NICU Basics Kirsti Martin MD PGY 5 NICU

NICU Basics Kirsti Martin, MD PGY 5

NICU Learning Objectives Learn about transitional physiology and how this relates to neonatal resuscitation Learn the differences between sick and well infants, and when an infant needs a higher level of care in a NICU Learn about the care of and diseases affecting premature infants, to gain perspective when you care for them in a primary care setting Learn and build upon basic ICU concepts in your first exposure to ICU care Do as much cool stuff as possible!

Today’s Learning Objectives Learn some basics about prematurity, including Definition Potential Complications Delivery Room Management Systems-Based Approach to Preterm Admission Milestones of the Hospital Course Discharge Criteria Highlight important information to know on your first day in the NICU

Prematurity Preterm labor Maternal infection Neonatal infection Premature rupture of membranes Advanced cervical dilation …. . ? Preterm induction of labor or preterm c-section delivery Most commonly seen for pre-eclampsia Delivery for fetal decelerations in HR while mother admitted for other reasons (non -reassuring fetal heart tracing)

Prematurity Periviability – 23 -24 weeks gestation Lungs still in canalicular phase of embryonic development Canaliculi form from terminal bronchioles respiratory bronchioli and alveolar ducts (not sacs yet) Type 1 pneumocytes (primary structural cell of alveoli) just differentiating from type II Capillary network surrounding terminal bronchioles from mesenchyme just forming Surfactant begins to be produced by type II pneumocytes by 24 weeks Parents counseled about active ICU care vs comfort care without resuscitation Extremely preterm – less than 28 weeks gestation Very preterm – less than 32 weeks gestation Thought process behind the care of these infants is similar, with lower gestational ages more complicated due to higher risk for hemodynamic instability, poor respiratory status, feeding intolerance, etc

Prematurity Infants born less than 32 weeks or 1500 g (3 lbs 4. 9 oz) at risk for Respiratory Distress Syndrome – difficulty with oxygenation and/or ventilation due to lack of surfactant production Bronchopulmonary dysplasia – the lasting respiratory effects of being born prematurely with underdeveloped lungs; can involve chronic changes to lungs as a result of mechanical ventilation – defined as the need for oxygen or respiratory support at 36 weeks corrected gestational age Intraventricular hemorrhage – bleeding of the vessels in the germinal matrix, found in the lateral ventricles of the brain Necrotizing enterocolitis – disease of the intestines with multifactorial causes; can cause bowel inflammation/necrosis, abdominal perforation requiring abdominal surgery for resection of affected areas Retinopathy of prematurity – abnormal development of retinal blood vessels secondary to exposure to supplemental oxygen; can cause blindness Apnea of prematurity – prolonged pauses in breathing secondary to immature neural regulation of breathing Hypothermia Hypo/hyperglycemia Infection ……

How we care for preterm infants The OB team calls you to say that they will be going to the OR shortly for the delivery of a 27+4 week infant Mother is a 29 year old G 1 P 0; came to triage for rupture of membranes earlier today, and now the fetal heart rate keeps decreasing into the 80 s before recovering; lasting ~3 minutes Prenatal labs – A+, ab negative, Hep Bs. Ag neg, HIV negative, RPR non-reactive, rubella immune, varicella immune, G/C negative, GBS unknown Mother received one dose of betamethasone this morning, as well as IV magnesium and antibiotics Estimated fetal weight from this morning’s ultrasound is 800 g

Important Highlights Blood type and antibody status HIV If positive would need to initiate treatment urgently (IV penicillin) Betamethasone Antenatal steroids work to rapidly mature the fetal lung to prepare for birth Complete course (two doses 24 hrs apart; complete 48 hrs from first dose) decreases risk of BPD, IVH, NEC, etc… Magnesium If positive or unknown, would need Hep B vaccine and HBIG within 12 hrs RPR If positive would need to initiate treatment urgently (IV zidovudine) Hep. Bs. Ag Risk of hyperbilirubinemia due to hemolysis from Rh disease, ABO incompatibility, other Ab mediated process A tocolytic but has also been shown to decrease the risk of cerebral palsy in premature infants Antibiotics Treat an infection that may have been caused by or be a result of premature rupture of membranes May partially treat fetal infection
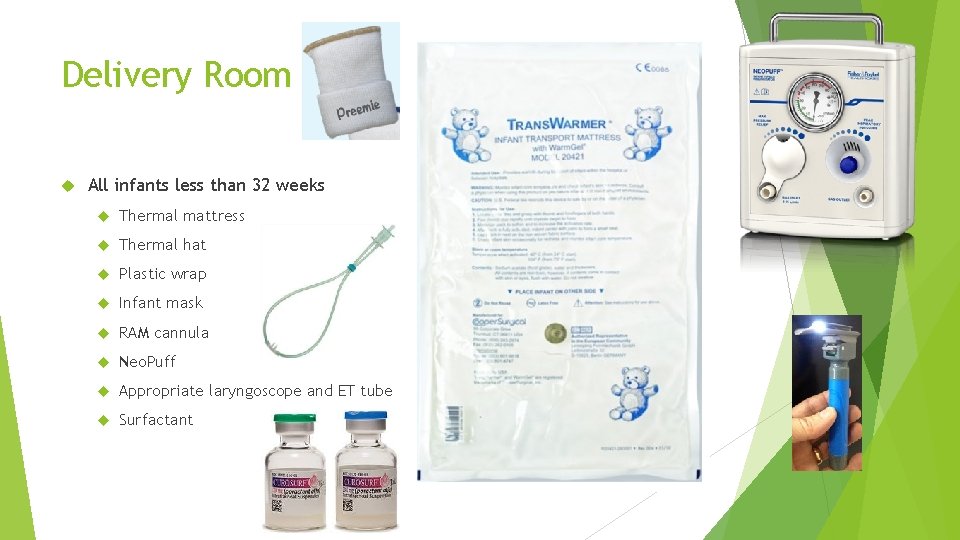
Delivery Room All infants less than 32 weeks Thermal mattress Thermal hat Plastic wrap Infant mask RAM cannula Neo. Puff Appropriate laryngoscope and ET tube Surfactant

Neo. Puff Demonstration https: //www. youtube. com/watch? v=G 9 -Kezha. XJM

Infant is born Infant with good tone and spontaneous respirations, so delayed cord clamping x 30 seconds By transfer to the warmer, infant no longer breathing Simultaneously Infant placed in Neo. Wrap, on thermal mattress, and thermal hat placed RAM cannula placed into nose and pulse oximeter placed on right hand Nurse listens to heart rate HR is 70, and infant is still not breathing HR increases to 140, breath sounds are heard bilaterally, and infant begins to have spontaneous respiratory effort Breaths given via RAM cannula – NIPPV (non-invasive positive pressure ventilation) with peak inspiratory pressure (PIP) 25 and positive end-expiratory pressure (PEEP) 7 Fi. O 2 is titrated to maintain saturations appropriate for time of life At 10 minutes of life, on NIPPV 25/7 x 30, FIO 2 30%, infant placed in transporter and brought to NICU for admission

Systems Respiratory – consider the need for early surfactant based on FIO 2 requirement, work of breathing, or blood gas Access- place UVC with goal to be finished with placement and xray by 1 hour of life Cardiovascular – make sure blood pressure/perfusion is appropriate FEN/GI – write TPN/IV fluids and feeds for the infant Hematology – assess the infant’s hematology status ID – assess the infant’s risk for infectious disease Neuro – is the infant at risk for IVH?

Respiratory During transport, infant with desaturations requiring increase in NIPPV to 28/8 x 30, Fi. O 2 40% Due to high Fi. O 2 requirement suggestive of respiratory distress syndrome, infant will likely benefit from administration of exogenous surfactant to decrease surface tension in the alveoli and prevent atelectasis, promote gas exchange Infant is intubated, surfactant is administered by injection through a feeding tube into the ET tube in two equal aliquots, and infant is extubated back to NIPPV (INSURE method) After surfactant, Fi. O 2 decreases to 21% (nice job!) Sometimes, the need for surfactant is not this obvious early on Fi. O 2 requirement doesn’t happen until later (if at all) May have good oxygenation but poor ventilation (need blood gas to tell) Apnea of prematurity may start with resultant worsening respiratory status

Access Central access required to provide concentrated IV nutrition (total parenteral nutrition, TPN) Also used to draw labs Umbilical venous catheter Inserted through umbilical vein, passes through ductus venosus, into the inferior vena cava Goal location above diaphragm, at ~T 7 -8 All infants less than 31 weeks or 1500 g; 31 -32 weeks depends on clinical preference Umbilical arterial catheter Inserted into one of two umbilical arteries, passes into internal iliac artery, common iliac artery, and into aorta Carrier fluid is run through the line, and outputs a blood pressure waveform Goal location is T 6 -9 Less commonly used in our unit unless infant requires significant respiratory support or is hemodynamically unstable
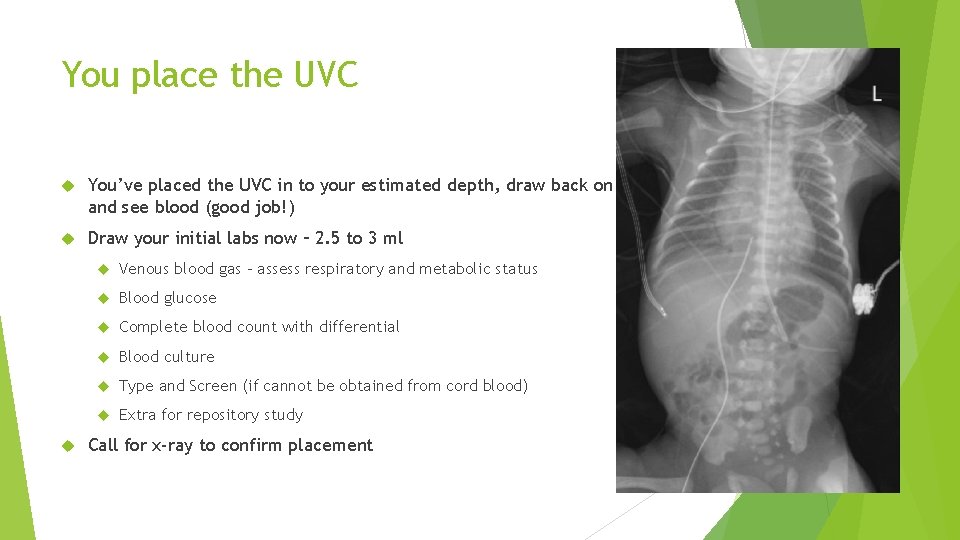
You place the UVC You’ve placed the UVC in to your estimated depth, draw back on your syringe, and see blood (good job!) Draw your initial labs now – 2. 5 to 3 ml Venous blood gas – assess respiratory and metabolic status Blood glucose Complete blood count with differential Blood culture Type and Screen (if cannot be obtained from cord blood) Extra for repository study Call for x-ray to confirm placement

Respiratory VBG - p. H 7. 25/p. CO 2 55/p. O 2 75/HCO 3 19/ base excess -4 At the time the VBG was drawn, the transcutaneous CO 2 monitor (TCOM) was reading 58 As you settle the infant after securing the UVC and putting the top of the “giraffe” (humidified isolette) down, the TCOM continues to downtrend and settles at 45 Infant receives first dose of caffeine at 4 hours of life (20 mg/kg), then daily after this (10 mg/kg) for prevention of apnea of prematurity

Cardiovascular Blood pressure typically obtained by cuff pressure, less commonly via UAC Desired mean arterial pressure (MAP) = infant’s gestational age in weeks Premature infants can have slight dip in MAP a few hours after birth (just below expected range), but if perfusion is good, urine output is stable, and infant otherwise stable, will typically recover without extra intervention

Hematology CBC WBC count 10. 5 with ANC 3000, 2 bands, 50 neutrophils Hb/Hct 15. 3/45. 7 Platelets 200 Normal premature Hct is 45, normal term Hct is 55 Transfuse PRBCs on first day for less than 35 Normal platelets 150 -450 k Transfusion thresholds vary with illness severity; typically between 30 -50 k Assess white blood cell count to see if it suggests infection Normal WBC count roughly 5, 000 -30, 000 Make sure ANC >1500 Calculate the I: T ratio (bands+other immature forms divided by neutrophils plus all immature forms) if >0. 2, more suggestive of infection

Hematology Order daily serum total bilirubin levels to start the second day of life Premature infants at higher risk for hyperbilirubinemia due to Increased RBC turnover due to decreased life span of premature RBC increased bilirubin production Decreased bilirubin clearance and conjugation due to immature liver Increased enterohepatic circulation of bilirubin At higher risk for bilirubin induced neurologic dysfunction Due lower albumin more free, unbound bilirubin that can cross the blood-brain barrier See survival guide for premature bilirubin curve for when to start phototherapy

Infectious Disease All infants under 32 weeks get 48 hour “sepsis rule out” While blood culture pending, ampicillin and gentamicin given x 48 hours Dosage and intervals in Epic! Optimal coverage for most common neonatal infections - Group B strep, E. coli Remember to obtain mother’s HIV, Hep. B, RPR, and GBS status GBS frequently unknown with preterm delivery, that’s ok

Fluids/Feeds Enteral feeds must be advanced slowly due to small stomach and risk of NEC Breast milk or donor breast milk (need consent) Preterm formula has significantly increased risk of NEC vs breast milk Fed via small orange feeding tube either through nose or mouth into stomach Refer to feeding protocol for recommendations for fluid amounts by GA On your survival guide! For 27 weekers, we start at 90 ml/kg/day Start feeds at 10 ml/kg/day within 6 -8 hours of birth, advance by 10 ml/kg BID Start TPN/Intralipids and carrier fluid through the second port of UVC at 80 ml/kg/day

Feeds Starting at 10 ml/kg/day 10 ml x 0. 8 kg = 8 ml/day kg/day 8 ml/day divided by 8 feeds in 24 hours (feeds are q 3 hrs) = 1 ml q 3 hrs To increase by 10 ml/kg BID 10 ml/kg = 1 ml q 3 hrs as above Write to increase feeds by 1 ml every 12 hours

Maximum Feeds Max feeds are typically 160 ml/kg/day Use birthweight to calculate this until infant surpasses birth weight 160 ml x 0. 8 kg = 128 ml/day , divided by 8 feeds/day = 16 ml/feed kg/day Initial feed order – Start feeds at 1 ml q 3 hrs. Advance by 1 ml q 12 hrs to a max of 16 ml q 3 hrs.

TPN/Carrier fluid Stock TPN started on first day typically – protein and glucose (D 10 base) Carrier fluids (heparinized ½ sodium acetate at 0. 5 ml/hr or 12 ml/day) plus TPN to equal 80 ml/kg/day Carrier fluid –--- 12 ml divided by 0. 8 kg = 15 ml/kg/day 80 ml/kg/day – 15 ml/kg/day = 65 ml/kg/day TPN ---- 65 ml x 0. 8 kg = 52 ml/day, divided by 24 hr/day = 2. 16 ml/hr (2. 2 ml/hr) kg/day

Intralipids The source of fat in TPN; stock TPN does not include this When you write custom TPN the next day, you must account for the intralipid as part of your total fluids 1 g IL = 5 ml/kg/day, 2 g IL = 10 ml/kg/day, 3 g IL = 15 ml/kg/day Total fluids of 80 ml/kg/day = 15 ml/kg/day carrier + 65 ml/kg/day TPN/IL So if we start 2 g IL, our TPN amount will decrease from 65 to 55 ml/kg/day 55 ml x 0. 8 kg = 44 ml/day, divided by 24 hrs/day = 1. 8 ml/hr kg/day

Decreasing IV fluids (TPN/IL) 80 ml/kg/day + (feeds) 80 ml/kg/day = Total fluid 160 ml/kg/day Feeds will continue to increase, but your TPN will need to decrease as feeds increase to keep total fluids at 160 ml/kg/day Feeds increase by 1 ml every 12 hours The IV fluid equivalent of 1 ml feed every 3 hours is 1 ml = 0. 33 ml/hr 3 hours With each feed increase of 1 ml every 12 hrs, decrease IV fluids by 0. 3 ml/hr to maintain TF 160 ml/kg/day

Other things to order on admission AM daily BMP while on TPN, to adjust TPN electrolytes or fluid status as needed AM daily triglycerides as needed when intralipid introduced or increased Head ultrasound to assess for IVH one week from birth; would rather have it 7 -10 days out than earlier than 7 days from birth Caffeine! Vitamin K and erythromycin!

General Progression of Hospital Course Infant weans slowly from NIPPV to CPAP over the course of weeks; Fi. O 2 remains in the low 20 s, increasing mostly with apnea of prematurity spells; at 32 -33 weeks CGA, infant trialed off of CPAP in room air, and is hopefully successful! Sometimes need positive pressure for longer, sometimes need low flow nasal cannula; some infants go home with nasal cannula Caffeine discontinued when apnea spells decrease (around 33+5 weeks) UVC comes out between DOL 5 and 6 when feeds reach 120 ml/kg/day, reaches full feeds by 1 week Feed and grow! At 34 weeks, neurologically mature enough to suck, swallow, and breathe; can start to learn to orally feed at breast or with bottle

Discharge Criteria No apnea, bradycardia, or desaturation spells at rest requiring intervention for at least 5 days Must be 10 days off of caffeine Must be 1800 grams (4 pounds – carseats do not fit infants smaller than this) Must be able to keep themselves warm in an open crib while dressed and swaddled Must be able to take enough feeds by mouth (without NG tube) to stay hydrated and gain weight; typically between 120 and 160 ml/kg/day Must pass carseat test without A/B/D episodes Typically between 37 -44 weeks CGA

Note This is how an uncomplicated, ideal NICU course may go, and there are plenty of infants who have uncomplicated, ideal courses! However, there are many things that can go wrong, or be more severe, that make things more complicated – you will learn about all of these things along the way! Keep this system by system thought process in your head with each premature admission, and you will be able to write the admission orders and understand the care super well! Never be afraid to ask for help!
- Slides: 30