Network Bulletinpolicy and protocol updates preview August 2021
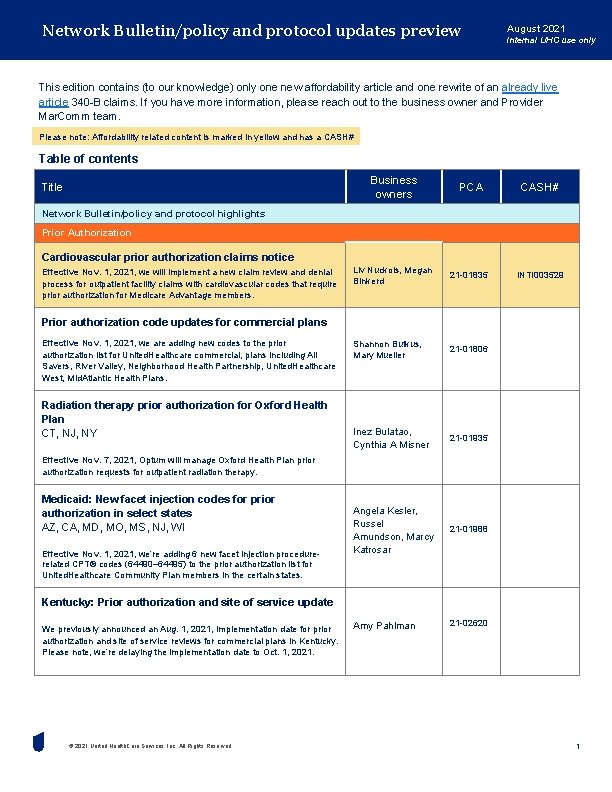
Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only This edition contains (to our knowledge) only one new affordability article and one rewrite of an already live article 340 -B claims. If you have more information, please reach out to the business owner and Provider Mar. Comm team. Please note: Affordability related content is marked in yellow and has a CASH# Table of contents Business owners Title PCA CASH# Network Bulletin/policy and protocol highlights Prior Authorization Cardiovascular prior authorization claims notice Effective Nov. 1, 2021, we will implement a new claim review and denial process for outpatient facility claims with cardiovascular codes that require prior authorization for Medicare Advantage members. Liv Nuckols, Megan Binkerd 21 -01835 Shannon Butkus, Mary Mueller 21 -01806 Inez Bulatao, Cynthia A Misner 21 -01935 Angela Kesler, Russel Amundson, Marcy Katrosar 21 -01988 Amy Pahlman 21 -02620 INTI 003529 Prior authorization code updates for commercial plans Effective Nov. 1, 2021, we are adding new codes to the prior authorization list for United. Healthcare commercial, plans including All Savers, River Valley, Neighborhood Health Partnership, United. Healthcare West, Mid. Atlantic Health Plans. Radiation therapy prior authorization for Oxford Health Plan CT, NJ, NY Effective Nov. 7, 2021, Optum will manage Oxford Health Plan prior authorization requests for outpatient radiation therapy. Medicaid: New facet injection codes for prior authorization in select states AZ, CA, MD, MO, MS, NJ, WI Effective Nov. 1, 2021, we’re adding 6 new facet injection procedurerelated CPT® codes (64490‒ 64495) to the prior authorization list for United. Healthcare Community Plan members in the certain states. Kentucky: Prior authorization and site of service update We previously announced an Aug. 1, 2021, implementation date for prior authorization and site of service reviews for commercial plans in Kentucky. Please note, we’re delaying the implementation date to Oct. 1, 2021. © 2021 United Health. Care Services, Inc. All Rights Reserved. 1
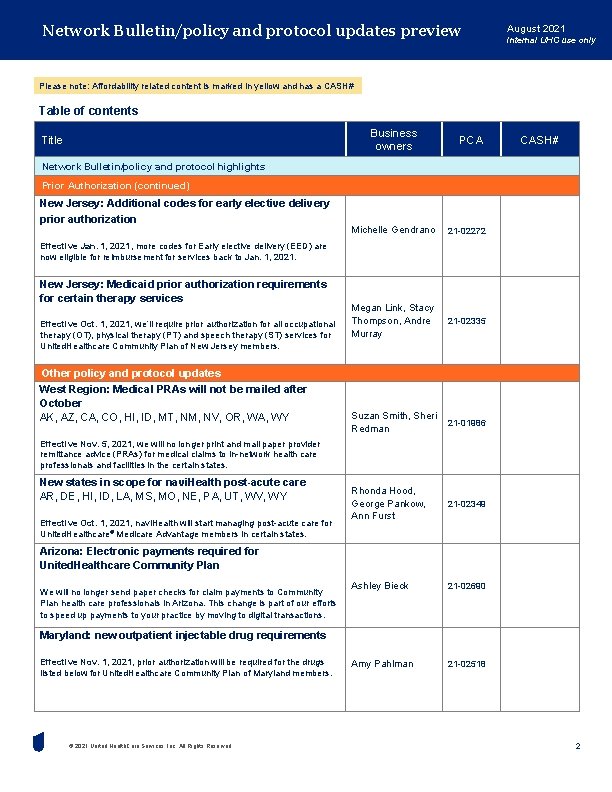
Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Please note: Affordability related content is marked in yellow and has a CASH# Table of contents Business owners Title PCA CASH# Network Bulletin/policy and protocol highlights Prior Authorization (continued) New Jersey: Additional codes for early elective delivery prior authorization Michelle Gendrano 21 -02272 Megan Link, Stacy Thompson, Andre Murray 21 -02335 Suzan Smith, Sheri Redman 21 -01986 Rhonda Hood, George Pankow, Ann Furst 21 -02349 Ashley Bieck 21 -02690 Amy Pahlman 21 -02518 Effective Jan. 1, 2021, more codes for Early elective delivery (EED) are now eligible for reimbursement for services back to Jan. 1, 2021. New Jersey: Medicaid prior authorization requirements for certain therapy services Effective Oct. 1, 2021, we’ll require prior authorization for all occupational therapy (OT), physical therapy (PT) and speech therapy (ST) services for United. Healthcare Community Plan of New Jersey members. Other policy and protocol updates West Region: Medical PRAs will not be mailed after October AK, AZ, CA, CO, HI, ID, MT, NM, NV, OR, WA, WY Effective Nov. 5, 2021, we will no longer print and mail paper provider remittance advice (PRAs) for medical claims to in-network health care professionals and facilities in the certain states. New states in scope for navi. Health post-acute care AR, DE, HI, ID, LA, MS, MO, NE, PA, UT, WV, WY Effective Oct. 1, 2021, navi. Health will start managing post-acute care for United. Healthcare® Medicare Advantage members in certain states. Arizona: Electronic payments required for United. Healthcare Community Plan We will no longer send paper checks for claim payments to Community Plan health care professionals in Arizona. This change is part of our efforts to speed up payments to your practice by moving to digital transactions. Maryland: new outpatient injectable drug requirements Effective Nov. 1, 2021, prior authorization will be required for the drugs listed below for United. Healthcare Community Plan of Maryland members. © 2021 United Health. Care Services, Inc. All Rights Reserved. 2
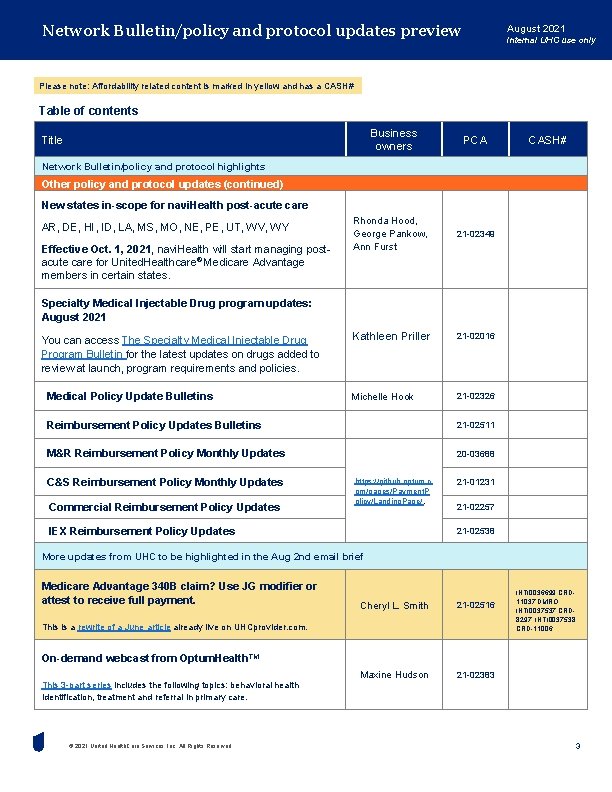
Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Please note: Affordability related content is marked in yellow and has a CASH# Table of contents Business owners Title PCA CASH# Network Bulletin/policy and protocol highlights Other policy and protocol updates (continued) New states in-scope for navi. Health post-acute care AR, DE, HI, ID, LA, MS, MO, NE, PE, UT, WV, WY Effective Oct. 1, 2021, navi. Health will start managing postacute care for United. Healthcare® Medicare Advantage members in certain states. Rhonda Hood, George Pankow, Ann Furst 21 -02349 Kathleen Priller 21 -02016 Michelle Hook 21 -02326 Specialty Medical Injectable Drug program updates: August 2021 You can access The Specialty Medical Injectable Drug Program Bulletin for the latest updates on drugs added to review at launch, program requirements and policies. Medical Policy Update Bulletins Reimbursement Policy Updates Bulletins 21 -02511 M&R Reimbursement Policy Monthly Updates 20 -03688 C&S Reimbursement Policy Monthly Updates Commercial Reimbursement Policy Updates https: //github. optum. c om/pages/Payment. P olicy/Landing. Page/. IEX Reimbursement Policy Updates 21 -01231 21 -02257 21 -02538 More updates from UHC to be highlighted in the Aug 2 nd email brief Medicare Advantage 340 B claim? Use JG modifier or attest to receive full payment. Cheryl L. Smith 21 -02516 Maxine Hudson 21 -02383 This is a rewrite of a June article already live on UHCprovider. com. INTI 0036699 CRD 11037 DMRO, INTI 0037537 CRD 8297, INTI 0037538 CRD-11006 On-demand webcast from Optum. Health. TM This 3 -part series includes the following topics: behavioral health identification, treatment and referral in primary care. © 2021 United Health. Care Services, Inc. All Rights Reserved. 3
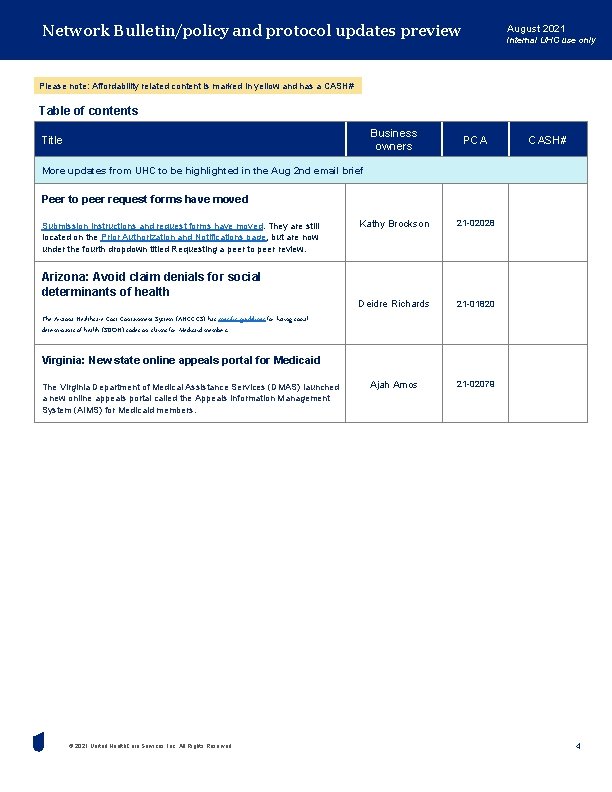
Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Please note: Affordability related content is marked in yellow and has a CASH# Table of contents Business owners PCA Kathy Brockson 21 -02028 Deidre Richards 21 -01820 Ajah Amos 21 -02079 Title CASH# More updates from UHC to be highlighted in the Aug 2 nd email brief Peer to peer request forms have moved Submission instructions and request forms have moved. They are still located on the Prior Authorization and Notifications page, but are now under the fourth dropdown titled Requesting a peer to peer review. Arizona: Avoid claim denials for social determinants of health The Arizona Healthcare Cost Containment System (AHCCCS) has specific guidelines for listing social determinants of health (SDOH) codes on claims for Medicaid members. Virginia: New state online appeals portal for Medicaid The Virginia Department of Medical Assistance Services (DMAS) launched a new online appeals portal called the Appeals Information Management System (AIMS) for Medicaid members. © 2021 United Health. Care Services, Inc. All Rights Reserved. 4

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Prior Authorization updates Cardiovascular prior authorization claims notice Notice of change to review process related to Cardiovascular codes that require prior authorization codes Minimize claims denials Effective Nov. 1, 2021, we will implement a new claim review and denial process for outpatient facility claims with cardiovascular codes that require prior authorization for Medicare Advantage members. The new process identifies and denies services and procedures associated with cardiovascular codes that have a prior authorization denial or missing prior authorization. If a prior authorization is not received or a prior authorization code is denied, the entire outpatient facility claim will be denied. Important information It is important that health care providers secure all required prior authorizations before performing procedures and that outpatient facilities confirm receipt of those authorizations prior to performing the procedure(s). Minimize claim denials Outpatient facilities should confirm that health care providers secure the appropriate prior authorizations prior to procedure date. Questions? Call United. Healthcare Provider Services at 877 -842 -3210. Prior authorization code updates for commercial plans Effective Nov. 1, 2021, we are adding new codes to the prior authorization list for United. Healthcare commercial, plans including All Savers, River Valley, Neighborhood Health Partnership, United. Healthcare West, Mid. Atlantic Health Plans. Updated codes • Arthroplasty • Breast reconstruction – gynecomastia: 19300 • Cartilage implants: 27415, 27416 • Cosmetic & reconstructive • Hysterectomy (In-patient only): 58267, 58280 • Orthognathic surgery • Pain injections and management • Potentially unproven: 0376 T • Prostate procedures • Spine surgery • Stimulators – neuro: L 8679, L 8683 • Transplant • Vein procedures What codes are being added? Additional reference can be found in the 2021 Summary of Changes to Advance Notification and Prior Authorization Requirements. Learn more • Applicable commercial policies • Current prior authorization requirements • Check requirements, submit new authorizations/notifications, check status and submit updates by registering forlive training or using the Prior Authorization and Notification Interactive User Guide © 2021 United Health. Care Services, Inc. All Rights Reserved. 5

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Prior Authorization updates Radiation therapy prior authorization for Oxford Health Plan Effective Nov. 7, 2021, Optum will manage Oxford Health Plan prior authorization requests for outpatient radiation therapy. What’s changing For Oxford Health Plan members, we’ll require prior authorization for the following radiation therapy services, formerly managed by evi. Core: • Intensity-modulated radiation therapy • Proton beam therapy • Stereotactic body radiation therapy/stereotactic radiosurgery • Fractionation for breast cancer, prostate cancer, lung cancer and bone metastasis • Image-guided radiation therapy • Special and associated radiation therapy services • Selective internal radiation therapy (SIRT), Yttrium 90 (Y 90) and implantable beta-emitting microspheres for treatment of malignant tumors Optum will begin accepting prior authorizations submissions Nov. 1, 2021, for prior authorizations effective Nov. 7, 2021, and later. This change will affect commercial health plan members in the Oxford Health Plan, effective Nov. 7, 2021. Any active radiation therapy prior authorizations requested up until Nov. 6, 2021, will remain in place through the former process. A new prior authorization request will be required for radiation therapy services on Nov. 7, 2021, and thereafter for specific CPT® codes (link to code list). Important notes • Prior authorization for radiation therapy will be part of the comprehensive management of oncology service requests in the Cancer Guidance Program • If you already received a prior authorization for radiation therapy services in scope for prior authorization administered prior to Nov. 7, 2021, you DO NOT need to submit a new prior authorization request for that approved treatment • The coverage determination guidelines we use for the radiation therapy services will be available at UHCprovider. com/policies > Medical & Drug Policies and Coverage Determination Guidelines for Commercial Submit a prior authorization request To submit an online request, beginning Nov. 1, 2021, for prior authorization, starting Nov. 7, 2021: 1. Go to the Provider Portal at UHCprovider. com > Sign in 2. Select Prior Authorization and then Radiology, Cardiology, Oncology and Radiation Oncology 3. Select service type, Radiation Oncology 4. After selecting Oxford as the product type, you will be directed to another website to process the authorization requests For more information, go to UHCprovider. com. Questions? Please email unitedoncology@uhc. com. Add CPT disclaimer: CPT® is a registered trademark of the American Medical Association. © 2021 United Health. Care Services, Inc. All Rights Reserved. 6

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Prior Authorization updates Medicaid: New facet injection codes for prior authorization in select states Effective Nov. 1, 2021, we’re adding 6 new facet injection procedure-related CPT® codes (64490‒ 64495) to the prior authorization list for United. Healthcare Community Plan members in the following states: Arizona California Maryland Mississippi Missouri New Jersey Wisconsin For complete details on facet injection protocol, please see the Community Plan Medical & Drug Policies and Coverage Determination Guidelines. To submit prior authorizations online: Go to UHCprovider. com and click Sign In to access the United. Healthcare Provider Portal Select Prior Authorizations from the blue navigation bar at the top of the page Click Create New Submissions (located in the create a new notification or prior authorization request box) Training available Check out the following to help you manage prior authorizations online: Prior Authorization and Notification self-paced guide Track It for status request information updates Questions? Please contact your local Network Management representative or call United. Healthcare Provider Services, toll-free, at 877842 -3210, 7 a. m. – 5 p. m. CT, Monday–Friday. CPT® is a registered trademark of the American Medical Association. © 2021 United Health. Care Services, Inc. All Rights Reserved. 7

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Prior Authorization updates Kentucky: Prior authorization and site of service update Update Aug. 1, 2021: We previously announced an Aug. 1, 2021, implementation date for prior authorization and site of service reviews for commercial plans in Kentucky. Please note, we’re delaying the implementation date to Oct. 1, 2021, as outlined below. For dates of service on or after Oct. 1, 2021, for United. Healthcare commercial plans, we’re expanding our prior authorization requirements to include certain surgical, screening colonoscopy, office and MRI/CT imaging procedures in Kentucky. • We’ll conduct site of service medical necessity reviews for surgical, screening colonoscopy and MRI/CT imaging procedures if the procedure is requested to be performed in an outpatient hospital setting • For office-based procedures, we’ll conduct site of service medical necessity reviews if the procedure is requested to be performed in an ambulatory surgical center We’ll use the following utilization review guidelines to facilitate these site of service medical necessity reviews: • Outpatient Surgical Procedures – Site of Service • Screening Colonoscopy Procedures – Site of Service • Magnetic Resonance Imaging (MRI) and Computed Tomography (CT) Scan – Site of Service • Office-Based Procedures – Site of Service More information is available in our frequently asked questions: • Site of Service Surgical and Screening Colonoscopy Commercial FAQ • Site of Service MRI/CT Commercial FAQ Questions? Call Provider Services at 800 -666 -1353. New Jersey: Additional codes for early elective delivery prior authorization As a follow-up to the Early elective delivery (EED) reimbursement changes effective Jan. 1, 2021, more codes are now eligible for reimbursement for services back to Jan. 1, 2021. Prior authorization Scheduled EEDs under 39 weeks of gestation due to medical necessity require an approved prior authorization or submitted notification. For information on how to submit electronically, visit UHCprovider. com/paan or call Provider Services at 888 -362 -3386, Monday through Friday, 8 a. m. to 6 p. m. Claim submissions Obstetricians, midwives, hospitals and clinics requesting New Jersey Family Care (NJFC) Medicaid reimbursement for a labor and delivery claim are required to report an ICD-10 -CM diagnosis code indicating the week of gestation (ICD-10 -CM category code Z 3 A). Claims submitted without a diagnosis code indicating the week of gestation will be denied by the NJFC Medicaid Program. Any claim reporting a week of gestation ICD-10 -CM diagnosis code of less than 39 weeks without one of the following diagnosis codes will also be denied: O 10, O 11, O 12, O 13, O 14, O 15, O 16, O 24, O 30, O 31, O 33, O 35, O 36, O 42, O 43, O 44, O 45, O 71 or R 03. Questions? Call Provider Services at 888 -362 -3368, Monday through Friday, 8 a. m. to 6 p. m. © 2021 United Health. Care Services, Inc. All Rights Reserved. 8

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Prior Authorization updates New Jersey: Medicaid prior authorization requirements for certain therapy services Effective Oct. 1, 2021, we’ll require prior authorization for all occupational therapy (OT), physical therapy (PT) and speech therapy (ST) services for United. Healthcare Community Plan of New Jersey members. Prior authorization requirements View the full list of the codes that require prior authorization Out-of-network physicians, facilities and other health care professionals must request prior authorization for all procedures and services, excluding emergency or urgent care These requirements will apply whether a member is new to therapy or will continue receiving therapy We’ll deny claims if prior authorization is not on file before the date of service, and you won’t be able to balance bill the member Prior authorization isn’t required for emergency or urgent services Medical necessity review When you submit a prior authorization request starting Oct. 1, 2021, we’ll review your request for medical necessity. We’ll provide an authorization if appropriate and send that determination to you and the member. Reviewing your requests before the effective date We’d like to help you get ready by offering a review for your patients who are or will start receiving therapy services before the prior authorization requirement effective date. Starting 30 days before the effective date, you can submit the patient information using the Prior Authorization and Notification tool at UHCprovider. com/paan. We’ll let you know if your request meets the Speech Language Pathology Services or Outpatient Physical and Occupational Therapycoverage determination guidelines. If the review shows that the request meets the coverage determination guidelines, we’ll give you an authorization number. With an authorization number, you won’t have to resubmit a request for that initial prior authorization. If the review shows that the request wouldn’t be approved under the coverage determination guidelines, we’ll give you more information about our decision. You may resubmit for review with more information. Questions? Please contact us at 866 -362 -3368. For Optum contracting and credentialing questions, contact Optum at 800 -873 -4575. © 2021 United Health. Care Services, Inc. All Rights Reserved. 9

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Other policy and protocol updates West Region: Medical PRAs will not be mailed after October Effective Nov. 5, 2021, for all United. Healthcare plans, we will no longer print and mail paper provider remittance advice (PRAs) for commercial medical claims to network health care professionals and facilities in the following states: • • • Alaska Arizona California Colorado Hawaii Idaho • • • Montana Nevada New Mexico Oregon Washington Wyoming Please share this information with others in your organization who need to know about this change. This change applies to most United. Healthcare plans in the region. * It does not affect Optum Pay™ subscribers with electronic funds transfer (EFT). If you receive an electronic remittance advice (ERA)/835 and a paper PRA, your paper PRA will no longer be mailed, but your ERA process remains unchanged. If you work with an outside vendor, such as a revenue cycle management company, for your mail processing, please discuss with them to determine how this change may affect your contract or processing arrangements. Options to view PRAs electronically There are several ways you can view PRAs electronically. Choose the one that works best for your practice or facility: • Document Vault: This secure online repository of reports and claim-related communication is available through the United. Healthcare Provider Portal. PRAs are produced at the time of payment processing and available for you to access the next day in Document Vault. Explore Document Vault Verify your access • Optum Pay: Through our affiliation with Optum Pay, you can reconcile remittance data with basic portal or premium portal access. Basic portal access is free to those enrolled in ACH/direct deposit through Optum Pay. Premium portal access is a fee-based service that includes additional practice management features and data aggregation tools. (Premium portal access is available at no additional cost for those receiving virtual card payments from United. Healthcare. ) Learn more • EDI: Set up Electronic Remittance Advice (ERA) 835 transactions using Electronic Data Interchange (EDI) to receive your PRAs electronically. An additional benefit is the capability to autopost payments into your practice management or hospital information system. Contact your clearinghouse to start the process. Note: ERA/385 setup takes about 30 days from when we receive the request. Check out EDI Upcoming digital transitions The move toward digital (paperless) delivery of reports and claim-related communication for network health care professionals will continue throughout 2021 and 2022. Announcements will be made on UHCprovider. com/news 90 days before mailings end so you have time to prepare. Questions? Please contact United. Healthcare Provider Services, toll-free, at 877 -842 -3210, TTY/RTT 711, 7 a. m. – 5 p. m. CT, Monday–Friday. *PRAs will continue to be mailed to: Behavioral Health; American Association of Retired Persons (AARP®) Medicare supplement products and All Savers Insurance, Sierra Health and Life; Rocky Mountain Health Plan; UHCWest; United. Health. One; UMR; United. Healthcare Global; Student Resources; Home and Community Based Services; Optum VA Critical Care Network (CCN). © 2021 United Health. Care Services, Inc. All Rights Reserved. 10

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Other policy and protocol updates New states in-scope for navi. Health post-acute care Effective Oct. 1, 2021, navi. Health will start managing post-acute care for United. Healthcare® Medicare Advantage members in Arkansas, Delaware, Hawaii, Idaho, Louisiana, Mississippi, Montana, Nevada, Pennsylvania, Utah, West Virginia and Wyoming. This is in addition to the post-acute care management change that went into effect for certain states on June 1, 2021, and Aug. 1, 2021. This includes prior authorization, concurrent (continued stay) review and discharge planning for members transitioning to and receiving skilled care in: • Skilled nursing facilities (SNFs) • Acute Inpatient Rehab (AIR) • Long-Term Acute Care (LTAC) Plans included: • Medicare Advantage Plans previously managed by United. Healthcare • Dual Eligible Special Needs Plans (DSNP) • Chronic Special Needs Plans (CSNP) Plans not included: • United. Healthcare Institutional Special Needs Plans (ISNP) • United. Healthcare Institutional-Equivalent Special Needs Plans (IE-SNP) • Any Medicare Advantage members included in a delegated risk agreement to provider medical groups (e. g. , Optum Care Network) • United. Healthcare commercial plans • United. Healthcare Community Plans (Medicaid Only Plans) • Long-Term Support Services (LTSS) What happens next You'll receive an email invitation to attend a provider education session. Attending the session will help ensure a smooth transition for you, your teams and our members. To learn more about navi. Health and the United. Healthcare partnership, visit navihealth. com/united-provider-info. Please bookmark this site and check back frequently. Ongoing updates will be posted. © 2021 United Health. Care Services, Inc. All Rights Reserved. 11

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Other policy and protocol updates Arizona: Electronic payments required for United. Healthcare Community Plan We will no longer send paper checks for claim payments to Community Plan health care professionals in Arizona. This change is part of our efforts to speed up payments to your practice by moving to digital transactions. You will need to choose between two options for receiving payment from United. Healthcare: Automated Clearing House (ACH) /direct deposit: We recommend ACH because it’s the quickest form of payment available and there are no fees for the service. Payments can be routed by both the tax ID number (TIN) and National Provider Identifier (NPI) number level. • Enrollment generally takes less than 10 minutes. You will need to provide your current bank account information. • If you prefer this payment option, we encourage you to complete your registration as soon as possible. We cannot hold claim payments while registration is finalized and ACH is activated with your financial institution. Sign up now Virtual Card Payment (VCP): If you don’t enroll in ACH, in most instances you’ll receive a virtual card payment from Optum Pay. VCPs are electronic payments that use credit card technology to process claim payments. There is no requirement to share bank account information. • A 16‐digit, single-use virtual card will be issued for payment (single or multiple claims). You’ll receive a VCP in the mail; for quicker access, you can choose to view the VCP statement in Document Vault or the Optum Pay portal. • Each VCP is issued for the full amount of the claim payment. However, VCPs are subject to additional terms and conditions, including fees, between you and your card service processor. • You can enroll in ACH even after receiving a virtual card payment. However, ACH will only apply to future payments and can’t be applied to previously payments made. Payment information available online We recommend using one of the following to view the Provider Remittance Advice (PRA) documents for these electronic payments: 1. Document Vault, our secure online repository of reports and claim-related communication. PRAs are produced at the time of payment processing and available for you to access the next day in Document Vault. 2. Optum Pay Basic Portal with unlimited users, is available to those who enroll in ACH/direct deposit. You can access up to 13 months of payment data, including downloadable PRAs and 835 files. 3. Optum Pay Premium Portal, available at no additional cost if you receive VCPs through Optum Pay, or with a 0. 5% per payment fee if you choose to enroll. Premium portal access has all the features of the basic portal, as well as additional practice management features and data aggregation tools. While PRAs are currently being mailed, we will be moving to digital-only access in late 2021 and early 2022. Questions? Visit UHCprovider. com/payment or view our Frequently Asked Questions for more information. The following states are already effective for electronic payments: California, Hawaii, Maryland, Massachusetts, Michigan, Missouri, Nebraska, North Carolina, Ohio, Oklahoma, Pennsylvania, Rhode Island, Tennessee, Texas, Virginia, Washington and Wisconsin In Colorado, Georgia and New Jersey, if you do not consent to receive virtual card payments and you don’t want to set up direct deposit, call 877 -548 -0460 to receive a paper check. If you are an out-of-network provider in Florida, New Mexico, New York or Oregon, and you do not consent to a virtual card payment or you don’t have direct deposit, call 877 -548 -0460 to receive a paper check. © 2021 United Health. Care Services, Inc. All Rights Reserved. 12

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Other policy and protocol updates Maryland: new outpatient injectable drug requirements Effective Nov. 1, 2021, prior authorization will be required for the drugs listed below for United. Healthcare Community Plan of Maryland members: Adakveo® Crysvita® Evenity® Exondys 51® Fasenra® Gamifant® Givlaari® Ilumya™ Kalbitor® Luxturna® Onpattro® Radicava® Reblozyl® Tepezza® Ultomiris® Vyepti® Vyondys 53® If you administer any of these medications without first completing the prior authorization process, the claim may be denied. Members can’t be billed for services denied due to failure to complete the prior authorization process. You can submit prior authorization requests: • Online: Use the Prior Authorization and Notification tool on UHCprovider. com To view the clinical policies for these drugs, go to Medical & Drug Policies and Coverage Determination Guidelines. Questions? Call the Provider Services phone number on the member’s health care identification card. © 2021 United Health. Care Services, Inc. All Rights Reserved. 13

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Other policy and protocol updates Specialty Medical Injectable Drug program updates: August 2021 You can access The Specialty Medical Injectable Drug Program Bulletin for the latest updates on drugs added to review at launch, program requirements and policies. © 2021 United Health. Care Services, Inc. All Rights Reserved. 14

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Other policy and protocol updates Medical Policy Updates: July 2021 United. Healthcare Commercial & Affiliates United. Healthcare Commercial Medical Policy Update Bulletin: August 2021 United. Healthcare Oxford Policy Update Bulletin: August 2021 United. Healthcare West Benefit Interpretation Policy Update Bulletin: August 2021 United. Healthcare West Medical Management Guideline Update Bulletin: August 2021 United. Healthcare Exchange Plans United. Healthcare Value & Balance Exchange Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan of Indiana Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan of Kentucky Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan of Louisiana Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan of Mississippi Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan of North Carolina Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan of Pennsylvania Medical Policy Update Bulletin: August 2021 United. Healthcare Community Plan of Tennessee Medical Policy Update Bulletin: August 2021 United. Healthcare Medicare Advantage Coverage Summary Update Bulletin: August 2021 United. Healthcare Medicare Advantage Policy Guideline Update Bulletin: August 2021 United. Healthcare Dental Policy Update Bulletin: August 2021 © 2021 United Health. Care Services, Inc. All Rights Reserved. 15

Network Bulletin/policy and protocol updates preview August 2021 Internal UHC use only Other policy and protocol updates Reimbursement Policy Update Bulletins: August 2021 You can review the details on reimbursement policy updates through the following: United. Healthcare Commercial Plan Reimbursement Policies Update Bulletin: August 2021 United. Healthcare Community Plan Reimbursement Policies Update Bulletin: August 2021 United. Healthcare Individual Exchange Plan Reimbursement Policies Update Bulletin: August 2021 United. Healthcare Medicare Advantage Reimbursement Policy Update Bulletin: August 2021 © 2021 United Health. Care Services, Inc. All Rights Reserved. 16

Other updates from UHCprovider. com August 2021 Internal UHC use only Medicare Advantage 340 B claim? Use JG modifier or attest to receive full payment. Use JG modifier or attest to receive accurate Medicare Advantage 340 B payments Are you a non-exempt 340 B Medicare Advantage health care professional? If so, to receive accurate claim payments involving separately payable, Outpatient Perspective Payment System (OPPS) drugs and biologics with status indicator K, United. Healthcare requires 1 of 2 things: 1. The JG modifier (if purchased through the 340 B program), or 2. Attestation that this drug or biologic wasn’t purchased through the 340 B program Claim review and notification begins July 23 Beginning July 23, 2021, if neither is provided, we will assume the drug was purchased through the 340 B program and adjust the claim to provide reimbursement at the discounted 340 B rate of average sales price (ASP) minus 22. 5%. If you are set up to receive ACE/Smart Edits, within 24 hours of claim submission, you will receive a message on your 277 CA clearinghouse report indicating the claim may be subject to 340 B coding and billing requirements. Options to modify your claim If you receive an ACE/Smart Edit notification, you have 2 choices to modify your original claim submission and be considered for full payment: 1. If you purchased the drug or biologic through the 340 B program: Update and resubmit the claim with the JG modifier as follows: • Place the modifier on the UB claim form, Service Line Remarks status K drugs line • For a claim with multiple drug lines, use the appropriate 340 B modifier on separate claim lines for each separately payable, non-pass through 340 B-acquired drug (status indicator K) 2. If you did not purchase through the 340 B program: Attest that the drug or biological was not purchased through the 340 B program as follows: • Use the UB claim form Service Line Remarks field (see example below) • The attestation must include: • The word “attests” • The reason why the item was not obtained via the 340 B program (according to CMS guidance) in the Status K drug line, and • The specific Drug code (if multiple drug codes were billed) • Do not include the JG modifier If the JG modifier or attestation is not provided If you submit 340 B claims without the JG modifier or attestation, benefits for the claim will be determined based on the discounted 340 B rate. Your provider remittance advice (PRA) will indicate that the claim was paid with a 340 B program payment discount. Continue to the next page… © 2021 United Health. Care Services, Inc. All Rights Reserved. 17

Other updates from UHCprovider. com August 2021 Internal UHC use only Medicare Advantage 340 B claim? Use JG modifier or attest to receive full payment. …continued In the future Please adjust your billing process to include the JG modifier on appropriate claims or attestations when drugs or biologics are purchased outside of the 340 B program. Doing so prevents Smart Edit or other notifications and helps ensure prompt and accurate claim processing. Other 340 B updates and reminders • Drug payment rate: United. Healthcare will continue to pay for 340 B-acquired drugs (status indicator K) that include the JG modifier at the discounted rate of average sales price (ASP) minus 22. 5% • Medicare billing requirements: 340 B facilities must follow Centers for Medicare & Medicaid Services (CMS) coding and billing requirements, and provide accurate and complete claim documentation upon request • Ongoing payment reviews: United. Healthcare will continue to do retrospective reviews on paid 340 B claims Additional resources • Smart Edits: Visit our Smart Edits webpage and see the Claims Payer List for United. Healthcare, Affiliates and Strategic Alliances for a full list of eligible payer IDs • CMS Medicare Fee-for-Service (FFS) Program Frequently Asked Questions: More information on using JG/TB modifiers Questions? Contact your Provider Advocate or United. Healthcare Provider Services, toll-free, at 877 -842 -3210, 7 a. m. – 5 p. m. CT, Monday–Friday. *As defined in the Affordable Care Act, section 1927(k) © 2021 United Health. Care Services, Inc. All Rights Reserved. 18
Other updates from UHCprovider. com August 2021 Internal UHC use only Peer to peer request forms have moved Submission instructions and request forms have moved. They are still located on the Prior Authorization and Notifications page, but are now under the fourth dropdown titled Requesting a peer to peer review. You can also schedule (or reschedule) a Peer to Peer review by contacting the Peer to Peer Support team by email at UHC_Peer. To. Peer_Scheduling@uhc. com or toll-free, at 800 -955 -7615, 7 a. m. – 7 p. m. CT Monday–Friday. Request form updates include: • Why peer to peer reviews are done • What to know before making a request • What you’ll need to fill out the request form Questions? For general questions about Peer to Peer reviews, please call United. Healthcare Provider Services, toll-free, at 877 -842 -3210, 7 a. m. – 5 p. m. CT Monday–Friday. © 2021 United Health. Care Services, Inc. All Rights Reserved. 19

Other updates from UHCprovider. com August 2021 Internal UHC use only Arizona: Avoid claim denials for social determinants of health The Arizona Healthcare Cost Containment System (AHCCCS) has specific guidelines for listing social determinants of health (SDOH) codes on claims for Medicaid members. Please follow these guidelines to help ensure you’re billing us correctly when including SDOH codes on claims: • Social determinant ICD-10 diagnosis code(s) in code range Z 55–Z 65 cannot be listed as the primary ICD-10 diagnosis code(s) • These codes should only be used as secondary or tertiary diagnosis codes • We’ll deny claims submitted to us with ICD-10 diagnosis codes Z 55–Z 65 listed as the primary diagnosis code(s) • If this happens, you’ll need to submit a corrected claim Learn more For more information about coding and reporting guidelines, please see: • AHCCCS Social Determinants of Health ICD-10 Code List • Centers for Medicare & Medicaid Services (CMS) ICD-10 -CM Guidelines, pages 17– 18: ICD-10 -CM Official Guidelines for Coding and Reporting Please note: Coding and reporting guidelines may be updated at any time. Questions? • Call Provider Services at 800 -445 -1638 for AHCCCS Complete Care (ACC) and Developmental Disabilities (DD) • Call 800 -293 -3740 for Arizona Long-Term Care System (ALTCS) © 2021 United Health. Care Services, Inc. All Rights Reserved. 20

Other updates from UHCprovider. com August 2021 Internal UHC use only Virginia: New state online appeals portal for Medicaid The Virginia Department of Medical Assistance Services (DMAS) launched a new online appeals portal called the Appeals Information Management System (AIMS) for Medicaid members. No change for internal appeals When filing the first level of appeal, continue using the current United. Healthcare appeals process. The new AIMS portal will handle the next level of appeal after the appeals process is exhausted with United. Healthcare. AIMS training Training on how to use the AIMS portal is available on the DMAS website at dmas. virginia. gov/appeals. Questions? Contact DMAS Appeals at 804 -371 -8488. © 2021 United Health. Care Services, Inc. All Rights Reserved. 21

© 2021 United Health. Care Services, Inc. All Rights Reserved. 22
- Slides: 22