NEONATAL SEPSIS Definition generalized infection commonly bacterial during


NEONATAL SEPSIS
![*Definition -generalized infection [commonly bacterial] during the first 4 weeks of life associated with *Definition -generalized infection [commonly bacterial] during the first 4 weeks of life associated with](http://slidetodoc.com/presentation_image_h2/590251aec4aef4d662e647194e6743d6/image-3.jpg)
*Definition -generalized infection [commonly bacterial] during the first 4 weeks of life associated with general systemic manifestations and positive blood culture. -In 40% of cases associated with meningitis.

CAUSITIVE ORGANISMES *Organism most commonly associated with early-onset infection include: - Group B streptococcus, E. coli, H. influenzae, Klebsiella, L. monocytogens. *Orgasnism most commonly associated with late onset sepsis: Coagulase– negative staphylococci, staphylococcus aures, E. coli

Klebsiella, Pseudomonas GBS candida, anaerobes, streptococcus pneumonae, N. meningitis. Viruses such adenovireus, RSV, rotavirus, HSV, CMV, HIV may present with a late onset sepsis-like picture
: *Pathophysiology: *Cellular immunity: T-cells represent an immature population Which donot proliferate as adult T-cells when activated and donot effectively produce cytokines.

Natural killer cells are found in small number and are functionally immature. Also memory T-cells are deficient. Neonatal neutrophils or polymorphonuclear cells is deficient in chemotaxis and killing capacity. *Humoral immunity:

Igm levels are generally low at birth unless the infant was exposed to an infection during pregnacy. Ig. G and Ig. E levels are low. Complement cytotoxic components that lead to killing of organisms especially gram negative bacteria are deficient, this dificiency is more marked in preterm infant. Intrinsic factors in NICU like plastic mediums found in intravascular catheters and nasal tubes Enhance organisim attachment to the

Surface of catheter, the adherance creats acapsule between microbes and catheter preventing C 3 deposition and phagocytosis.

Predisposing factors 1 -maternal infection before delivery e. g UTI, bacterial endocarditis, septecemia. 2 -Preterm labour. 3 -Preterm premature rupture of membranes (prior to 37 comlete weeks). 4 -Prolong rupture of membrane (more than 18 hour before delivery). 5 -Maternal tempreture 38 c or higher during labour.

6 -prematurity and low birth weight or infant who required hospitalization and manipulation as infants of diabetic mothers. 7 -babies with congenital defects leading to exposure of entenal organes as meningoceles or omphalocels. 8 -mothers with no antenatat care, poor hygiene, low socioeconomic status, cervicitis not treated well…etc.

*CLINICAL MANIFSTATIONS ONSET: -early onset septicemia : present atfirst week of life. -late onset septicemia : appear 8 -28 days after delivery.

*C LINICALL FEATUERS: 1early: hypothermia more common than fever specially prematur e, poor suckling , lethargic, hypo tonic. 2manifestations in established case: -GIT: vomiting, conistipation, diahrrea, … -RS: tachepnea, apnea, RD, cough. -CVS: tachycardia, bradycardia, cyanosis, …

-CNS: convultions, tremers, bulking anterior fontanelle, abscent mororeflex, … -BLOOD: juandice, aneamia, purpura, … 3late manifestations: organomegaly, direct hyperbilurubinemia, DIC, convultions.

*Diagnosis: A History. B Clinical manifstations. C investigations: 1sepsis work-up: which include: -blood cultur. -csf analysis and cultur. -urine analysis and cultur. -gasteric aspirate gram staine in the first 24 hrs after birth. -buffy coate smear. -cultur from any septic focus.
![2indirect evidence of bacterial infections: -CBC: aneamia, leucocytosis[mor than 30 , 000], leucopenia[lessthan 3, 2indirect evidence of bacterial infections: -CBC: aneamia, leucocytosis[mor than 30 , 000], leucopenia[lessthan 3,](http://slidetodoc.com/presentation_image_h2/590251aec4aef4d662e647194e6743d6/image-16.jpg)
2indirect evidence of bacterial infections: -CBC: aneamia, leucocytosis[mor than 30 , 000], leucopenia[lessthan 3, 000]with increased neutrophils specialy immatur form[band celles], thrombocytopenia. -Increased ESR and c-reactive protein. 3other investigations: -serum bilurubin. -chest x-ray[pneumonia]. -Blood gases, p. H, HCO 3, RFT, LFT.

*TREATMENT 1General: -care of feeding. -anti convulsunts. -warming. -fresf blood transfution. -care of the umblical cord. -fluid and electrolyte balance. -ventiletory assistance.

2specific: -acombination of antibiotics are given till the result of cultur sensetivity are available. acombination of ampicllin and gentamycine or cefotaxime and amycacine are given by the i. v roote. -treatment is continuoed for 10 -14 days.

Dose of drugs: Ampicillin: if less than 7 days <2 kg: 50 -100 mg/kg/24 hrs divided 12 hrly >2 kg: 75 -150 mg/kg/24 hrs divided 8 hrly If more than 7 days <2 kg: 75 -150 mg/kg/24 hrs divided 8 hrly >2 kg: 100 -200 mg/kg/24 hrs divided 6 hrly

High dose penicillin 250, 000 u/kg/24 hrs is appropriate for GBS meningitis. Gentamicin: Preterm<30 wks 2. 5 mg/kg/24 hrs once. Preterm>30 wks 2. 5 mg/kg/dose given 12 hrly Term: <7 days 5 mg/kg/24 hrs once or divided 12 hrly Term: >7 days 2. 5 mg/kg/dose 8 hrly

Cefotaxime: 100 mg/kg/24 hrs given 12 hrly

*Prognosis: With early diagnosis and treatment, infant are not likely to experience long term health problems associated with neonatal

Sepsis, however, if early signs and-or risk factor are missed, the mortility rate increases. Residual neurologic damage occure in 15 -30% of neonates with septic meningitis.

Not all neonates with poor feeding, vomiting, diarrhea, lethargy and hypoglycemia have neonatal sepsis , you have to think of metabolic inborn error.

*ACUTE BACTERIAL MENINGITIS -DEFENITION: acute inflammation of the membranes covering the brain and spinal cord with evidence of bacteria and polymorphonuclear leucocyte in the csf.

*ETIOLGY 1in neonatal period : E. colli, Klebsiella, proteu and pseudomonas, group. B strepto cocci and lesteria monocytogens are important causative organisms. 2in infancy and childhood : H. influenza, pneumococci and meningococci.

PATHOGENSIS Most commonly result from heamatogenous spread of microorganisms from adistant of infection or direct spread of organism. *CLINICAL PICTURE: 1Acute onset of fever , poor feeding, … 2manifestations of increased intracranial pressure. 3distrubted consciousness from drowsiness up to coma.

4convulsions. 5signs of meningeal irritation. 6purpura and shok. 7paralytic manifestations.

DIAGNOSIS 1clinnical picture. 2investigations: -lumbar puncture for CSF analysis. -Blood cultuer and cultuer from escarping of skin lesions in cases of meningococcal septicemia. -CT. SCAN of the brain.
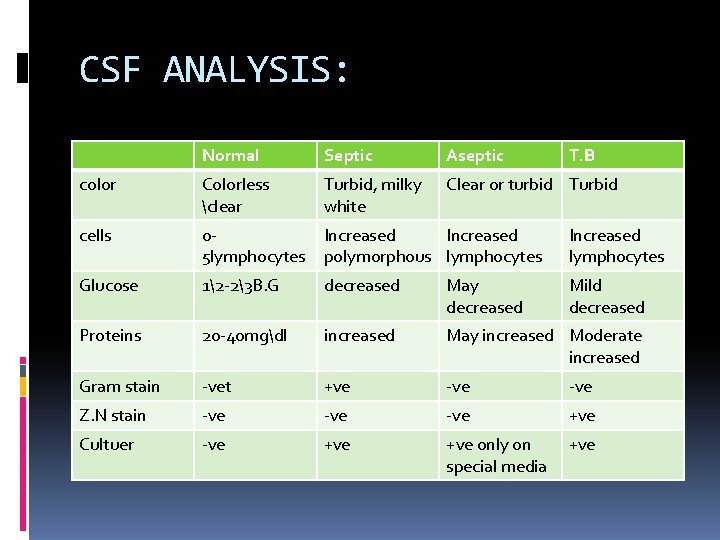
CSF ANALYSIS: Normal Septic Aseptic T. B color Colorless clear Turbid, milky white Clear or turbid Turbid cells 05 lymphocytes Increased polymorphous lymphocytes Increased lymphocytes Glucose 12 -23 B. G decreased May decreased Mild decreased Proteins 20 -40 mgdl increased May increased Moderate increased Gram stain -vet +ve -ve Z. N stain -ve -ve +ve Cultuer -ve +ve only on special media +ve
![COMPILICATIONS 1hydrocephalus 2subdural effution. 3vascular collaps[shok]. 4metastatic infections. 5defrent forms of paralysis. 6brain damage COMPILICATIONS 1hydrocephalus 2subdural effution. 3vascular collaps[shok]. 4metastatic infections. 5defrent forms of paralysis. 6brain damage](http://slidetodoc.com/presentation_image_h2/590251aec4aef4d662e647194e6743d6/image-31.jpg)
COMPILICATIONS 1hydrocephalus 2subdural effution. 3vascular collaps[shok]. 4metastatic infections. 5defrent forms of paralysis. 6brain damage with its seguelae.

MANGEMENT: 1prevention. 2Treatment of the patients: A. general: -Antipyretics, care of feeding , Anticonvulsunt, frosamide and manetol for increased ICP, medical and neurological asessmsnt of the pt, IV dexamesasone. B. specefic: -commbination of ampicillin – Gentamycin or ampicillin and cefotaxim are used till the cultuer results are available. Therapy is continuo for 10 -14 days or 3 weeks.

C. Treatment of compilications. -hydrocephalus for neurosergery. -subdural effution: dialy tapping of the subdural space through the lateral angle anterior fontanelle.

- Slides: 34