Neonatal Sepsis Steve Spencer MD Objectives Review of

Neonatal Sepsis Steve Spencer, MD

Objectives • • • Review of terminologies associated with neonatal infections Review risk factors for neonatal infections Review presentations of neonatal sepsis Review most common organisms and treatments We will concentrate on the child <3 months of age

Cases • You are on-call tonight when the ER calls with two kids

Cases • Kid 1 • • • 9 week old, term baby 100. 6 temp Looks well CBC WNL UA clean Everyone at home with colds • Kid 2 • • • 12 day old, term baby Fever to 101 Jaundiced Seizures WBC of 3. 2 K PLT of 89 Do you treat these kids the same or different and why?

Your Text

Terminologies • • Rule out sepsis Neonate with fever Neonatal sepsis Serious Bacterial Infection (SBI) Occult Bacteremia Neonate- the first month 28 days of life Infant- up to one year

Back When I was an Intern…. . • • Any kid 3 months or less with fever got admitted Kids stayed longer If it sneezed, writhed, wiggled or wheezed, it got an LP Kids had to crawl seven miles through the snow, up hill both ways, to daycare…. .

Age Groups • • • Currently ages 0 -28 days automatically admitted by most clinicians 1 -3 months is a grey zone guided by clinical opinion Greater than three months generally not admitted

Why Have Recommendations Changed? • • GBS prophylaxis Immunizations • HIB, Pneumococcus • • Better understanding of neonatal physiology Better laboratory techniques Better understanding of the disease Different antibiotics

Definition of Fever • • “Gold Standard” is generally thought of as 100. 4 (38. 0) rectally with a glass mercury thermometer Lots of ways to take a baby’s temperature • I recommend using a quality thermometer • When in doubt, let the pros sort it out • In Newborn Nursery, need to counsel parents about significance of fever in neonate

Why the Worry? • • • Neonatal immune system immature Perinatal exposure to pathogens via birth canal High rate of infection in kids less than 3 months with fevers • >4% age 0 -28 days with bacteremia or meningitis (drops to 1% by 3 months) • Almost 10% with UTI • Rates increase with degree of fever • • 39 C with >10% rate of bacteremia Well appearing infant may have an infection

Why not admit everybody? • • • Not without risk of hospital acquired infection Cost Lost time to parents at work Family stress etc

What data supports our practice? • • Rochester criteria Philadelphia criteria Boston criteria Etc

Risk Factors • • • Prematurity and low birth weight Maternal GBS Prolonged rupture of membranes Maternal chorioamnionitis Sibling with sepsis Meconium at delivery Need for resuscitation Male child Multiple gestation
“Early” Pathogens (first week) • Group B Strep (GBS) • • • Incidence used to be 4 -6/1000 live births (0. 4%) Now <0. 1% after prenatal screening guidelines E. coli • Every few decades flips back and forth with GBS as most common cause • Gram negative rods (esp. in urine) • Occasional Salmonella sepsis • • • Listeria monocytogenes Herpes Simplex Enterovirus

“Late” Pathogens (~1 -2 weeks) • • GBS or group A strep Enterics/Enterococcus in urine HSV Enterovirus, RSV, Flu

Community Acquired (after 4 -6 weeks) • • Pneumococcus Meningococcus GABHS Haemophilus influenzae (HIB) not really a problem anymore

Signs/Symptoms Most by themselves mean little, but three (or two) strikes and you are Out! • Temperature irregularity • Fever • Hypothermia • Tone and Behavior • • • Poor tone Weak suck Shrill cry Weak cry Irritability • Skin • • • Poor perfusion Cyanosis Mottling Pallor Petechiae Unexplained jaundice

Signs/Symptoms • Feeding Problems • Vomiting • Diarrhea • Abdominal distension • Hypo or Hyperglycemia • Cardiopulmonary • • Tachypnea Retractions Tachycardia for age Bradycardia in first few days of life • Hypotension for age • Low PO 2

Signs/Symptoms • • • Sunken fontanelle Bulging or pulsating fontanelle Neck stiffness CAN NOT be used Babies can be bacteremic but look well Presence of a “cold” does not change anything
PIDJ April 2005 • Study in India found that any two of these signs had an almost 100% sensitivity for sepsis and over 90% mortality • • • Reduced sucking Weak cry Cool extremities Vomiting Poor tone Retractions

Labs • • Normal WBC (5 -15 K) is better than high WBC is better than very high WBC (over 35 K) which is better than very low WBC (<5 K) Less than 28 days- blood, urine, CSF cultures +/stool • Get urine culture, even if UA WNL • • >28 days see handout CXR if respiratory symptoms

Lab Dilemmas- Urine collection • Don’t use bag urines! • A negative culture on a bag urine is negative • A positive means nothing • Cath or Suprapubic aspirate? • SPA- any growth is considered a positive • Cath • • Can have false positives, especially if uncirc’d male New debates on what constitutes a positive culture Most references use >10 K CFU’s as positive, some use as little as 1 K (equals one plaque) Microbiologists feel we should use 100 K on all samples regardless of source

Lab Dilemmas- The Bloody Tap
The Bloody Tap • Don’t ask me, you should have gotten it right the first time

The Bloody Tap • • No right answer Results can vary based on the amount of blood in amount of CSF, what is the HCT, what is the peripheral WBC count etc. Some use CBC to CSF ratios. Sometimes seems like too many WBC’s or seems OK Sometimes just need to re-tap

Treatment • Age 0 to ~4 -6 weeks • • Ampicillin/Aminoglycoside Ampicillin/Cefotaxime Amp kills GBS and Listeria Gent and Cefotaxime for GNR’s • Ceftriaxone not used- causes neonatal hepatitis and biliary sludging

Aminoglycosides • Disadvantages • Ototoxicity • Nephrotoxicity • Need for levels • Advantages • Little resistance • Cheap (30 cents or so a dose) • Highly concentrated in urine • No need for levels if QD dosing in a 48 hour admission

Treatment • After 4 -6 weeks, ampicillin and a 3 rd generation cephalosporin • Offers better coverage for community acquired organisms • At 4 -8 weeks, switch to cephalosporin alone.

What About Herpes? • • Some clinicians begin acyclovir on all neonatal admissions for fever We use the guideline of “Fever Plus” • HSV is rare & tends to present in certain ways • Fever in addition to • • • Hepatitis/jaundice Meningitis Seizures Thrombocytopenia Vesicles Rash/purpera

HSV Risk Factors • Maternal history- only present in • Maternal primary infection- as many as 50% of babies infected • • • Active lesions ROM > 4 -6 hours Fetal scalp electrode Prematurity Caregiver with cold sore/fever blister

HSV in Neonate • Three types • • • SEM (Skin, Eye, Mucous membranes)- 15% Isolated CNS- 35% Disseminated (+/- CNS)- 50% • 75% HSV-2 25% HSV-1 • Incidence 1: 1 K-5 K births
HSV timing • • • SEM (Skin, Eye, Mucous membranes)- can be early Isolated CNS- 2 -3 weeks Disseminated (+/- CNS, +/-SEM)- ~1 week
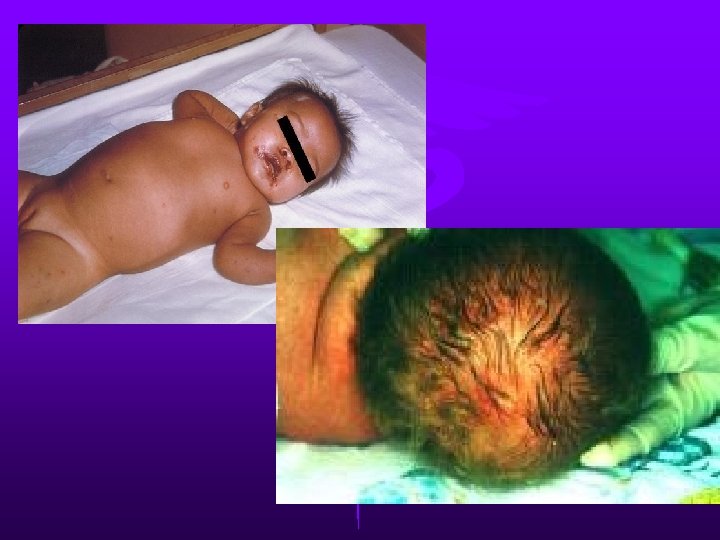

HSV Labs- three points • CSF PCR alone DOES NOT rule out HSV

HSV Labs- if do it, do it right • • • CSF for PCR (>98% sensitive, >95% specific) and/or culture (30 -50%) CSF tends to be “bloody”– 100 -200 RBC with elevated WBC Mucous membrane cultures • Eyes, ears, anus, mouth, nose, vesicles if present, some add urine • In nursery, wait 24 hours after birth to culture (indicates active infection)

HSV Labs cont. • LFT’s • I now get for any R/O SBI kid that I am worried enough about to get a BMP • Serial CBC’s • Thrombocytopenia • Leukopenia • • • Tzank smear of lesions(~40% sensitive, not specific) DFA or EIA of lesions (80% sensitive) Serology NOT useful
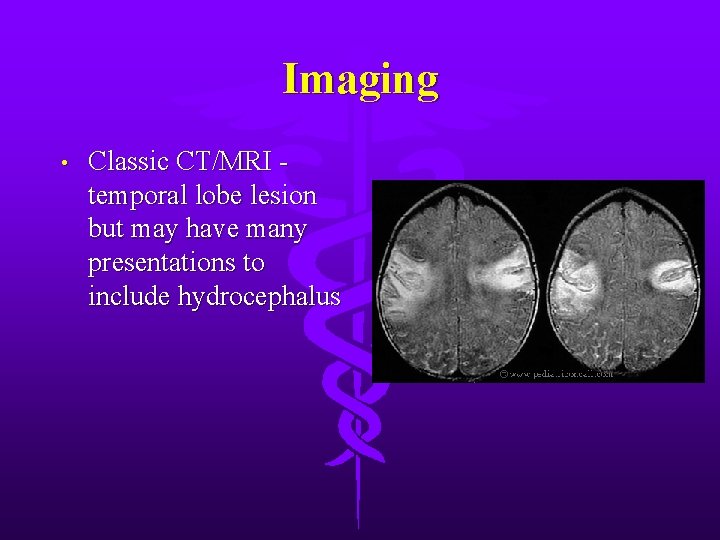
Imaging • Classic CT/MRI temporal lobe lesion but may have many presentations to include hydrocephalus

HSV treatment • Acyclovir 20 mg/kg/dose Q 8 hrs • • • SEM only- 14 days Disseminated (no CNS)- 21 days CNS- at least 21 days (PCR must clear)

Cases • Kid 1 • • • 9 week old, term baby 100. 6 temp Looks well CBC WNL UA clean Everyone at home with colds • Kid 2 • • • 12 day old, term baby Fever to 101 Jaundiced Seizures WBC of 3. 2 K PLT of 89
- Slides: 40