NHS Breast Cancer Screening Programme Carly Taylor Breast

NHS Breast Cancer Screening Programme. Carly Taylor Breast Screening Navigator Breast Cancer Screening Unit. Email: carly. taylor@mbht. nhs. uk Royal Lancaster Infirmary.

Breast Screening Service. The North Lancashire and South Cumbria Breast Screening Service is part of the National Breast Screening Programme and provides a free breast screening service for eligible well women, serving residents in North Lancashire and South Cumbria. The NHS England Breast Screening Programme is a rolling one which calls women from GP practices in turn every 3 years from the age of 50 -70. Not every woman will receive an invite as soon as she is 50, but each woman should receive her first invite before the age of 53. Some women outside this age group (47 - 49 and 71 - 73) are also screened as part of an age extension trial. Extended appointments and pre appointment ‘tours’ of the screening unit are available for women with learning disabilities. Women with breast implants are able to have a mammogram. Mammographers are always female.
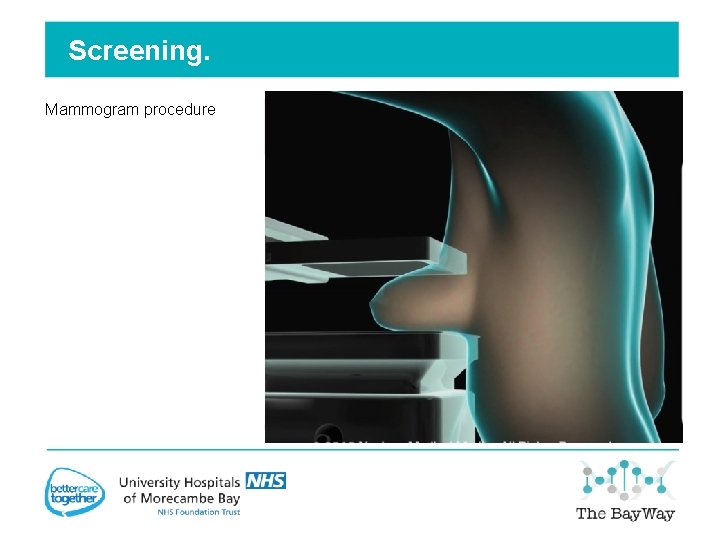
Screening. Mammogram procedure Mammogram Images.
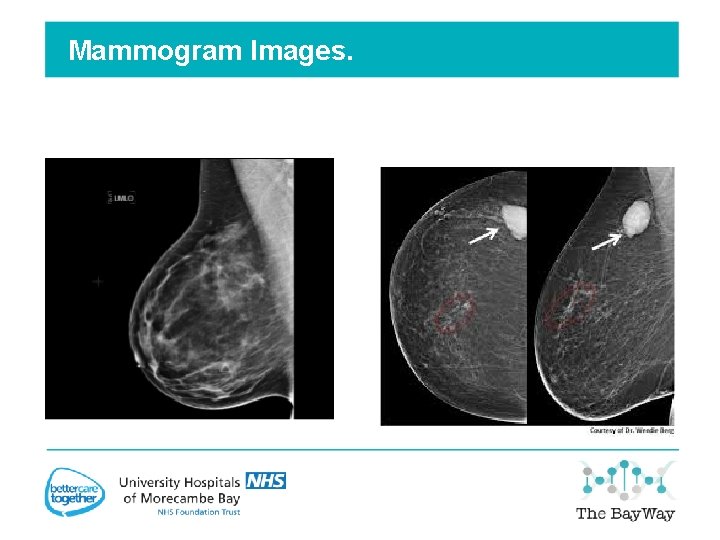
Mammogram Images.

Following Screening. Most women will have a normal reading and be invited again in 3 years time. Some women – about 1 in 23 are called back for further assessment. Most women will not have breast cancer. Further tests may include: • Clinical examination of the breasts and lymph nodes. • Another mammogram. • An ultrasound scan of the breast. • Breast tissue biopsy.
Breast Cancer Prevalence in the UK. • Breast cancer is the most commonly diagnosed cancer in women in the UK. • There were 54, 900 cases of breast cancer in the UK in 2015, that works out at approximately 150 cases diagnosed every day. • One in eight women in the UK will develop breast cancer at some point in their lifetime. Diagnosis Statistics for Women in the UK
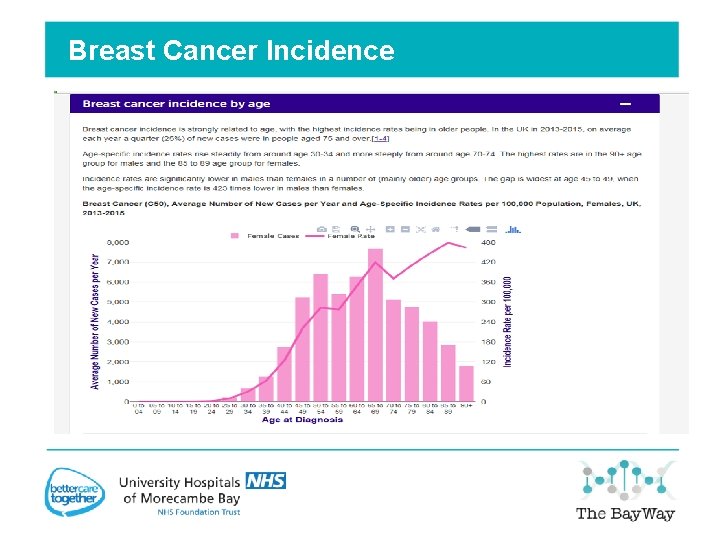
Breast Cancer Incidence

Risk Factors. • Over weight or obese. • Lifestyle factors – drinking alcohol, smoking, lack of exercise, high fat diet. • Age – most breast cancer is diagnosed at 50+. • Early menstruation. • Late menopause. • Late or no pregnancies. • Prolonged use of HRT. • Family history.

Symptomatic. Most breast lumps (90%) aren't cancerous, but it's always best to have them checked by your doctor. A GP must be seen if any of the following symptoms are experienced: • A new lump or area of thickened tissue in either breast. • Changes in the size or shape in one or both breasts. • Blood-stained discharge from either of your nipples • A lump or swelling in either of your armpits • Dimpling on the skin of your breasts • A rash on or around your nipple • A change in the appearance of your nipple, such as becoming sunken into your breast
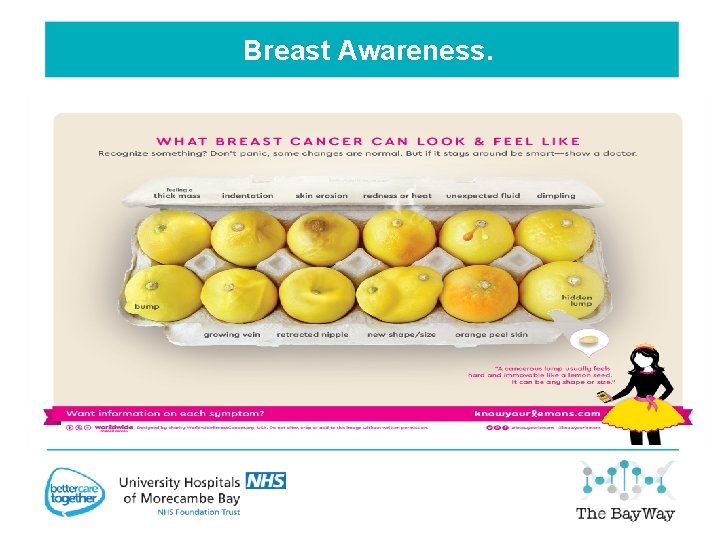
Breast Awareness.

Ways we can reduce our risk. Be aware of your alcohol consumption. https: //www. drinkaware. co. uk/tools/app/ Be more physically active. Make healthier food choices.

Barriers to Breast Screening. • Family commitments. • Work Commitments. • Location. • Illness. • Lack of awareness. • Previous bad experience. • Invasive procedure.
Uptake rates for screening. Uptake Levels During the three year period from 2013 -2016 out of the 125’ 299 ladies invited for screening 32, 533 failed to attend their breast screening appointment. 26% of women do not attend. Uptake levels over the whole geographical area are slightly higher than the national average, however, it is within the Blackpool and some Preston areas of Lancashire where uptake rates are at the lowest levels. In the screening round 2012 – 2015, average uptake rates achieved in Blackpool was 62% and in Preston, also 62%.

Blackpool residents focus group findings. • Discussions during some focus groups revealed a lack of awareness around both the breast cancer screening programme and breast cancer risk. • Some women had little or no knowledge of the programme regarding eligible age, the age extension trial and how often you should be screened. • Many women amongst these groups believed that family history was the most significant risk factor – believing themselves to be low risk without family history. • Little or no awareness of lifestyle factors as breast cancer risk. • Lack of knowledge regarding symptoms and breast awareness.

GP Endorsement. How you may be able to improve uptake in your practice. • • • How many eligible patients do you have? What % of your patients have not responded to Breast Screening invitation? What can you tell the patient about Breast Screening? Who in your practice team can manage these activities? Can your practice send letters? Make telephone calls? Advise patients as they come into contact with practice. Text reminder service – Mjog. Display screening information. * Information found at NCIN – GP Practice Profile: https: //fingertips. phe. org. uk/profile/cancerservices This information can be used to contact patients, encourage them and offer them further advice/signposting. Consider checking how your practice’s uptake and coverage compares with local and national averages.

Questions?
- Slides: 16