Neuro ICU Nurse Practitioner Conference Morbidity and Mortality

Neuro. ICU Nurse Practitioner Conference Morbidity and Mortality

Identifying Information Mrs. D is a 30 year old woman with a 1 year history of worsening headaches and visual field defects. MRI showed large cystic lesion extending from suprasellar region to the ventricles, with rim enhancing multiloculated tumor in hypothalamus. Now DOS s/p resection. Uneventful surgical course except for bradycardia during traction on the carotid, and slow emergence necessitating narcan.

History PAST MEDICAL HISTORY Hypertension Craniopharyngioma PAST SURGICAL HISTORY C-Section 2003 Tubal ligation 2004

Physical Findings Immediately Post-Op NEURO: Sleepy but arousable. AOx 3. f/cx 4 with 5/5 strengths. No pronator drift. Still with visual field defect. GCS 14 (E 3 V 5 M 6) HEAD: normocephalic, atraumatic EYES: PERRLA, conjunctiva clear, sclerae anicteric , briskly reactive pupils 2 -3 mm Bil NECK: trachea is midline and without any JVD RESPIRATORY: CTA bilaterally, moving air well, breath sounds symmetric CARDIOVASCULAR: RRR, normal S 1 & S 2, no MRG GI: soft, ND, normal bowel sounds, and non tender EXTREMITIES: adequate distal perfusion SKIN: Intact , Warm, Dry

Physical Findings 9 Hours Post-Op NEURO - Lethargic, without any eye opening to stimulation. Grunts to deep sternal rub. Does not follow commands x 4 but briskly localizes. Pupils are unequal but briskly reactive, 4 mm on the left and 2 mm on the right, but GCS 8 (E 1 V 2 M 5) HEAD: normocephalic, atraumatic EYES: PERRLA, conjunctiva clear, sclerae anicteric Briskly reactive pupils 2 -3 mm Bil NECK: trachea is midline and without any JVD RESPIRATORY: CTA bilaterally, moving air well, breath sounds symmetric CARDIOVASCULAR: RRR, normal S 1 & S 2, no MRG GI: soft, ND, normal bowel sounds, and non tender EXTREMITIES: adequate distal perfusion SKIN: Intact , Warm, Dry
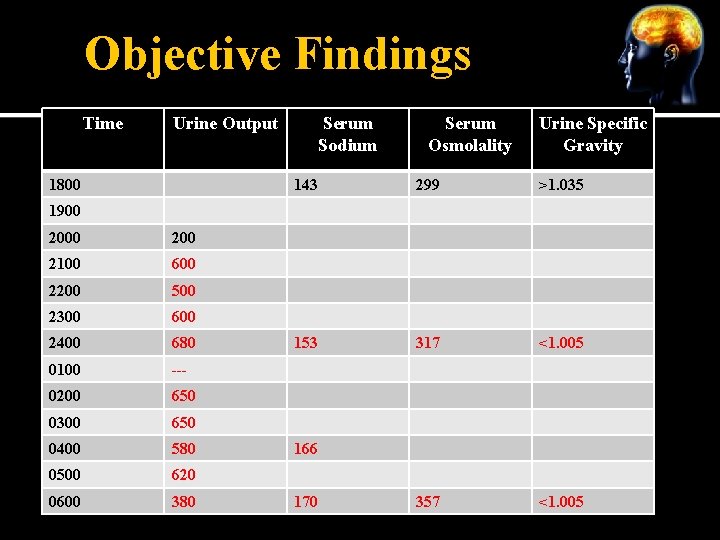
Objective Findings Time Urine Output 1800 Serum Sodium Serum Osmolality Urine Specific Gravity 143 299 >1. 035 153 317 <1. 005 357 <1. 005 1900 200 2100 600 2200 500 2300 600 2400 680 0100 --- 0200 650 0300 650 0400 580 0500 620 0600 380 166 170
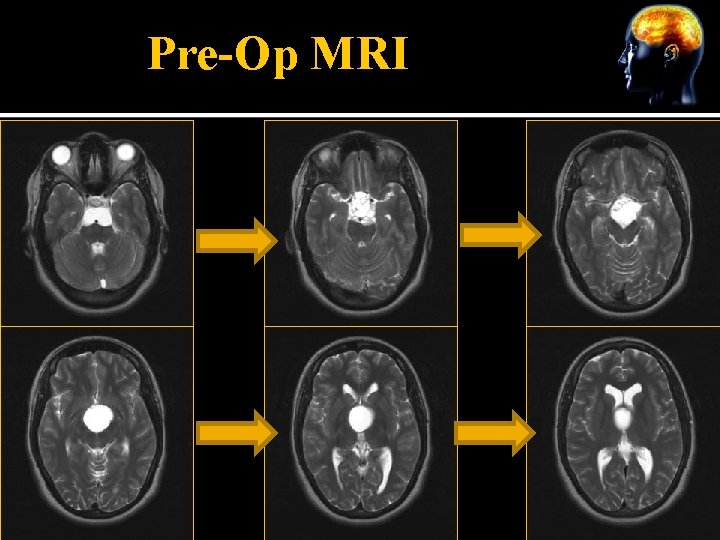
Pre-Op MRI
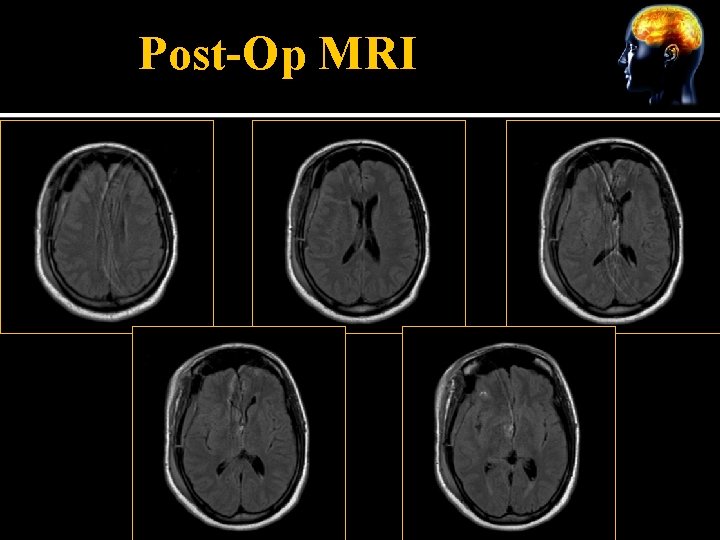
Post-Op MRI

Hospital Course Typical hospital course 1 -2 days in the ICU If no DI can be transferred to the floor and home in another day or two If develop DI longer stay in the ICU Patient’s hospital course has been prolonged to an 11 day hospital stay

Complications Severe hypernatremia dehydration 10 L free water deficit Altered level of consciousness High risk for seizures
Pathophysiology

Craniopharyngiomas 2. 5 -4% of all brain tumors 80 -90% of neoplasms arising in the pituitary region Tend to arise from anterior superior margin of the pituitary Some may arise primarily from the 3 rd ventricle Almost all have solid or cystic components Are not malignant but due to difficulty in curing they are considered “malignant in behavior” Neurological disturbances, such as headache and visual field defects are initial findings
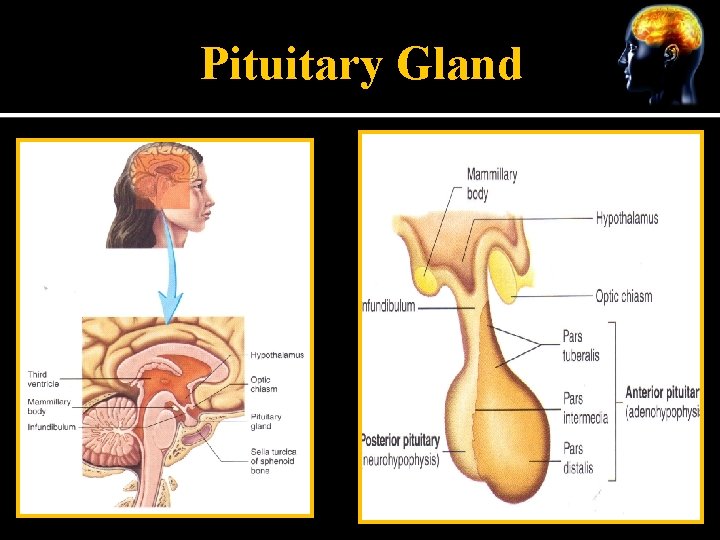
Pituitary Gland

Diabetes Insipidus CENTRAL /NEUROGENIC Decrease in production of antidiuretic hormone (ADH) or brain edema causes blockage in the pathway from the hypothalamus to the posterior pituitary NEPHROGENIC Decrease in the responsiveness of the renal tubule to ADH

Causes of Nephrogenic DI Familial X-linked trait Pyelonephritis Renal amyloidosis Myeloma Potassium depletion Sickle cell anemia Chronic hypercalcemia Sjogren syndrome Radiocontrast dye Drugs Lithium Demeclocycline Amphotericin B Aminoglycosides Cisplantin Rifampin

Causes of Central DI PRIMARY Familial (dominant trait) Wolfram Syndrome DIDMOAD SECONDARY TSH Craniopharyngioma Brain Death Tumors Other mass lesions pressing on the hypothalamus – A-comm aneurysms Head injury Primarily basal skull fractures Encephalitis and meningitis Drug induced Ethanol and Dilantin inhibit ADH release

Patterns of Central DI Transient DI Prolonged Triphasic DI response
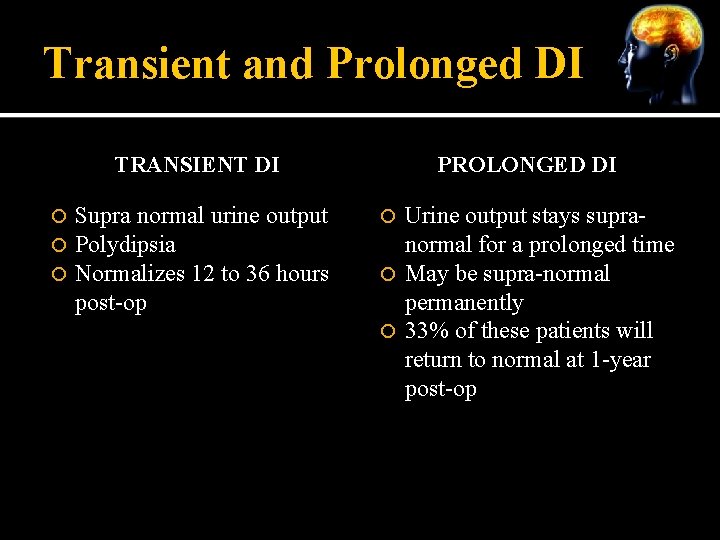

Transient and Prolonged DI TRANSIENT DI Supra normal urine output Polydipsia Normalizes 12 to 36 hours post-op PROLONGED DI Urine output stays supranormal for a prolonged time May be supra-normal permanently 33% of these patients will return to normal at 1 -year post-op

Triphasic Response Phase 1: Injury to the pituitary reduces ADH levels for 4 -5 days Polyuria/Polydipsia Phase 2: Cell death liberated ADH for the next 4 -5 days leading to transient normalization or even SIADH Phase 3: Reduced or absent ADH secretion leading to either transient or prolonged DI

Clinical Findings of DI SIGNS AND SYMPTOMS Polydipsia 2 to 20 L Daily Polyuria > 300 cc/hr for 2 consecutive hours Dilute urine LABORATORY FINDINGS High normal to High serum sodium High serum osmolality Low urine osmolality (specific gravity 1. 001 to 1. 005)
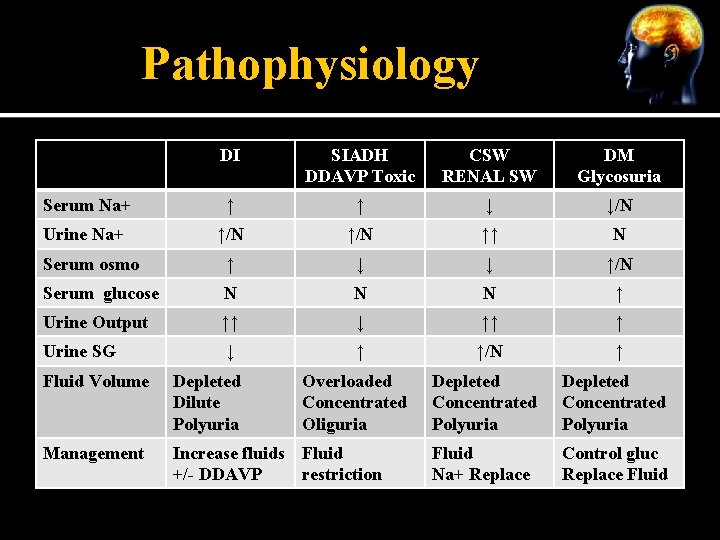
Pathophysiology DI SIADH DDAVP Toxic CSW RENAL SW DM Glycosuria Serum Na+ ↑ ↑ ↓ ↓/N Urine Na+ ↑/N ↑↑ N Serum osmo ↑ ↓ ↓ ↑/N Serum glucose N N N ↑ Urine Output ↑↑ ↓ ↑↑ ↑ Urine SG ↓ ↑ ↑/N ↑ Overloaded Concentrated Oliguria Depleted Concentrated Polyuria Fluid Na+ Replace Control gluc Replace Fluid Volume Depleted Dilute Polyuria Management Increase fluids Fluid +/- DDAVP restriction

Antidiuretic Hormone Prevents the output of large volumes of urine and can constrict blood vessels to increase blood pressure Sometimes called “Vasopressin” Synthesized primarily by neuron cell bodies in the supraoptic nucleus of the hypothalamus Transported by axons of the hypothalamohypophsial to the posterior pituitary where it is secreted

Antidiuretic Hormone Osmoreceptors synapse with neurosecretory cells in the hypothalamus Osmoreceptors monitor blood osmolality and blood volume Increased osmolality stimulates osmoreceptors to leads to secretion of ADH from posterior pituitary Target tissue is the renal tubules where ADH leads to increased water retention
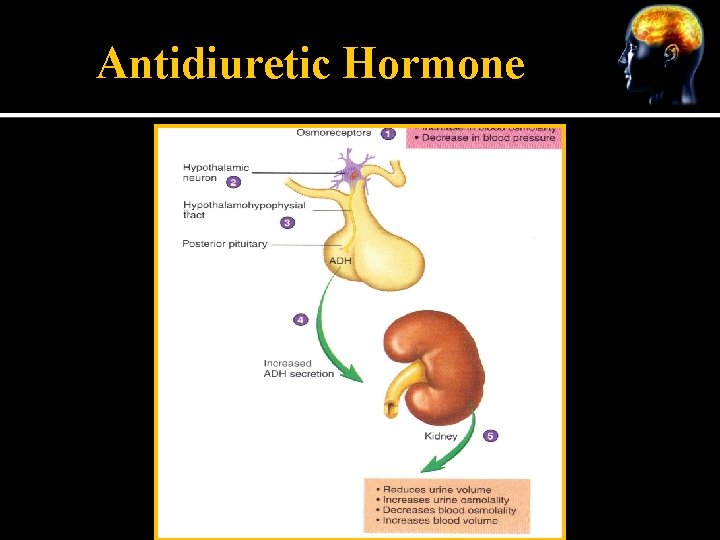
Antidiuretic Hormone

Antidiuretic Hormone ADH attaches to a V 2 receptor and activates a cascade through a Gs protein, adenylyl cyclase, c. AMP and protein kinase A Cascade leads to insertion of a aquaporin-2 into the apical membrane of the collecting duct Water then moves through aquaporin-2 in response to an osmotic gradient and then through aquaporins-3 and -4 in the basolateral membrane and back into circulation
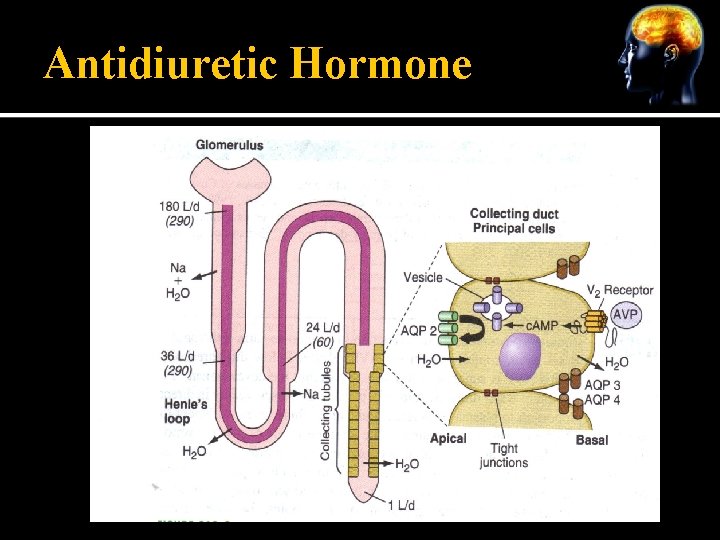
Antidiuretic Hormone
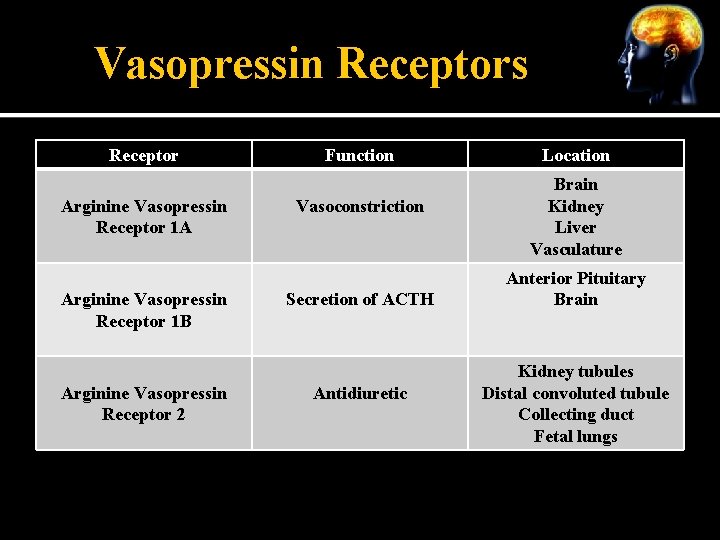
Vasopressin Receptors Receptor Arginine Vasopressin Receptor 1 A Arginine Vasopressin Receptor 1 B Arginine Vasopressin Receptor 2 Function Vasoconstriction Secretion of ACTH Antidiuretic Location Brain Kidney Liver Vasculature Anterior Pituitary Brain Kidney tubules Distal convoluted tubule Collecting duct Fetal lungs

Management

Managment of DI Primarily the management of DI in the NCU is handled by Endocrine At no time should the ICU team order or dose DDAVP In the short-term if needed may start a vasopressin infusion In most awake patients their thirst mechanism will prevent them from becoming too dehydrated

Management of DI Desmopressin Acetate DDAVP Long-acting synthetic analog of vasopressin Minimal V 1 activity Antidiuretic-to-pressor ratio is 4000 times that of vasopressin Half-life is 1. 5 to 2. 5 hours

Management of DI Vasopressin Activates both V 1 and V 2 receptor Reduces diuresis through increased water permeability and water reabsorption in the collecting ducts Extrarenal V 2 receptors regulate release of coagulation factor VIII and von Willebrand factor

Management of DI ARGININE VASOPRESSIN DESMOPRESSIN

Questions?
- Slides: 33