NeonatalPediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate















































- Slides: 58

Neonatal/Pediatric Cardiopulmonary Care Resuscitation

2 When To Resuscitate n Need usually related n Combination of n Can occur in

3 Causes of Fetal Asphyxia n n

4 Apnea

5 Effect of Asphyxia on Lungs n Initial adaption to extrauterine life requires 2 steps: – –

6 Effect of Asphyxia on Lungs Blood flow continues through d. a. & f. o. (by-passing lungs) Pulmonary hypertension Pulmonary vasoconstriction Asphyxia Apneic or ineffective respirations Negative pressure not generated to open Alveo li to push fluid out Pa. O 2 , Pa. CO 2 , p. H

7 Effect of Asphyxia on Lungs If asphyxia severe with lactic acidosis Ventilation alone will not change acid-base imbalance

8 Effect of Asphyxia on Lungs n In severe cases - might be beneficial to give HCO 3 to – – –

9 Effect of Asphyxia on Lungs n NOTE: Adequate ventilation must be maintained when bicarb given!!! Why? ?

10 Effect of Asphyxia on Lungs

11 Preparation For Resuscitation n

12 Basics of Neonatal Resuscitation 3 steps: n A- n B- n C-

13 Resuscitation Cycle Evaluation Decision Action

14 Steps in Resuscitation 1 st step =

15 Mechanisms of Heat Loss n Radiation – Loss to n Conduction – Loss to n Evaporation – Loss when n Convection – Loss to
16 Causes of Heat Loss n n n

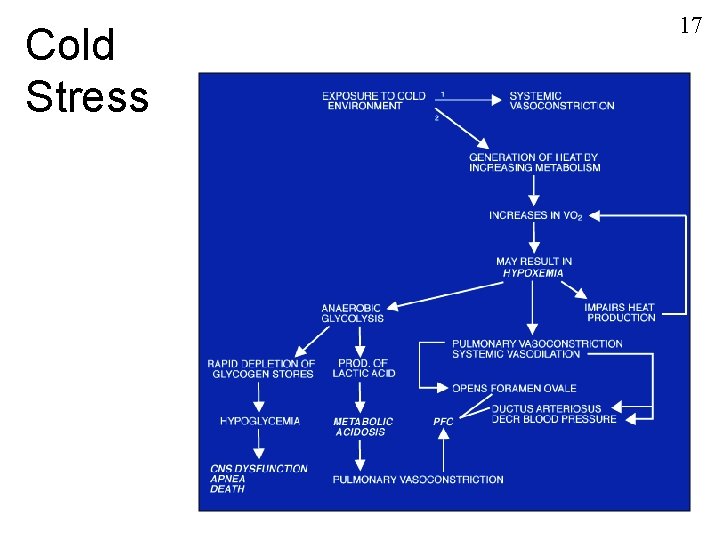
Cold Stress 17

18 Steps in Resuscitation Next Step = Open airway n n

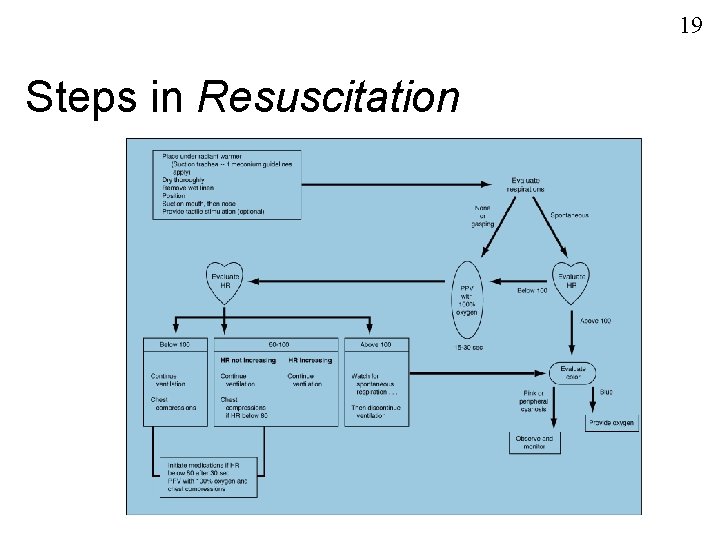
19 Steps in Resuscitation

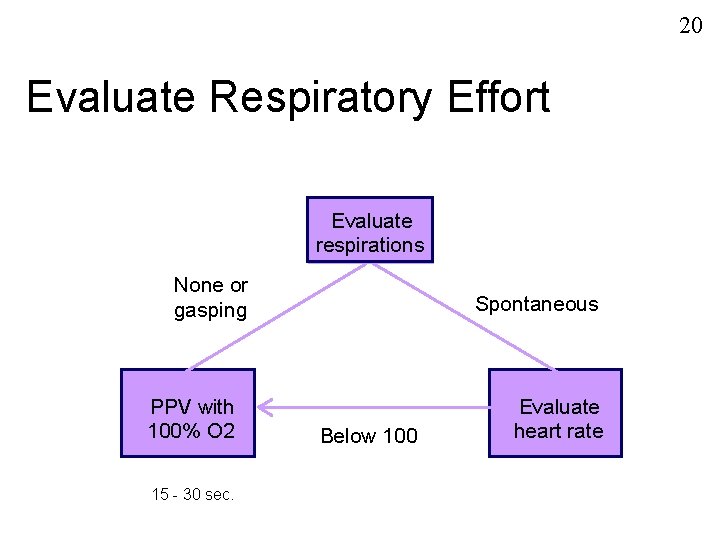
20 Evaluate Respiratory Effort Evaluate respirations None or gasping PPV with 100% O 2 15 - 30 sec. Spontaneous Below 100 Evaluate heart rate

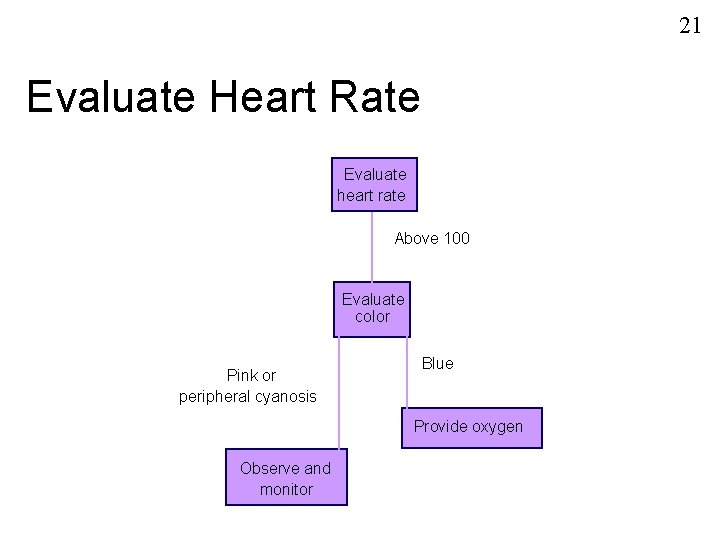
21 Evaluate Heart Rate Evaluate heart rate Above 100 Evaluate color Pink or peripheral cyanosis Blue Provide oxygen Observe and monitor

22 Indications for PPV n n

23 Positive Pressure Ventilation n Flow-inflating bag n Self-inflating bag n Pressure gauge n Oxygen flow 5 -8 lpm n Pop-off at 30 -40 cm. H 2 O

24 PPV Technique n n n Slightly extend neck Mask held with thumb & forefinger Bag squeezed with fingertips Initial rate Done for 15 -30 sec. , then re-evaluate May require -

25 Re-evaluate Heart Rate

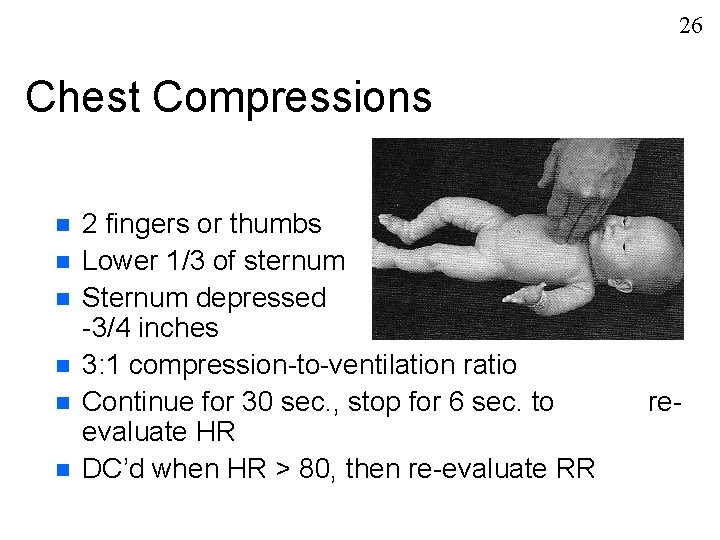
26 Chest Compressions n n n 2 fingers or thumbs Lower 1/3 of sternum Sternum depressed -3/4 inches 3: 1 compression-to-ventilation ratio Continue for 30 sec. , stop for 6 sec. to evaluate HR DC’d when HR > 80, then re-evaluate RR 1/2 re-

27 Indications for Intubation Bag/mask ventilation is difficult or ineffective n Prolonged PPV is required n Thick meconium is present in amniotic fluid n Suspicion of diaphragmatic hernia n

28 ETT Sizes

29 Laryngoscope Blades n Size 1 for n Size 0 for n

30 Intubation Technique n Same as adult n Limit attempts to - n Provide blow-by oxygen at - n ETT tip midway between carina & clavicles n Cut ETT to leave -

31 Medications - Uses n n n

32 Medications - Routes n n

33 Instillation Into ETT N A V E L O 2

34 Medications - Indications n HR < 80 despite PPV and chest compressions for at least 30 sec. n HR is 0

35 Epinephrine n Powerful sympathomimetic – – – 1 st drug given n IV or ETT, delivered rapidly n Repeated q 3 -5’ until HR n

36 Volume Expanders n Given if hypovolemic – BP – Pallor with adequate oxygenation – HR > 100 with weak pulses – Failure to respond to resuscitation Whole blood, 5% albumin, plasma expanders, NS n IV, may be repeated as needed n

37 Sodium Bicarbonate n Prolonged arrest & not responding n Alkaline to buffer metabolic acidosis n Only given when ventilation is adequate n IV

38 Narcan (naloxone) n Reversal of narcotic depression – Demerol (meperidine) – Morphine sulfate – Fentanyl (Sublimaze) n IV, IM, sub-q, ETT n Given rapidly

39 Dopamine n n n

40 APGAR Scoring n n

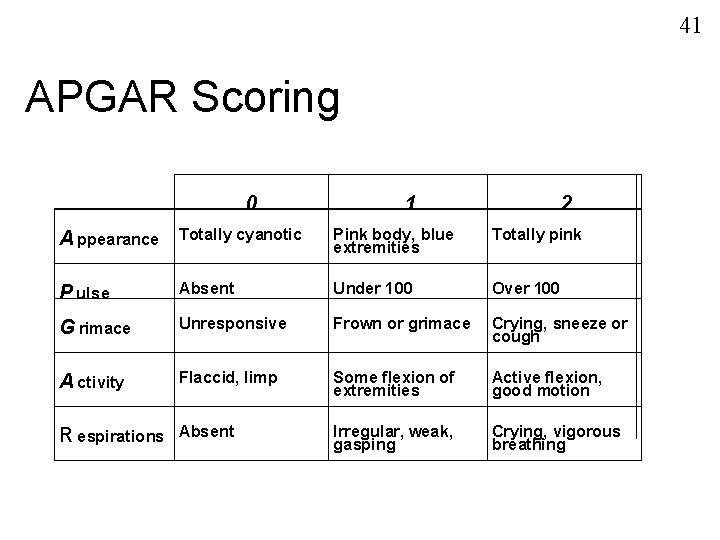
41 APGAR Scoring 0 A ppearance Totally cyanotic 1 2 Pink body, blue extremities Totally pink P ulse Absent Under 100 Over 100 G rimace Unresponsive Frown or grimace Crying, sneeze or cough A ctivity Flaccid, limp Some flexion of extremities Active flexion, good motion Irregular, weak, gasping Crying, vigorous breathing R espirations Absent

42 Serum Glucose Sources n Nutritional needs of fetus supplied by Mom & regulated by placenta n Fetus prepares for postnatal life by energy stores & developing enzymedependant processes for usage of stored energy

43 Serum Glucose Energy Storage n Glycogen – – n Triglycerides (brown fat) – –

44 Serum Glucose Post-delivery At 2 hours By 3 days -

45 Serum Glucose Hypoglycemia Term Preterm -

46 Hypoglycemia - Signs n n n Tremors Irritability or Moro reflex Apnea/tachypnea Cyanosis Seizures n n n Lethargy Hypothermia Weak/high-pitched cry Poor feeding Vomiting CV failure

47 Hypoglycemia

48 Hypoglycemia - Causes n n n n Hyperinsulinism Prematurity IUGR Starvation Sepsis Shock Asphyxia n n n n Hypothermia Glucogen Storage Disease Galactosemia Adrenal insufficiency Polycythemia Congenital heart defects Iatrogenic causes

49 Hyperinsulinism n Fetus of diabetic Mom n Rh incompatibility n Insulin-producing tumors n Maternal tocolytic therapy (ritodrine, terbutaline)

50 Glucose Measurement n Glucose Test Strip “Dextrostik” n “One Touch” n Lab sample (blood glucose)

51 Hypoglycemia Treatment Early feeding (oral) n D 10 W n – 200 mg/kg bolus over 1 -3 minutes – Con’t IV, 4 -8 mg/kg/min. until feedings started n Treat cause

52 Umbilical Blood Sampling n n

53 Umbilical Vein Catheter (UVC) n Usually placed in - n Drug administration during -

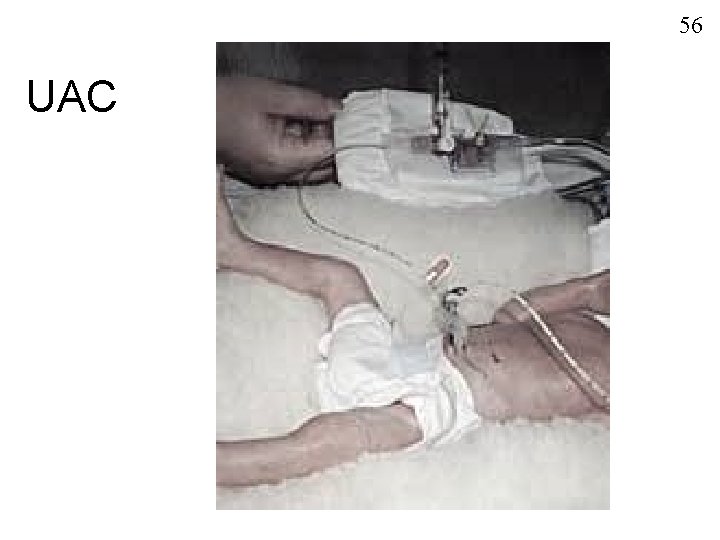
54 Umbilical Artery Catheter (UAC) Indications n n n

55 Umbilical Artery Catheter (UAC) Placement 5 Fr. catheter (>1250 g), 3. 5 Fr. catheter (<1250 g) n Sterile procedure n Heparinized-filled catheter n Tip L 3 -4 for low catheter, T 8 for high catheter (in aorta below renal a. , above bifurcation of femoral a. ) n

56 UAC

57 Umbilical Artery Catheter Complications n n n

58 Umbilical Artery Catheter Sampling Technique n n