Neurologic Complications of Immunization M R Ashrafi Professor

























- Slides: 33

Neurologic Complications of Immunization M. R Ashrafi Professor Of Pediatric Neurology Children’s Medical Center Tehran university Of Medical Sciences

Adverse Events Following Immunization / AEFI Vaccine Reaction Program Error Coincidental Injection Reaction Unknown

AEFI / Neurologic Complications Vaccine Reaction Hypotonic-Hyporesponsive Episode Persistent Crying Seizure Encephalopathy Paralytic poliomyelitis Guillaine-Barre Syndrome

Hypotonic-Hyporesponsive Episode Worrisome uncommon shock-like reaction to DTP Occurs within 24 hours with a mean interval of 12 hours Incidence of 0. 06 % of DPT-immunized infants Approximately one-half of infants are febrile The episode subsides in minutes to at most 4 hours Leaving no apparent residua

AEFI / Neurologic Complications Vaccine Reaction Persistent or high pitched crying of 1 hour or more was seen in 3. 5 % of DPT-immunized infants. Drowsiness was seen in approximately 32 -62 % of DPTimmunized infants. A transient increase in ICP , manifested by a bulging fontanel , has been encountered after DPT immunization.

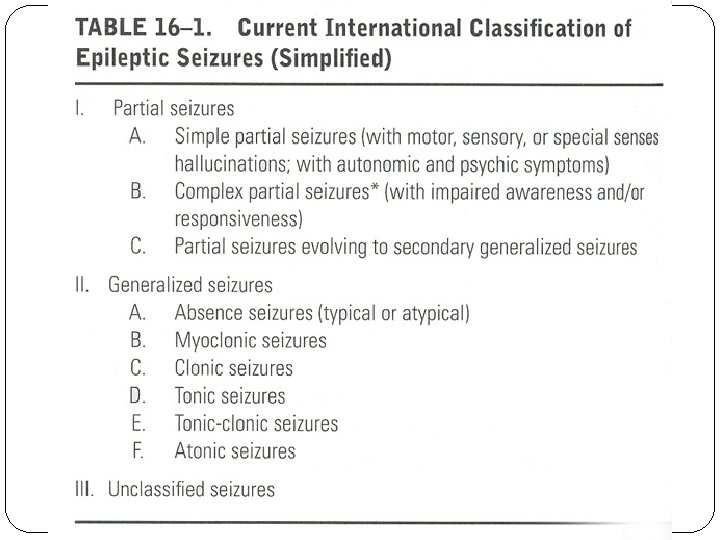
AEFI / Neurologic Complications Vaccine Reaction The use of whole-cell pertussis vaccine has been associated with febrile and afebrile seizures , which are generalized and typically occur within 72 hours after immunization. FS occur in 1 : 1750 immunization


Acute Encephalopathy Generalized febrile or nonfebrile convulsions , altered consciousness and serious neurologic or psychologic residua can occur within 72 hours of DPT immunization. Incidence of 1 : 165000 immunization The prognosis for survival is good Major neurologic residua in 77 % of cases such as MR and epilepsy.

Acute Encephalopathy Acute encephalopathy can follow immunization with measles or MMR vaccine. Occur between 2 – 15 days after immunization , and peak onset of encephalopathy on days 8 or 9. Seizures , altered behavior or consciousness and ataxia. Death or mental regression is common No cases of encephalopathy have been identified after administration of monovalent mumps or rubella vaccines.

AEFI / Neurologic Complications Vaccine Reaction Hypotonic-Hyporesponsive Episode Persistent Crying Seizure Encephalopathy Paralytic poliomyelitis Guillaine-Barre Syndrome

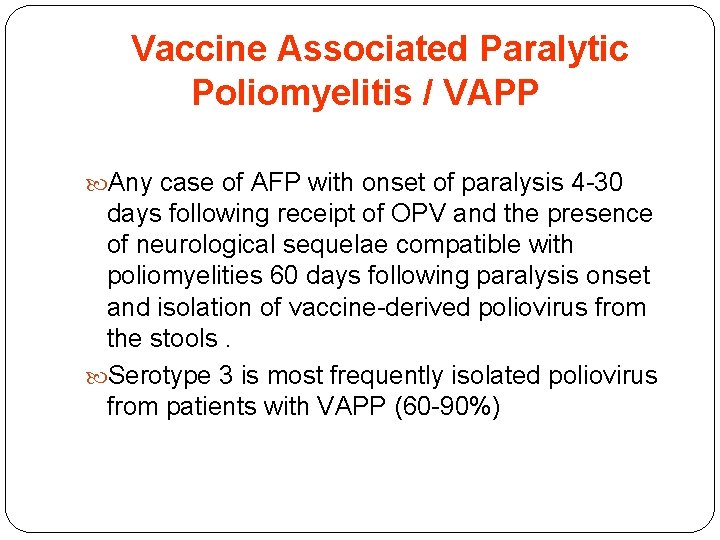
Vaccine Associated Paralytic Poliomyelitis / VAPP Any case of AFP with onset of paralysis 4 -30 days following receipt of OPV and the presence of neurological sequelae compatible with poliomyelities 60 days following paralysis onset and isolation of vaccine-derived poliovirus from the stools. Serotype 3 is most frequently isolated poliovirus from patients with VAPP (60 -90%)

The following criteria must be fulfilled before diagnosis of VAPP Paralysis should be clinically compatible with poliomyelitis (residual paralysis at 60 days ) Adequate stool negative for wild polio Ruled out other illnesses Evaluation by expert committee

Contact VAPP Known contact with a vaccinee that received OPV 7 -70 days before onset of paralysis of the patient and the contact between the patient and vaccinee should have occurred 4 -30 days before paralysis onset. Half of the cases of VAPP reported from America are among contacts of vaccinated children

VDPV (Vaccine-derived poliovirus ) Usually 1 -15% differences from parent OPV strains Classified as wild. Extensive period of virus excretion or transmission.

AEFI / Neurologic Complications Vaccine Reaction Hypotonic-Hyporesponsive Episode Persistent Crying Seizure Encephalopathy Paralytic poliomyelitis Guillaine-Barre Syndrome

GBS study group diagnostic criteria Required for diagnosis : üProgressive motor weakness involving more than one extremity üAreflexia or marked hyporeflexia

GBS study group diagnostic criteria §Strongly supportive of diagnosis : üInitial absence of fever üProgressive over days to a few weeks üOnset of recovery 2 -4 weeks after cessation of progression üRelatively symmetric weakness üMild sensory sign and symptoms üCranial nerve palsies üAutonomic dysfunction üElevation of CSF protein after one week of symptoms üSlowed NCV

GBS / Etiology üTwo-thirds of patients report an antecedent , acute infectious illness , most commonly a respiratory tract infection or gastroenteritis. üThe interval between the prodromal infection and the onset of GBS symptoms varies between 1 -3 weeks. üCMV is the most common viral trigger of GBS. üC. Jejuni is recognized as the most frequent antecedent pathogen for GBS.

Preceding Events q. Infection Campylobacter Jejuni Cytomegalovirus EBV / HIV / VZV / Lyme Disease q. Vaccination Rabies / Swine Flu / Tetanus / OPV / Meningococcus q. Neoplasia Lymphoma / Hodgkin Disease q. Drug Captopril / Danazole / Penicillamine /Amitriptyline Heavy metals / Nitrofurantoin / Hydralazine

Adverse Events Following Immunization / AEFI Vaccine Reaction Program Error Coincidental Injection Reaction Unknown

AEFI / Neurologic Complications injection Reaction / Faint Syncope is defined as a sudden loss of consciousness and postural tone , because of transient cerebral hypoperfusion , followed by spontaneous recovery. Syncope is rare in childhood and more common in adolescence particularly in girls. Syncope is seen in about 15 % of individuals under the age of 18 years. 30 to 50 % of children have at least one episode of syncope by adolescence. Vasovagal (75 % ) Reflex Decreased venous return Cardiac

Syncope & Faint q. Vasovagal ( Neurocardiogenic Syncope ) Triggered by pain & emotional upset. q. Reflex Hyperventilation , violent coughing , hot bath , defecation and micturition. q. Reduced venous return Valsalva maneuver q. Cardiac syncope §Cardiac asystole ( Stokes-Adams Syndrome) §Arrhythmia §Left ventricular outflow obstruction §Anemia §Prolonged QT interval : Romano-Ward syndrome ( AD) Jervell-Lange-Nielsen Syndrome ( AR )

Syncope & Faint q. Prodromal phase or presyncope §Light-headedness , blurred vision , epigastric discomfort , nausea , pallor , diaphoresis. q. Loss of consciousness §Is usually brief ( few seconds to 1 -2 minutes ) followed by rapid spontaneous recovery without persistent neurologic deficits. §In 40 % of cases syncopal attacks are accompanied by a convulsion. ( usually tonic spasm , less often clonic or TC ) q. Postictal period §May be accompanied by nausea , pallor and diaphoresis.

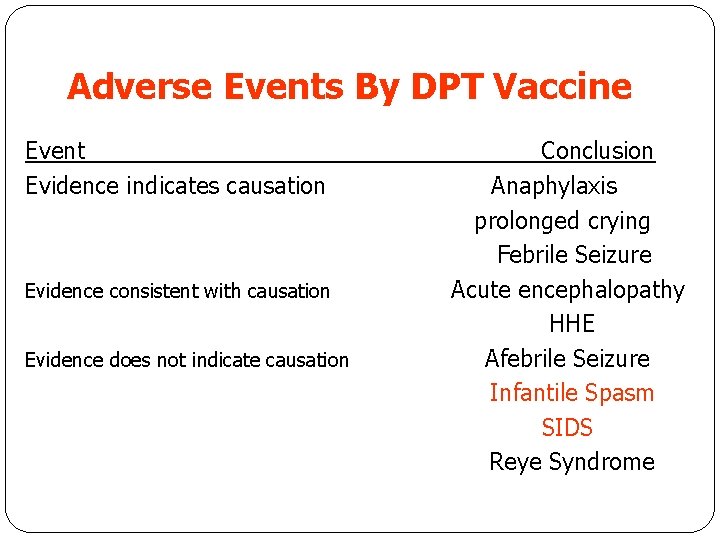
Adverse Events By DPT Vaccine Event Evidence indicates causation Evidence consistent with causation Evidence does not indicate causation Conclusion Anaphylaxis prolonged crying Febrile Seizure Acute encephalopathy HHE Afebrile Seizure Infantile Spasm SIDS Reye Syndrome

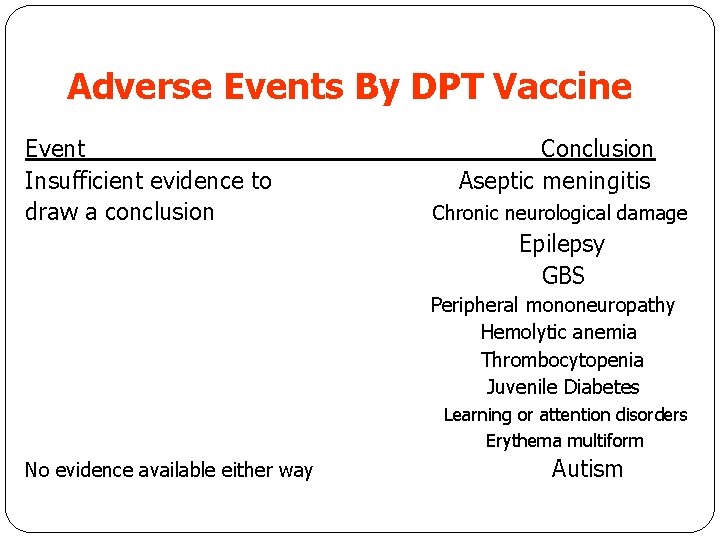
Adverse Events By DPT Vaccine Event Insufficient evidence to draw a conclusion Conclusion Aseptic meningitis Chronic neurological damage Epilepsy GBS Peripheral mononeuropathy Hemolytic anemia Thrombocytopenia Juvenile Diabetes Learning or attention disorders Erythema multiform No evidence available either way Autism

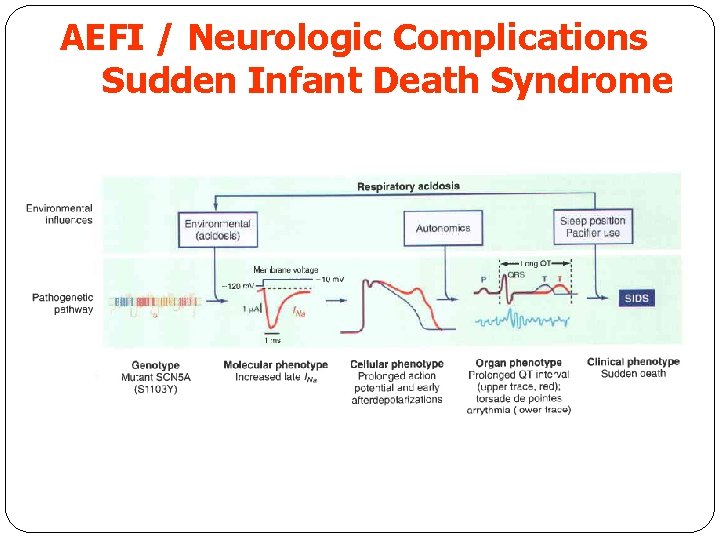
AEFI / Neurologic Complications Sudden Infant Death Syndrome SIDS is defined as the sudden death of an infant that is unexpected by history and unexplained by a thorough postmortem examination , which include a complete autopsy , investigation of the scene of death , and review of the medical history. Infants are at greatest risk of SIDS at 2 -4 months of age , with most deaths having occurred by 6 months. Male infants are 30 -50 % more likely to be affected than females. The actual risk for SIDS in individual infants is determined by complex interactions between genetic and environmental risk factors.

AEFI / Neurologic Complications Sudden Infant Death Syndrome

AEFI / Neurologic Complications Sudden Infant Death Syndrome No association between immunization and SIDS has been found.


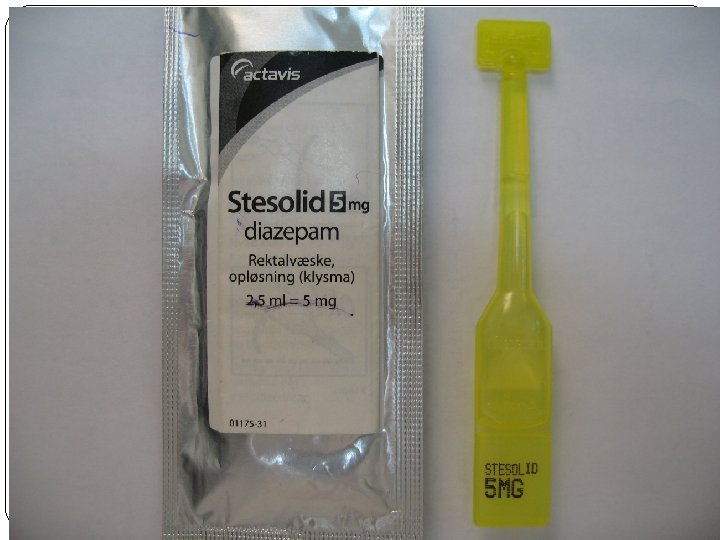
§Diazepam IV / PR / IO üIV : 0. 1 to 0. 3 mg/kg /dose every 10 -15 min üPR : 0. 2 to 0. 5 mg/kg/dose üMaximum dose of DZP is 10 -20 mg/dose. üDZP should be administered at a rate of 1 -2 mg/min. üDZP stops seizure within 5 to 10 min in 80 % of status. üMedian time to stop seizure : 2 min üPeak effect : 1 to 5 min üDuration of action : 20 to 30 min üA longer acting AED should be given if DZP successfully stops the status.

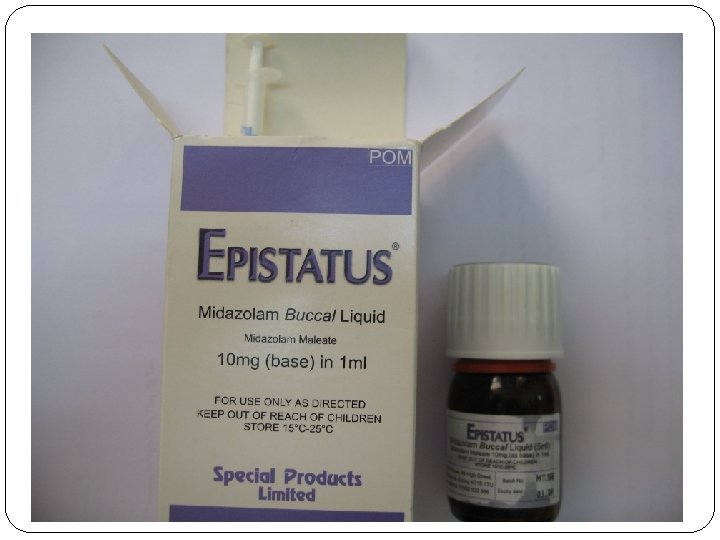
§Rectal Diazepam üRectal diazepam is an effective and safe treatment for prolonged seizures outside the hospital. üIt achieves blood levels adequate for seizure treatment more rapidly than any route except for IV one. üIt has FDA approval for acute repetitive seizures but not for Status. üReports mention its successful use in status. • Buccal and intranasal midazolam are other treatment options.

