New ways of models of care Managed care




































- Slides: 43

New ways of models of care? • Managed care • Empowerment and self-care

Cost containment • • • Demographic Epidemiological Quality- adding finance as a new indicator The professions Marketization and consumerism Spiralling cost of universal open access care

Blank and Burau (2010) • Control via • Supply side • Demand side Read Chapter 4

Important Changes in Health Management 22 • Three points: – Chronic disease is the major reason for seeking healthcare. – Treating chronic medical conditions requires a different model of care – The “new” models of care for chronic conditions require a change in both patient and provider roles The Global Burden of Disease, a study sponsored by the World Health Organization, projected that by the year 2020, mortality and disability from disease would shift from predominantly acute illnesses to chronic conditions.

3) Need for Change in Patient and Provider Roles 24, 25 • The “patient/professional” partnership involves collaborative care and selfmanagement education – Patients are expected to do what is needed on a daily basis – Providers act as consultants, resource persons, and offer treatment suggestions Healthcare Providers Provide clinical expertise, experience with the chronic condition, and evidence-based knowledge Patients Know more about themselves, what motivate them, what they are willing to change, and what has helped them feel better

Group Activity Good Chronic Care Requires Self-Management “Growing evidence from around the world suggests that patients with chronic conditions do better when they receive effective treatment within an integrated system of care which includes self-management support and regular follow up. ” 22 Consider the Following Questions: How would you create effective treatment that includes -management support and regular follow-up? What characterizes a prepared practice team? What characterizes an informed activated patient? 26 self

Common Techniques of managing health care: • ‘Queuing and Watchful waiting’ • ‘Gate keeping’ • ‘Case Management’ • ‘Primary Prevention’ • ‘Self Care’ (Robinson and Steiner, 1998, )

Utilisation Management/Managed care Those activities of a health care system which are designed to reduce the overall need for healthcare. (Kongsvedt 1996)

To Case Manage • “The aim of disease management is to take a more proactive approach to managing a disease in order to improve the likelihood of favourably altering it’s natural history. It is a comprehensive and integrated approach. The outcomes include improving quality of care and thus quality of life for the individual and reducing the cost of management of each individual “ • Plocher (1996)

U. S. and U. K. adapted models ‘Kings Fund’, (2004) and Robinson and Steiner, (1998), comments on the evidence of success of these models. • • • United Healthcare- Evercare model Kaiser Permanente approach The Castlefields Poject Pfizer- Informa. Care approach Unique Care


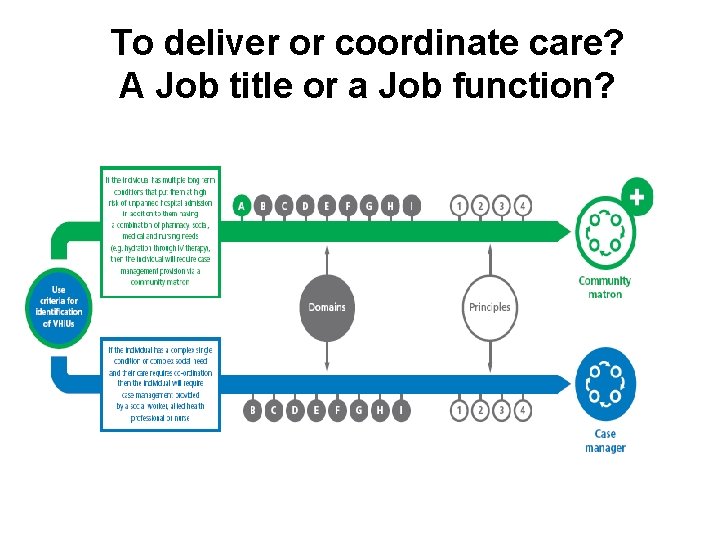
To deliver or coordinate care? A Job title or a Job function?

Three objectives in utilisation of care 1. Patient satisfaction 2. Quality 3. Cost containment Performance assessment and audit necessary to show value for money

Case Finding Who do we provide care for and why?



How do people access Healthcare? • • GP’s surgery – hospital referral Walk in Centres NHS direct Pharmacies The internet/computer terminals Emergency care Managed Care/Case Finding Evidence suggests that emergency care can be prevented by better management of care in the community.

• For a number for years nurses have been asked to be more ‘proactive’ • Why has it not changed to date?

What would happen if: • A person phoned you to ask you to come and assess them so that they do not get ill and can stay well? Managed care = ‘Assertive’

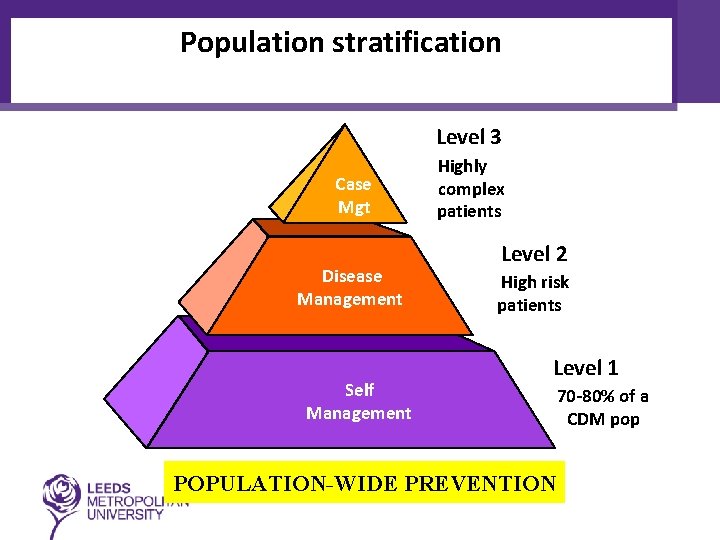
Population stratification Level 3 Case Mgt Disease Management Self Management Highly complex patients Level 2 High risk patients Level 1 POPULATION-WIDE PREVENTION 70 -80% of a CDM pop

Models – Evercare – Castelfields project – Kings fund – NPCDT

Levels of intervention • Primary prevention • Secondary prevention • Tertiary stage (Cochrane D (2001) Managed Care and Modernisation. Open University Press. Buckingham. Philadelphia)) Maintain patient as an active participant at all levels

Primary Prevention Reduce common factors that lead to ill-health. Examples • • Obesity Poor nutrition Lack of exercise Smoking Alcohol Stress Sunbathing Immunisation and vaccination

Examples • Health promotion • Support for those people who make unhealthy lifestyle choices (e. g. smokers) • Outreach workers to work with those who don’t access health care - E. g. the homeless, asylum seekers

Secondary Prevention • Screening and identification of early stages of disease – may not always be obvious e. g. type 2 diabetes, hypertension, osteoporosis • Preventing further disease progression of medium/ long term problems e. g. CVA. , MI, falls/fractures, small vessel disease

Examples • Identification of those at risk • Health screening – planned/opportunistic • Proactive management of diseases at the earliest stage possible • Guidelines/NSF’s/Pathways • Enabling people to self manage their own condition – personalised care plans • Expert Patient Programmes • Case Management, case finding

Tertiary Stage The disease progression is advanced • Manage symptoms • Reduce further progression • Manage exacerbations • Prevent other crises e. g. social problems, carer breakdown, mental health problems • End of life care

Sources of patient data • Quantative and qualitative • IT – The NHS is data-rich but information-poor. The wealth of available data is often not easily accessible by all those who could use it. The NHS needs to develop tools and expertise to use the data to identify high-risk patients

Cont… • Other staff, Benners ‘professional intuition’ • Locality wide information, ONS • Hospital data • Patient surveys or questionnaires.

Kings Fund • Categorise approaches into: – Threshold – Clinical Knowledge – Predictive modelling

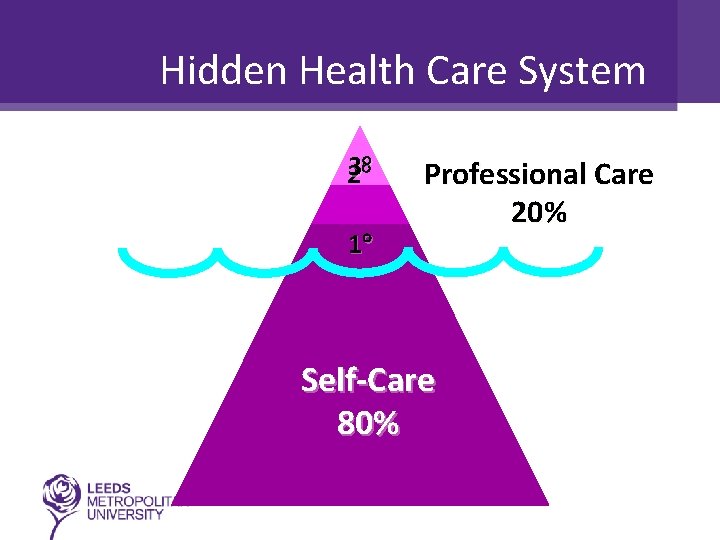
Hidden Health Care System 3 2 1 Professional Care 20% Self-Care 80%

DEFINITION OF SELF CARE ‘Actions individuals and carers take for themselves, their children, their families and others to stay fit and maintain good physical and mental health, meet social and psychological needs, prevent illness or accidents, care for minor ailments and long term conditions, and maintain health and wellbeing after an acute illness or discharge from hospital’ Department of Health (2005) Self Care: Real Choice. HMSO. London.

KEY STATISTICS DESCRIBING ACTIVITY AROUND SELF CARE IN ENGLAND • Over the counter medicines sales total £ 2 billion per year • Two-thirds of internet users have researched on line • Sales of consumer health magazines have grown at around 20% per year the last decade

• Around 1 million people are providing over 50 hours per week unpaid care • It has been estimated that self treatable disorders account for nearly 40% of GP time • In the UK self care comprises of 80% of all care episodes • Should be lots of opportunity for those working in primary care to encourage and support self care Do. H(2006) Our Health Our Care Our Say-A New Direction for Community Services. White Paper

• Empowerment

Empowering Approach? 13 “Empowerment occurs when the practitioner’s goal is to increase the capacity of the client to think critically and make autonomous, informed decisions…it also occurs when clients are actually making autonomous informed decisions” ü Reflect on your – Compliance vs. Adherence vs. Empowerment – – reactions ü Challenge – consider how fully the spirit of empowerment Empowerment is a process and an outcome can be applied in clinical settings No empowerment without respect with various patient populations

Defining Empowerment for Health Empowerment is a process by which people gain mastery over their lives. ” 14 J. Rappaport Empowerment is an educational process designed to help patients develop the knowledge, skills, attitudes, and degree of self-awareness necessary to effectively assume responsibility for their health-related decisions. ” 15 Feste – Anderson

Sharing of Power 16 Compliance “You must do what I tell you. ” An authoritative act designed to reduce patient autonomy and constrain freedom of choice Empowerment “Let’s decide together what is the best care for your conditions. ” An agreement designed to support the promotion of self-management, taking into account the patients’ perspectives on their condition, their goals, expectations, and needs

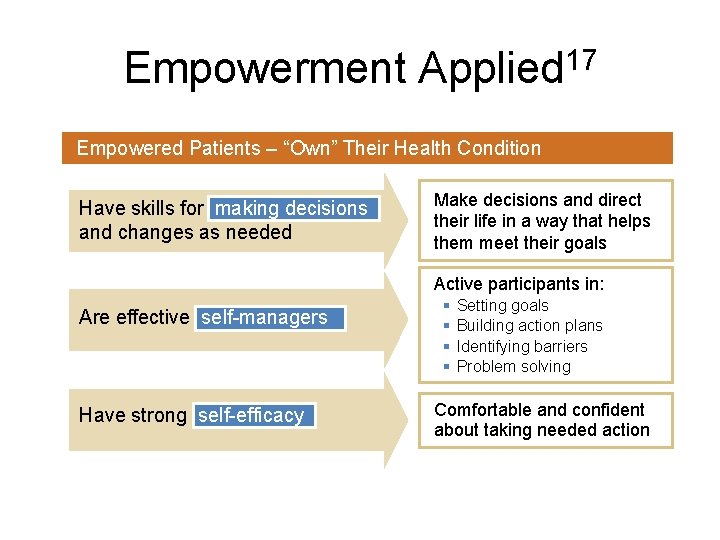
Empowerment Applied 17 Empowered Patients – “Own” Their Health Condition Have skills for making decisions and changes as needed Make decisions and direct their life in a way that helps them meet their goals Active participants in: Are effective self-managers Have strong self-efficacy § § Setting goals Building action plans Identifying barriers Problem solving Comfortable and confident about taking needed action

How Do Patients Become Empowered? 17, 18 Through Self-Management Education Traditional Patient Education Self-Management Education Offers information Teaches problem solving Defines problems Helps patients identify problems, make decisions, take actions Self-management compliments rather than substitutes for traditional patient education A partnership will require both educators and learners to interact with respect as equals

Paolo Freire 19 “There isn’t Dialogue Without Humility” – The content of education based on true dialogue is not intended to convey information or impose ideas – It is to provide an organized structure so individuals can • Identify their own Switching from a “banking” to a “problem–posing” approach to education “Education for liberation”

The Real Goal of Empowerment is Increased Self Efficacy… 21 Patient Empowerment Increased Sense of Self-Efficacy Enhanced Self -Management Skills “Increased self-efficacy allows patients to view disease and symptoms differently, giving more opportunities for effective self-management” 21

Reference List • Dixon J, Lewis R, Rosen R, Finlayson B, Gray D, 2004, “Managing Chronic Disease: What we can learn from the US experience? ”, The Kings Fund. • Hutt R, Rosen R, Mc. Cauley J, 2004, “Case-Managing Long-Term Conditions: What impact does it have in the treatment of older people? ”, The Kings Fund. • Robinson and Steiner, 1998, “Managed Health Care”, Open University Press. • www. patientsvoices. org. uk