NEURODEVELOPMENTAL DISABILITIES AND THE TRANSITION FROM PEDIATRIC TO

NEURODEVELOPMENTAL DISABILITIES AND THE TRANSITION FROM PEDIATRIC TO ADULT HEALTHCARE Diana M. Cejas, M. D. , M. P. H. Assistant Professor of Neurology

OBJECTIVES By the end of this presentation, you’ll be able to… 1. Describe the process of transitioning from pediatric to adult healthcare services 2. List the components of a transition plan 3. Start a conversation about transition to adult care

TRANSITIONING TO ADULTHOOD • Moving from adolescence to adulthood affects every aspect of life • Home / Community • Educational System • Healthcare System • This is a process, not a single event! • Can be complicated for children with special healthcare needs

WHAT IS HEALTHCARE TRANSITION? • “The planned movement of adolescents and young adults with chronic physical and medical conditions from a childcentered to an adult-oriented health care system”

GOALS OF TRANSITION 1. To improve the ability of youth to manage their own health care and effectively use health services 2. To ensure an organized process to facilitate transition preparation, transfer of care, and integration into adult care

WHY IS THIS IMPORTANT? • Children with complex conditions are living into adulthood • Inadequate, unplanned, or incomplete transition can illness and gaps in care • Patients may not return until they are in crisis

WHO’S WHO IN TRANSITION? • Who’s Involved? • Who Else? • Patients • Patient / Family Advocates • Parents / Caregivers • Educational Specialists • Primary Care Providers • Psychologists • Medical Specialists • Allied Health Professionals • And more!

SIX CORE ELEMENTS • The six components of health care transition support are…

SIX CORE ELEMENTS 1. Transition Policy • A written description of a practice’s approach 2. Transition Tracking and Monitoring • A process for identifying youth and monitoring them 3. Transition Readiness • Regular assessment of youth readiness to transition

SIX CORE ELEMENTS 4. Transition Planning • An individualized plan 5. Transfer of Care • Performed when an appropriate provider has been found 6. Transfer Completion • Confirmed after patient has been integrated into adult practice

DEVELOPING A TRANSITION POLICY • Describe the process • Explain when planning begins • Describe everyone’s role • Solicit provider, staff, patient, and family input

SAMPLE TRANSITION POLICY

TRANSITION TRACKING • A practice – specific process for identifying and monitoring youth • Standardized tools can streamline the process

SAMPLE WORKSHEET

READINESS ASSESSMENTS • Help identify patient needs and clarify goals • Assessments should be done annually • Standardized tools are available • All have separate versions for patients and parents / caregivers

SAMPLE READINESS ASSESSMENT

MAKING A TRANSITION PLAN • Goals of planning: 1. To prepare the youth to manage their own care 2. To empower youth to function independently in the adult healthcare system 3. To identify appropriate adult healthcare providers 4. To communicate with accepting providers

PLAN COMPONENTS • Comprehensive Medical Summary • Transition Timeline • Patient’s Understanding of their Diagnosis • Labs, Imaging, and Other Interventions to be Done Prior to Transfer • Patient’s Self-Management Skills • Readiness Assessments • Emergency Plans / Action Plans • Advanced Care Plans • Patient / Family Preferences and Goals of Care • Information about Guardianship / Medical Decision-Making

SAMPLE TRANSITION PLAN
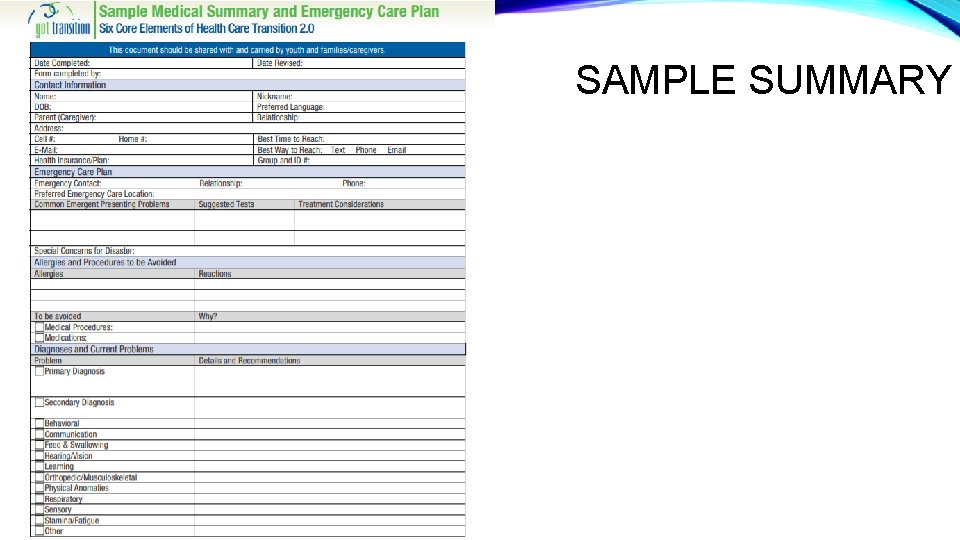

SAMPLE SUMMARY

WHAT SHOULD YOU TALK ABOUT? • The Youth’s Medical Condition(s) • Current Medications, Treatment Plans, and Side Effects • Troubling Symptoms • Mental Health and Wellness

TALKING TOPICS, CONTINUED • Puberty • Sexuality and Reproductive Issues • Genetic Counseling

TALKING TOPICS, CONTINUED • Substance Use • Housing • Driving • Medical Decision-Making • Employment • School

GUARDIANSHIP • A legal relationship where one individual is given the authority to make decisions on behalf of another individual who is no longer able to make / communicate decisions on their own • Not every person with ID needs guardianship!

TYPES OF GUARDIANSHIP • Person • Estate • General • Limited • Interim

GUARDIANSHIP ALTERNATIVES • Informal Support • Representative Payees • Supported Decision-Making • Power of Attorney • Foster Care 18 -21 • Healthcare Power of Attorney • Special Bank Accounts • Advance Directives • Living Trusts • Living Wills • Special Needs Trusts

THINGS TO REMEMBER • Patients with ID should not be excluded from transition planning! • Their goals and ideas should be included in the plan • Many patients with ID can develop health-management skills

ADOLESCENT VISITS • Adolescents should spend one-on-one time with their provider • Encourages them to take responsibility • Allows them to talk about sensitive topics • Allows providers to find out about goals

THE TRANSFER • Eventually, it will be time to transfer! • Gather documents and send them to the new provider • The transfer is not the end of transition! • Patients need close monitoring as they adapt

SAMPLE LETTER
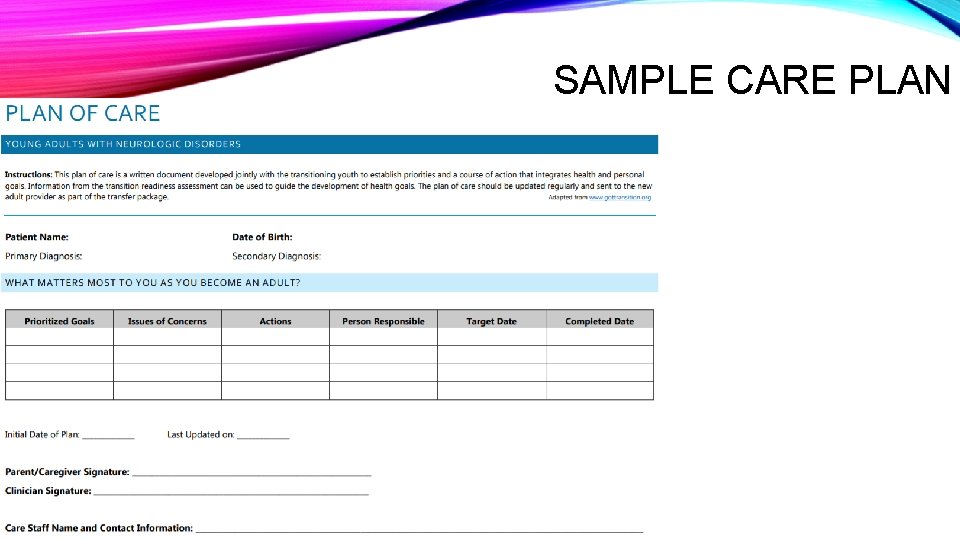
SAMPLE CARE PLAN

WHAT IF YOU CAN’T FIND AN ADULT PROVIDER? • Continue to search for an adult provider • Pediatrics continues to care for the patient • Specialty providers may continue on as a consultant
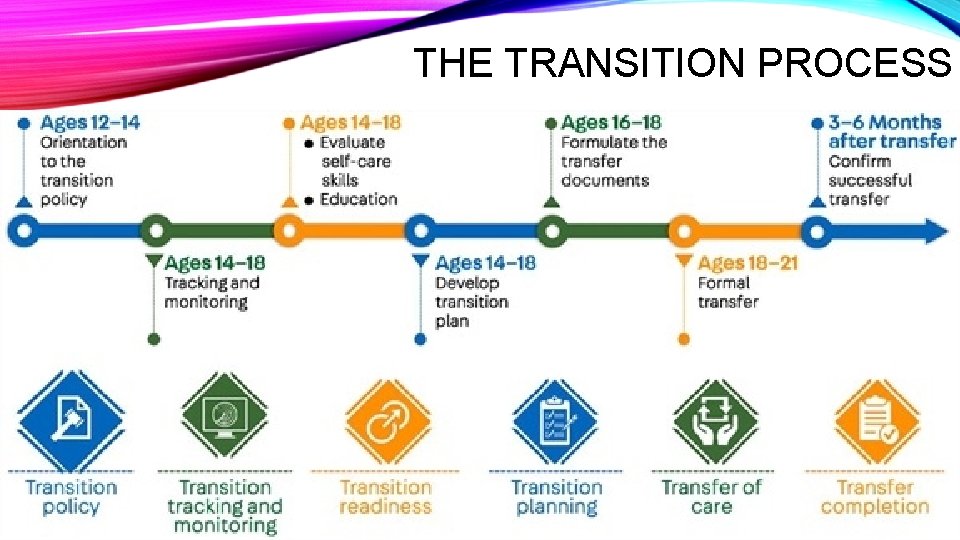
THE TRANSITION PROCESS

MORE THINGS TO REMEMBER • Talk about transition early and yearly! • Allow youth to start assuming some responsibility early • Start planning early!
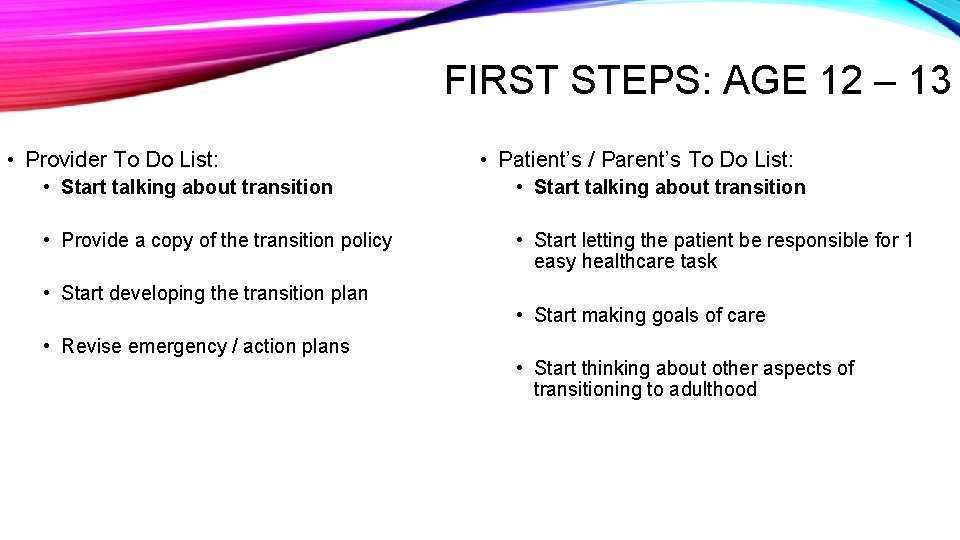
FIRST STEPS: AGE 12 – 13 • Provider To Do List: • Patient’s / Parent’s To Do List: • Start talking about transition • Provide a copy of the transition policy • Start letting the patient be responsible for 1 easy healthcare task • Start developing the transition plan • Revise emergency / action plans • Start making goals of care • Start thinking about other aspects of transitioning to adulthood

TALKING TOPICS AT 12 – 13 • Transition Process • Self-Advocacy Skills • Why Transition is Important • Getting Ready for High School • Adolescent Exam • Special Education Issues • Youth’s Health (and What They • Puberty Know About It)

TO DO AT 14 • Provider • Patient / Parents • Ask about guardianship • Look into guardianship and alternatives • Ask about post-high school plans • Ask for psychological testing • Review and revise the transition plan • Get ready for driving early • Give first readiness assessments • Allow the patient to take on more responsibilities • Update emergency plans • Start thinking about their new roles

TALKING TOPICS AT 14 • Puberty • Healthy Relationships • Legal Issues and Guardianship • Life After High School

TO DO AT 15 – 17 • Providers • Patient / Parent • Identify an appropriate adult provider • Look into adult providers • Review and revise the transition plan • Gather the patient’s health records • Repeat readiness assessments • Continue working on post-high school plans • Update emergency plans • Allow the patient to take on more responsibility • Develop the transition packet • Start coordinating the transfer

TALKING TOPICS AT 15 – 17 • Healthy Relationships • Emergency plans • Legal Issues • Advanced directives / medical power of attorney / living wills • Guardianship • Life After High School

AGES 18 AND UP • Transitioning starts • Providers communicate before and after transfer • The youth may want a final visit with their pediatric provider

CASE STUDY • Emmie is a 13 year old girl with tuberous sclerosis, drug-resistant epilepsy, and autism spectrum disorder with intellectual disability • Emmie’s healthcare providers: primary care, neurologist, psychiatrist, psychologist, OT, SLP • First visit • Practice transition policy reviewed • Overview of the transition process discussed • Transition team leader identified • Seizure action plan / emergency plan updated

EMMIE’S TRANSITION • Age 13 – 14 = initial plan made • Transition and emergency plans reviewed yearly • Readiness assessments done yearly • Age 15 – 16 = other planning • Post-high school planning at school • Guardianship process started

EMMIE’S TRANSITION • Age 17 = adult providers identified • Age 18 = first transfers begin • Age 19 – 21 = fully integrated into new clinics

CASE STUDY 2 • Jack is a 17 year old boy with drug-resistant epilepsy and intellectual disability • Jack’s healthcare providers: primary care, neurologist • Visit • Notification of physician retirement • Referred to adult epilepsy clinic • Seizure action plan updated

JACK’S TRANSITION • Age 17 = Referred to adult epilepsy clinic • Adult clinic 3 hours away • Adult clinic didn’t take Jack’s insurance • Age 18 = Looking for new insurance • Several missed appointments with adult epilepsy • Placed on no-show list

JACK’S TRANSITION • Age 19 = found local neurologist • Neurologist unfamiliar with Jack’s condition • Age 20 = transported to local ED in status epilepticus • Transferred to adult tertiary care hospital

HOW COULD PLANNING HAVE HELPED? • Identify barriers to accessing care before problems arise • Identify appropriate providers • Help patients make a safety net • Help Mom get started with the guardianship process

LAST THOUGHTS • A well organized process can help make things easier for patients, parents / caregivers, and providers

Questions?

Thank You!

REFERENCE • Acuña Mora M, Moons P, Sparud-Lundin C, Bratt E-L, Goossens E. Assessing the level of evidence on transfer and transition in young people with chronic conditions: protocol of a scoping review. Syst Rev. 2016; 5(1): 166. doi: 10. 1186/s 13643 -016 -0344 -z. • American Academy of Pediatrics, A. A. of, American Academy of Family Physicians, American College of Physicians, Transitions Clinical Report Authoring Group, Cooley, W. C. , & Sagerman, P. J. (2011). Supporting the Health Care Transition From Adolescence to Adulthood in the Medical Home. PEDIATRICS, 128(1), 182– 200. https: //doi. org/10. 1542/peds. 2011 -0969 • American College of Physicians. (2016). HVC Pediatric to Adult Care Transition Intellectual Disabilities/Developmental Disabilities (ID/DD). Retrieved from https: //www. acponline. org/system/files/documents/clinical_information/high_value_care/clinician_resources/pediatric_adult_care_transitions/gim_dd/idd_transitions_tools. pdf • Brown, L. W. , Camfield, P. , Capers, M. , Cascino, G. , Ciccarelli, M. , De Gusmao, C. M. , … Zupanc, M. (2016). The neurologist’s role in supporting transition to adult health care. Neurology, 87(8), 835– 840. https: //doi. org/10. 1212/WNL. 0000002965 • Center for Health Care Transition Improvement. (2014). Six Core Elements of Health Care Transition 2. 0. Retrieved from www. Got. Transition. org • Child Neurology Foundation. Transition of Care. Retrieved October 20, 2018, from http: //www. childneurologyfoundation. org/transitions/ • Dressler PB, Nguyen TK, Moody EJ, Friedman SL, Pickler L. Use of transition resources by primary care providers for youth with intellectual and developmental disabilities. Intellect Dev Disabil. 2018; 56(1): 56 -68. doi: 10. 1352/1934 -9556 -56. 1. 56. • Hagan JF, Shaw JS, Duncan PM, eds. 2008. Bright Futures: Guidelines for Health Supervision of Infants, Children, and Adolescents. Third Edition. Elk Grove Village, IL: American Academy of Pediatrics. • Oskoui M. Study on the Transition of Adolescents with Neurological Disorders ( STAND ). 2010; (November). http: //digitool. library. mcgill. ca/webclient/Stream. Gate? folder_id=0&dvs=1513635568283~852. Accessed December 18, 2017 • Teenagers with mental disability lack reproductive education and knowledge; still, many have had sex. (2003). Perspectives on Sexual and Reproductive Health, 35(4), April 2, 2014. • Tilton, A. H. , & De Gusmao, C. M. (2018, February). Transition from Pediatric to Adult Neurologic Care. CONTINUUM Lifelong Learning in Neurology. https: //doi. org/10. 1212/CON. 0000000570 • Wiegerink, D. , Roebroeck, M. , Bender, J. , Stam, H. , & Cohen-Kettenis, P. (2011). Sexuality of young adults with cerebral palsy: Experienced limitations and needs. Sexuality & Disability, 29(2), 119 -128. doi: 10. 1007/s 11195 -010 -9180 -6
- Slides: 52