Neonatology By Assist Prof Dr Amin Turki Evaluation

Neonatology By Assist Prof. Dr. Amin Turki

Evaluation of newborn history: Perinatal history should concentrate on the following: 1. Demographic and social data: socioeconomic status, parents age, race cal illnesses in the family: ardiopulmonary disorders, infectious diseases, genetic disorders, diabetes mellitus. ternal reproductive problems: stillbirth, prematurity, blood group sensitization.

ccurring in the present egnancy: vaginal bleeding, drugs used egnancy, acute illnesses, duration of rapture of membranes. iption of labor: duration, fetal presentation, fetal distress, fever. ivery: mode of delivery (vaginal or arean section), use of anesthesia or ations, use of forceps, Apgar score, need for resuscitation.

Growth and gestational age assessment: Physical signs may be useful in estimating gestational age at birth. Commonly used the new Ballard score (NBS), in which the gestational age is assist according to maturity of six physical signs which are; skin, languo hair, ears, breasts, genitals, and the planter surface creases. It's accurate to plus minus 2 wks

Apgar score It is a practical method of systematically assessing newborn infants immediately after birth to help identify infants requiring resuscitation. Its should be done at 1 st min. after delivery then repeated at 5 min, 10 min, and 20 min or according to the general status of the newborn.

Although the 1 - and 5 -minutes Apgar scores have almost no predictive values for longterm outcome, serial scores provide useful description of the severity of perinatal depression and the resuscitative efforts need. The Apgar score consist of 5 physical signs, as following:
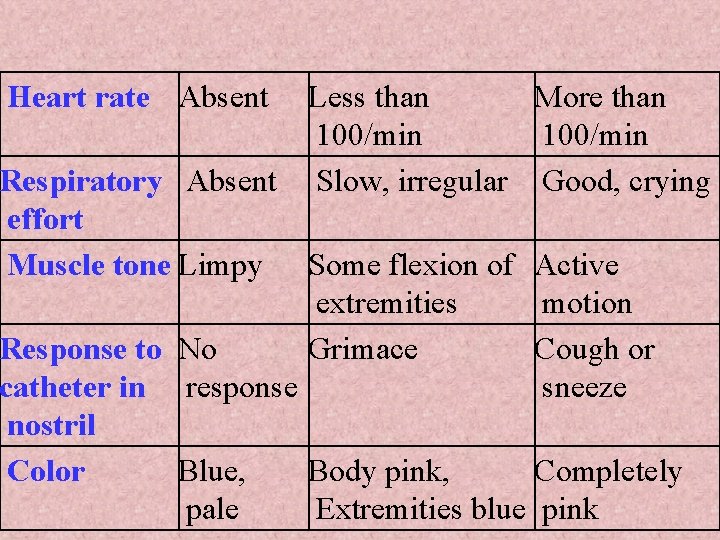
Heart rate Absent Less than More than 100/min Respiratory Absent Slow, irregular Good, crying effort Muscle tone Limpy Some flexion of Active extremities motion Response to No Grimace Cough or catheter in response sneeze nostril Color Blue, Body pink, Completely pale Extremities blue pink

Total score of 10 indicates an infant in the best possible conditions. nfant with a score of 0 -3 requires immediate resuscitation. Apgar score of 0 -3 at 20 min predicts high mortality and morbidity.

Care of the well newborn infants: 1. Maintenance of body heat: Infant should be dried immediately after birth and either wrapped in blanket or placed under warmer while having skin-toskin contact with the mother and if the newborn need resuscitation after birth, its should be done under radiant heat source.

Effects of cold injury on newborn infants: 1. Metabolic acidosis. 2. Hypoglycemia. 3. Hypoxemia. 4. Increased renal excretion of water and solutes.

2. Antiseptic skin and cord cares: duce the incidence of skin and umbilical infections (omphalitis), the lowing measures should be undertaken for any newborn infant : entire skin and cord should be ansed once infant temperature has abilized, with sterile cotton soaked in m water or a mild, non medicated soap.

ied and wrapped in sterile ets and taken to the nursery, the blanket can be discarded at the y door to reduce the chance of ng pathogenic organisms to the nursery. Daily treament of the umbilical cord with ple die, bactericidal agent or bacitracin reduce colonization with s. aureus and nic bacteria, or alternatively use chlorhexidine washing.

idly enforcing hand-to-elbow ing for 2 min initially and for 0 sec in the second wash for visitors entering the ery, shorter washes between ng infants should also be equired.

3. Eyes care: All infants should be protected against gonoccocal infection by installing 1% silver nitrate drops (best prophylactic therapy) or erythromycin 0. 5% and tetracycline 1% sterile ophthalmic ointments within 1 hr of birth.

4. Vitamin K: intramuscular injection of 1 mg of watersoluble vitamin K 1 is recommended for all infants immediately after birth to prevent hemorrhagic disease of newborn. Larger I. V. doses predispose to hyperbilirubinemia (jaundice) and kernicterus and should be avoided.

5. Feeding: The first feeding usually occurs by 3 hr of life in healthy term neonates, often as early as possible in the delivery room. You should encourage breast feeding, and the factors for successful breast feeding are: mediate postpartum mother –infant contact with suckling rooming-in. 2. Demand feeding.

sion of fathers in prenatal breast education and support from experienced women. oiding of pacifiers and supplemental formulas (unless medically indicated). Nursing should be at least 5 min at each breast, using both breasts, to allow a baby to obtain most of the available breast milk and to provide effective stimulation for creasing milk supply.

Indications that the baby is ready for feeding are: 1. Alertness and vigor. 2. Absence of abdominal distention. 3. Good bowel sounds. 4. Normal hunger cry. All of these signs are present within 3 -6 hr after birth in healthy term newborns, but are delayed in depressed and sick newborns.

Mechanism of first breath after delivery The initiation of the first breath after delivery depend on two major factors, which are removal of the lungs fluid and the presence of surfactant in the lungs.

Methods of removal of lungs fluid: By pulmonary circulation which increased y times at birth because of all the Rt. r output now perfuses the pulmonary vascular bed. y intermittent compressions of the chest during vaginal delivery. 3. By the pulmonary lymphatic. 4. Expelled by the infants. 5. Swallowed by the infants. 6. By aspiration from the orophyranx.

Factors impaired removal of lung fluids: 1. Cesarean section delivery. 2. Endothelial cells damage. 3. Hypoalbuminemia. 4. High pulmonary venous pressure. 5. Neonatal sedation.

Surfactant: Is lipoprotein synthesized and stored in type II alveolar cells composed of phosphatidylcholine (lecithin), phosphatidylglycerol, apoproteins (surfactant proteins (SP)-A, B, C, D) and cholesterol. Surfactant lining the alveoli enhances aeration of gas-free lungs by reducing surface tension, so it's lowering the pressure required to open alveoli

The opening pressure required to inflate the airless lungs are higher than those needed at any other period of life, they range from 10 -50 cm H 2 O compared with about 4 cm H 2 O for normal breathing in term infants and adults

This higher pressure to initiate respiration is required to: rcome the opposing forces of nsion (especially in small airways). come the viscosity of liquid remaining in the airways ntroduce about 50 ml of air in to the 20 -30 ml of which remains in the gs after the 1 st breathe to establish the tional residual capacity (FRC).

Stimulation factors of the 1 st breathe: 1. Decreased Po 2 and p. H and increased Pco 2 due to lack of placental circulation. 2. Redistribution of COP after umbilical cord clamping. 3. Decreased body temperature. 4. Various tactile stimuli.

Hypoxic-Ischemic encephalopathy Anoxia: refer to consequences of complete lack of oxygen. Hypoxia: refer to an arterial concentration of oxygen that is less than normal. Ischemia: refer to blood flow to cells or organs that is insufficient to maintain Their normal functions

Hypoxic-Ischemic encephalopathy (HIE): is a syndrome resulting from the effects of the hypoxia and ischemia on the brain cells. Its important cause of permanent damage to CNS cells, which may results in neonatal death (1520% of patients) or may be manifested latter as cerebral palsy or mental retardation (2530% of patients). HIE, passing clinically in 3 stages:
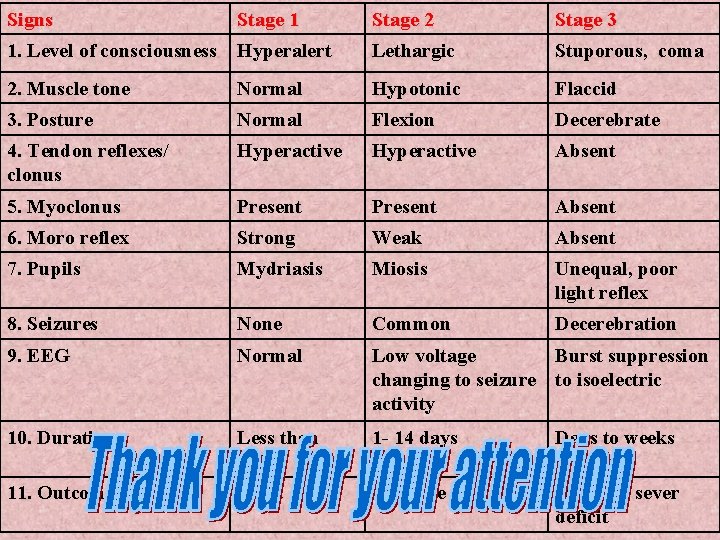
Signs Stage 1 Stage 2 Stage 3 1. Level of consciousness Hyperalert Lethargic Stuporous, coma 2. Muscle tone Normal Hypotonic Flaccid 3. Posture Normal Flexion Decerebrate 4. Tendon reflexes/ clonus Hyperactive Absent 5. Myoclonus Present Absent 6. Moro reflex Strong Weak Absent 7. Pupils Mydriasis Miosis Unequal, poor light reflex 8. Seizures None Common Decerebration 9. EEG Normal Low voltage Burst suppression changing to seizure to isoelectric activity 10. Duration Less than 24 hr 1 - 14 days Days to weeks 11. Outcome Good Variable Death or sever deficit
- Slides: 28