NHS longterm plan priorities for finance Richard Murray










- Slides: 14

NHS long-term plan: priorities for finance Richard Murray Chief Executive The King’s Fund 12 September 2019 © The King's Fund 2019

NHS long-term plan: priorities for finance Three issues: § Is it enough? § Financial commitments within the plan § The future financial architecture for the NHS

Priorities for finance: is it enough? What we don’t know What we do know £ 20. 5 bn/3. 4% for NHS revenue budgets to 2023/24 Flat(ish) real for the public health grant c. £ 1 bn extra for social care next year 3. 4% real for HEE next year Funding beyond next year for: • Capital • Workforce (HEE) • Public health • Social care

Key uncertainties: No 1 of 3: demand “In the modelling underpinning this long-term plan we have therefore not locked-in an assumption that its increased investment in community and primary care will necessarily reduce the need for hospital beds. Instead, taking a prudent approach, we have provided for hospital funding as if trends over the past three years continue. ” NHS long-term plan

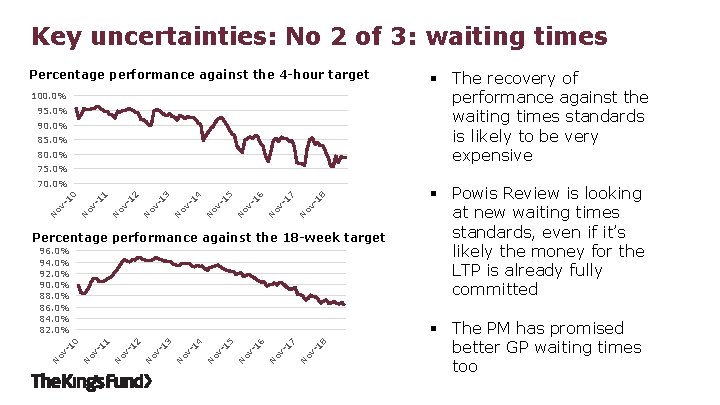
Key uncertainties: No 2 of 3: waiting times Percentage performance against the 4 -hour target 100. 0% 95. 0% 90. 0% 85. 0% 80. 0% 75. 0% 8 7 -1 ov ov N N N ov ov -1 -1 6 5 -1 4 N ov N N ov -1 3 -1 2 -1 ov N N N ov ov -1 -1 1 0 70. 0% Percentage performance against the 18 -week target 8 7 -1 ov N N ov -1 6 N ov -1 5 N ov -1 4 N ov -1 3 N ov -1 2 N ov -1 1 -1 ov N N ov -1 0 96. 0% 94. 0% 92. 0% 90. 0% 88. 0% 86. 0% 84. 0% 82. 0% § The recovery of performance against the waiting times standards is likely to be very expensive § Powis Review is looking at new waiting times standards, even if it’s likely the money for the LTP is already fully committed § The PM has promised better GP waiting times too

Key uncertainties: No 3 of 3: unplanned costs Ø Workforce problems are pervasive: the long-term plan needs these to be overcome but this must either be done without great expense, or come from HM Treasury Ø Some input prices – e. g. generic drugs – have proved more unstable in recent years Ø A hard Brexit presents a series of potentially expensive side effects for health and care

Financial commitments within the plan Most of the LTP’s (many) commitments relate to outcomes or processes e. g. number of people treated. There are important exceptions. Commitment Content Primary medical and community health services Ring-fenced local fund of at least £ 4. 5 bn in real terms by 2023/24 Mental health services Ring-fenced local fund of at least £ 2. 3 bn in real terms by 2023/24 CCG allocations Includes better needs assessment for community and mental health; no CCG +5% below target

Financial commitments within the plan And some important, but smaller ones Ø Rough sleepers Ø Children’s hospices Ø To complete radiotherapy machine upgrades Ø Programmes to reduce violence, bullying and harassment and to spread body cameras Ø Workforce Race Equality Standard funding

Financial architecture of 2012 Providers NHS Commissioners NHS England CCGs Contract via the national fee-forservice payment by results NHS Foundation Trusts NHS Trusts Non-NHS providers (including contractor professions) NHS providers are financially independent; must finance capital out of retained earnings or market-mimicking loans; with a failure regime to exit them from the market if they become insolvent; Monitor as the market regulator

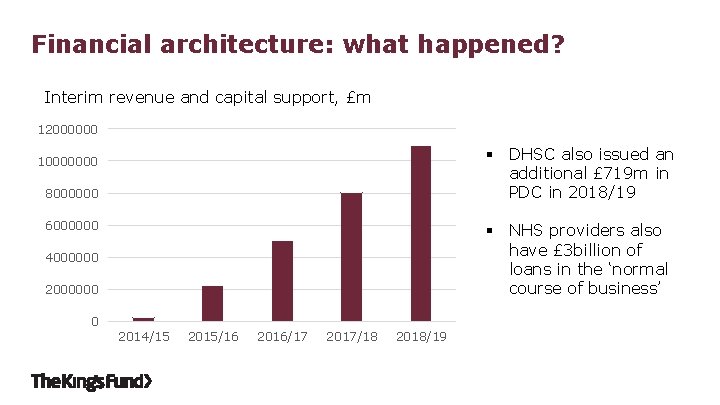
Financial architecture: what happened? Interim revenue and capital support, £m 12000000 § DHSC also issued an additional £ 719 m in PDC in 2018/19 10000000 8000000 6000000 § NHS providers also have £ 3 billion of loans in the ‘normal course of business’ 4000000 2000000 0 2014/15 2015/16 2016/17 2017/18 2018/19

Financial architecture: what happened? Ø The Failure regime was applied to South London NHS Trust and to Mid-Staffs NHS Foundation Trust, but never again Ø The introduction of large-scale `Sustainability Funds’ controlled by the centre, bypassing local contracting Ø Control Totals introduced Ø Monitor joins with NHS-TDA and then joins with NHS England Ø DHSC runs out of CDEL (capital), highlighting the conflict between Parliamentary controls and Foundation Trust freedoms Ø Deviations from tariff/PBR

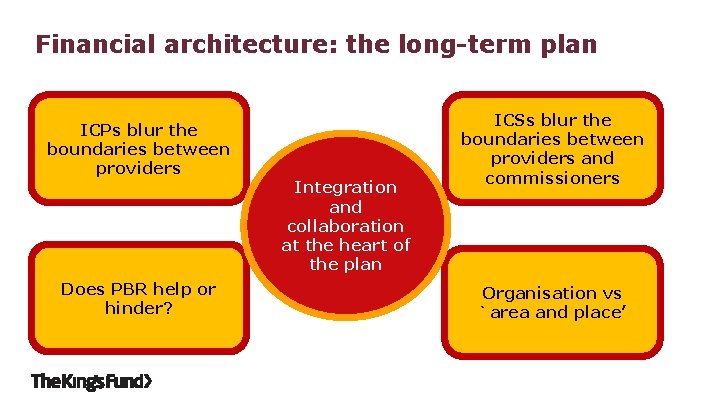
Financial architecture: the long-term plan ICPs blur the boundaries between providers Does PBR help or hinder? Integration and collaboration at the heart of the plan ICSs blur the boundaries between providers and commissioners Organisation vs `area and place’

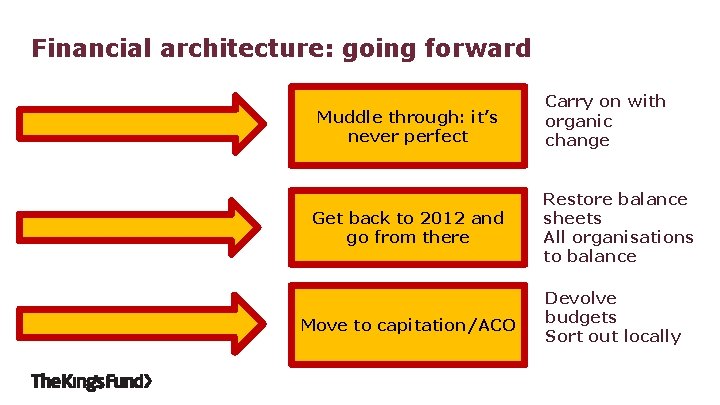
Financial architecture: going forward Muddle through: it’s never perfect Get back to 2012 and go from there Move to capitation/ACO Carry on with organic change Restore balance sheets All organisations to balance Devolve budgets Sort out locally

NHS long-term plan: priorities for finance Ø Manage today and the commitments in the plan Ø But begin to think through the future or risk short-term decisions that take us the wrong way Ø For what it’s worth: § Can we really work without organisations? § Can we really work without a real understanding of benchmark costs and budget? § But avoid the rigidity of PBR and make allocation decisions at area level