Never work with children or animals David I


























- Slides: 32

Never work with children or animals David I Campbell Consultant Paediatric Gastroenterologist Sheffield Children’s Hospital

• I don't care to belong to a club that accepts people like me as members. Groucho Marx

A characteristic of the normal child is he doesn't act that way very often Even when freshly washed and relieved of all obvious confections, children tend to be sticky. Fran Lebowitz Children are unpredictable. You never know what inconsistency they're going to catch you in next. Franklin P. Jones

Paediatric pharmacology • 50 -90% agents used in children not for their primary use. • Practice by extrapolation of dose and risk. • Especially high usage of off-label and licence in complex rare diseases.


…. and in humans

GORD Corner stone of treatment 1. Feed thickeners 2. Prokinetics 3. Antacids – Ranitidine 3 mg/kg tds – Omeprazole 1 mg/kg od

The “What” of GORD • Lower oesophageal sphincter – Muscle – Nerve – Mucosa

A less commonly recognised side effect of PPI’s

Less commonly recognised side effect of PPI’s • C. difficile colitis – 3 month usage, any agent. – “Less is more” approach – Drug holidays – Advise GP’s to screen stools if child develops diarrhoea

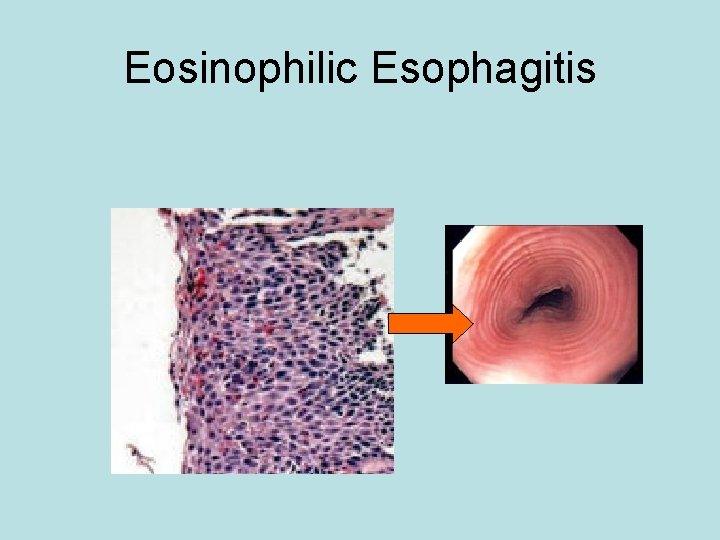
Eosinophilic Esophagitis

Therapies for EE • In paediatric practice close association with GORD. • Often continue PPI • 5 food elimination diet • Budesonide 500 mcg in 15 mls of simple Syrup (od/bd)

IBD The phenomenon • 40 : 100, 000 • Incidence of Crohn’s risen 3 fold in last 10 years. • UC also rising • Younger age of onset • More severe paediatric disease phenotype • Crohn’s more colonic disease

What is it? • Idiopathic inflammatory disorder of the gastrointestinal tract classified as: 1. Crohn’s disease (involving anywhere along the GI tract from mouth to anus). 2. Ulcerative colitis (involving the large bowel only, but in a confluent manner). 3. Indeterminate colitis (colonic disease but with atypical features).

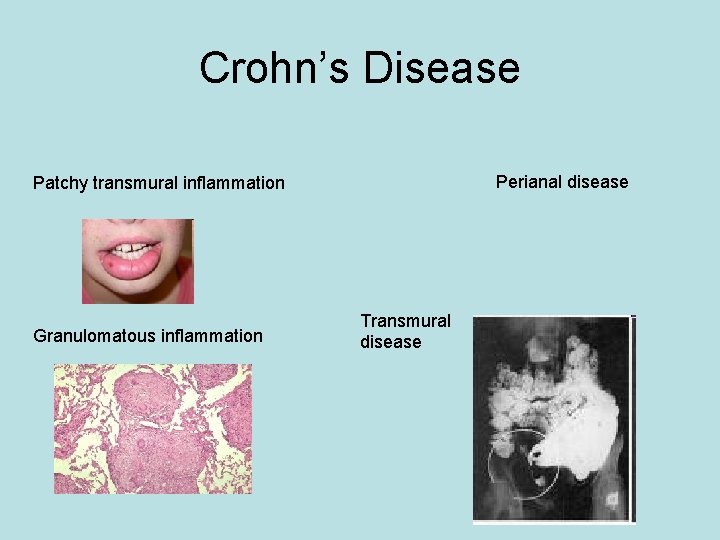
Crohn’s Disease Perianal disease Patchy transmural inflammation Granulomatous inflammation Transmural disease

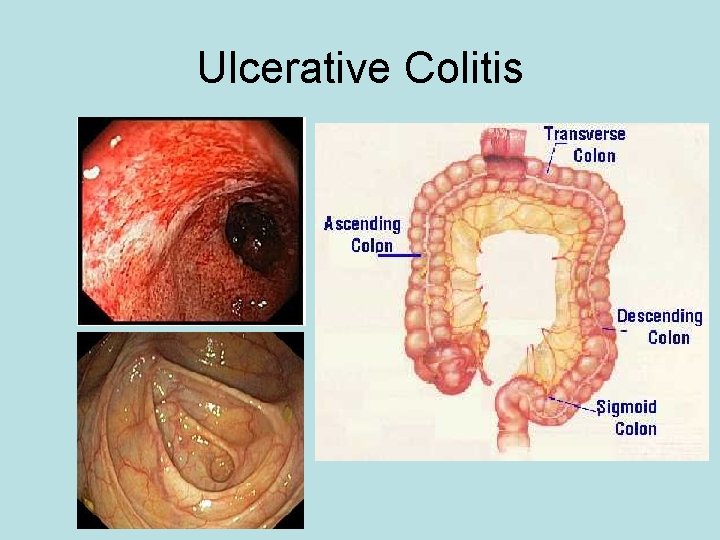
Ulcerative Colitis

Strategies • Induce remission and then maintain remission. • Induction of remission: Steroids, liquid nutritional therapy, biological agents, cyclosporin, surgery. • Maintenance of remission: 5 -ASA, low dose steroids, azathioprine, biologicals.

Drugs • 5 -aminosalicylates • Mild to moderate UC. • Mechanism of action unclear. • Recent warnings to remember monitor U+E 6 -12 monthly. • Headaches (mesalazine associated with myocarditis).

Steroids • Both induction (can be IV) and occasionally maintenance (UC). • Both extremes of excessive use and fear. • Concurrent use of ranitidine with high doses (prednisolone 2 mg/kg).

Steroids II • Use of higher doses? • Induction of remission in fulminant colitis or steroid resistance: IV hydrocortisone, methyl pred or dexamethasone. • GVHD or allograft rejection 20 mg/kg methyl pred • Doses above 100 mg qds hydrocortisone no more effective in IBD. • If unresponsive consider surgery (cy. A for UC or IFX).

Azathioprine • 6 -TG prodrug. • TPMT status. • HGPRT • 60% Chance of maintenance of remission long term in Crohn’s.

Why is azathioprine a good drug? • Mainly dose dependant side effects that can be screened. • • Haematological Renal Hepatitis “Pancreatitis” • How do we screen.

Regular blood monitoring

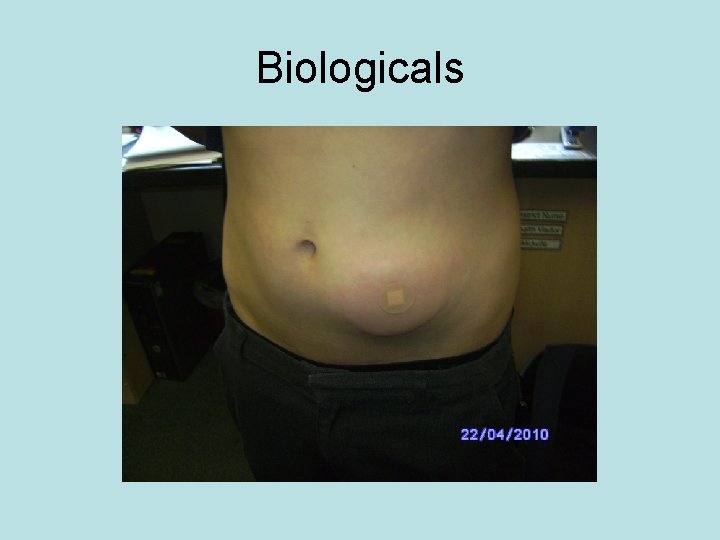
Biologicals

Infliximab • Chimeric mouse antibody • Blocking Th 1 memory cells. • Antibody mediated cell lysis. • Induction of lymphocyte apoptosis.

Alternatives to Remicade® • • Humira (Adalimumab) (Visilizumab, etanercept): Not effective Certolizumab-Crohn’s Natalizumab (Crohn’s and UC) Astrocytoma and Multifocal leukoencephalopathy

Effectiveness of Remicade® • 80% reduction in hospitalization, 50% reduction in surgery (fistulating disease). • Accent trial showed early response from day 1 high predictor for long term remission (with maintenance treatment), steroid withdrawal

Biologicals • Cancer risk • 1: 1000 but HSTL • Only 15 cases, but all Crohn’s related • Lower risk but also other NHL with aza/6 MP. • Infections – Serious infections 4%, all infections 10% – TB, nocardia, gram negative, listeria

But children and animals might lead the way. Single gene disorders that potently Inhibit the immune system. • Chronic gut inflammation • Autoimmune disease

“Never” work with children or animals? • We get unique insights in to pathophysiology of disease from both. • New drugs have been developed from single gene disorders (particularly in mouse knock-out models). • Risk of c. difficile in long term PPI use.

Conclusions II • Incidence of EE rising, second line treatment focusing on budesonide. • Reminder of some of issues with IBD drugs particularly biologicals. • Risk of cancers, severe acute allergic reactions and sepsis, but still a highly effective form of treatment.

Thank you for your attention Any questions?