New Adult Cardiovascular Life Support Guidelines Robert W

New Adult Cardiovascular Life Support Guidelines Robert W. Neumar, MD, Ph. D, FACEP University of Pennsylvania School of Medicine Immediate Past Chair, ACLS Subcommittee © 2010 American Heart Association. All rights reserved.

Presenter Disclosure Information Robert W. Neumar, MD, Ph. D New Adult Cardiovascular Life Support Guidelines FINANCIAL DISCLOSURE: Research Grants: NIH/NINDS Acorda Therapeutics UNLABELED/UNAPPROVED USES DISCLOSURE: §Devices for initiation and maintenance of post-cardiac arrest therapeutic hypothermia §Cold saline for initiation and maintenance of post-cardiac arrest therapeutic hypothermia post-cardiac arrest

Outline • • • CPR Sequence Airway CPR Quality CPR Pharmacology Therapeutic Hypothermia Post-Cardiac Arrest PCI © 2010 American Heart Association. All rights reserved.

CPR Sequence Change: From A-B-C to C-A-B Initiate chest compressions before ventilations Why? Goal: To reduce delay to CPR, sequence begins with skill that everyone can perform Emphasize primary importance of chest compressions for professional rescuers © 2010 American Heart Association. All rights reserved.
CPR Starts with Compressions Many adults with witnessed arrest have ventricular fibrillation (VF)/pulseless ventricular tachycardia (VT), and require Chest compressions Early defibrillation Chest compressions can be started immediately (no equipment needed) Opening airway, providing ventilation may significantly delay other actions Ventilation delayed by 18 seconds or less © 2010 American Heart Association. All rights reserved.

Healthcare Provider ADULT BLS Sequence • Recognize unresponsive adult with no breathing or no normal breathing (ie, only agonal gasps) • Activate emergency response, retrieve AED (or send someone to do this) • Check for pulse (no more than 10 seconds) • If no pulse, begin sets of 30 chest compressions and 2 breaths • Use AED as soon as available © 2010 American Heart Association. All rights reserved.

Airway © 2010 American Heart Association. All rights reserved.

2010 New Science: Airway Confirmation and Monitoring of Endotracheal Tube Placement • Unrecognized endotracheal tube misplacement remains unacceptably high Wirtz, 2007, 213; Timmermann 2007, 619 • Waveform capnography verifies tracheal tube position in victims of cardiac arrest with 100% sensitivity and 100% specificity. Silvestri, 2005, 497; Grmec 2002, 701; Trikha, 1999, 347; Tong, 2002, 159; Zaleski, 1993, 244; Holland, 1993, 608; Ko, 1993, 91; Linko, 1983, 199; Wayne, 1999, 107; Williamson, 1993, 511

2010 New Science: Airway Confirmation and Monitoring of Endotracheal Tube Placement • Non-waveform capnometry, colorometric Et. CO 2 detectors, and mechanical devices (syringe aspiration and inflating bulb esophageal detectors) do not exceed the accuracy of auscultation and direct visualization for confirming the tracheal position of a tracheal tube in victims of cardiac arrest. Capnometry: Takeda, 2003, 153; Tanigawa, 2001, 375; Tanigawa, 2000, Bozeman, 1996, 5951; Grmec, 2002, 701; Anton 1991, 271; Li, 2001, 223 Colorimetric ETCO 2 detector: Ornato, 1992, 518; Anton, 1991, 271; Mac. Leod, 1991, 267; Varon, 1991, 289; Schaller, 1997, 57; Bhende, 1995, 395; Li, 2001, 223 Mecahnical devices: Tanigawa, 2001, 375; Pelucio, 1997, 563; Takeda, 2003, 153; Tanigawa, 2001, 375; Tanigawa, 2000, 1432

Endotracheal Intubation • Continuous waveform capnography is recommended in addition to clinical assessment as the most reliable method of confirming and monitoring correct placement of an endotracheal tube (Class I, LOE A) • Providers should observe a persistent capnographic waveform with ventilation to confirm and monitor endotracheal tube placement in the field, in the transport vehicle, on arrival at the hospital, and after any patient transfer to reduce the risk of unrecognized tube misplacement or displacement © 2010 American Heart Association. All rights reserved.
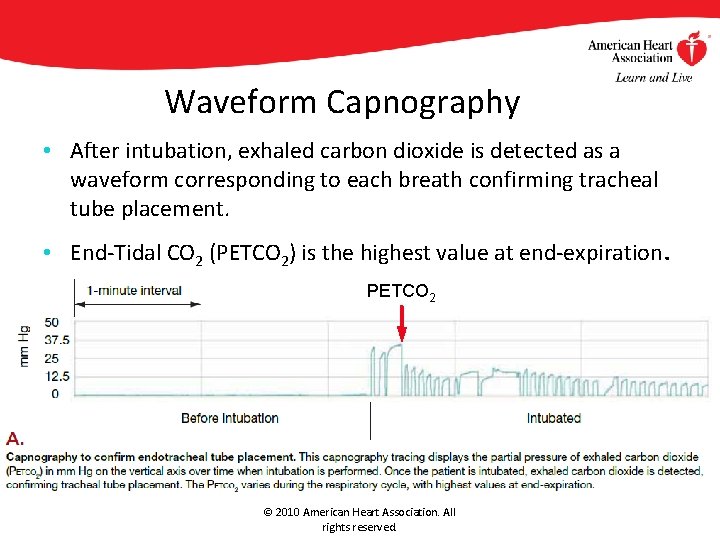
Waveform Capnography • After intubation, exhaled carbon dioxide is detected as a waveform corresponding to each breath confirming tracheal tube placement. • End-Tidal CO 2 (PETCO 2) is the highest value at end-expiration. PETCO 2 © 2010 American Heart Association. All rights reserved.

Management of Cardiac Arrest © 2010 American Heart Association. All rights reserved.
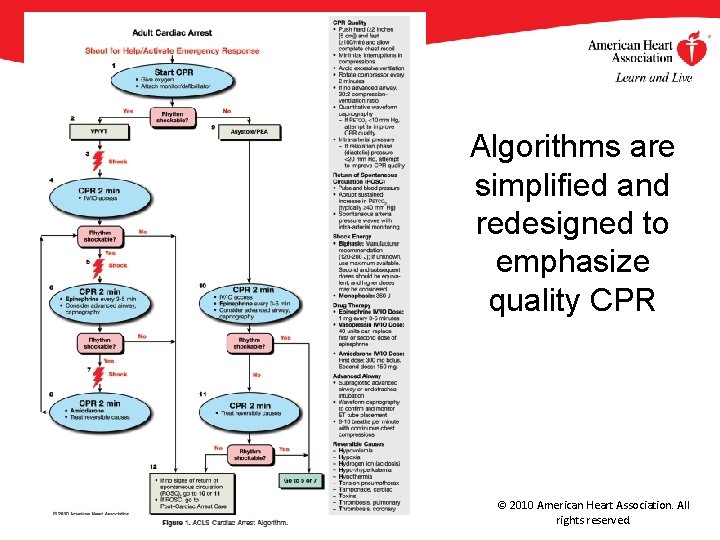
Algorithms are simplified and redesigned to emphasize quality CPR © 2010 American Heart Association. All rights reserved.
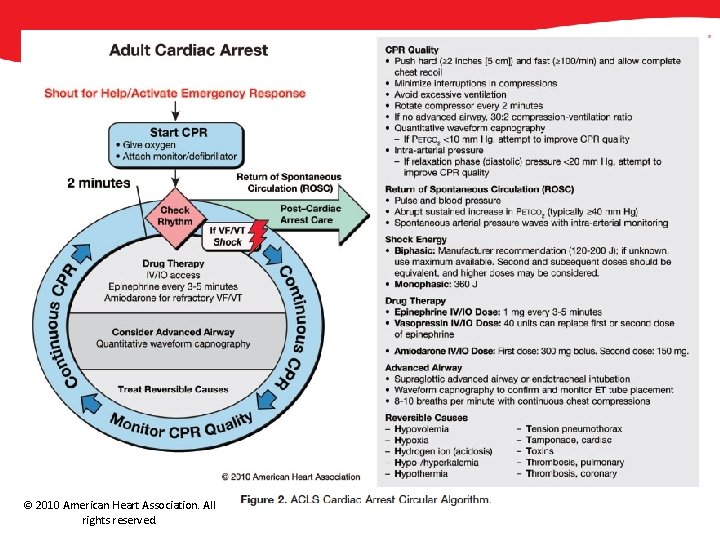
© 2010 American Heart Association. All rights reserved.
![CPR Quality Mechanical Parameters Push hard (≥ 2 inches [5 cm]) Push fast (≥ CPR Quality Mechanical Parameters Push hard (≥ 2 inches [5 cm]) Push fast (≥](http://slidetodoc.com/presentation_image_h/e57bed6e98bb92cbada49ffa11e8767c/image-15.jpg)
CPR Quality Mechanical Parameters Push hard (≥ 2 inches [5 cm]) Push fast (≥ 100/min) Allow complete chest recoil Minimize interruptions in compressions Avoid excessive ventilation © 2010 American Heart Association. All rights reserved.

CPR Quality Physiologic Parameters Quantitative waveform capnography If PETCO 2 <10 mm Hg attempt to improve CPR quality Intra-arterial pressure If relaxation phase (diastolic) pressure <20 mm Hg attempt to improve CPR quality © 2010 American Heart Association. All rights reserved.
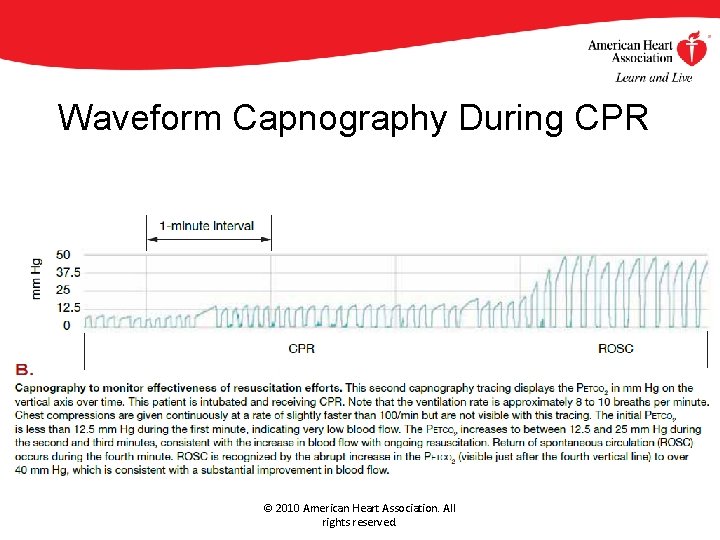
Waveform Capnography During CPR © 2010 American Heart Association. All rights reserved.
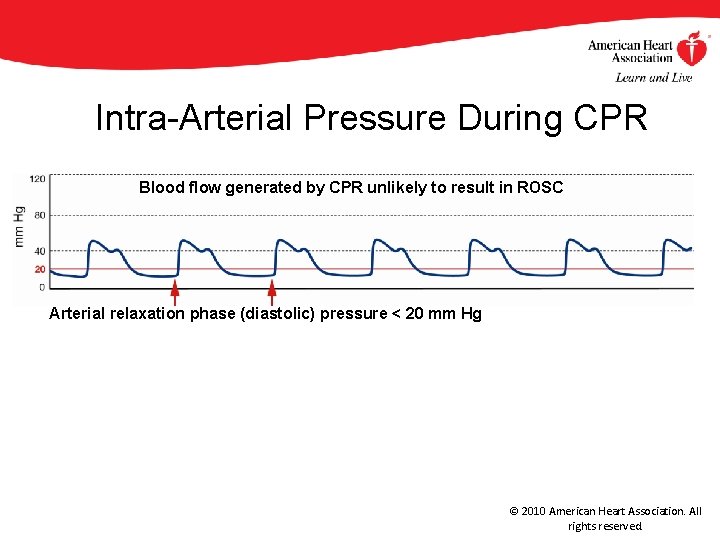
Intra-Arterial Pressure During CPR Blood flow generated by CPR unlikely to result in ROSC Arterial relaxation phase (diastolic) pressure < 20 mm Hg Improved chance of ROSC Arterial relaxation phase (diastolic) pressure 40 mm Hg © 2010 American Heart Association. All rights reserved.

2010 New Science: CPR Pharmacology JAMA 2009
![2010 New Science: CPR Pharmacology • One study [Olasveengen, JAMA, 2009] prospectively randomized patients 2010 New Science: CPR Pharmacology • One study [Olasveengen, JAMA, 2009] prospectively randomized patients](http://slidetodoc.com/presentation_image_h/e57bed6e98bb92cbada49ffa11e8767c/image-20.jpg)
2010 New Science: CPR Pharmacology • One study [Olasveengen, JAMA, 2009] prospectively randomized patients to IV or no IV during management of adult out-of-hospital cardiac arrest. • ROSC 40% IV vs. 25% no IV (OR, 1. 99; 95% CI, 1. 48 -2. 67)] • Hospital Discharge 10. 5% IV vs. 9. 2% no IV (OR, 1. 16; 95% CI, 0. 74 -1. 82)] • Good Neurologic Outcome 9. 8% IV vs. 8. 1% no IV (OR, 1. 24; 95% CI, 0. 77 -1. 98)]. • This study was not adequately powered to detect clinically important differences in long-term outcomes.

CPR Pharmacology • Atropine: changed – No longer recommended for routine use in management of PEA or asystole • • • Epinephrine: unchanged Vasopressin: unchanged Amiodarone: unchanged Lidocaine: unchanged Sodium Bicarbonate: unchanged – Routine use not recommended (Class III, LOE B). • Calcium: unchanged – Routine use not recommended (Class III, LOE B). © 2010 American Heart Association. All rights reserved.

Post-Cardiac Arrest Care © 2010 American Heart Association. All rights reserved.

Post-Cardiac Arrest Care 60 -80% of patients that regain a pulse after cardiac arrest die before hospital discharge Implementation of comprehensive systems of care for post-cardiac arrest patients consistently results in improved survival with good neurologic function © 2010 American Heart Association. All rights reserved.

Post-Cardiac Arrest Care A comprehensive, structured, multidisciplinary system of care should be implemented in a consistent manner for the treatment of post-cardiac arrest patients (Class I, LOE B) Programs should include: • Therapeutic hypothermia • Optimization of hemodynamics, ventilation, and oxygenation • Immediate coronary reperfusion with PCI when indicated • Glycemic control • Neurological diagnosis, management, and prognostication © 2010 American Heart Association. All rights reserved.
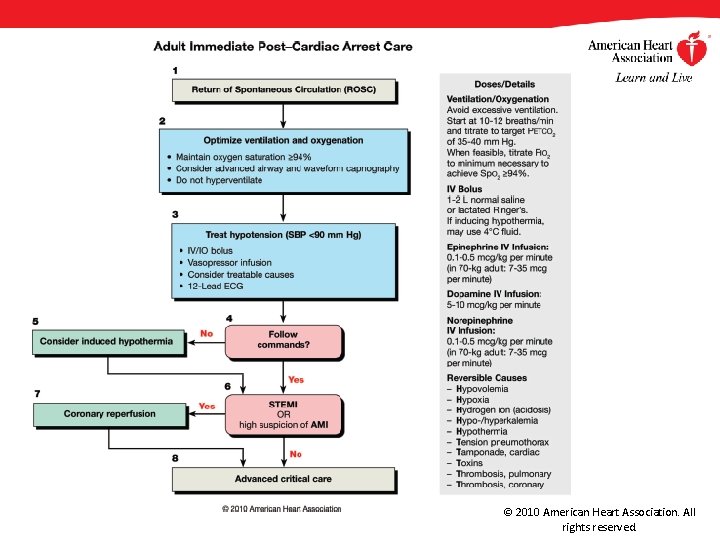
© 2010 American Heart Association. All rights reserved.

Post-Cardiac Arrest Hypothermia Comatose (ie, lack of meaningful response to verbal commands) adult patients with ROSC after out-of-hospital VF cardiac arrest should be cooled to 32°C to 34°C (89. 6°F to 93. 2°F) for 12 to 24 hours (Class I, LOE B) Induced hypothermia also may be considered for comatose adult patients with ROSC after in-hospital cardiac arrest of any initial rhythm or after out-of-hospital cardiac arrest with an initial rhythm of pulseless electric activity or asystole (Class IIb, LOE B) © 2010 American Heart Association. All rights reserved.

Post-Cardiac Arrest ACS/AMI A 12 -lead ECG should be performed as soon as possible after ROSC (Class I, LOE A). Appropriate treatment of ACS or STEMI, including PCI or fibrinolysis, should be initiated regardless of coma (Class I, LOE B). Coma and the use of induced hypothermia are not contraindications or reasons to delay PCI or fibrinolysis. © 2010 American Heart Association. All rights reserved.

Post-Cardiac Arrest Primary Percutaneous Coronary Intervention (PPCI) For patients with out-of-hospital cardiac arrest due to VF in the setting of STEMI (or new or presumably new LBBB), emergent angiography with prompt recanalization of the infarct-related artery is recommended (Class I, LOE B) PPCI after ROSC in subjects with arrest of presumed ischemic cardiac etiology may be reasonable, even in the absence of a clearly defined STEMI (Class IIb, LOE B) © 2010 American Heart Association. All rights reserved.

© 2010 American Heart Association. All rights reserved.
- Slides: 29