – 6 months to 1 year in pulmonary or disseminated form – 1 year or longer, with CNS involvement • Surgical drainage when required – chest wall abscesses and empyema may require surgical débridement Menendez R et Al, Pulmonary infection with Nocardia species: a report of 10 cases and review. Eur Respir J 1997; 10(7): 1542– 6. Kanne J et Al, CT findings of pulmonary nocardiosis. AJR 2011; 197(2): W 266 W 272

CASE 2 • M/71 • C. C: dyspnea for 2 -3 months • S/P Right thyroidectomy for papillary thyroid cancer (5 YA)
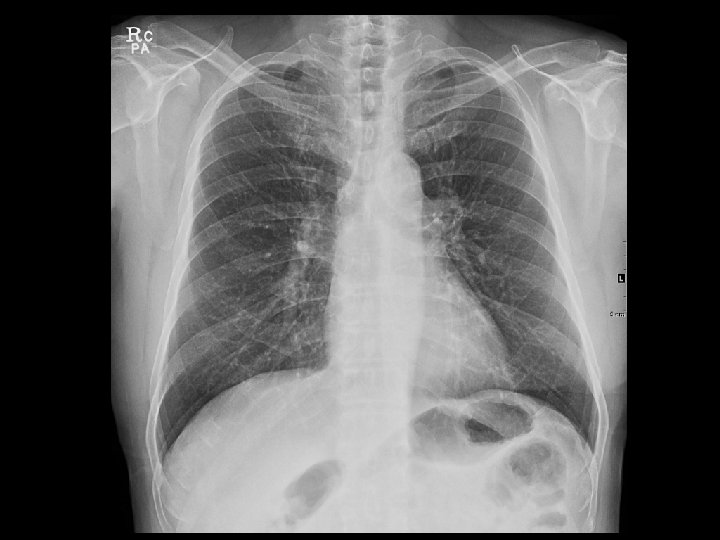
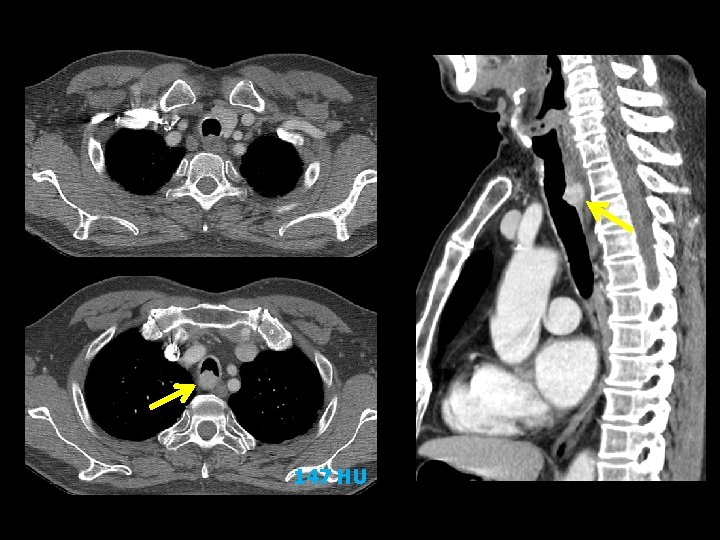
147 HU
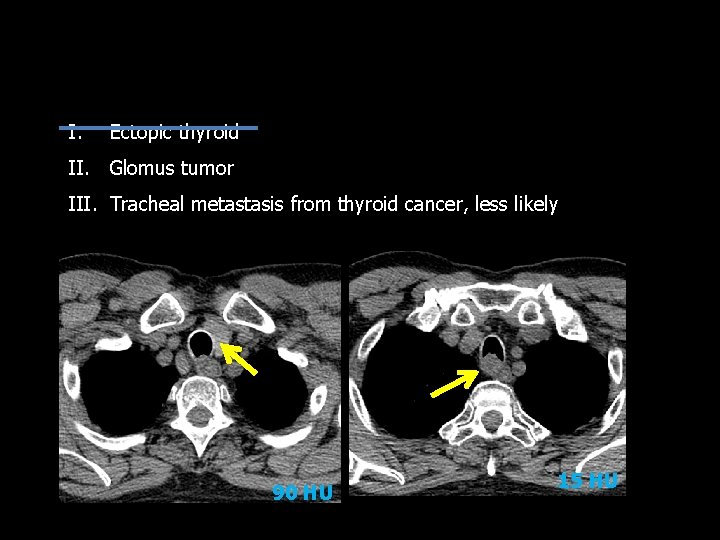
I. Ectopic thyroid II. Glomus tumor III. Tracheal metastasis from thyroid cancer, less likely 90 HU 15 HU
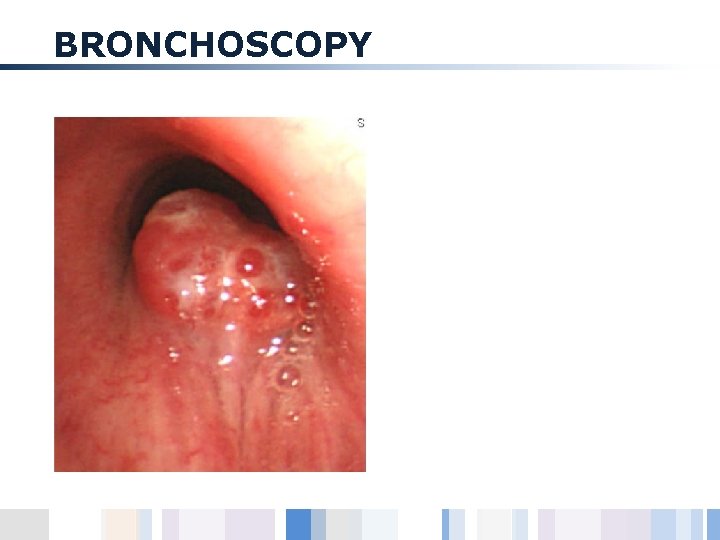
BRONCHOSCOPY
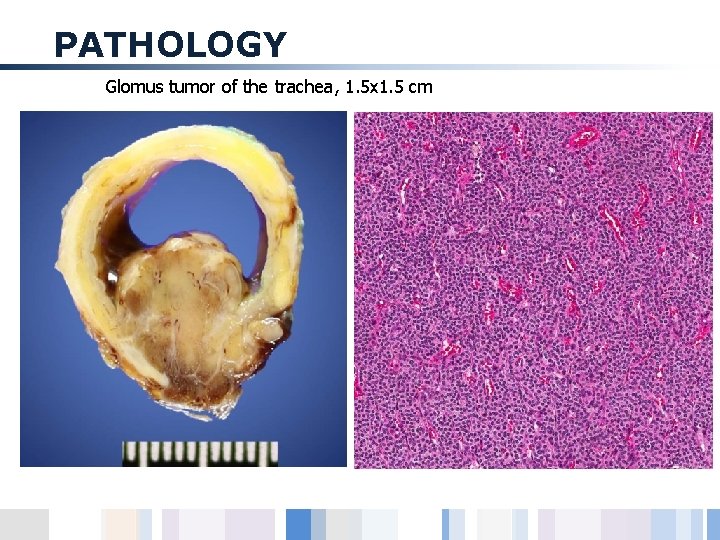
PATHOLOGY Glomus tumor of the trachea, 1. 5 x 1. 5 cm
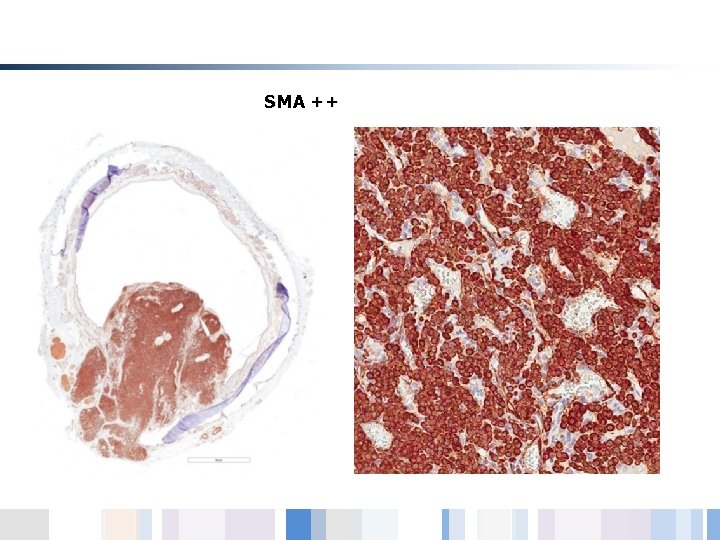
SMA ++

Glomus tumor of the Trachea

TRACHEAL GLOMUS TUMOR • Glomus tumor : benign, rare neoplasm of perivascular smooth muscle – m/c in subungal area – Unusual sites of origin : stomach, mediastinum, lung and trachea • Glomus tumor of trachea : extremely rare (< 100 cases in literature) – – – Even distribution in upper / middle / lower trachea Posterior wall of the trachea Submucosal origin, endoluminal polypoid growth Mean 2. 0 cm (1. 2 - 4. 5 cm) Mostly not invasive Characteristic histology : sheets and nests of round cells surrounding numerous vascular spaces

TRACHEAL GLOMUS TUMOR • Presentation – Dyspnea, cough, hemoptysis – May mimic asthma • Treatment – Excision : TOC • To prevent potential airway obstruction – Recurrence in 10% – ND-Yag LASER, rigid bronchoscopic resection
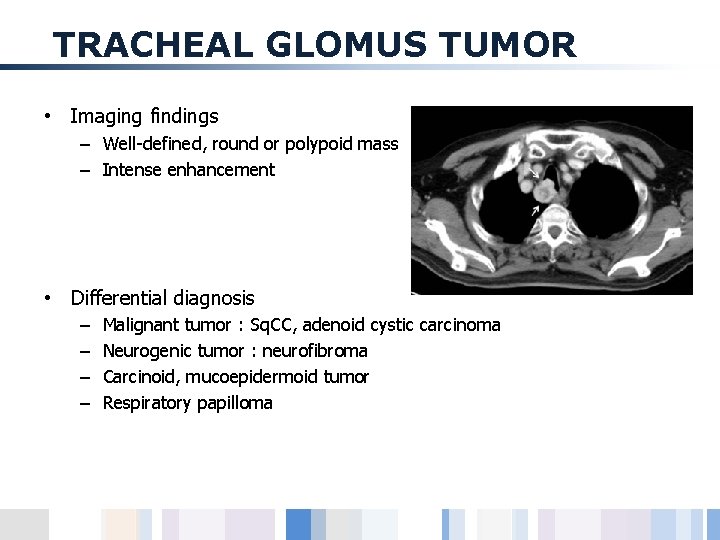
TRACHEAL GLOMUS TUMOR • Imaging findings – Well-defined, round or polypoid mass – Intense enhancement • Differential diagnosis – – Malignant tumor : Sq. CC, adenoid cystic carcinoma Neurogenic tumor : neurofibroma Carcinoid, mucoepidermoid tumor Respiratory papilloma
- Slides: 16