Neutropenia in Pediatrics Bradd Hemker MD Pediatric and

Neutropenia in Pediatrics Bradd Hemker MD Pediatric and Adolescent Hematology and Oncology Department of Pediatrics and Human Development Michigan State University

Objectives • Define neutropenia and risks associated with various levels of neutropenia • Review causes of neutropenia in childhood • Discuss proper initial evaluation and management of neutropenia • Discuss when to refer to pediatric hematologist

Definition of Neutropenia • Absolute Neutrophil Count (ANC) – ANC = WBC x (% bands + segs) • Normal ANC: 1500/mm 3 • Neutropenia – Mild: 1000 -1500 – Moderate: 500 -1000 – Severe: <500 • Age matters (slightly)

Pediatric Neutropenias • History – Recurrent infections – Recurrent oral ulcers

Neutropenia Related Infection • Risk of serious bacterial or fungal infection when ANC <500 • Also depends on bone marrow reserve – Inability to make neutrophils (SCN or chemotherapy) = higher risk – Destruction of neutrophils (auto-immune) = lower risk

Causes of Neutropenia • Acquired – Infection – Infiltrative bone marrow disease – Immune mediated – Medication • Congenital – Severe Congenital – Cyclic neutropenia – Chronic benign neutropenia of childhood – Chronic neutropenia of childhood – Benign Ethnic Neutropenia – Schwachman Diamond syndrome

Infection related neutropenia • Most common cause of low ANC in pedatrics • viral or bacterial – May be immune mediated • +/- anti-granulocyte antibodies – Direct bone marrow suppression – Marginalization of neutrophils • Treatment: none typically needed – May take 3 -4 weeks or longer to resolve!

Auto-Immune Neutropenia • • Often triggered by infection May be part of broader auto-immune disorder Anti-granulocyte antibodies positive Treatment – +/- IVIG, steroids, GCSF – Only if severe infection (ie hospitalized) • May take years to resolve!

Neonatal Alloimmune Neutropenia • Maternal antibodies to paternal antigens on fetal platelets • Identical to Rh disease of newborn • Typically resolves spontaneously over weeks to few months • Diagnosis: testing of parental blood
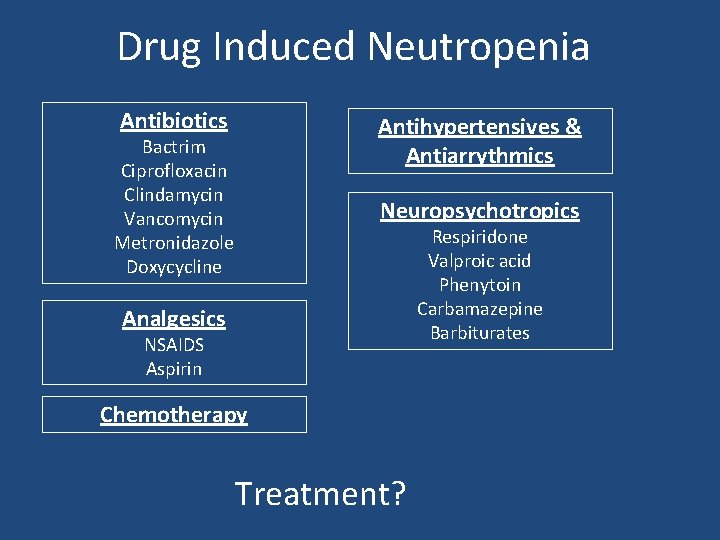
Drug Induced Neutropenia Antibiotics Antihypertensives & Antiarrythmics Bactrim Ciprofloxacin Clindamycin Vancomycin Metronidazole Doxycycline Neuropsychotropics Respiridone Valproic acid Phenytoin Carbamazepine Barbiturates Analgesics NSAIDS Aspirin Chemotherapy Treatment?

Congenital Neutropenias • Severe Congenital Neutropenia (Kostmann Syndrome) – Incidence ~1/1, 000 – Severe infections early in life—pneumonia, abscesses, etc – Inability to make neutrophils ANC very low – Typically diagnosed in infancy • Elastase 2 mutation (ELA-2) – Treatment: GCSF

Congenital Neutropenias • Schwachmann Diamond Syndrome – Neutropenia, pancreatic insufficiency – Presents in 1 st 10 years of life with steatorrhea, growth failure and infections – Physical anomalies are common (cleft palate, syndactyly, strabismus)

Congenital Neutropenia • Cyclic Neutropenia – Blood counts cycle every ~21 days • ANC most pronounced – Recurrent fevers, bacterial infections when ANC low – Diagnosis • Standard = CBC twice weekly x 6 weeks • ELA-2 testing – Treatment: GCSF if significant infectious history

Congenital Neutropenia • Chronic Neutropenia of Childhood – ANC often <500 – Associated with significant infectious history – Diagnosis of exclusion • No evidence of cycling counts • Normal bone marrow • +/- anti-granulocyte antibodies – Treatment: GCSF if significant infections

Congenital Neutropenia • Chronic Benign Neutropenia of Childhood – ANC often <500 – Not associated with significant infectious history – Diagnosis of exclusion • No evidence of cycling counts • Normal bone marrow • +/- anti-granulocyte antibodies – Treatment: GCSF if significant infections

Congenital Neutropenia • Syndrome associated neutropenia – – – – Myelokathexis (WHIM syndrome) Glycogen storage disease type 1 Mitochondrial disorders Congenital cobalamin deficiency X-linked agammaglobulinemia Chediak-Higashi syndrome GCSF receptor mutations

Benign Ethnic Neutropenia • Overall WBC and ANC vary by ethnic group – African Americans tend to run lower compared to causcasians – ANC of 1100 may not be abnormal for some patients! • Slightly low ANC without any signficant infectious history may not require any further work up!

Workup of Neutropenia • History, exam – Recurrent infections – Recurrent oral ulcers • Labs – CBC w/ differential – Anti-granulocyte antibodies

Workup of Neutropenia • If suspect post-infectious – Repeat labs in 3 -4 weeks – if ANC remains low but improved and patient is clinically well—repeat in another 3 -4 weeks. – If no change over this time consider referral to hematologist

When to worry. . . • ANC <500 with fever – hospitalization for blood cultures, IV antibiotics • Worrisome history – Recurrent fevers, night sweats, weight loss, enlarged lymph nodes, refusal to walk, bone pain • Worrisome exam – Lymphadenopathy, organomegaly

When to Refer • Persistently low ANC (< 1000) regardless of infectious history • Mildly low ANC with significant infectious history • Worrisome history or exam findings that are not improving as viral symptoms do. . .

Pediatric Hematology Neutropenia Work-Up • Detailed history regarding infections, ulcers, diarrhea, etc. • Repeat CBC w/ manual diff – Review peripheral smear – Concern for other cytopenias or other WBC morphologic abnormalities bone marrow asp/bx • Cyclic neutropenia work-up – CBC twice weekly x 6 weeks – ELA 2 gene testing • Repeat counts every 2 -4 weeks—less often if patient stable without ongoing infectious concerns • Bone marrow evaluation

Treatment of Neutropenia • Granulocyte colony stimulating factor (GCSF) – 1 -5 mcg/kg SQ • Daily • Three times per week • Weekly. . . • When? – Symptomatic neutropenia (serious infection) – Prevention of neutropenia (if h/o serious infections)

Chronic Neutropenia • Children need evaluation with any fevers – CBC w/diff – Blood culture – +/- empiric antibiotics (ceftriaxone) • If ANC < 500 hospitalize for IV antibiotics until blood cultures negative and ANC improving • If ANC > 500 treat like any other child

Questions? Bradd. Hemker@hc. msu. edu

References • • Donadieu et al. Congenital neutropenia: diagnosis, molecular bases and patient management. Orphanet J Rare Dis. 2011; 6: 26 James RM, Kinsey SE. The investigation and management of chronic neutropenia in children. Arch Dis Child. Oct 2006; 91(10): 852 -858 Walkovich K, Boxer LA. How to approach Neutropenia in Childhood. Pediatrics in Review. 2013; 34; 173 Horwitz et al. Neutrophil elastase in cyclic and severe congenital neutropenia. Blood 2007, 109(5): 1817 -1824 Dale et al. Cyclic Neutropenia. Seminars in Hematology. 2002, 39(2): 89 -94 Berliner et al. Congenital and Acquired Neutropenia. American Society of Hematology Education Book. 2004, 1: 63 -79 Andersohn et al. Systematic Review: Agranulocytosis Induced by Nonchemotherapy Drugs. Ann Intern Med. 2007; 146: 657 -665
- Slides: 26