NEWER MODES OF VENTILATION DR PRATHEEBA DURAIRAJ M

NEWER MODES OF VENTILATION DR. PRATHEEBA DURAIRAJ, M. D, D. A 5. 12. 2007

o Discovery of the potential for mechanical ventilation to produce ventilatorassociated lung injury has resulted in the development of new lung protective strategies

AIM o To enhance respiratory muscle rest o Prevent deconditioning / atrophy of muscles o Improve gas exchange o Prevent lung damage o Improve patient synchrony o Help in weaning process

Volume Ventilation o o o Stable, consistent tidal volume delivery and minute ventilation, which is independent of patient’s lung mechanics BUT Pressures variable and difficult to control Resultant high peak pressure Slow rise to peak pressure, distribution of ventilation may not be optimized Set flow rate may not match patient’s demand Increased muscle workload from flow asynchrony, may compromise patient comfort gas exchange cardiac function
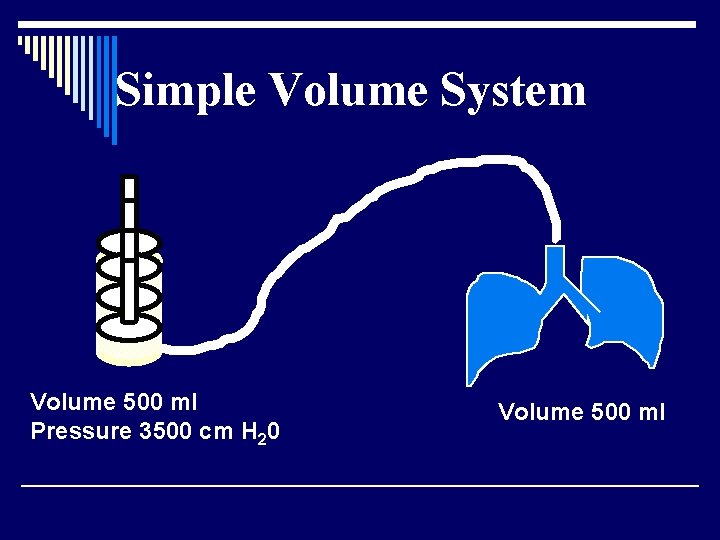
Simple Volume System Volume 500 ml Pressure 3500 cm H 20 Volume 500 ml

Simple Volume System Pop! Volume 2000 ml Pressure 3500 cm H 20
Pressure Control Ventilation Benefits �� o Variable flow capability for patient demand o �� Reduced patient inspiratory muscle workload o �� Lower peak inspiratory pressures o �� Adjustable inspiratory time o �� Rapid filling of the alveoli o �� Improved gas distribution, V/Q matching, and oxygenation Disadvantages o �� Delivered tidal volume is variable and depends upon the patient’s lung mechanics including changes in airway resistance and lung compliance o �� May have adverse effects on volume delivery
NEWER MODES VOLUME PRESSURE

o Clinicians Want the Best of All Possible Worlds Advantages of both pressure and volume ventilation o ���� “You can’t always get what you want, ” (Rolling Stones), so…get what you need. o ���� What’s new?
![Basic principles o Trigger –machine & patient [flow / presssure ] o Flow triggerig Basic principles o Trigger –machine & patient [flow / presssure ] o Flow triggerig](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-10.jpg)
Basic principles o Trigger –machine & patient [flow / presssure ] o Flow triggerig – less work –prefered o Too sensitive – auto triggering o Limit variable [ pressure / volume ] o Cycle variable –volume , flow , pressure , time

TYPES INVASIVE APRV BIPAP Self adaptive modes Proportional assist ventilation Independent ventilation High frequency ventilation Extracorporeal membrane oxygenation Liquid ventilation NONINVASIVE o o o o

NON INVASIVE VENTILATION o Negative pressure ventilators (Tank and Cuirass ventilators) were the only noninvasive methods of assisting ventilation for many years mainly for ventilating large number of victims of Polio during their acute illness. o use of NIMV has increased in last decade in various conditions to avoid complications of intubation.

Types o Positive Pressure Ventilation o Negative Pressure Ventilation

Mechanism of Action o Improvement in pulmonary mechanics and oxygenation In COPD, oxygen therapy often worsens hypercarbia and respiratory acidosis. Augments alveolar ventilation and oxygenation without raising Pa. CO 2 o Partial unloading of respiratory muscles Reduces trans-diaphragmatic pressure, pressure time index of respiratory muscles and diaphragmatic electromyographic activity Alteration in breathing pattern with an increase in tidal volume, decrease in respiratory rate and increase in minute ventilation. o NIMV also overcomes the effect of intrinsic PEEP

Advantages of NIMV o Preservation of airway defense mechanism o Early ventilatory support: an option o Intermittent ventilation possible o Patient can eat, drink and communicate o Ease of application and removal o Patient can cooperate with physiotherapy

Contd… o Improved patient comfort o Reduced need for sedation o Avoidance of complications of endotracheal intubation: upper airway trauma, sinusitis, otitis, nosocomial pneumonia o Ventilation outside hospital possible o Correction of hypoxaemia without worsening hypercarbia o Ease to teach paramedics and nurses

Disadvantages o Mask uncomfortable/claustrophobic o Time consuming for medical and nursing staff o Facial pressure sores o Airway not protected o No direct access to bronchial tree for suction if secretions are excessive o Less effective?

Indications of NIMV Hypercapnic acute respiratory failure o Acute exacerbation of COPD o Post extubation o Weaning difficulties o Post surgical respiratory failure o Thoracic wall deformities o Cystic fibrosis o Status asthmaticus o Obesity hypoventilation Syndrome Hypoxaemic acute respiratory failure o Cardiogenic pulmonary oedema o Community acquired pneumonia o Post traumatic respiratory failure o ARDS o Weaning difficulties o Chronic Respiratory Failure o Immunocompromised Patients

Contraindications o o o o o Respiratory arrest Unstable cardiorespiratory status Uncooperative patients -confused , agitated Unable to protect airway- impaired swallowing and cough Facial Oesophageal or gastric surgery Craniofacial trauma/burn Anatomic lesions of upper airway Vomiting Impaired conciousness

Relative Contraindications o Extreme anxiety o Massive obesity o Copious secretions o Need for continuous or nearly continuous ventilatory assistance

Prerequisites for successful Non. Invasive support o Patient is able to cooperate o Patient can control airway and secretions o Adequate cough reflex o Patient is able to co-ordinate breathing with ventilator o Patient can breathe unaided for several minutes o Haemodynamically stable o Blood p. H>7. 1 and Pa. CO 2 <92 mm. Hg o Improvement in gas exchange, heart rate and respiratory rate within first two hours o Normal functioning gastrointestinal tract

Interface o Interfaces are devices that connect ventilator tubing to o o o the face allowing the entry of pressurized gas to the upper airway. Nasal and oronasal masks and mouth pieces, CPAP helmet are currently available interfaces. Masks - made from a non irritant material such as silicon rubber. - minimal dead space and a soft inflatable cuff to provide a seal with the skin. Nasal mask - better tolerated but less effective – leak Face masks are more useful in acute respiratory failure Nasal masks, Mouth piece , CPAP helmet are used most often in chronic respiratory failure

Ventilators - conventional o o o Advantages Fi. O 2 can be set Alarm & monitoring back up Back up ventilation Separate insp & exp limbs – prevent rebreathing Inspiratory pressure > 20 cm H 2 O can be set Disadvantages o Expensive o Less flexible &portable o Leak compensation not present – requires tight interface

NPPV Ventilators o Advantages o cheaper o flexible &portable o Leak compensation present – does not requires tight interface o Inspiratory pressure of 20 cm H 2 Ois maximum available Disadvantages o Fi. O 2 cannot be set o Due to leak – high oxygen flows o Single limb – rebreathing

Modes of Ventilation o CPAP o It is not a true ventilator mode as it does not actively o o assist inspiration. CPAP by nasal mask provides pneumatic splint which holds the upper airway open in patients with nocturnal hypoxaemia due to episodes of obstructive sleep apnoea. CPAP increases FRC and opens collapsed alveoli. CPAP reduces left ventricular transmural pressure therefore increases cardiac output. – effective for treatment of pulmonary oedema. Pressures are usually limited to 5 -12 cm of H 2 O - higher pressure tends to result in gastric distension
![BILEVEL POSITIVE AIRWAY PRESSURE [ BI LEVEL PAP] o Unique flow triggering &leak compensation BILEVEL POSITIVE AIRWAY PRESSURE [ BI LEVEL PAP] o Unique flow triggering &leak compensation](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-26.jpg)
BILEVEL POSITIVE AIRWAY PRESSURE [ BI LEVEL PAP] o Unique flow triggering &leak compensation o Spontaneous mode –cycle between IPAP (Up to 30 cm H 2 O)& EPAP (Up to 15 cm of H 2 O)- PATIENT TRIGGERED PRESSURE SUPPORTED o IPAP = PEEP +PS / EPAP = PEEP in PCV SPECIAL MACHINES o Have blower unit to compensate air leaks upto 180 L /mt o Pressure limited back up o Adjustable sensitivities , maximum inspiratory time , adjustable Fi. O 2 -available
![BI LEVEL PAP[contd…] o INDICATIONS o CONTRA INDICATIONS o Worsening o Unstable hypoventilation/ hypoxemia BI LEVEL PAP[contd…] o INDICATIONS o CONTRA INDICATIONS o Worsening o Unstable hypoventilation/ hypoxemia](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-27.jpg)
BI LEVEL PAP[contd…] o INDICATIONS o CONTRA INDICATIONS o Worsening o Unstable hypoventilation/ hypoxemia o Chronic ventilatory muscle dysfunction o Post intubation difficulty o Upper airway obstruction –laryngeal oedema, strictures o o Haemodynamics Vomiting Neurologically abnormal Pneumothorax Deteriorating respiratory parameters

PSV o Non-invasive PSV can be administered with standard critical care ventilator or bilevel portable devices. -patient triggered, pressure limited , flow cycled ventilation o PSV mode has unique ability to vary inspiratory time breath by breath, permitting close matching with the patient's spontaneous breathing pattern Advantages (a) Patient-ventilator synchrony (b) Improved patient comfort (c) Reduced diaphragmatic work

Volume limited ventilation o ventilators are usually set in assist-control mode with high tidal volume (10 -15 ml/kg) to compensate for air leak. o suitable in obesity or chest wall deformity who need high inflation pressure neuromuscular diseases who need high tidal volume for ventilation Proportional assist ventilation (PAV) o This is a newer mode of ventilation. o In this mode ventilator has capacity of responding rapidly to the patients' ventilatory efforts. o By adjusting the gain on the flow and volume signals, one can select the proportion of breathing work that is to be assisted.

Goals of NIMV Short Term o Relieve symptoms o Reduce work of breathing o Improve or stabilize gas exchange o Good patient-ventilator synchrony o Optimize patient comfort o Avoid intubation Long Term o Improve sleep duration and quality o Maximize quality of life o Enhance functional status o Prolong survival

Protocol for Non Invasive Ventilation o o o o Explain to the patient what you are doing and what to expect Setup the ventilator by the bed side Keep the head of the patient's bed at >45 degree angle Choose the correct interface Turn on the ventilator and dial in the settings Attach O 2 at 2 litres per minute Hold the mask gently over the patient's face until the patient becomes comfortable with it. Strap the face mask on using the rubber head strap and minimize air leak without discomfort. Connect humidification system.

o Monitor- respiratory rate, heart rate, level of dyspnoea, O 2 o o o saturation, blood pressure, minute ventilation, exhaled tidal volume, abdominal distension and ABG Initial ventilator setting should be very low ie. IPAP of 6 cm H 2 O, and EPAP of 2 cm. H 2 O Increase EPAP by 1 -2 cm increments till the patient triggers the ventilator in all his inspiratory efforts. Increase IPAP in small increments, keeping it 4 cm. H 2 O above EPAP, to a maximum pressure, which the patient can tolerate without discomfort and major leaks. Titrate pressure to achieve a respiratory rate of <25 breaths/min and Vt >7 ml/kg Increase Fi. O 2 to improve O 2 saturation to 90%
![Complications and Side effects AIR LEAK [80 -100%] MASK RELATED o Discomfort o Facial Complications and Side effects AIR LEAK [80 -100%] MASK RELATED o Discomfort o Facial](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-33.jpg)
Complications and Side effects AIR LEAK [80 -100%] MASK RELATED o Discomfort o Facial skin erythema o Claustrophobia o Skin necrosis- particularly over bridge of nose o Retention of secretions o Failure to ventilate o Upper airway obstruction o o o FLOW RELATED Nasal congestion Sinus /ear pain Nasal dryness Eye irritation Gastric distension MAJOR COMPLICATIONS o Aspiration pneumonia - < 5% o Hypotension o Pneumothorax

CRITERIA FOR FAILURE OF NPPV o o o MAJOR Respiratory arrest Loss of consciousness Psychomotor agitation Haemodynamic instability Heart rate <50 b/m MINOR o Respiratory rate > 35 /mt o p. H <7. 30 o Pao 2 <45 mm. Hg Intubate when one major / two minor criteria

INVASIVE VENTILATION
![Pressure Regulated Volume Control [PVRC] o Available on the Servo 300 o Assist control Pressure Regulated Volume Control [PVRC] o Available on the Servo 300 o Assist control](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-36.jpg)
Pressure Regulated Volume Control [PVRC] o Available on the Servo 300 o Assist control mode o Variable, decelerating flow pattern o Breaths are –patient TRIGGER, time cycled, assist/control Establishes a “learning period” to determine patient’s compliance, which establishes regulation of pressure/volume o Aim – is to deliver preset TV/ MV / frequency with constant pressure [minimum] during the entire inspiration

Pressure Regulated Volume Control (PRVC) o �� Inspiratory pressure is regulated based on the Pressure/Volume calculation of the previous breath, compared to a target tidal volume o The ventilator continuously adapts the inspiratory pressure in responses to changing compliance and resistance to maintain the target tidal volume o Results in breath-to-breath variation of inspiratory pressure Limitations: o Only an A/C mode and requires a change to Volume Support for weaning o Only guarantees volume distally and not at patient airway
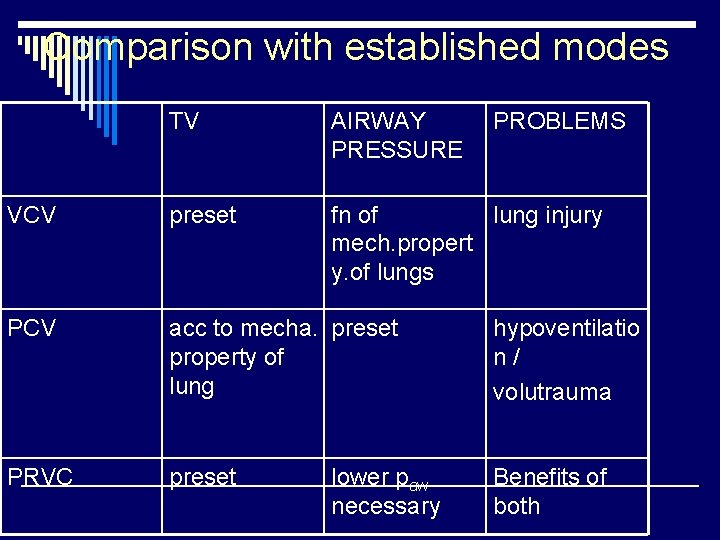
Comparison with established modes TV AIRWAY PRESSURE VCV preset fn of lung injury mech. propert y. of lungs PCV acc to mecha. preset property of lung hypoventilatio n / volutrauma PRVC preset Benefits of both lower paw necessary PROBLEMS

Applications of PRVC o ALI o Asthma o COPD o Postop patient o Pediatric patient o Pts with no breathing capacity- need initial high flow rates o In whom VT has to be controlled –surfactant therapy

Benefits o Can be used in all populations o Low peak inspiratory pressure o Inspiratory pressure adapts to mechanical properties of lung o ⇩ CVS interference o Improved gas distribution o Less need for sedation o Greater patient comfort
![BIPHASIC POSITIVE AIRWAY PRESSURE [BIPAP] o Pressure controlled ventilation allowing o o o o BIPHASIC POSITIVE AIRWAY PRESSURE [BIPAP] o Pressure controlled ventilation allowing o o o o](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-41.jpg)
BIPHASIC POSITIVE AIRWAY PRESSURE [BIPAP] o Pressure controlled ventilation allowing o o o o spontaneous ventilation Shifts between two levels of PAP P low – pressure akin to PEEP In PCV [lowest airway pressure] P high –pressure above PEEP [P plat] T high &T low Subdivisions – CMV to CPAP Single mode covers entire spectrum Finer adjustment done after connecting the patient to ventilator in VCV

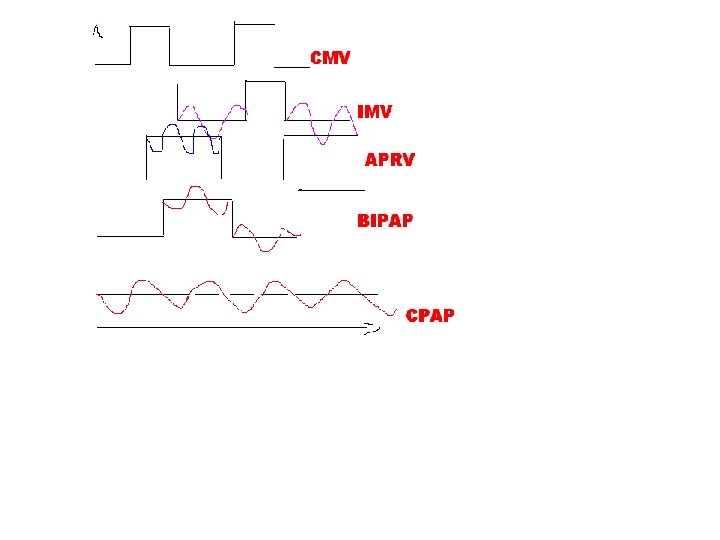
BIPAP -SUBDIVISIONS o CMV BIPAP-no Spontaneous breathing o IMV –BIPAP –spontaneous breathing at lower level o APRV – BIPAP - spontaneous breathing at higher level o Genuine BIPAP - spontaneous breathing at both levels o CPAP - spontaneous breathing at single CPAP level
p a w t

Setting up BIPAP o Adjusted with ABG values o High /low Pa. CO 2 /Normal Pa. O 2 o ⇧/⇩ VT/ RR o Alteration of P high /P low – ⇧/⇩VT o Alteration of T high/T low - ⇧/⇩ RR o Decreased Pa. O 2 ⇧mean airway pressure without altering VT/RR equidirectional alteration of P high /P low

ADVANTAGES OF BIPAP o Less sedation o Reduced atelectasis o Ideal mode in pts with inadequate spontaneous effort o In face of deteriorating gas exchange we can increase the invasiveness of ventilation without having to change mode

Airway Pressure Release Ventilation (APRV) o Outlined in 1987 o Continuous positive airway pressure with regular, brief, intermittent releases in airway pressure. o The release phase results in alveolar ventilation and removal of carbon dioxide. o APRV, unlike conventional CPAP, facilitates both oxygenation and CO 2 clearance o It is the high CPAP level [referred to as PEEP high or P high] which enhances oxygenation, o Timed releases to the low CPAP level [referred to as PEEP low or P low] aid in CO 2 clearance.

APRV –CONTD… o Whereas more conventional modes of ventilation begin the ventilatory cycle at a baseline pressure and elevate airway pressure to accomplish tidal ventilation o APRV commences at an elevated baseline pressure and follows with a measured pressure release. o During APRV, spontaneous breathing may occur at either the plateau pressure or deflation pressure levels. o Available on Dräger and Puritan Bennett ventilators

APRV –CONTD… o Elevated baseline airway pressure during APRV may produce near complete recruitment o Minimizes low volume lung injury from cyclic recruitment o APRV is less likely to produce over-inflation or highvolume lung injury, as airway pressures are lowered (released) to accomplish ventilation. o Needs a High flow CPAP circuit with release valve

Advantages of APRV Ø Lower peak airway pressures Lower minute ventilation Ø Decreased adverse effects upon circulatory function Ø Spontaneous ventilation the entire ventilatory cycle Ø Decreased need for sedation Ø Near elimination of neuromuscular blockade Recruitment of alveoli Ø Ø

Indications for APRV o ALI or low-compliance lung disease. o patients with airway disease. CONTRAINDICATIONS o Patients with Increased airway resistance

Settings of APRV o When changing a patient’s mode of ventilation to APRV, the initial o o o settings are partly deduced from values of conventional ventilation. The clinician converts the plateau pressure of the conventional mode to P High and seeks an expired minute ventilation of 2 to 3 L/minute, less than when on conventional ventilation. . P Low is often initially set at 0 cm of water pressure. A P Low of zero produces minimal expiratory resistance, thus accelerating expiratory flow rates, facilitating rapid pressure drops. T High is set at a minimum of 4. 0 seconds. A T High of less than 4. 0 seconds begins to impact mean airway pressure negatively. T Low is set between 0. 5 and 1. 0 seconds (often at 0. 8 seconds). With these settings (P High = 35 cm of water pressure, P Low = 0 cm of water pressure, T High = 4. 0 seconds, T Low = 0. 8 seconds), the mean airway pressure will equal 29. 2 cm of water pressure.

Pressure support ventilation o Weaning mode o Patient trigger , flow cycled o Each inspiratory effort is augmented by specific amount of positive pressure at airway o PS Terminated when insp. Flow falls below a minimum trigger volume o Level of PS – Max insp pressure / 3 o Peak airway pressure - plateau

` o ADVANTAGES o Less WOB low pressure high volume work similar to spontaneous [SIMV –high pr/low volume work] o Easy acceptability o Physiological conditioning of respiratory muscles o WEANING o Pressure level is decreased gradually o Extubated when adequate gas exchange is achieved with PS of 5 cm H 2 O

Volume Assured Pressure Support (VAPS) o Patient triggering o Allows spontaneous breathing without support o Variable flow, volume ventilation o Decelerating, non-limited, variable flow rate o Guaranteed tidal volume delivery �� o �� If targeted volume is not delivered at this pressure, breath continues to guarantee volume - �� PIP and inspiratory time increase o �� Guarantees volume on current breath (no previous breath averaging) o �� Combines the advantages of pressure and volume ventilation breath to breath.

Characteristics of VAPS o �� The ventilator continuously measures the flow and pressure and calculates delivered volume o Depending on the actual settings, breath may be flow, volume, or time cycled o �� If the target tidal volume has been delivered, inspiration is terminated (flow cycled breath) o �� If preset tidal volume has not been achieved, the set flow will persist until the desired volume has been reached (volume cycled breath) o �� Safety limits include high pressure and maximum inspiratory time�� o Used in the Management of acute and recovering lung disease

Benefits of VAPS o �� Lower peak airway pressure o �� Reduced patient work of breathing o �� Improved gas distribution o �� Less need for sedation o �� Improved patient comfort

Applications of VAPS o �� A patient who requires a substantial level of ventilatory support and has a vigorous ventilatory drive to improve gas distribution and synchrony o �� A patient being weaned from the ventilator and having an unstable ventilatory drive to supply a back -up tidal volume as a “safety net” in case the patient’s effort or/and lung mechanics change o Limitations: o �� Will only increase pressure, not lower pressure with changing mechanics o �� Increases inspiratory time to assure volume

Volume support ventilation o Support mode o Has PVRC as back up mode o Allows spontaneous if preset MV is achieved o If fails, deliver preset TV /MV in lowest possible pressure o Set TV /RR close to spontaneous o Set trigger , insp. time, upper pressure limit, lower & upper MV alarm

Applications of VSV o Patients with limited breathing capacity o Ready to be weaned o Post op patient with intact resp. drive o Pts recovering from ALI o Pts with ventilator dependence o Pts requiring breath to breath variations in inspiratory pressure support

BENEFITS OF VSV o Low PIP o Inspiratory pressure adapts to mechanical property of lung o Backup with PRVC o CVS interference o Greater comfort o Less sedation o Improved gas distribution

Dual modes o Continously regulate applied pressure / flow to achieve o o o o o targeted MV/TV based on feed back loop Provide full /partial ventilatory support Modify their operation within the confines of an individual breath Dual control within breath / dual control breath to breath Types Volume –assured pressure support Pressure augumentation Volume support Pressure regulated volume control Variable pressure /volume control
![Proportional assist ventilation [PAV] o PAV instructs machine to act as auxillary muscle – Proportional assist ventilation [PAV] o PAV instructs machine to act as auxillary muscle –](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-62.jpg)
Proportional assist ventilation [PAV] o PAV instructs machine to act as auxillary muscle – vigor controlled by patient power adjusted by us to off set resistive & elastic requirements o Pressure assistance - proportional to variable combination of inspired volume and inspiratory flow rate[ by patient] o Machine amplify patients efforts o Dis advantage: o Requires a back up in case of apnoea

Independent lung ventilation o In protection of secretions of one lung o Asymmetric disease – contusion , aspiration , Atlectasis, o o o pulmonary embolism Thoracic procedures ILV – synchronously [rate linked ventilators , single ventilator with different circuits Asynchronously [ 2 ventilators] Differential PEEP with higher pressure to injured lung – key strategy Equal tidal volume to both lungs Low respiratory rate to injured lung –prevent lung injury

Liquid ventilation -PAGE o Partial [ both gas & PFC –conventional ventilator can be o o o o used] Total – only PFC [ needs special equipment] Ventilator used to perform the WOB because of high viscous resistance PERFLUROOCTYL BROMIDE Inert , surface tension < water CO 2 - Four times soluble, O 2 – twenty times soluble Non absorbable & poor solvent for surfactant Fill FRC with PFC & bubble oxygenate with ventilator
![Perflurocarbon associated gas exchange [PAGE] o IN RDS In infants o Advantages o Inert Perflurocarbon associated gas exchange [PAGE] o IN RDS In infants o Advantages o Inert](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-65.jpg)
Perflurocarbon associated gas exchange [PAGE] o IN RDS In infants o Advantages o Inert agent o Increased oxygen delivery o Liquid – recruit alveoli & Prevents collapse of alveoli during expiration o Coat alveoli – stop release of free radicals o Reduce surface tension at alveolar lining – Improve dynamic compliance o Used as surfactant & vasodilatory agent
![Inverse ratio ventilation [IRV] o I: E -2: 1 -4: 1 o Normal – Inverse ratio ventilation [IRV] o I: E -2: 1 -4: 1 o Normal –](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-66.jpg)
Inverse ratio ventilation [IRV] o I: E -2: 1 -4: 1 o Normal – 1: 2 o Improves oxygenation by auto PEEP/ increase mean o o o o airway pressure, ⇧ time for gas diffusion ⇩Intrapulmonary shunting Improves V/Q matching –lung recruitment ⇩ Dead space ventilation Adverse effects : barotrauma high rate of trans vascular fluid flow – pulmonary edema Needs sedation PC –IRV – with PCV , peak airway pressures are kept at minimum Indicated in ARDS & Diffuse lung injury

High frequency ventilation o Very low TV < anatomical dead space at rates >normal rate o HFPPV[ 60 -100/mt] o HFJV [100 - 200/mt] o HFO [600 - 3000/ mt] o HFFI-High frequency flow interruption o High frequency percussive ventilation

HFFI-High frequency flow interruption o A device interrupts gas flow or high pressure at frequencies > 15 Hz o emersions HFFI – a conduit with a ball in centre which moves to and fro at 200 cycles / mt interrupting and along gas flow

High frequency percussive ventilation o Recently introduced o High frequency breaths superimposed on conventional breaths o Pneumatically powered time cycled / pressure limited ventilator with inspiratory &expiratory oscillation o Unique is sliding venturi or phasitron mechanism o Phasitron se at 200 - 900 b/mt superimposed on conventional 10 - 15 b/mt

High frequency percussive ventilation o Phasitron mechanism o At the heart of device is sliding venturi with jet orifice o o at its mouth On inspiration a diaphragm connected to venturi fills with gas & pushes it forward blocking expiratory port & jet comes in short percussive pulsations Due to high pressure gradient between mouth & alveolus –large amount of air entrained As gradient drops further into inspiration, air entrainment decreases but jet pulsations continue Cycles to expiration

High frequency oscillation o Most widely used o Inspiration& Expiration active o Sinusoidal flow o TV > DEADSPACE o Electronically controlled proportioning valves – provide positive pressure high frequency breaths in inspiratory limb o A jet venturimeter in expiratory limb creates –ve pressure – expiration is active

High frequency ventilation o Gas exchange 1. bulk gas flow 2. coaxial flow 3. molecular diffusion 4. pendulft o Advantage Lower peak airway pressure ⇧FRC Efficient gas exchange Lower transpulmonary pressure

High frequency ventilation o INDICATION o CONTRAINDICATION o Bronchopleural fistula o COPD o Neonatal RDS o Air leak syndromes o Diffuse lung injury o Pneumothorax o Bronchoscopy

Adaptive support ventilation o Excellent mode for initiating ventilation , support & weaning o Galileo ventilator o Set patient weight , PEEP, pressure limit &volume control [ 100 ml /kg in adults , 200 ml/kg in children ] o Breath to breath assessment is done *PS is constantly adjusted o If inadequate , mandatory breaths delivered o Similar to PSV when spontaneous is present SIMV when inadequate
![Neurologically adjusted ventilatory assist [NAVA] o Developed to overcome limitations of PAV o Electrical Neurologically adjusted ventilatory assist [NAVA] o Developed to overcome limitations of PAV o Electrical](http://slidetodoc.com/presentation_image_h/c717a5dea05847d96587326058a6ff7d/image-75.jpg)
Neurologically adjusted ventilatory assist [NAVA] o Developed to overcome limitations of PAV o Electrical activity of inspiratory muscles – index of inspiratory neural drive o Processed signal –transferred to ventilator to regulate ventilation o Research tool

Biologically variable ventilation (BVV) o Mimics spontaneous breath – breath variability o Ventilator modulate RR/VT –fixed MV o Based on concept that alveolar recruitment achieved by high volumes exceeds decruitment caused by small volumes with net result being improvement in compliance & oxygenation o Under research

Automatic tube compression o New component of ventilatory support under o o o trial Should be Combined with PSV, PAV, BIPAP Available on Drager Evita 4 & Puritan Bennett 840 In intubated patient – pressure difference exists between proximal &distal end of the ETT � PETT = Paw – Ptrach � PETT - Reflects energy required for convective transport of gases

ATC –CONTD… o V &Paw measured at proximal end of ETT and fed into o o ATC controller by staff Based on this, ATC controller selects the tube coefficients characterizing the corresponding pressure –flow relationship of the tube Inspiratory PS in ATC mode equals actual pressure drop across the tube By this closed loop system ventilator automatically compensate for ETT resistance in inspiration & expiration Reduces WOB & increases patients comfort

Advances & Adjuncts in Pediatric Mechanical Ventilation VENTILATION STRATEGIES o open lung concept by HFOV in RDS /CDH o Permissive hyper capnia –low TV At high rates o Prone ventilation –ALI Recruitment of dorsal lung, copious drainage of secretions, extra vascular lung water is reduced

CONTD… VENTILATORY MODES o Adaptive support ventilation o PAV o PRVC o NIV o BIPAP o HFV ADJUNCTS o Inhaled NO o Tracheal gas insufflations o PAGE o surfactant therapy

FUTURE ? ! o Noninvasive ventilation is becoming popular o New therapies for ARDS – HFO o To improve gas exchange – prone ventilation , nitric oxide inhalation o Lung recruitment maneuvers- CPAP 35 -40 cm of H 2 O with PEEP set at 2 cm of H 2 O above Pflex &TV < 6 ml / kg o Ventilatory adjuncts –automatic tube compensation, partial liquid ventilation

- Slides: 82