Neuromuscular conditions Cerebral Palsy Prof Mohammed Zamzam Professor


Neuromuscular conditions Cerebral Palsy Prof. Mohammed Zamzam Professor & Consultant Pediatric Orthopedic Surgeon

Definition Non progressive, cerebral damage occurring before brain maturation (1 -2 years) resulting in muscle weakness, spasticity and other symptoms

Incidence 0. 5 -2/1000 in premature deliveries

Causes Ø Prenatal : Maternal disease/ Toxemia Cerebral deformity/ Hemorrhage Inborn error of metabolism Ø Perinatal : Labour/ Respiratory complications Perinatal infections

Causes Ø Postnatal : Infection Violence Convulsion

Classification Topographic Classification Ø Diplegia : (Arms & Legs much more in legs), most patients eventually walk Ø Tetraplegia : (Arms & Legs & Trunk) High mortality rate, most pts unable to walk. IQ is low

Classification Topographic Classification Ø Hemiplegia : Upper & lower limbs on one side (upper more than lower limbs), with spasticity, patients eventually walks Ø Bilateral Hemiplegia Ø Paraplegia (Legs) Ø Monoplegia Ø Triplegia

Classification Physiological Classification Spastic : Ø Commonest 50 -60% Ø Most important for the Orthopedic Surgeon Ø Increased muscle tone (Jack knife spasticity) Ø Slow restricted movements Ø Increased reflexes Ø Babinski +ve

Classification Physiological Classification Athetosis : Ø 20 -25% Ø ? Kernicterus Ø Involuntary, uncontrolled slow movement Ø Normal reflexes Ø +/- Muscle rigidity or tremors Ø NOT FOR SURGERY

Classification Physiological Classification Ataxia : Ø 1 -5% Ø Inability to control /coordinate movement when they start Ø Intention tremor Ø Nystagmus / unbalanced gait Ø NOT FOR SURGERY

Classification Physiological Classification Rigidity : Ø 5 -7 % Ø Lead pipe rigidity Mixed type : A combination of spasticity and athetosis with whole body involvement
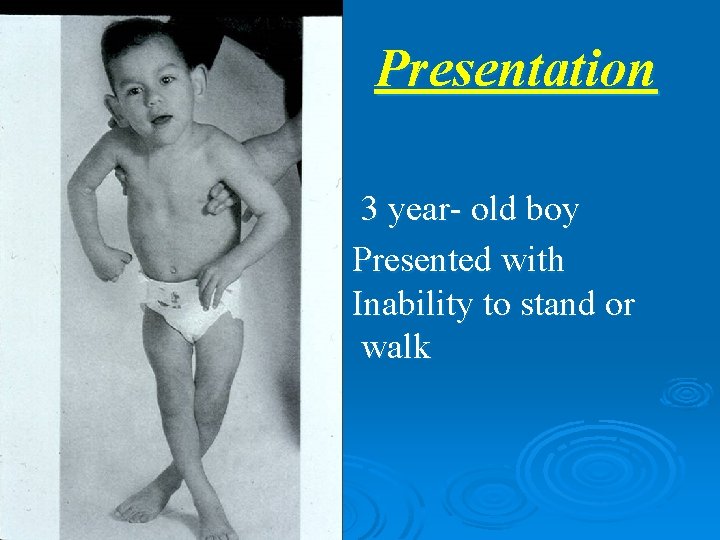
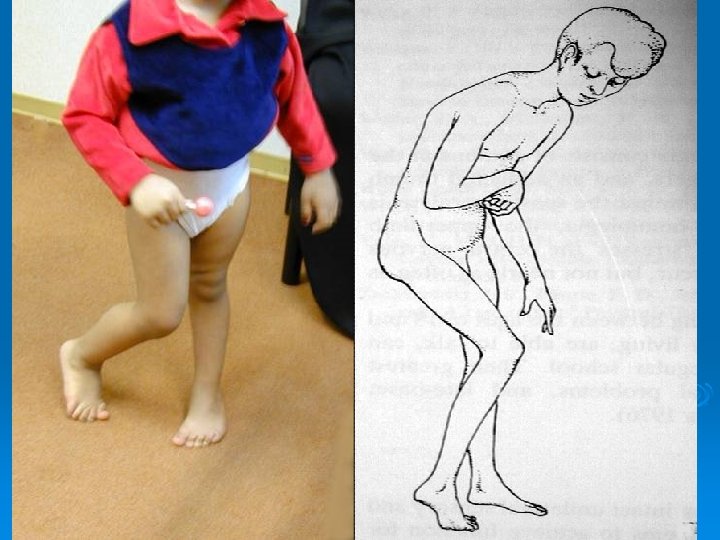
Presentation 3 year- old boy Presented with Inability to stand or walk
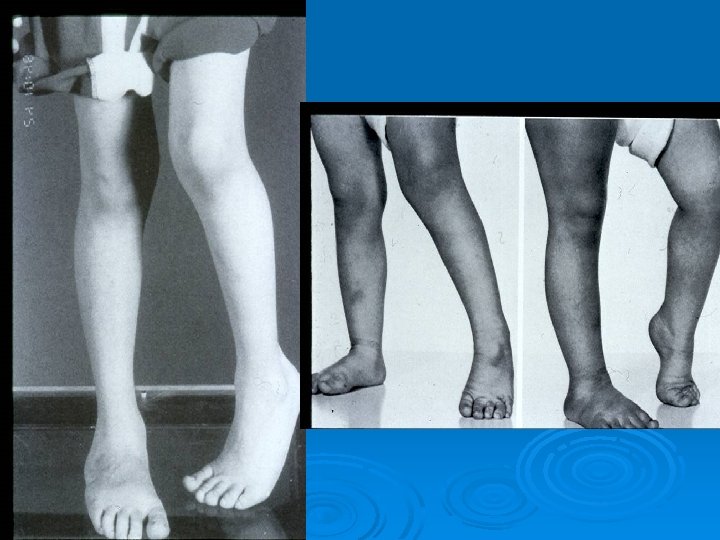

Deformities Upper limb : Ø Shoulder adduction/internal rotation Ø Elbow flexion Ø Forearm pronation Ø Wrist and fingers flexion

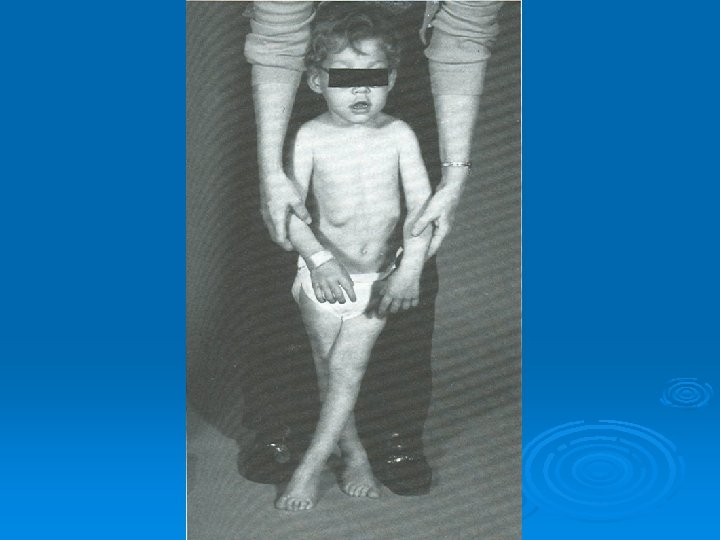
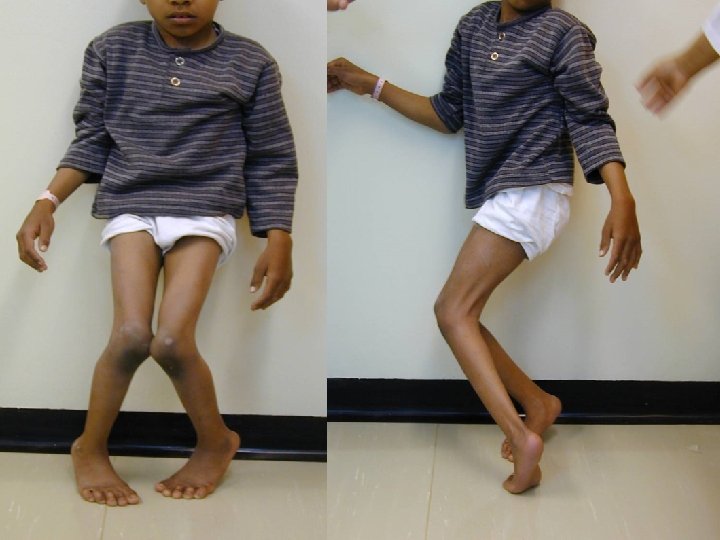
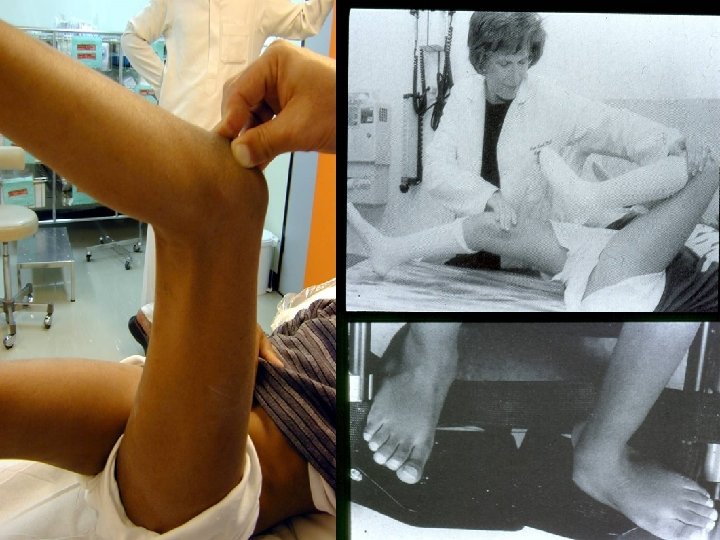
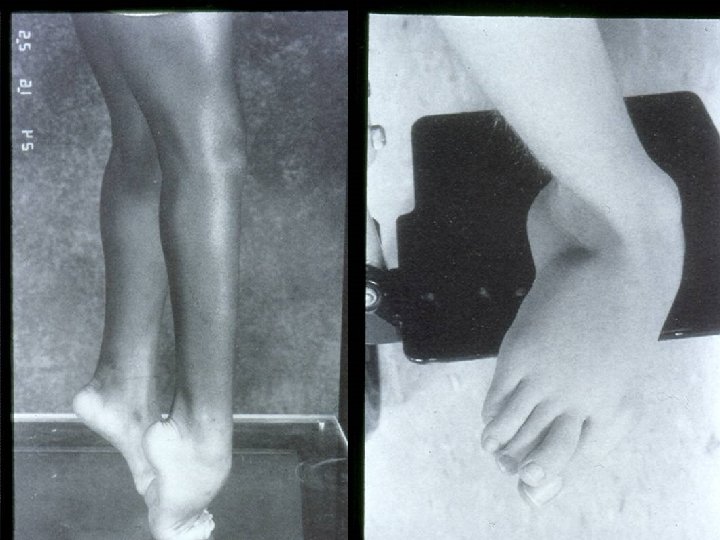
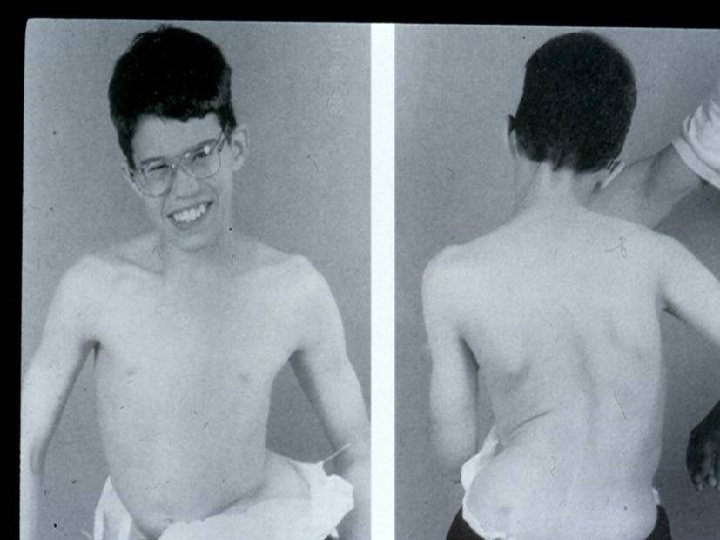
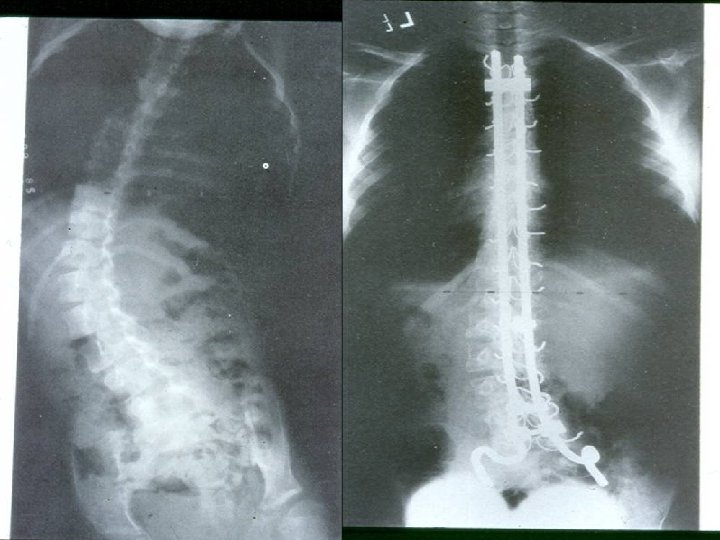
Deformities Lower limb : Ø Hip adduction/flexion/internal rotation Ø Knee flexion Ø Feet equinus / varus or valgus Ø Gait scissoring Spine : kyphoscoliosis
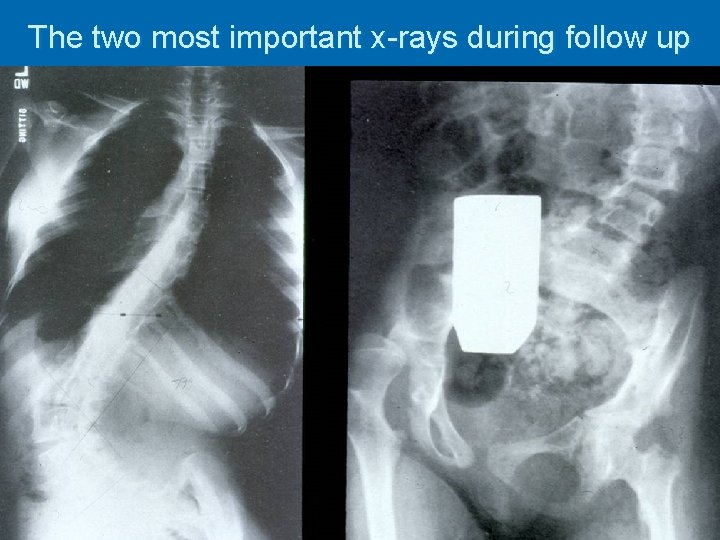
The two most important x-rays during follow up

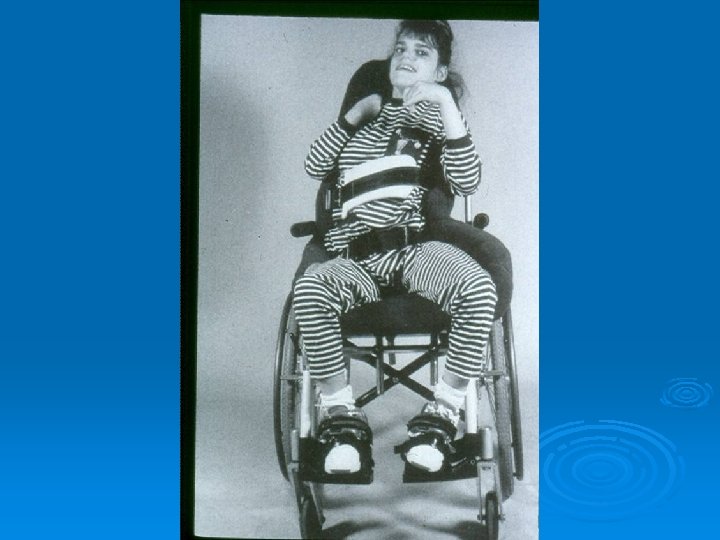
Management Aim of treatment : Ø AS INDEPENDENT AS POSSIBLE Ø Avoid pain (hip arthritis) Ø Maintain sitting posture Ø Maintain spinal stability Ø Social benefit
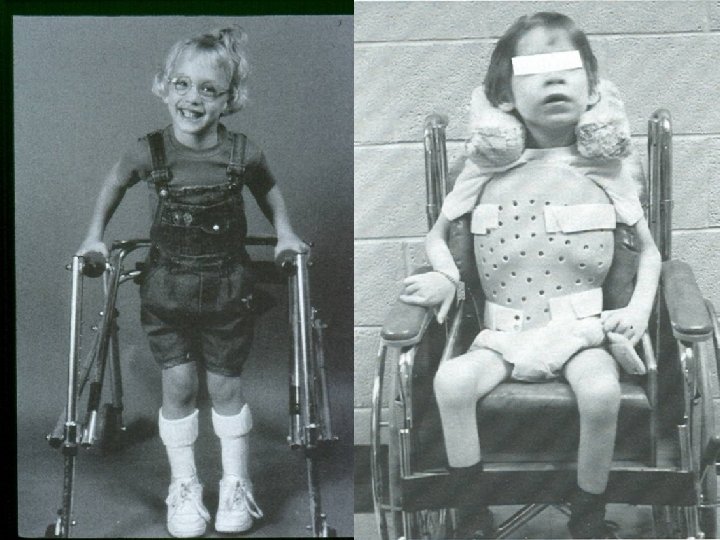

Management Multidisciplinary : Ø Ø Ø Orthotics before and after surgery Physiotherapy/Occupational therapy Orthopedic Surgery Neurosurgery/ Pediatric Neurology Speech therapy
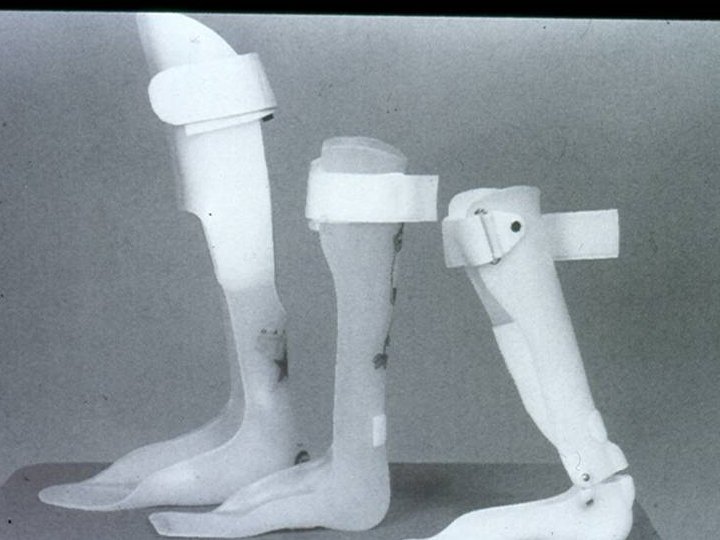

Management Ø History Ø Exam Ø Investigation Ø Treatment The degree of retardation is of great importance in treatment planning

Management Exercise : Ø Ø Ø Start early (1 st month) when suspected Qualified Physiotherapist/ PARENTS Prevent contractures Develop coordination Mental exercise Use Orthotics/POP/Casts if needed

Management Surgery : Ø Best in Spastic Hemiplegics and severe deformities Ø Contraindicated in Athetoid & Ataxic

Management Goal of Surgery : Ø Ø Ø Decrease spasm Release of contractures Correct deformities Rebalance muscles Stabilize flail joints

Management Options of Surgery : Ø Ø Ø Ø Neurectomy Tenoplasty Muscle lengthening (Recession) Tendon Transfer Bony surgery Osteotomy/Fusion Spinal surgery
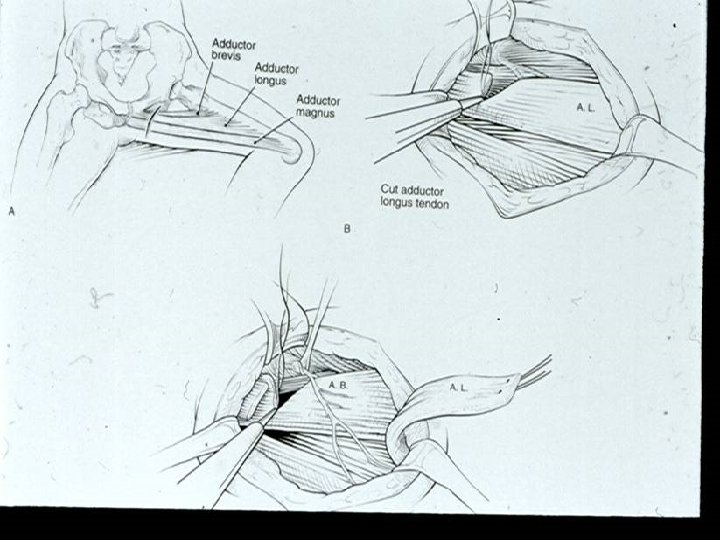
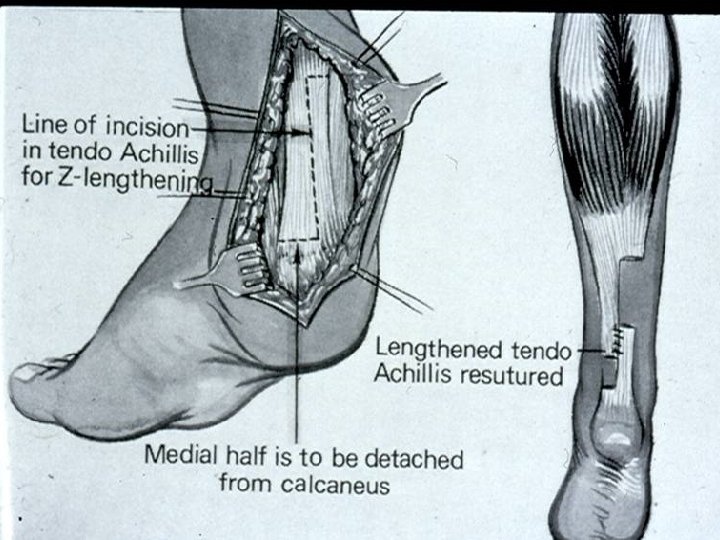
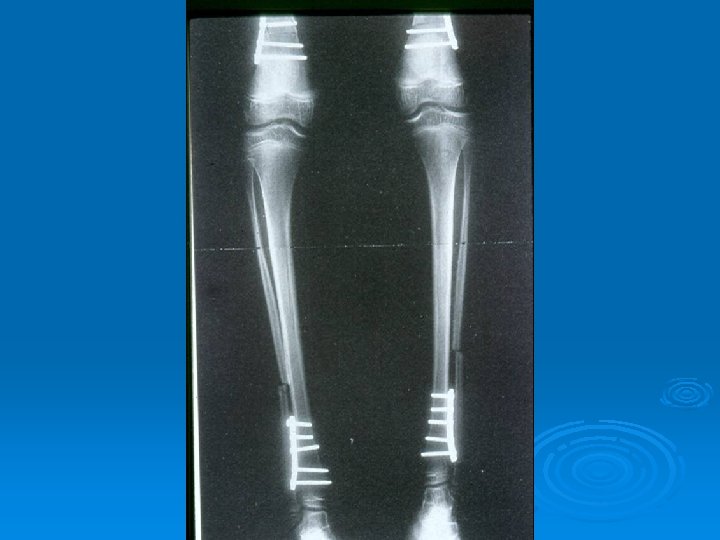
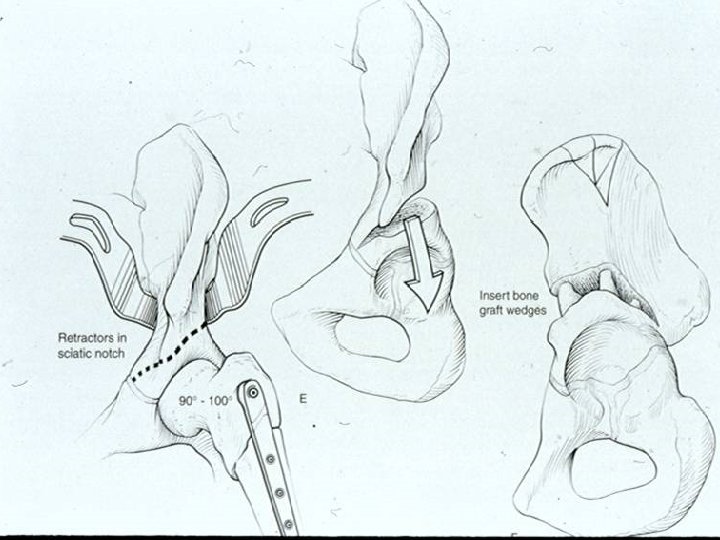
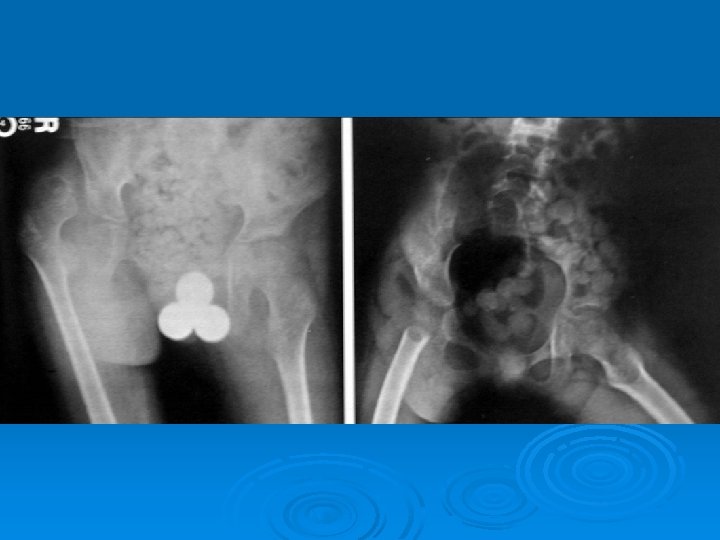

Management Intramuscular botulinum toxin: Ø Temporarily reduces dynamic spasticity Ø It is thought that its use promotes normal muscle growth and avoids the development of soft tissue contracture

- Slides: 41