Neuron The neuron is the basic cell of

Neuron • The neuron is the basic cell of the nervous system • Neurons provide an instant method of cellular communication

Neuron • There are unimaginable variations in neuron structure and function • There are many common features and physiology
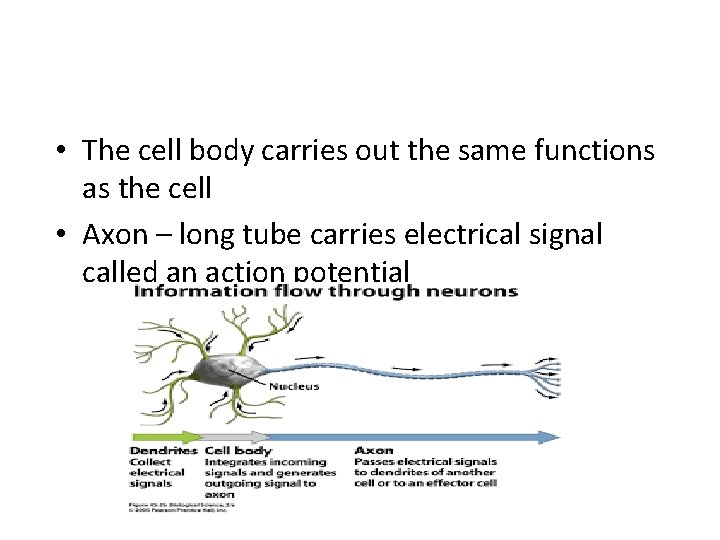
• The cell body carries out the same functions as the cell • Axon – long tube carries electrical signal called an action potential

• Action potential – is the electrical signal that is carried down the axon • -the action potential is carried only one way
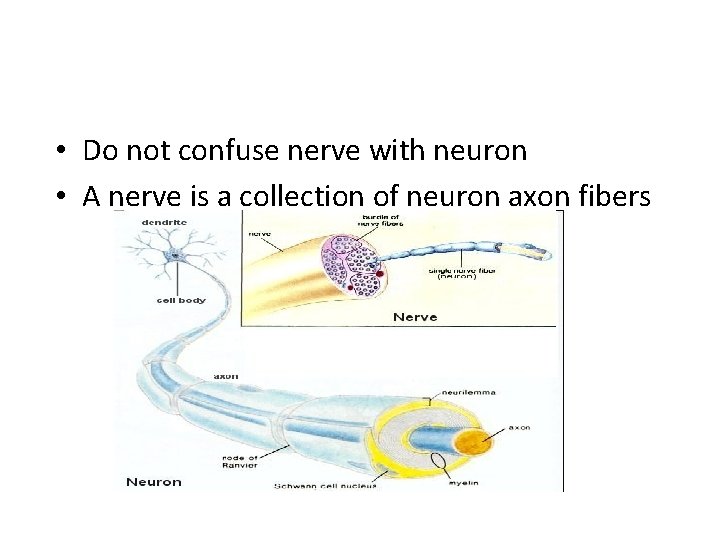
• Do not confuse nerve with neuron • A nerve is a collection of neuron axon fibers

• The signals in nerves can run both ways • - Efferent (Out) • - Afferent (In)
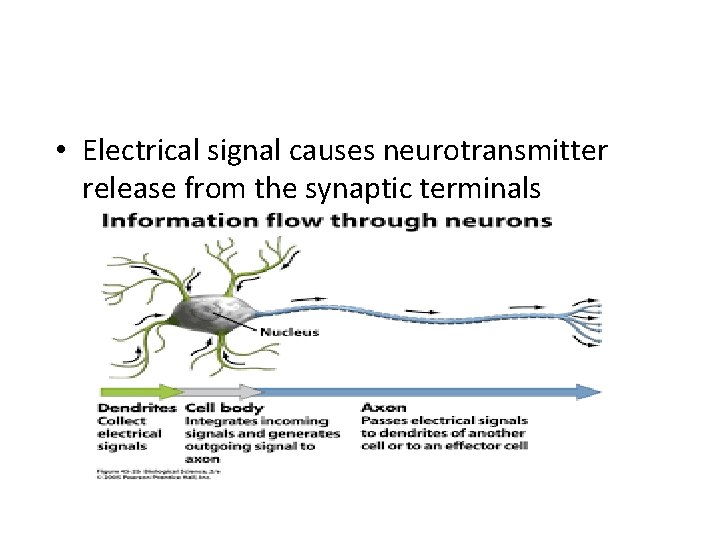
• Electrical signal causes neurotransmitter release from the synaptic terminals
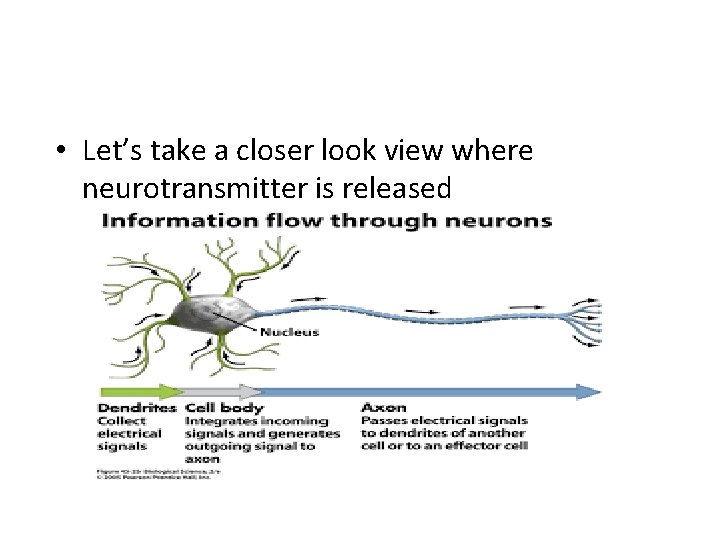
• Let’s take a closer look view where neurotransmitter is released
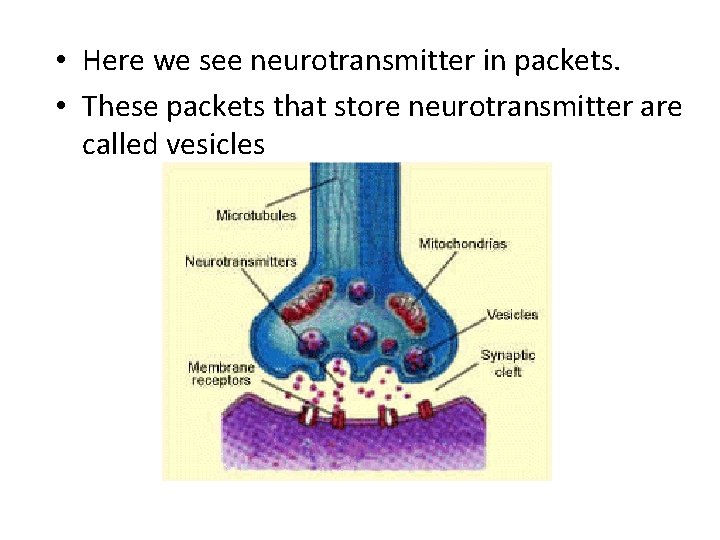
• Here we see neurotransmitter in packets. • These packets that store neurotransmitter are called vesicles
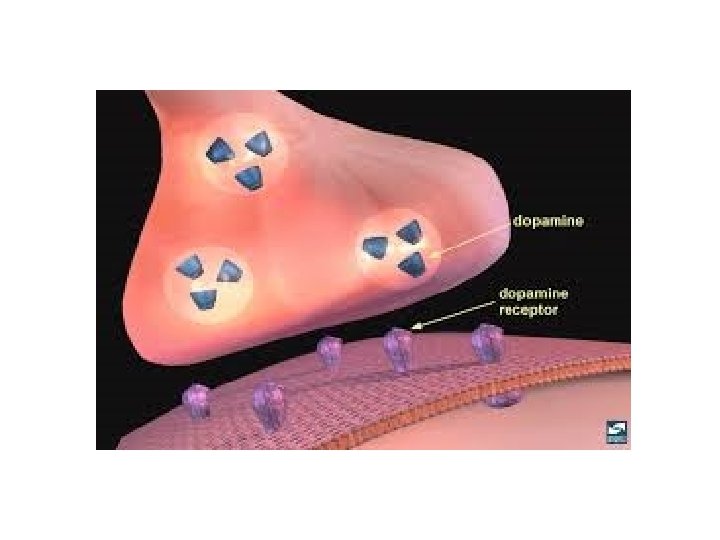
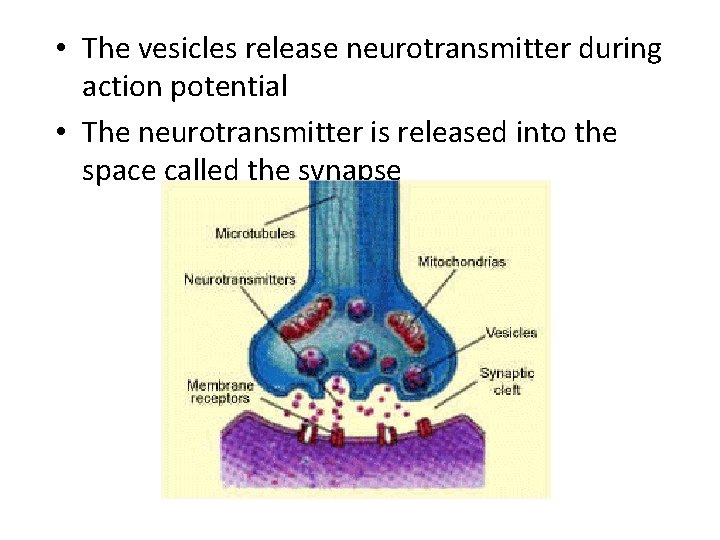
• The vesicles release neurotransmitter during action potential • The neurotransmitter is released into the space called the synapse
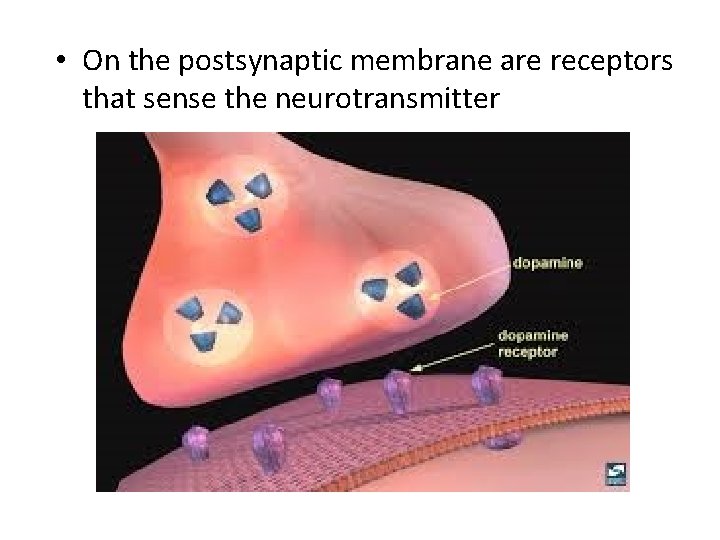
• On the postsynaptic membrane are receptors that sense the neurotransmitter

• Neurotransmitters • -chemicals released from neurons to communicate with: muscle, organ, other neurons

CNS Neurotransmitters • Acetylcholines • Catecholamines – Dopamine, norepinephrine, epinephrine Serotonin GABA – Gama Amino Butyric Acid

• Acetylcholine is made from: Acetyl. Co. Enzyme. A – made by mitochondria as part of energy transfer Choline – lecithin has fatty acids that contain choline
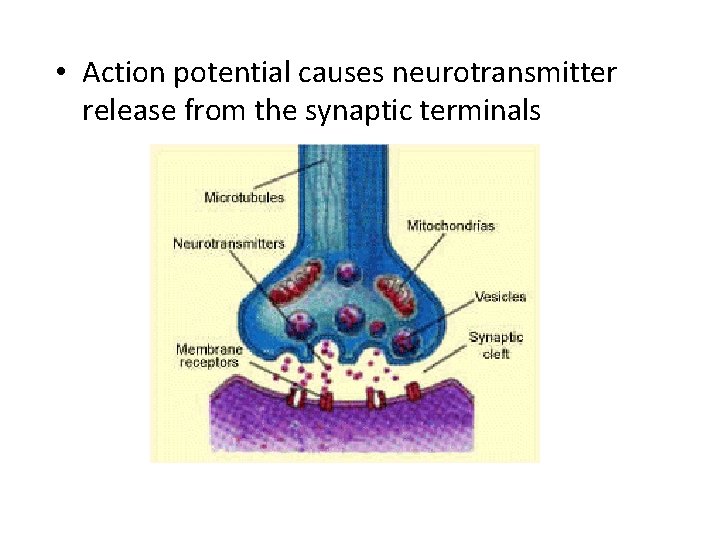
• Action potential causes neurotransmitter release from the synaptic terminals

GABA • Is inhibitory • GABA opens chloride channels • Opening chloride channels cancels the excitatory effect of opening sodium channels

• Small inhibitory neurons keep large neurons quiet • Loss of inhibition results in excessive neuron activity • Small inhibitory neurons use GABA as a neurotransmitter
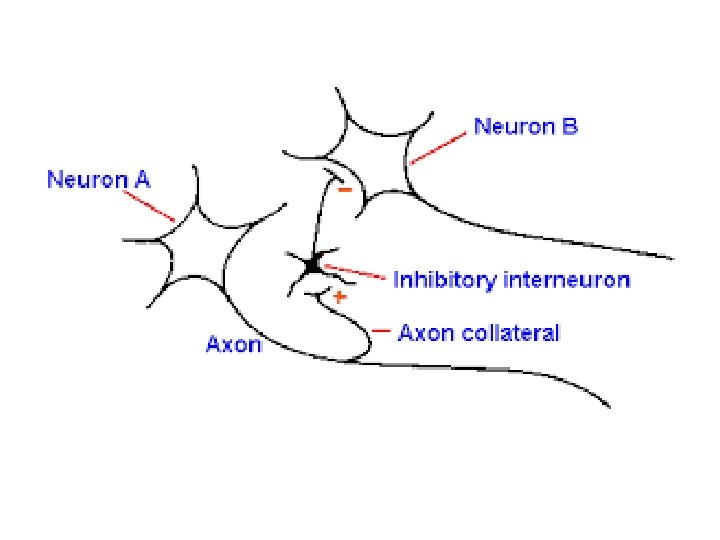

Where is Acetylcholine? • Neuromuscular junction • The neurotransmitter that signals voluntary muscle movement is acetylcholine • The receptor type is nicotinic
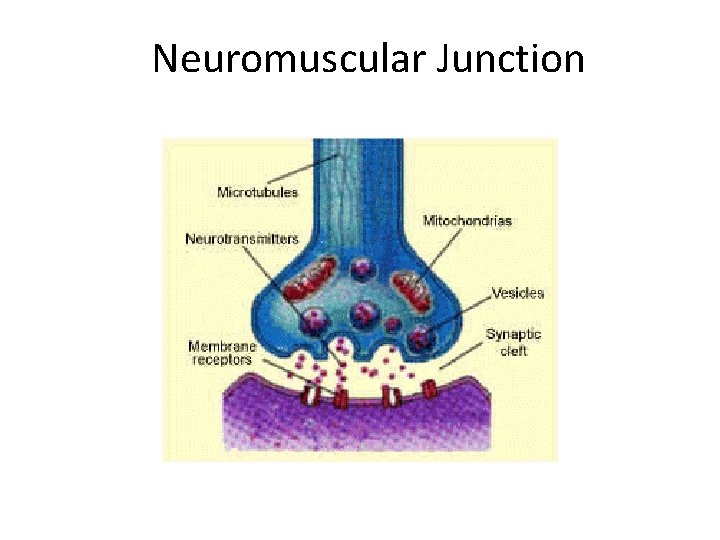
Neuromuscular Junction

Myasthenia Gravis • Weakness is caused by circulating antibodies that block acetylcholine receptors at the postsynaptic neuromuscular junction
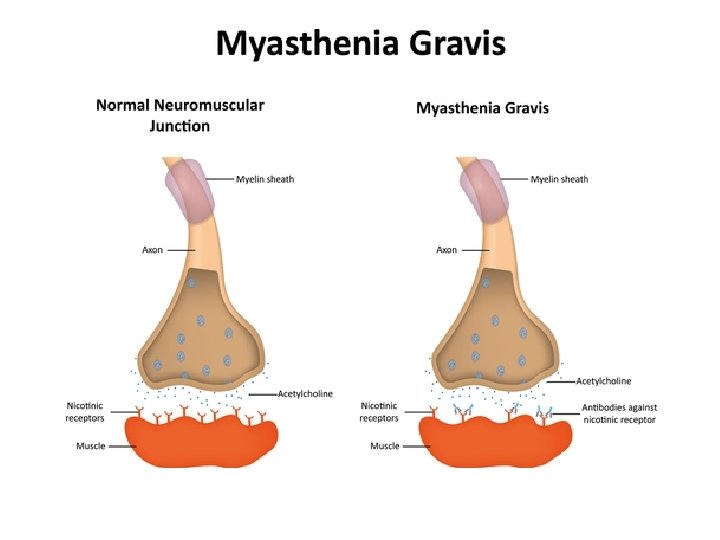

Where is acetylcholine? • ANS • The neurotransmitter that signals parasympathetic smooth muscle movement is acetylcholine • The receptor type is muscarinic
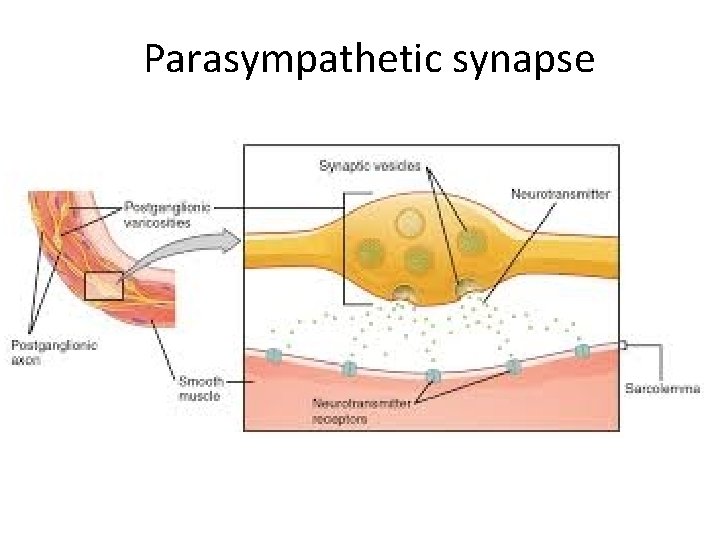
Parasympathetic synapse
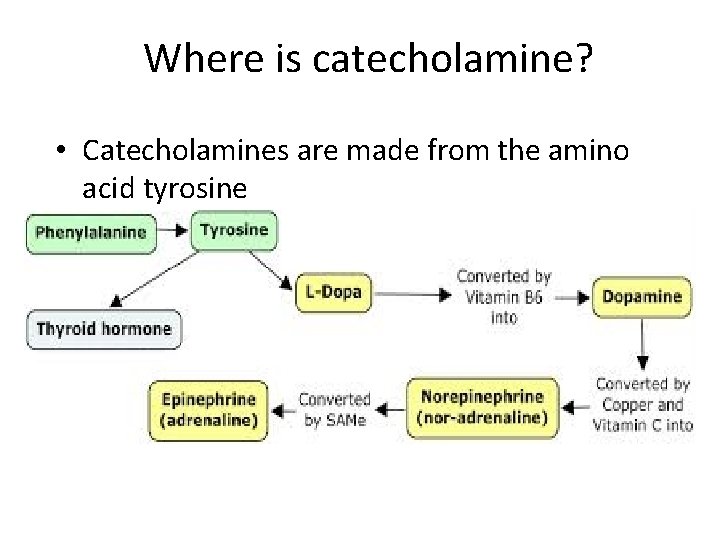
Where is catecholamine? • Catecholamines are made from the amino acid tyrosine

Where is catecholamine? • ANS • The neurotransmitter that signals sympathetic smooth muscle movement and organs is epinephrine and norepinephrine • The receptor type is alpha and beta
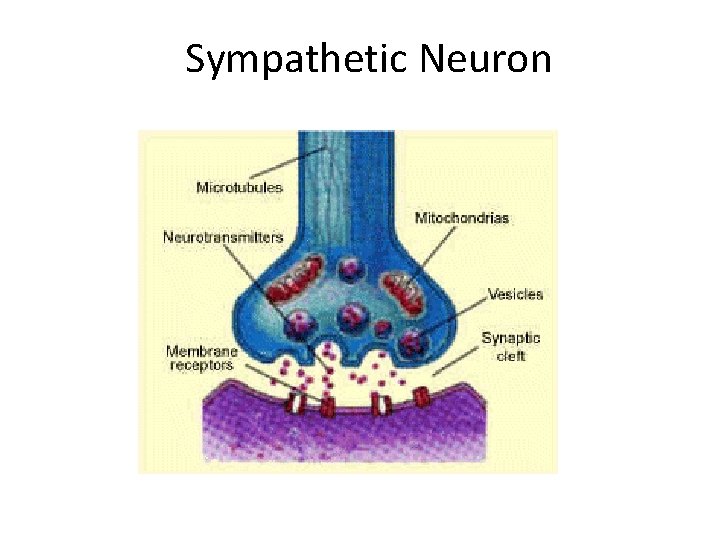
Sympathetic Neuron

Where are catecholamine? • CNS • We will discuss catecholamine medications when we talk about Parkinson’s disease

ANS Neurotransmitters • Acetylcholine • Catecholamines – -norepinephrine, epinephrine
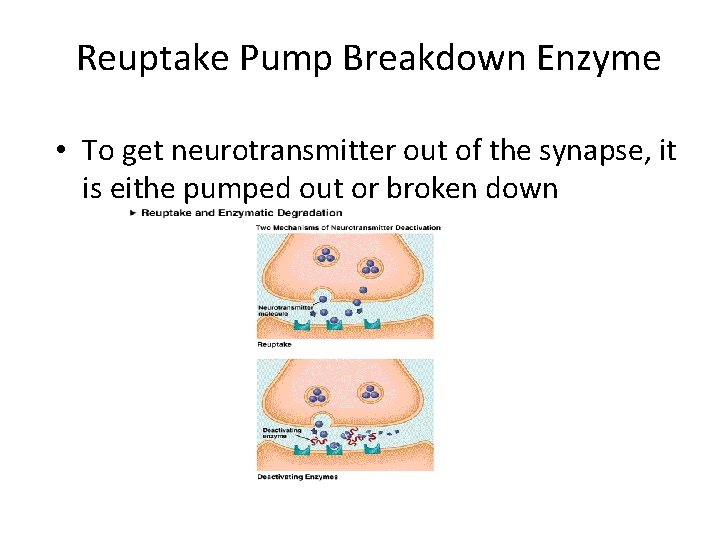
Reuptake Pump Breakdown Enzyme • To get neurotransmitter out of the synapse, it is eithe pumped out or broken down
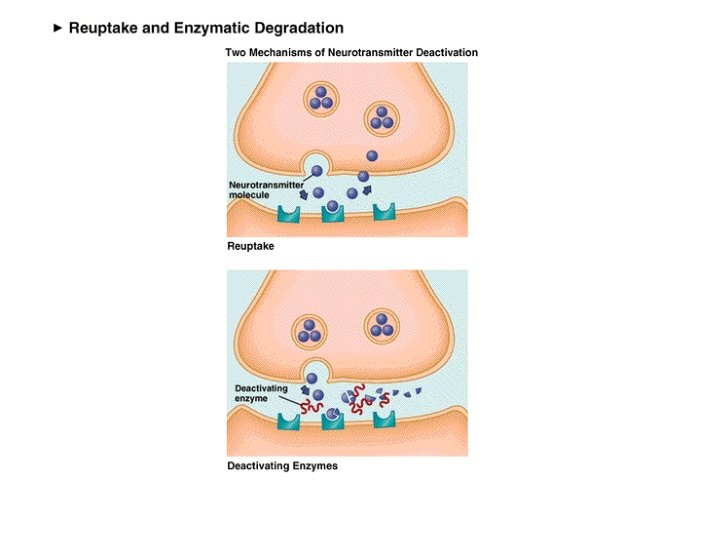

Ach. E • Acetylcholine Esterase • Breaks down acetylcholine in the synapse • So if block acetylcholine esterase, we end up with more acetylcholine in the synapse

SSRI • Selective Serotonin Reuptake Inhibitors • Serotonin is pumped out of the synapse by uptake pumps • If we block these uptake pumps, we end up with more serotonin in the synapse

• Let’s talk more about receptors

Gated Ion Channels • Opening ion channels, like sodium channels, can cause a voltage change across the cell membrane • Instant ON/OFF
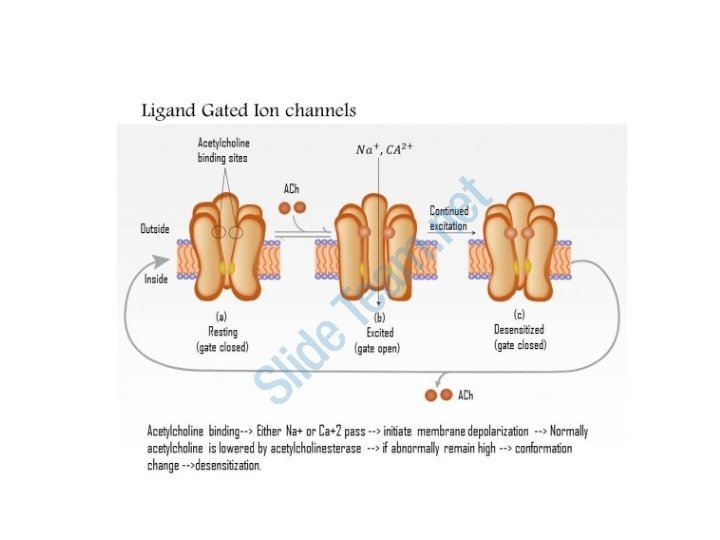

Second Messenger Activation • Allows complex chemical reactions to occur • Gradual Metabolic Changes
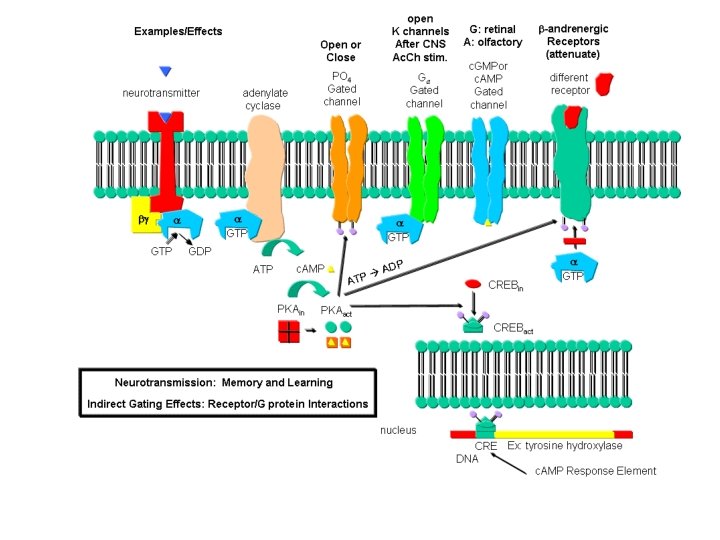
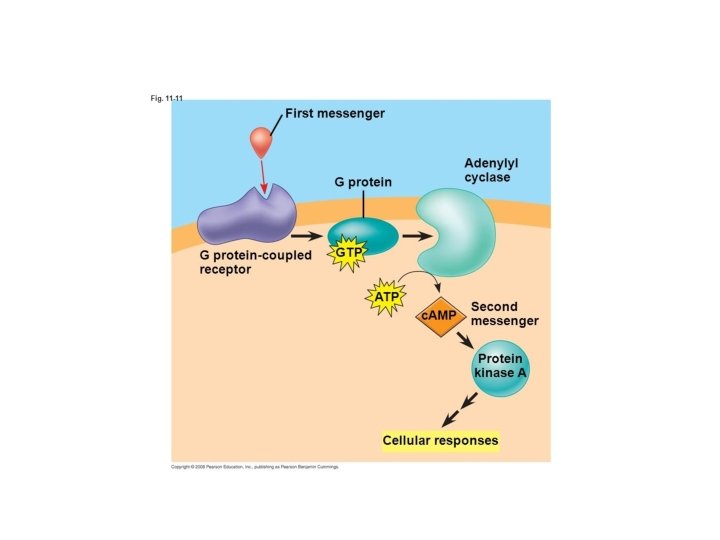

Cyclic AMP activates many different regulatory proteins: • Receptor Regulation • Metabolism Regulation • DNA Regulation
• Cyclic AMP also deactivates many different regulatory proteins

• Cyclic AMP is a second messenger

• Phosphodiesterase removes c. AMP
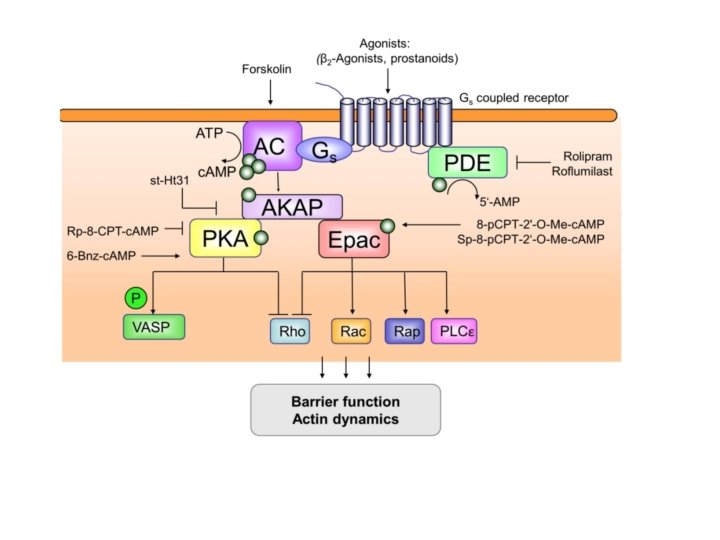

• Phosphodiesterase inhibited by caffeine • Caffeine increases cyclic AMP
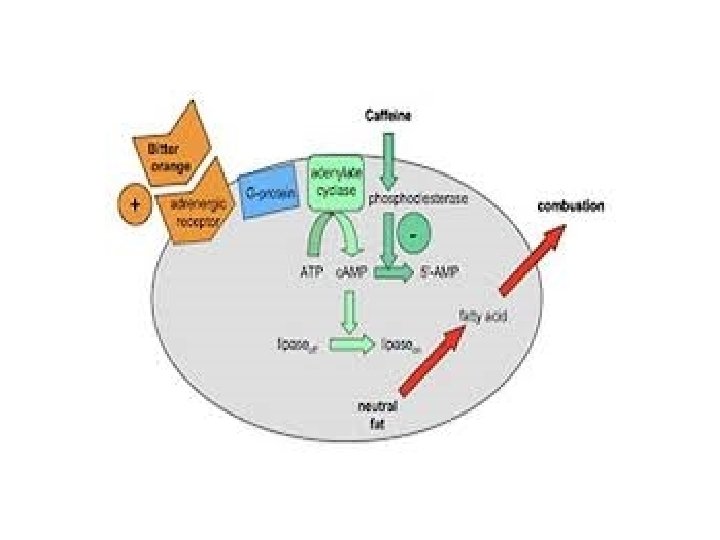
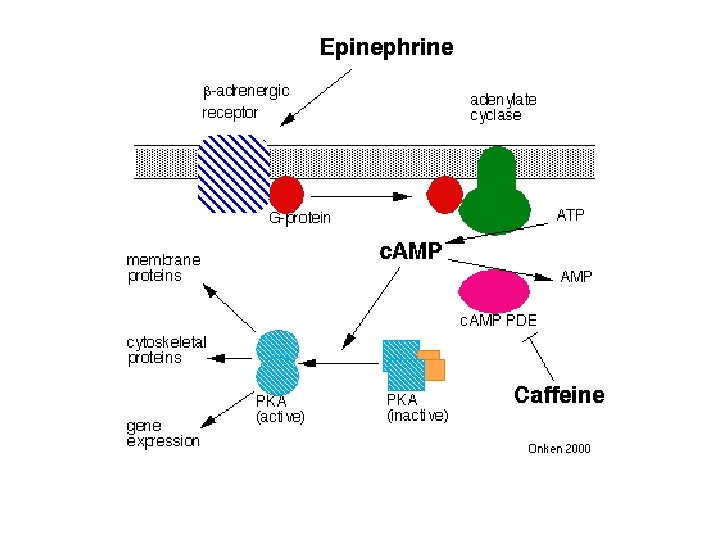

• Activating second messengers will cause metabolic changes • More gradual and long lasting

GABA • GABA is inhibitory • GABA opens chloride channels • Opening chloride channels inhibits neurons because the negative charge cancels the positive charge
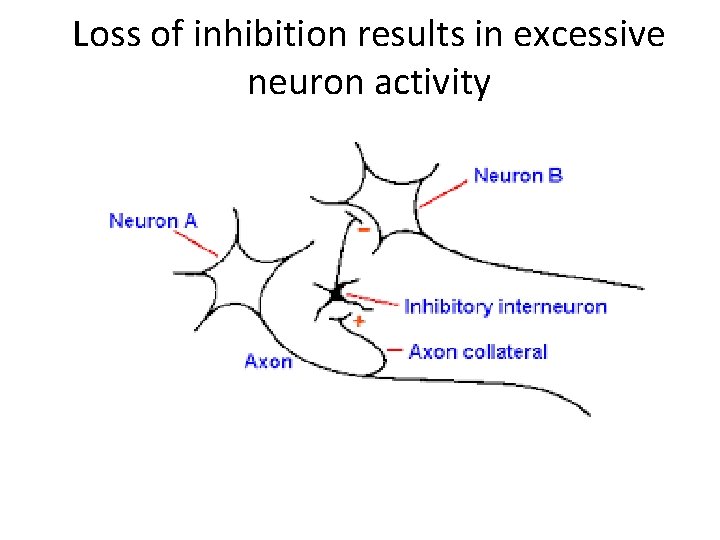
Loss of inhibition results in excessive neuron activity
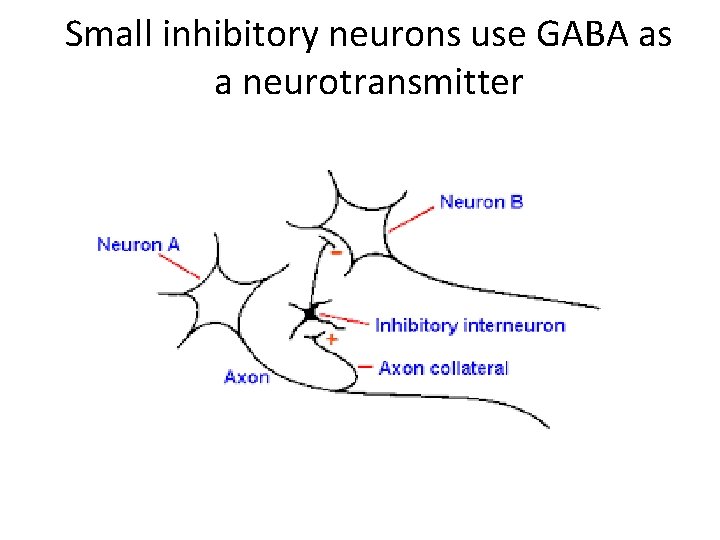
Small inhibitory neurons use GABA as a neurotransmitter

GABA opens chloride channels
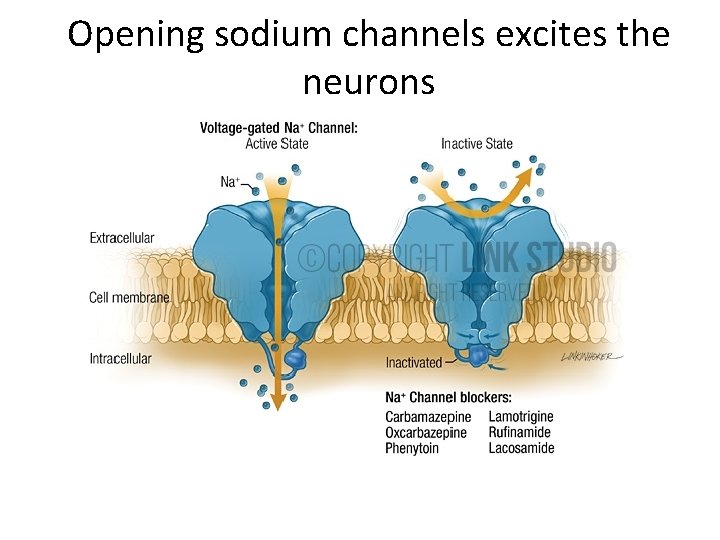
Opening sodium channels excites the neurons
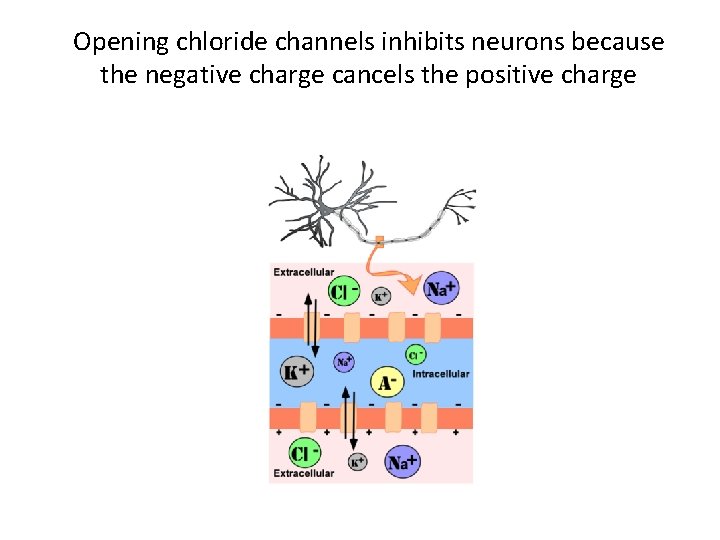
Opening chloride channels inhibits neurons because the negative charge cancels the positive charge

• • • Na. Cl Table salt Put Na. Cl into water Na+ and Cl(Sodium ions and chloride ions)
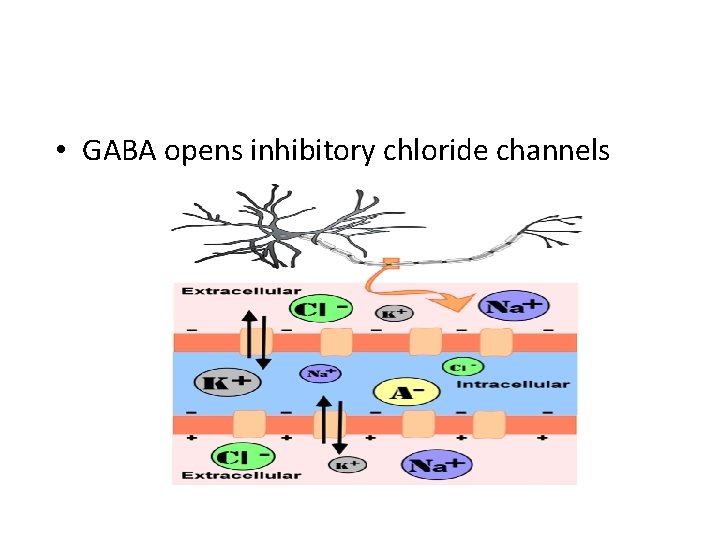
• GABA opens inhibitory chloride channels
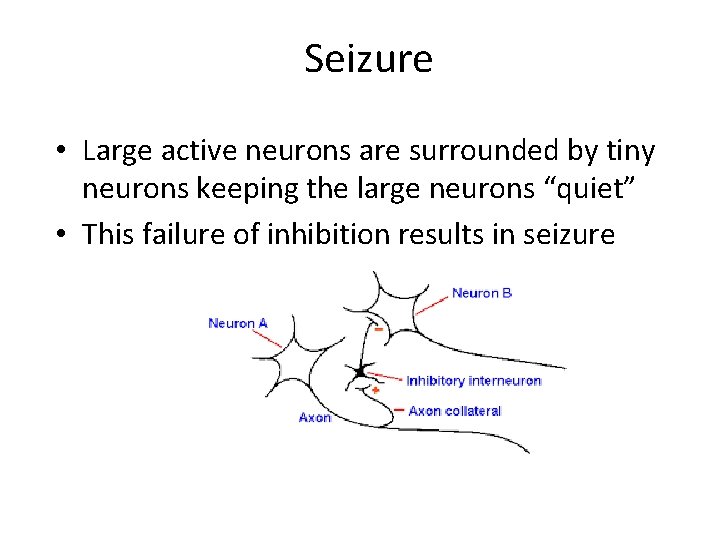
Seizure • Large active neurons are surrounded by tiny neurons keeping the large neurons “quiet” • This failure of inhibition results in seizure

Benzodiazepines • GABA Agonists – Diazepam (Valium)

Diazepam (Valium) • • Anxiolytic, used in treatment of anxiety Alcohol withdrawal Anticonvulsants used to stop seizure PO, IV, PR – rectally for seizures (Diastat)

More Benzodiazepines • • • Alprazolam (Xanax) Chlordiapoxide (Librium) Clonazepam (Klonopin) Clorazepate( Tranxene) Diazepam

Benzodiazepines • The different use of benzodiazepines is determined by prolonged onset of action and elimination half-life • Benzodiazepines are metabolized by the liver. • They have long half-lives • The action of benzodiazepines last a long time • Must be used with caution in the elderly and people with liver disease

Benzodiazepine Toxicity • Excess level of benzodiazepine result in drowsiness, coma, respiratory depression, and can be lethal for these reasons

• If immediate respiratory support is provided while benzodiazepine wears off there are no lasting signs of toxicity • “Touch the Ambu bag and the Romazecon” before giving any IV benzo

Flumazenil (Romazicon) • Antagonizes benzodiazepines, reversing their effect • IV only • Very short half-life, so repeated doses may be required

• Because benzodiazepines are used to stop seizures • Flumazenil (Romazicon) can cause seizures, caution is required

Barbiturates • Are GABA agonists too • Barbiturates and benzodiazepines each have their own receptor site on the GABA chloride channel

Barbiturates (GABA Agonists) • • Phenobarbital “Phenobarb” - seizures Butabital (Esgic, Fioricet, Phrenilin) -pain

• Barbiturates can be taken to prevent seizures • Benzodiazepines cannot, they are only used to stop seizures in progress

Benzodiazepines & Barbiturates • • • Sedative (relaxes, calms) Hypnotic (sleepy) Anxiolytic (antianxiety) Anticonvulsant (antiseizure) Used in anesthesia Hepatic metabolism

Seizures vs Epilepsy • • • Simple – no loss of consciousness Complex – loss of consiousness Partial – onset with localized symptoms Generalized 10 and 20 Grand Mal, Petit Mal, Absence Post Ictal – stuporous state after seizures

The anticonvulsants • • • Phenytoin (Dilantin) – Na channel blocker Carbamazepine – Na channel blocker Valproic Acid – GABA increaser Phenobarbital – GABA agonist Benzodiazepines – GABA agonist

Anticonvulsants (GABA Agonists) • Pregabalin (Lyrica) • Gabapentic (Neurontin)
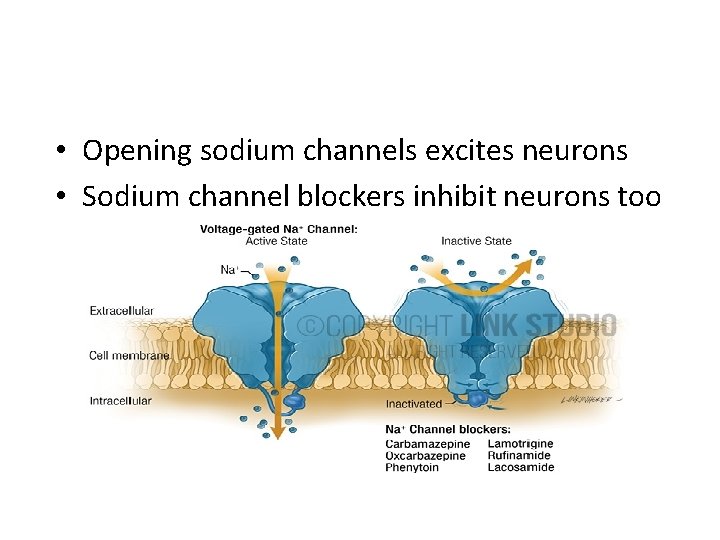
• Opening sodium channels excites neurons • Sodium channel blockers inhibit neurons too

Phenytoin (Dilantin) • • Na+ channel blocker Is a hydantoin anticonvulsant PO IV (can cause hypotension, give slowly)

Phenytoin (Dilantin) toxicity • • Gingival hyperplasia (gum disease) Confusion Check serum levels Can cause fetal hydantoin syndrome

Carbamazepine Tegretol • Na+ channel blocker • Is a carboxamide anticonvulsant • PO

Carbamazepine Tegretol toxicity • Requires frequent CBC testing • Aplastic anemia and agranulocytosis

Local Anesthesia • Lidocaine is a sodium channel blocker used as a local anesthetic • Sometimes epinephrine is added to occlude local blood vessels, keeping lidocaine from being carried away by the blood

Lidocaine toxicity • Is due to entry into systemic blood • CNS and cardiovascular toxicity

• CNS lidocaine toxicity can cause nervousness, tingling around the mouth, tinnitus, tremor, dizziness, blurred vision, seizures, coma and respiratory depression

• Cardiovascular lidocaine toxicity can cause cardiovascular collapse if person depends on ventricular rhythm

Drug Classes: • • Tri Cyclic Antidepressants (TCA) Mono Amine Oxidase Inhibitors (MAOi) Serotonin Reuptake Inhibitors (SSRI) Miscellaneous Agonists – -these are the antidepressants

TCA, MOAi, SSRI, are used in: • • Depression Anxiety Obsessive compulsive disorder Dysthymia Headache Smoking cessation Obesity

SSRI • Is a selective serotonin reuptake inhibitor • More available serotonin because uptake is inhibited

There are many SSRIs in the market: • • • Fluoxetine (Prozac) Sertraline (Zoloft) Paroxetine (Paxil) Citalopram (Celexa) Escitalopram (Lexapro)

• All SSRIs warn of suicidal ideation especially in youth

TCA’s Tricyclic Antidepressants • TCA’s prevent the reuptake of serotonin and norepinephrine

TCA’s • Amitryptyline is a TCA used for depression, and pain as well. • Especially useful for headaches

TCA’s • • Clomipramine (Anafranil) Doxepin Desipramine Imipramine (Tofranil)

TCA toxicity • TCA’s can be cardiotoxic in excessive dosages • Alkalinization by giving bicarbonate helps prevent TCA toxicity and increases elimination

MAOi Monoamine oxidase inhibitors • Prevent breakdown of catecholamines and serotonin • Safety is a concern with MAOi because of all the possible toxic interactions with other CNS drugs

MAOi • Phenelzine (Nardil) • Selegiline (Eldepryl) • Linezolid (Zyvox) – -antibiotic with MAOi properties

MAOi • Many SSRI’s like Prozac, TCAs and many other adrenergic and CNS medications are “contraindicated” to use within 14 days of MAOi therapy

MAOi • How many drugs can you find that are contraindicated for use within 14 days of MAOi therapy? • Difference between life and death

Parkinson’s disease • Is a progressive degenerative neurologic disease that affects movement

Resting Tremor Video

Shuffled Gait Video
Cog Wheel Rigidity Video

Choreoathethosis Video

Parkinson’s Disease • Is a progressive degenerative disease of the Basal Ganglia of the brain • Loss of neurons from the substantia nigra “black substance”
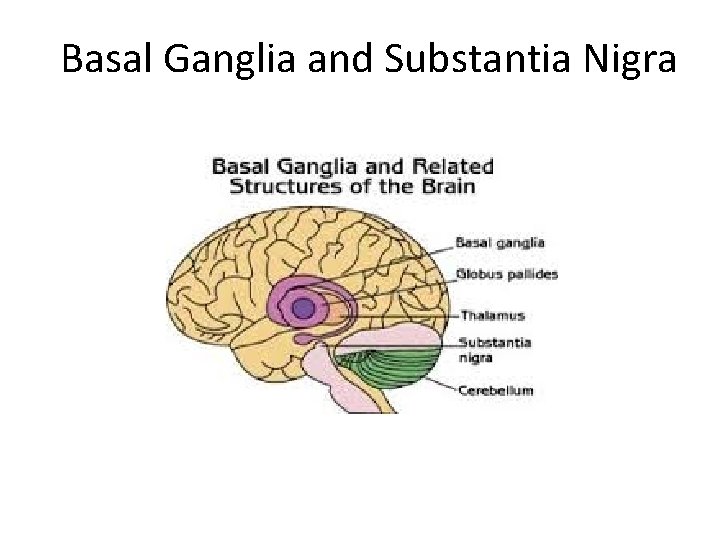
Basal Ganglia and Substantia Nigra
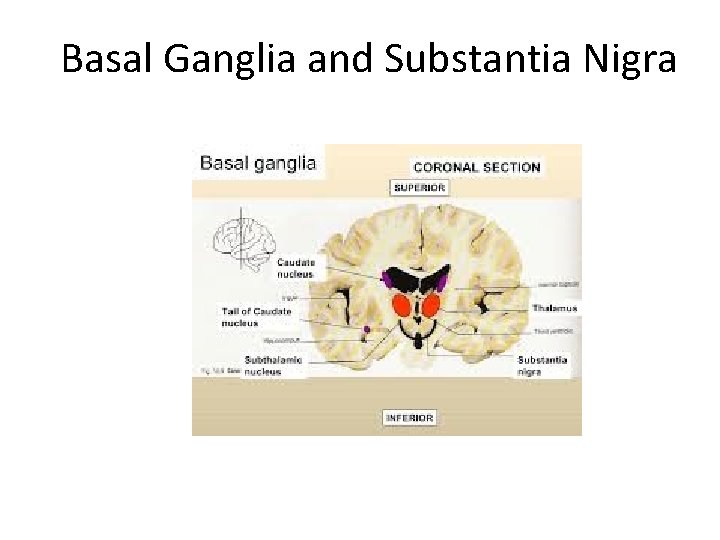
Basal Ganglia and Substantia Nigra

MPTP & Parkinsonism • In the 1980’s a rapidly progressive form of parkinsonism began to emerge in the youth • These healthy young people used a drug synthesized by an amateur chemist

MPTP & Parkinsonism • The chemist thought he was making MPPP, an analog of Meperidine (Demerol) a narcotic analgesic • What he actually made was MPTP, a brain poison

MPTP & Parkinsonism • Users of this “bathtub” Meperidine (Demerol) were poisoned with MPTP and developed a rapidly progressive form of Parkinsonism • These events led to MPTP as an animal model of Parkinsonism

MPTP & Parkinsonism • MPTP is converted by MAO into a toxin that is selectively taken up by the Substantia Nigra causing cell death

Drugs used to treat Parkinson’s • Increase Dopamine • Raise or block acetylcholine

Antiparkinsonian Drugs • Dopamine increasers: – MAOi – COMT inhibitors – Dopamine Precursors – Dopa-decarboxylase inhibitors – Dopa Agonists

Antiparkinsonian Drugs • Sinemet – Combination of • Carbidopa which blocks peripheral breakdown of… • Levodopa which is a precursor of dopamine Without Carbidopa, Levodopa would be broken down quickly in the blood and not enter the brain

Antiparkinsonian Drugs • Acetylcholine Increasers – Acetyl Cholinesterase Inhibitors • (Ach increased)

Antiparkinsonian Drugs • Acetyl Choline Blockers • -diphenhydramine (Benadryl) • -benztropine (Cogentin)

Psychosis • Mental illness that markedly interferes with a person’s capacity to meet life’s everyday demands • In a specific sense, it refers to a thought disorder in which reality is grossly impaired

Psychosis • • Alcohol and certain drugs can induce psychosis Bipolar disorder (manic depression) Brain tumors Epilepsy Depression with psychotic features Schizophrenia Dementia Stroke

Schizophrenia • Is a disease of the brain resulting in a thought disorder involving delusions, hallucinations and disorganized speech and behavior

Schizophrenia & Psychosis • Antipsychotic agents are used to treat schizophrenia, psychosis and other behavioral disturbances

Schizophrenia & Psychosis • Traditionally, antipsychotic drugs are called dopamine antagonists – D 2 blockers We now know that antipsychotic agents have mixed actions on dopamine and serotonin receptors

Antipsychotic Agents • Phenothiazine antipsychotics: – - Chlorpromazine (Thorazine) – - Thioridazine (Mellaril) – -Fluphenazine (Prolixin) – - Can be used IM

Antipsychotic Agents • Other older antipsychotics: – - haloperidol (Haldol)

Antipsychotic Agents • Newer antipsychotics: – - Clozapine (Clorzaril) – - Olanzapine (Zyprexa) – - Quetiapine (Seroquel) – - Risperidone (Risperdal)

Newer antipsychotics: • - aripiprazole (Abilify) • - mixed dopamine serotonin agonist/antagonist

Antipsychotic Toxicity • Because antipsychotic agents block dopamine… • Antipsychotic agents can cause parkinson’s like symptoms

Antipsychotic Toxicity • Antipsychotic agents can cause parkinsonian symptoms: – -Acute dystonic reactions
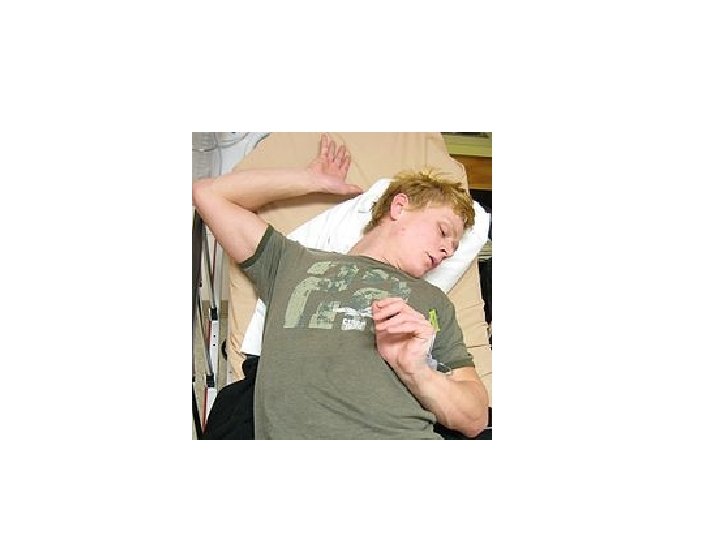

Antipsychotic Toxicity • Acute dystonic reactions • -treated with the same anticholinergics used in Parkinson’s – - diphenhydrazine (Benadryl) – - benztropine (Cogentin) – - DO NOT USE LEVODOPA

Antipsychotic Toxicity • Long term use of antipsychotic agents can cause parkinsonian symptoms:

Antipsychotic Toxicity • Tardive Dyskinesia • - mouth and tongue spasms (orolingual spasms) • - eyelid spasms (blepharospasm)


Tardive Dyskinesia

Treatment of Tardive Dyskinesia • -eliminate anticholinergic medications • - switch to newer antipsychotic • - benzodiazepines

Other unwanted antipsychotic effects • Sedation • Hypotension

Alzheimer’s Disease • A degenerative disease of the brain resulting in dementia • The disease is caused due to irreversible progressive deterioration of brain cells, especially the cerebral cortex and hippocampus

Alzheimer’s Disease • Loss of cognitive functions such as memory, movement coordination, pattern recognition, judgment and reasoning

Alzheimer’s • Acetyl cholinesterase inhibitors are used to slow the progression of Alzheimer’s - Donepezil (Aricept) - Rivastigmine (Exelon) - Galantamine (Razadyne)

Alzheimer’s • Depression – Antidepressants Behavioral problems - antipsychotics - benzodiazepines

Black Box Warning • Newer antipsychotic medications have Black Box warnings regarding their increased risk of death in elderly patients with dementia related psychosis


Endorphins & Opiate Receptors • Endorphins are naturally occuring brain peptides that regulate pain by acting upon specific receptors • Opiates derived from opium act upon these receptors

The opiate morphine • Morphine, the typical opioid agonist, has long been known to relieve pain with maximum efficacy

The opiate morphine • Morphine was purified from crude opium from poppy seeds • Named after Morpheus, the Greek God of dreams

Morphine • • • Analgesia Euphoria Sedation Respiratory Depression Cough Supression Pinpoint Pupils (Miosis) Nausea Vomiting Constipation Itching (Pruritus)

Strong opiate agonists • • • Morphine Hydromorphone Oxymorphone Heroin Methadone Fentanyl (Duragesic patch)

Mild to moderate opiate agonists • • Propoxyphene (Darvon, Darvocet) Codeine (Tylenol #3) Hydrocodone (Vicodin, Norco) Oxymorphone (Percocet, Oxycontin)

Opiate Antagonist • Nalaxone (Narcon) is used to block or reverse the effects of opiates • Nalaxone (Narcon) is used IV to block or reverse the effects of opiates • Effect is dramatic and within 1 -3 minutes • Short duration of action (1 -2 hours), may need to repeat

Addiction • Opiates • Benzodiazepines • Central acting sympathomimetics – Amphetamine – Cocaine Ethanol (Et. OH)

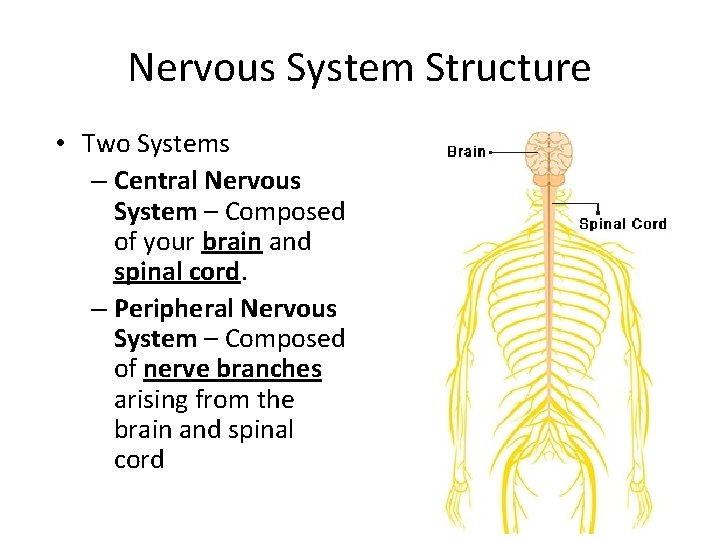
Nervous System Structure • Two Systems – Central Nervous System – Composed of your brain and spinal cord. – Peripheral Nervous System – Composed of nerve branches arising from the brain and spinal cord

Nervous System Function • The nervous system is a network of specialized cells, which coordinate the actions of an individual by sending signals from one part of the body to the other.

Vocabulary • Neurons – a nerve cell that transmit information throughout the body via the nervous system. • Synapse - is a small gap or junction between two neurons. • Neurotransmitters – chemical messengers that carry messages across the synapse.
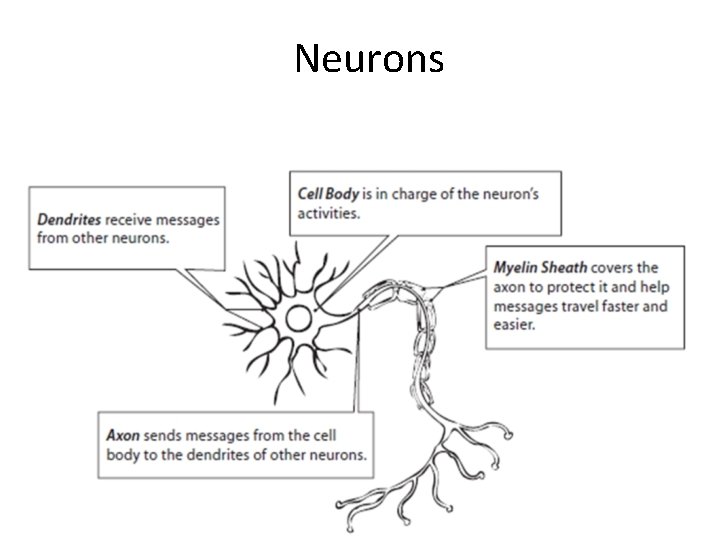
Neurons
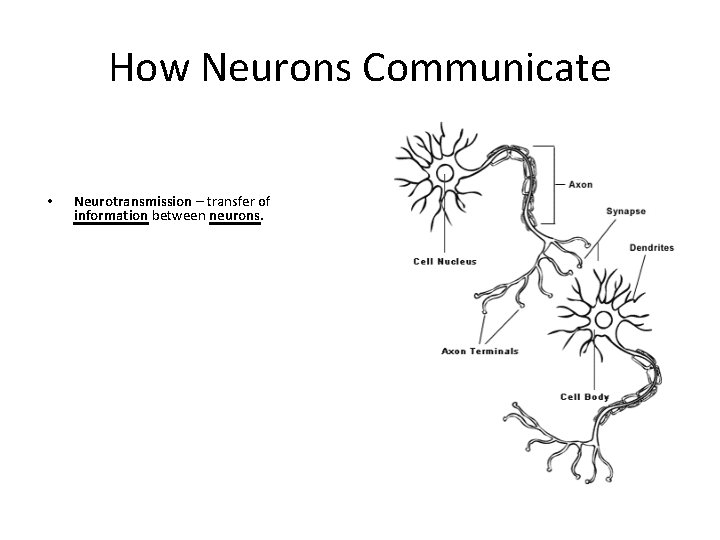
How Neurons Communicate • Neurotransmission – transfer of information between neurons.

Process of Neurotransmission 1. Brain generates an electrical impulse or action potential 2. Action potential signals neurotransmitters to move toward axon terminals 3. Neurotransmitters are released into synapse 4. Neurotransmitters bind to receptors on the dendrites 5. Process is repeated.
How Neurons Communicate

How Neurons Communicate • Neurotransmitters – what are they again? ? – Chemical messengers that carry messages across the synapse. – They either excite or inhibit neurons – Examples of neurotransmitters include • Dopamine • Serotonin • Norepinephrine

How Neurons Communicate Dopamine Controls voluntary movements of the body and is associated with the reward mechanism of the brain. Regulates the pleasurable emotions Serotonin Inhibitory neurotransmitter which has been found to have a significant effect on emotion, mood anxiety Norepinephrine Excitatory neurotransmitter and it regulates mood and both physical and mental arousal
- Slides: 155