NIHR Southampton Biomedical Research Centre NAFLD and extrahepatic

NIHR Southampton Biomedical Research Centre NAFLD and extra-hepatic complications: what tests, which treatment and why worry? Christopher Byrne Professor of Endocrinology and Metabolism University of Southampton & University Hospital Southampton NIHR Biomedical Research Centre Southampton The Southampton Biomedical Research Centre is funded by the National Institute for Health Research (NIHR) and is a partnership between University Hospital Southampton Foundation Trust and the University of Southampton

Disclosures Research support Abbott/Pronova Research support Chr Hansen

Content NAFLD: what is it and does it matter? The spectrum of liver disease in NAFLD and extra-hepatic complications: Relationships between NAFLD, obesity, type 2 DM and CVD NAFLD: what tests? Case report of person presenting with NAFLD: which treatments?
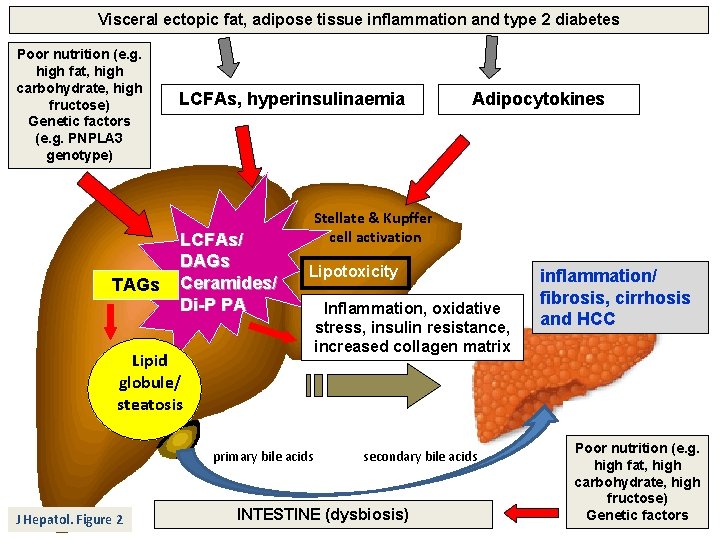
Visceral ectopic fat, adipose tissue inflammation and type 2 diabetes Poor nutrition (e. g. high fat, high carbohydrate, high fructose) Genetic factors (e. g. PNPLA 3 genotype) TAGs LCFAs, hyperinsulinaemia LCFAs/ DAGs Ceramides/ Di-P PA Stellate & Kupffer cell activation Lipotoxicity Lipid globule/ steatosis primary bile acids J Hepatol. Figure 2 Adipocytokines Inflammation, oxidative stress, insulin resistance, increased collagen matrix secondary bile acids INTESTINE (dysbiosis) inflammation/ fibrosis, cirrhosis and HCC Poor nutrition (e. g. high fat, high carbohydrate, high fructose) Genetic factors
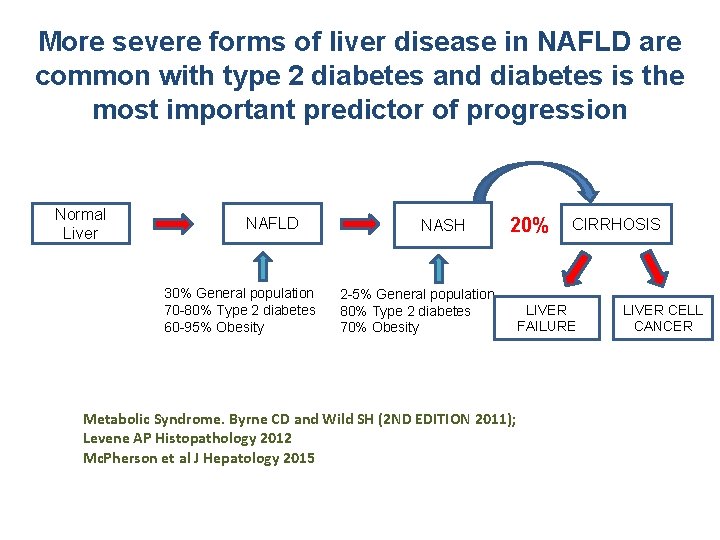
More severe forms of liver disease in NAFLD are common with type 2 diabetes and diabetes is the most important predictor of progression Normal Liver NAFLD 30% General population 70 -80% Type 2 diabetes 60 -95% Obesity NASH 20% 2 -5% General population 80% Type 2 diabetes 70% Obesity Metabolic Syndrome. Byrne CD and Wild SH (2 ND EDITION 2011); Levene AP Histopathology 2012 Mc. Pherson et al J Hepatology 2015 CIRRHOSIS LIVER FAILURE LIVER CELL CANCER
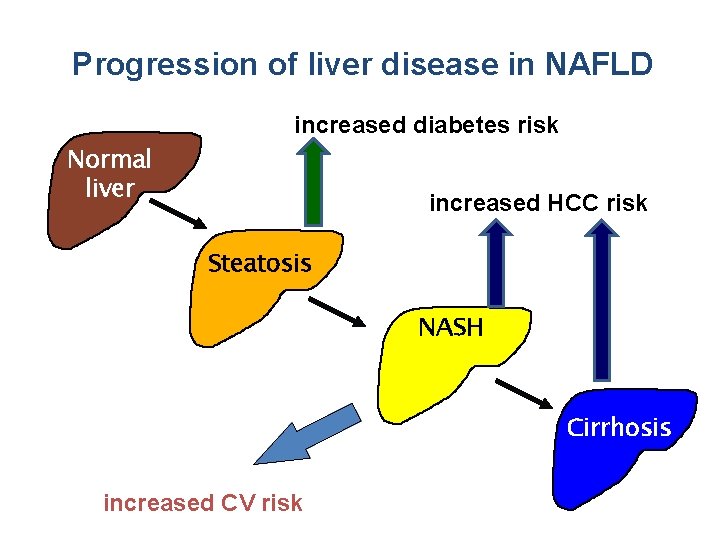
Progression of liver disease in NAFLD increased diabetes risk Normal liver increased HCC risk Steatosis NASH Cirrhosis increased CV risk
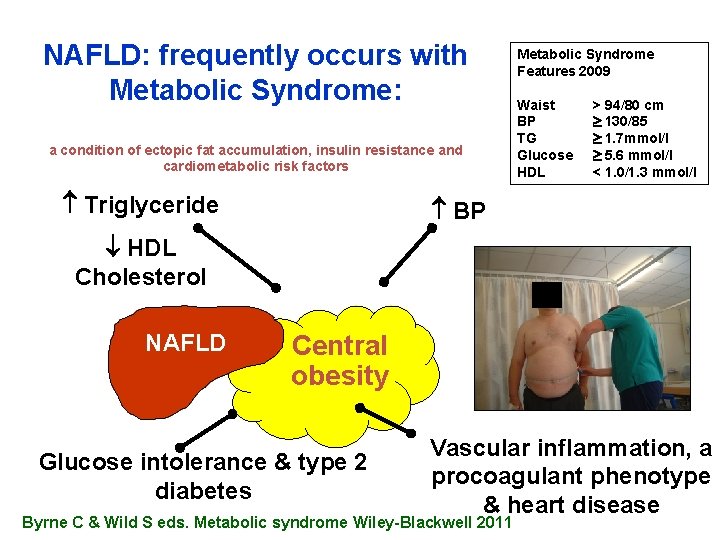
NAFLD: frequently occurs with Metabolic Syndrome: a condition of ectopic fat accumulation, insulin resistance and cardiometabolic risk factors Triglyceride Metabolic Syndrome Features 2009 Waist BP TG Glucose HDL > 94/80 cm 130/85 1. 7 mmol/l 5. 6 mmol/l < 1. 0/1. 3 mmol/l BP HDL Cholesterol NAFLD Central obesity Glucose intolerance & type 2 diabetes Vascular inflammation, a procoagulant phenotype & heart disease Byrne C & Wild S eds. Metabolic syndrome Wiley-Blackwell 2011

Does NAFLD matter? Southampton-Seoul & Southampton Verona collaborations (2012 -date) • • • • • • Can simple biochemical and anthropometric measures be used to predict who will develop NAFLD? . . . . No BMC Gastroenterology 2012 Does NAFLD predict incident diabetes? . . Yes Diabetes Care 2012 a, JCE&M 2013 Does NAFLD predict incident hypertension? . . . Yes Journal of Hepatology 2014 What is the relationship between NAFLD and pre-clinical atherosclerosis? Diabetes Care 2012 b, ATVB 2013…………NAFLD is an independent risk factor Does fatty liver occur in metabolically healthy obese people. . . Yes in some NMCD 2013, JCE&M 2015 Circulating markers of liver function and cardiovascular disease risk……Increased GGT is associated with all cause, cancer and CVD mortality (probably a marker of oxidative stress and NOT NAFLD or ALD. Arterioscler Thromb Vasc Biol. 2015 May 14. pii: ATVBAHA. 115. 305235. [Epub ahead of print] Clinical Chemistry 2015 Jul 7. pii: clinchem. 2015. 240424 How should NAFLD be managed in people with diabetes? . . . . Needs to be identified and treated! JCE&M 2013 NAFLD and incident AF. . . NAFLD is an independent risk factor for incident AF PLo. S One 2014 NAFLD and aortic and mitral valve calcification ……. . increased incidence Metabolism 2015 May 1. pii: S 0026 -0495(15)00108 -0. doi: 10. 1016/j. metabol. 2015. 04. 003. [Epub ahead of print] Increased HDL-C/Apo-AI ratio and CVD mortality…. increased HDL-C/Apo-AI ratio is associated with increased all cause, cancer and CVD mortality Heart. 2015 Apr; 101(7): 553 -8.

Extra-hepatic complications of NAFLD • Cardiovascular disease and cardiac disease • Type 2 diabetes • Chronic renal failure (defined by e. GFR≤ 60 ml/min or proteinuria) Byrne C & Targher G J Hepatol 2015 18/06/2013
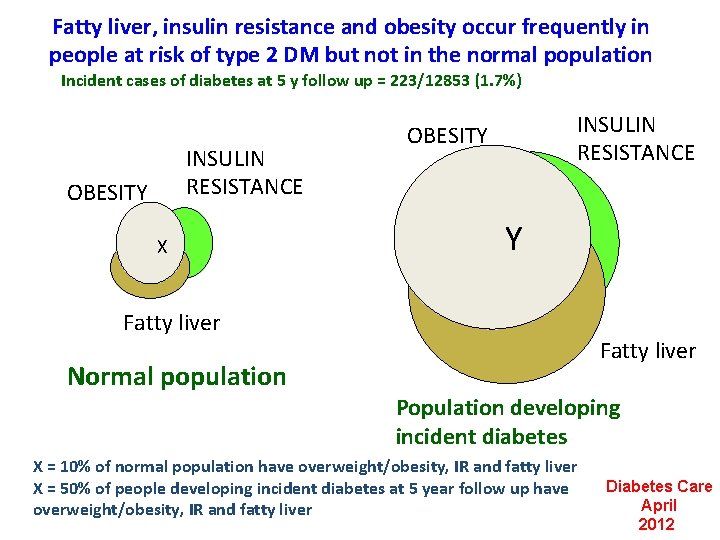
Fatty liver, insulin resistance and obesity occur frequently in people at risk of type 2 DM but not in the normal population Incident cases of diabetes at 5 y follow up = 223/12853 (1. 7%) INSULIN RESISTANCE OBESITY X INSULIN RESISTANCE OBESITY Y Fatty liver Normal population Population developing incident diabetes X = 10% of normal population have overweight/obesity, IR and fatty liver X = 50% of people developing incident diabetes at 5 year follow up have overweight/obesity, IR and fatty liver Diabetes Care April 2012
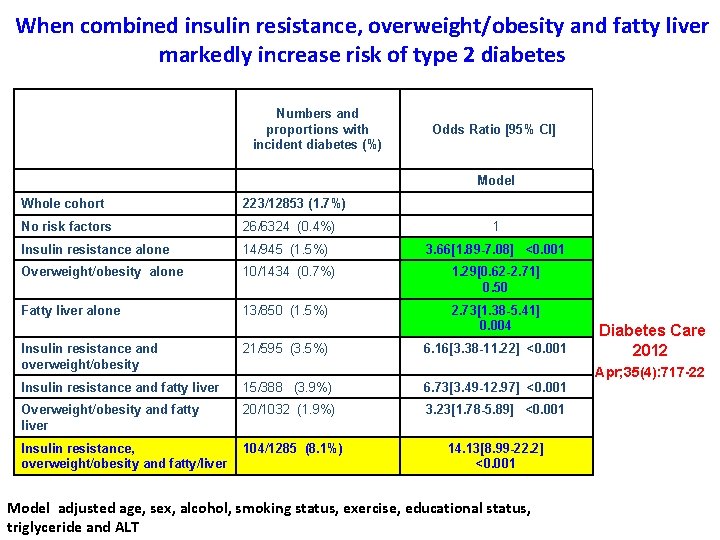
When combined insulin resistance, overweight/obesity and fatty liver markedly increase risk of type 2 diabetes Numbers and proportions with incident diabetes (%) Odds Ratio [95% CI] Model Whole cohort 223/12853 (1. 7%) No risk factors 26/6324 (0. 4%) 1 Insulin resistance alone 14/945 (1. 5%) 3. 66[1. 89 -7. 08] <0. 001 Overweight/obesity alone 10/1434 (0. 7%) 1. 29[0. 62 -2. 71] 0. 50 Fatty liver alone 13/850 (1. 5%) 2. 73[1. 38 -5. 41] 0. 004 Insulin resistance and overweight/obesity 21/595 (3. 5%) 6. 16[3. 38 -11. 22] <0. 001 Insulin resistance and fatty liver 15/388 (3. 9%) 6. 73[3. 49 -12. 97] <0. 001 Overweight/obesity and fatty liver 20/1032 (1. 9%) 3. 23[1. 78 -5. 89] <0. 001 Insulin resistance, overweight/obesity and fatty/liver 104/1285 (8. 1%) 14. 13[8. 99 -22. 2] <0. 001 Diabetes Care 2012 Apr; 35(4): 717 -22 Model adjusted age, sex, alcohol, smoking status, exercise, educational status, triglyceride and ALT
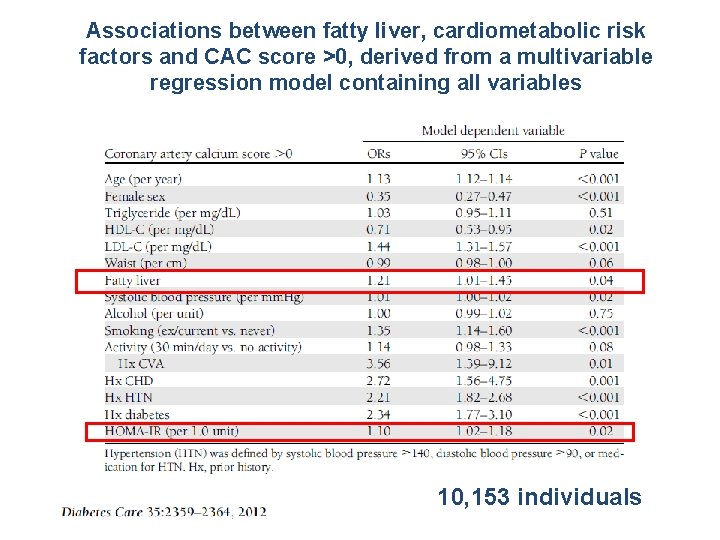
Associations between fatty liver, cardiometabolic risk factors and CAC score >0, derived from a multivariable regression model containing all variables 10, 153 individuals

What tests? - case report 45 y man Asymptomatic Smokes 10/day – 20 years Type 2 diabetes – 1 year Sedentary occupation, 14 -21 units alcohol/wk Married, 2 children ‘unfit & stressed at work’ Metformin 2 g/day

O/E BMI 36 kg/m 2 ‘Increased waist circumference’ 104 cms Bp 145/90 mm. Hg Fasting glucose 9. 0 mmol/l Chol 6. 0 mmol/l, LDL = 3. 2 mmol/l Fasting Tg = 4. 0 mmol/l HDLc = 0. 8 mmol/l Hb. A 1 c = 9. 0 % NB all five features of Met. S

ALT = 50 iu/l ( 5 -35 iu/l) g. GT = 50 iu/l ( < 55 iu/l) LFTs otherwise entirely normal U&E normal Urinalysis – trace protein ACR = 2. 5 mg/mmol

Ultrasound test diagnoses liver fat only [or possibly ‘Fatty liver index test (BMI + waist + TG + GGT + algorithm ≥ 60’] ‘Echogenic liver texture in keeping with moderate to severe fatty liver’ Liver fibrosis markers (normal or increased) Hyaluronic acid (HA) normal, PIIIPNP increased [and TIMP-1] (HA + PIIINP + TIMP 1 + algorithm = ELF test, Siemens) Other causes of fatty liver disease Alcohol intake? - minimal Iron status - normal Autoantibodies – slight increases anti smooth cell Ig. G Immunoglobulins - normal Hepatitis status (? Hep B or C infection) negative
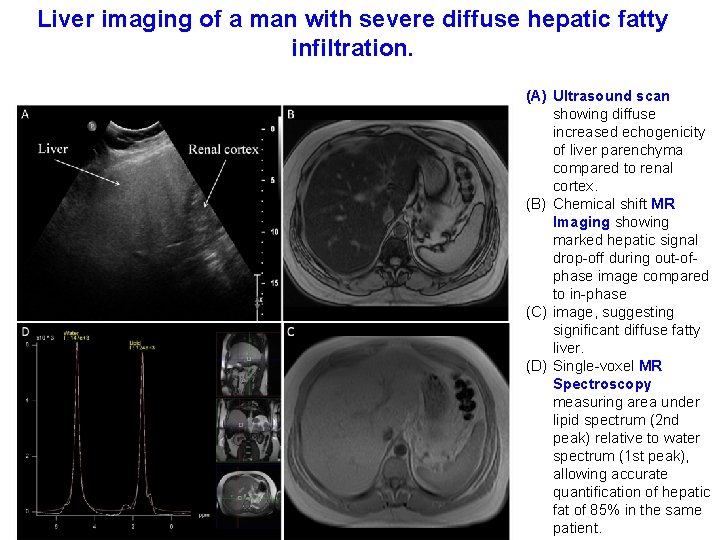
Liver imaging of a man with severe diffuse hepatic fatty infiltration. (A) Ultrasound scan showing diffuse increased echogenicity of liver parenchyma compared to renal cortex. (B) Chemical shift MR Imaging showing marked hepatic signal drop-off during out-ofphase image compared to in-phase (C) image, suggesting significant diffuse fatty liver. (D) Single-voxel MR Spectroscopy measuring area under lipid spectrum (2 nd peak) relative to water spectrum (1 st peak), allowing accurate quantification of hepatic fat of 85% in the same patient.
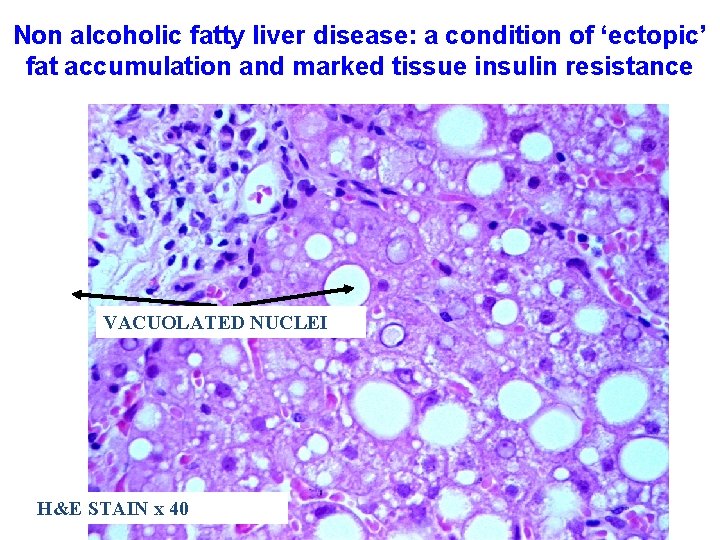
Non alcoholic fatty liver disease: a condition of ‘ectopic’ fat accumulation and marked tissue insulin resistance VACUOLATED NUCLEI H&E STAIN x 40
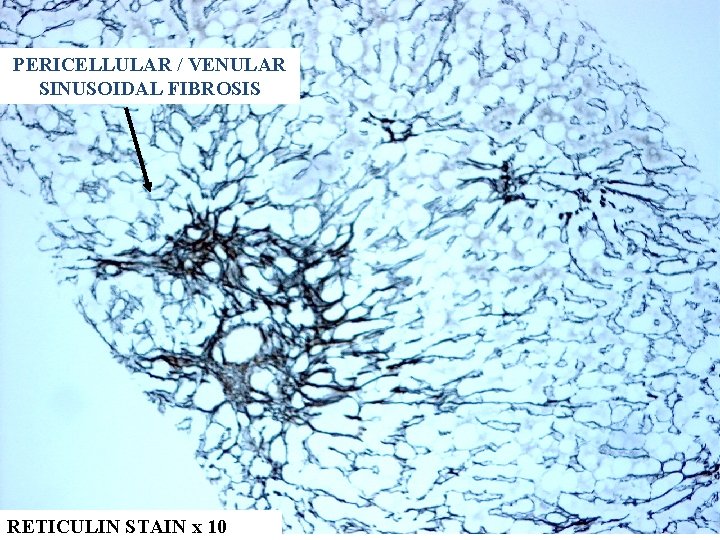
PERICELLULAR / VENULAR SINUSOIDAL FIBROSIS RETICULIN STAIN x 10
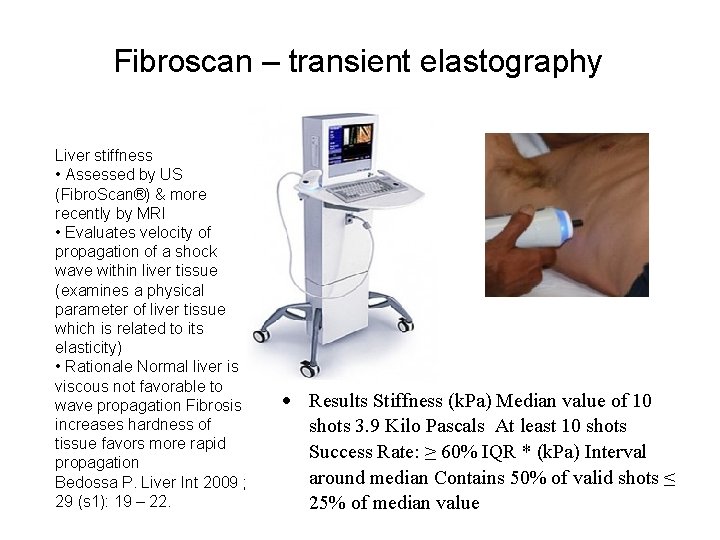
Fibroscan – transient elastography Liver stiffness • Assessed by US (Fibro. Scan®) & more recently by MRI • Evaluates velocity of propagation of a shock wave within liver tissue (examines a physical parameter of liver tissue which is related to its elasticity) • Rationale Normal liver is viscous not favorable to wave propagation Fibrosis increases hardness of tissue favors more rapid propagation Bedossa P. Liver Int 2009 ; 29 (s 1): 19 – 22. Results Stiffness (k. Pa) Median value of 10 shots 3. 9 Kilo Pascals At least 10 shots Success Rate: ≥ 60% IQR * (k. Pa) Interval around median Contains 50% of valid shots ≤ 25% of median value
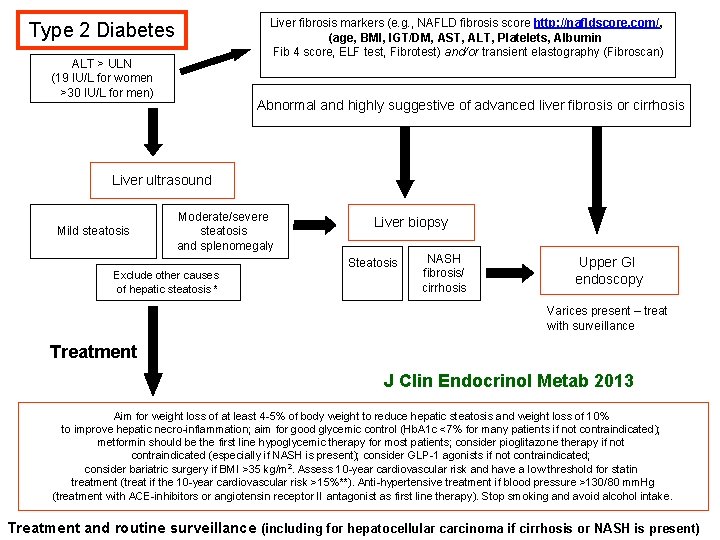
Liver fibrosis markers (e. g. , NAFLD fibrosis score http: //nafldscore. com/, (age, BMI, IGT/DM, AST, ALT, Platelets, Albumin Fib 4 score, ELF test, Fibrotest) and/or transient elastography (Fibroscan) Type 2 Diabetes ALT > ULN (19 IU/L for women >30 IU/L for men) Abnormal and highly suggestive of advanced liver fibrosis or cirrhosis Liver ultrasound Mild steatosis Moderate/severe steatosis and splenomegaly Exclude other causes of hepatic steatosis * Liver biopsy Steatosis NASH fibrosis/ cirrhosis Upper GI endoscopy Varices present – treat with surveillance Treatment J Clin Endocrinol Metab 2013 Aim for weight loss of at least 4 -5% of body weight to reduce hepatic steatosis and weight loss of 10% to improve hepatic necro-inflammation; aim for good glycemic control (Hb. A 1 c <7% for many patients if not contraindicated); metformin should be the first line hypoglycemic therapy for most patients; consider pioglitazone therapy if not contraindicated (especially if NASH is present); consider GLP-1 agonists if not contraindicated; consider bariatric surgery if BMI >35 kg/m 2. Assess 10 -year cardiovascular risk and have a low threshold for statin treatment (treat if the 10 -year cardiovascular risk >15%**). Anti-hypertensive treatment if blood pressure >130/80 mm. Hg (treatment with ACE-inhibitors or angiotensin receptor II antagonist as first line therapy). Stop smoking and avoid alcohol intake. Treatment and routine surveillance (including for hepatocellular carcinoma if cirrhosis or NASH is present)

Treatment? • Lifestyle • Weight loss, physical activity (alcohol? ) • Nutrition? • Drugs – Metformin- no effect – GLP-1 agonists –weight loss benefical – Statins – no effect but safe – Pioglitazone – may be beneficial but side effects – Vitamin E - ? hazardous – Omega-3 fatty acids –possibly – Probiotics? – FXR agonists – FLINT trial showed benefit and stopped early
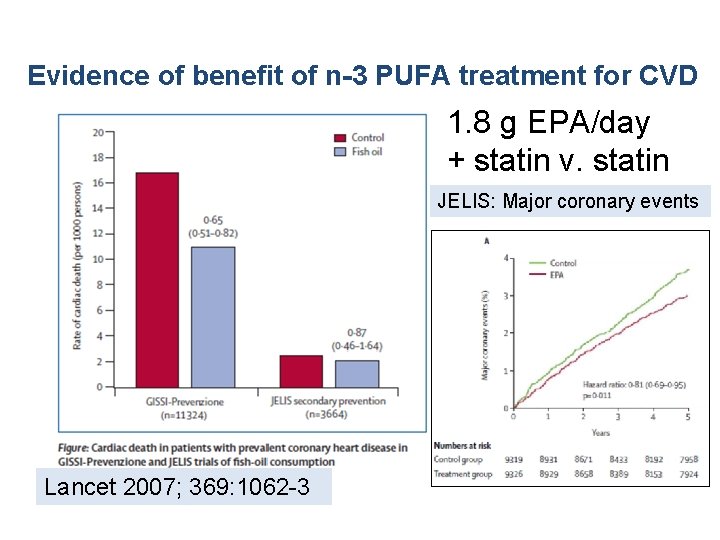
Evidence of benefit of n-3 PUFA treatment for CVD 1. 8 g EPA/day + statin v. statin JELIS: Major coronary events Lancet 2007; 369: 1062 -3
Will high dose omega-3 PUFA improve liver disease AND decrease CVD risk in NAFLD? Study design Wessex Evaluation of fatty Liver and Cardiovascular markers in NAFLD (non alcoholic fatty liver disease) with OMacor th. Erapy Several PICs from around NAFLD • Double blind placebo-control trial • Treatment: Omacor 4 gr per day or 4 g olive oil (placebo) Ø Omacor 1 gr capsule (1000 mg) of omega-3 -acid comprising EPA (460 mg) and DHA (380 mg) x 4. • Duration of intervention: 15 -18 months • Primary outcome: Decrease in liver fat (magnetic resonance spectroscopy-MRS) • Improvements in two histologically validated liver fibrosis scores Scorletti E, et al on behalf of the WELCOME* Trial Investigators. Contemporary Clinical Trials. 2014.
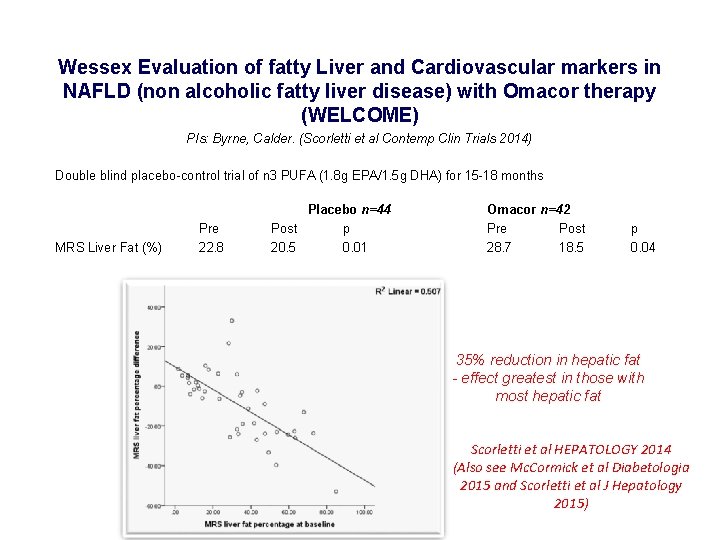
Wessex Evaluation of fatty Liver and Cardiovascular markers in NAFLD (non alcoholic fatty liver disease) with Omacor therapy (WELCOME) PIs: Byrne, Calder. (Scorletti et al Contemp Clin Trials 2014) Double blind placebo-control trial of n 3 PUFA (1. 8 g EPA/1. 5 g DHA) for 15 -18 months MRS Liver Fat (%) Pre 22. 8 Placebo n=44 Post p 20. 5 0. 01 Omacor n=42 Pre Post 28. 7 18. 5 p 0. 04 35% reduction in hepatic fat - effect greatest in those with most hepatic fat Scorletti et al HEPATOLOGY 2014 (Also see Mc. Cormick et al Diabetologia 2015 and Scorletti et al J Hepatology 2015)

Is Synbiotic treatment beneficial for NAFLD? ‘INvestigation of SYnbiotic Treatm. Ent in NAFLD’ (INSYTE) Investigation of the effects of a synbiotic on liver fat, disease biomarkers and intestinal microbiota in non-alcoholic fatty liver disease www. clinicaltrials. gov registration number NCT 01680640 Local research ethics committee approval has been granted (REC reference: 12/SC/0614).

NAFLD and diabetes: does it matter, what tests and what treatment? Conclusions: • NAFLD very common in diabetes: diabetes increases risk of progression • NAFLD risk factor for type 2 DM/CVD/HCC/cirrhosis independently of central obesity and IR and other features of Met. S • NAFLD – diagnosis begins with abnormal ALT and ultrasound (detects liver fat only). Biomarkers useful for severe fibrosis. • Fibroscan useful for serious fibrosis • Biopsy still the gold standard • Lifestyle and management of risk factors and

Philip Calder Geraldine Clough Acknowledgments • Loke Bhatia Keith Mc. Cormick Debbie Smith Eleonora Scorletti Lucinda England Gillian Wise Sanchia Triggs Bridget Clancy Gemma Rood Norma Diaper Kate Nash/Mark Wright/Nick Sheron Nick Curzen Drubo Rahkit Angela Darekar, Alison Fletcher Jen Bryant, Charles Peebles Bournemouth, Poole, Winchester, Portsmouth, Basingstoke Io. W, • Oxford Leanne Hodson and Keith Frayn • Surrey Margaret Umbleby, Nicola Jackson, F. Shojaee. Moradie • BRC staff • WTCRF staff – Jennifer, Enrico and Kerrie Medical students, Pat Taylor and staff. Pharmacy (Joanna Cantle) • Seoul. Korea Ki-Chul Sung • Verona, Italy Giovanni Targher Funding Bodies Diabetes UK & NIHR Helen Moyses, Karen Long, Ching Cheng, Carrie Bolt
- Slides: 28