Neonatal Resuscitation Objectives List the indications for neonatal

Neonatal Resuscitation

Objectives • List the indications for neonatal resuscitation • Prepare the articles needed for the procedure • Explain the steps in neonatal resuscitation • Demonstrate the procedure of neonatal resuscitation

Neonatal resuscitation 10% neonates require some assistance at birth. 1% neonates need extensive resuscitative measures. Asphyxia accounts for 20 -25% newborn deaths.

How does a baby receive oxygen before birth? Oxygen diffuses across placenta from mother’s blood to baby’s blood. Lungs receive very little blood. Alveoli are fluid filled rather than air.
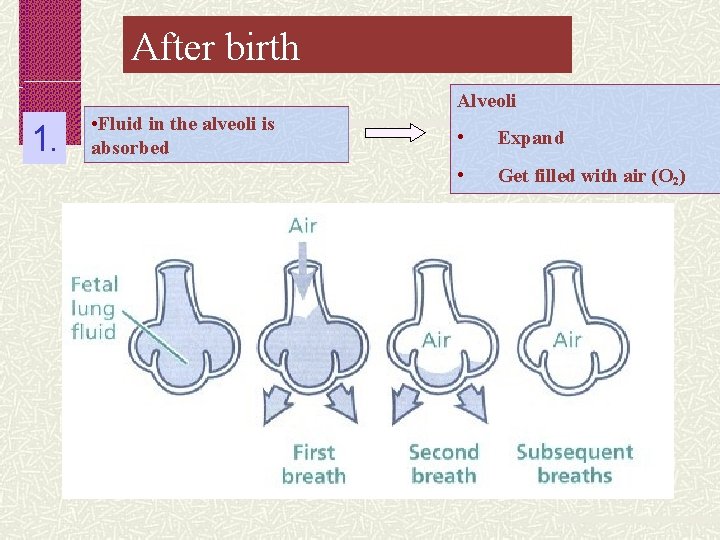
After birth Alveoli 1. • Fluid in the alveoli is absorbed • Expand • Get filled with air (O 2)
After birth 2. Umbilical arteries and veins are clamped Sudden increase in systemic blood pressure
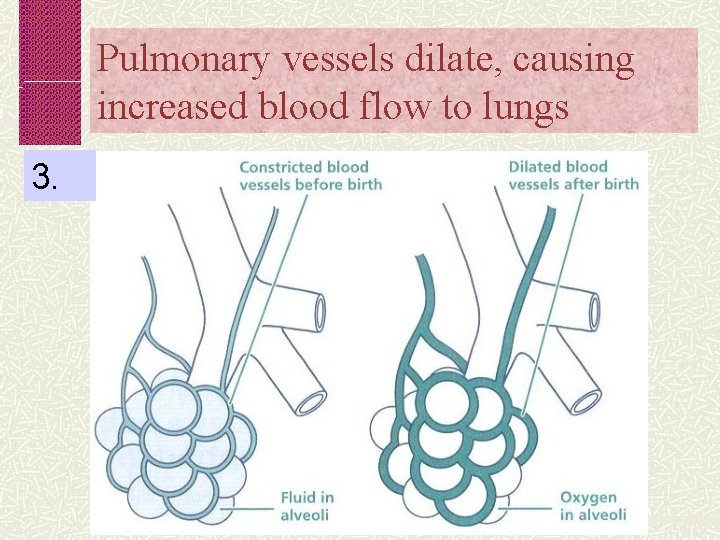
Pulmonary vessels dilate, causing increased blood flow to lungs 3.
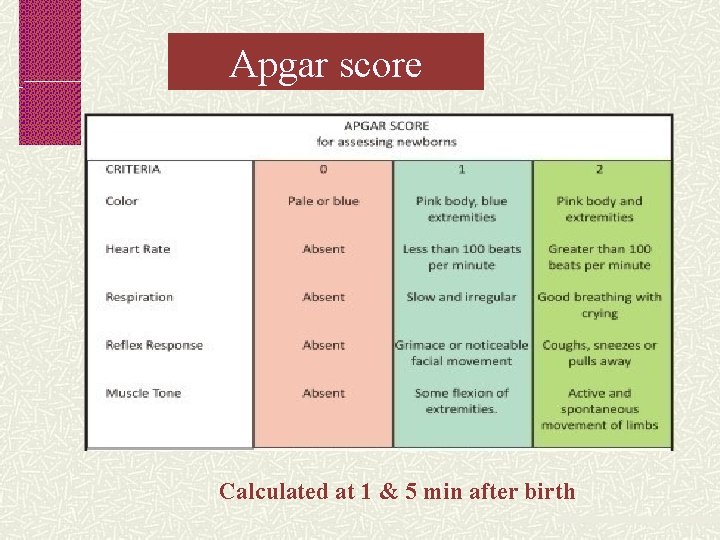

Apgar score Calculated at 1 & 5 min after birth

Consequences of interrupted transition 1. 2. 3. 4. The compromised baby may exhibit 1 or more of the following clinical findings: Low muscle tone Respiratory depression (apnea / gasping) Bradycardia Cyanosis

Antepartum Risks Maternal diabetes Chronic maternal illness Cardiovascular Thyroid Neurological Pulmonary renal Pre eclampsia Maternal infection Polyhydramnios Oligohydramnios Premature rupture of membranes IUGR/preterm Fetal malformation Maternal substance abuse No antenatal care Post term gestation Multiple gestation Anaemia Age <16 or > 35

Intrapartum Risks Emergency CS Instrumental delivery Abnormal position Premature labour Precipitous labour Chorioamnionitis Prolonged rupture of membranes Prolonged labour > 24 hrs Prolonged 2 ndstage of labour Fetal bradycardia Non-reassuring fetal heart rate pattern General anaesthesia Narcotics administered within 4 hours of delivery Meconium stained liquor Prolapsed cord Abruptio placentae Placenta previa

Fetal asphyxia Primary apnoea Apnoeic Blue Heart rate Resuscitate easily Secondary apnoeic White, floppy Heart rate Require active resuscitation

Equipment Needed for Resuscitation Radiant warmer Warm towel and blankets Resuscitation bag and mask Self inflating bag Anaesthetic bag Endotracheal tubes Laryngoscope Stethoscope Oxygen source and tubing Suction source and tubing Drugs and fluids Syringes, needles, cannulae, IV lines +/-Umbilical lines
Equipment Needed Overhead radiant warmer
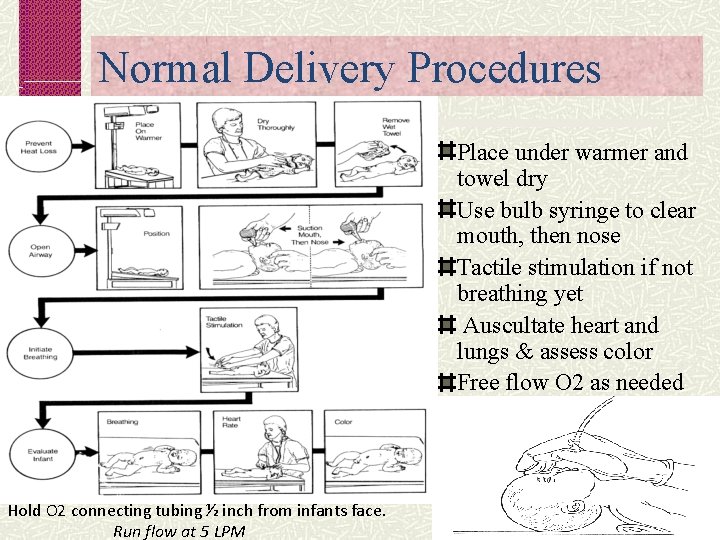
Normal Delivery Procedures Place under warmer and towel dry Use bulb syringe to clear mouth, then nose Tactile stimulation if not breathing yet Auscultate heart and lungs & assess color Free flow O 2 as needed Hold O 2 connecting tubing ½ inch from infants face. Run flow at 5 LPM

Steps in Resuscitation Warmth and stimulation and assessment for the 1 st 30 seconds Use warm cloth Replace when wet Rapidly assess Tone Colour Respiratory effort

Steps in Resuscitation - ABCDE Airway Clear airway if required Removal of secretions if present Suction mouth and nose DO NOT SUCTION IF AIRWAY IS CLEAR Positioning Supine or lateral Head in neutral or slightly extended position
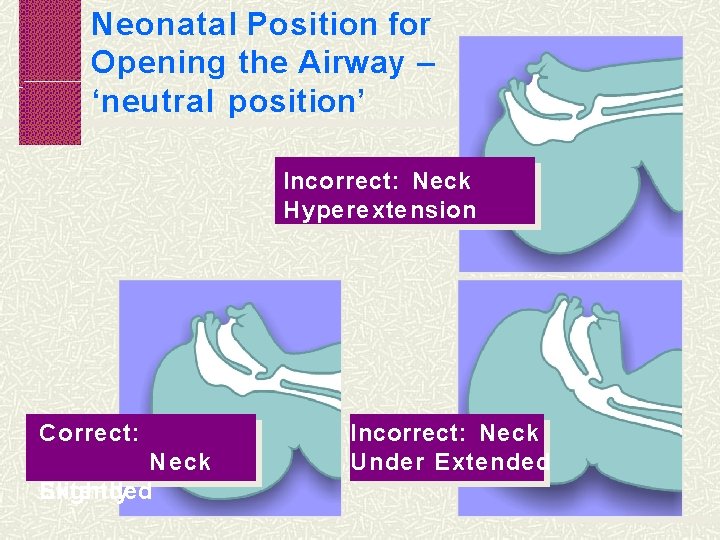
Neonatal Position for Opening the Airway – ‘neutral position’ Incorrect: Neck Hyperextension Correct: Neck Extended Slightly Incorrect: Neck Under Extended
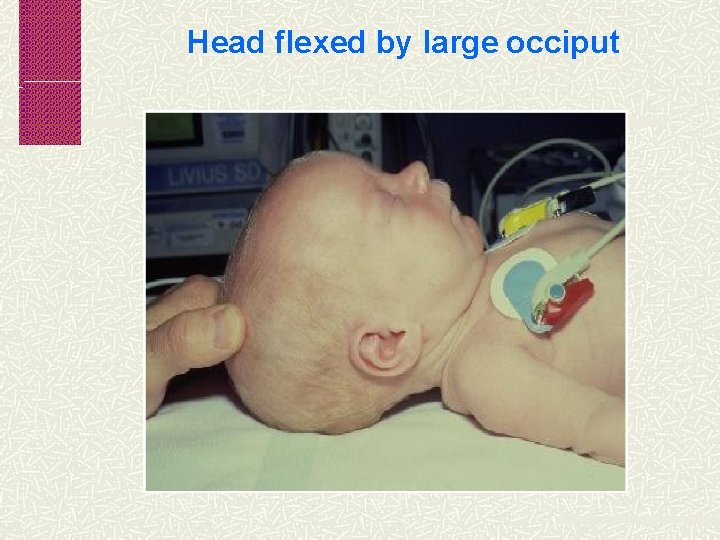
Head flexed by large occiput
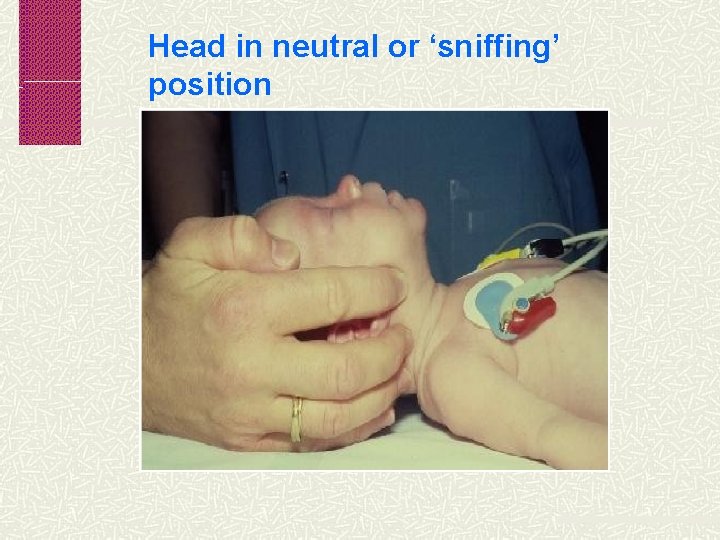
Head in neutral or ‘sniffing’ position
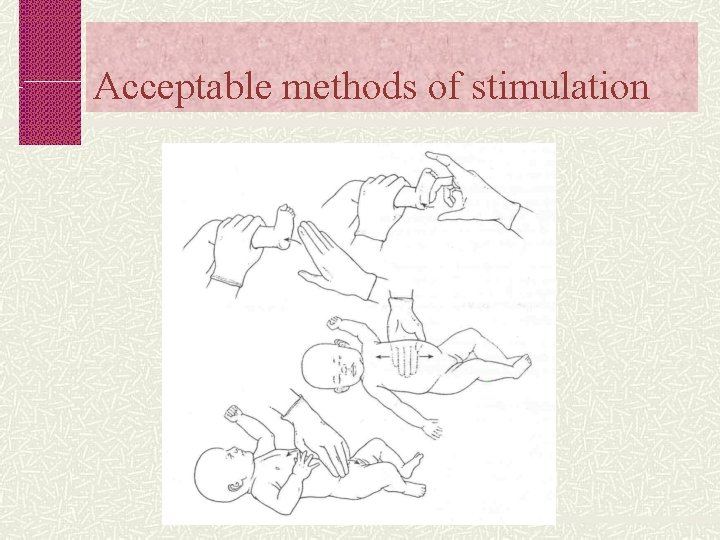
Acceptable methods of stimulation

Steps in Resuscitation - ABCDE Breathing Assessment of respiratory effort and colour Indications for oxygen administration Cyanosis Respiratory distress Give free flowing oxygen 5 L/min
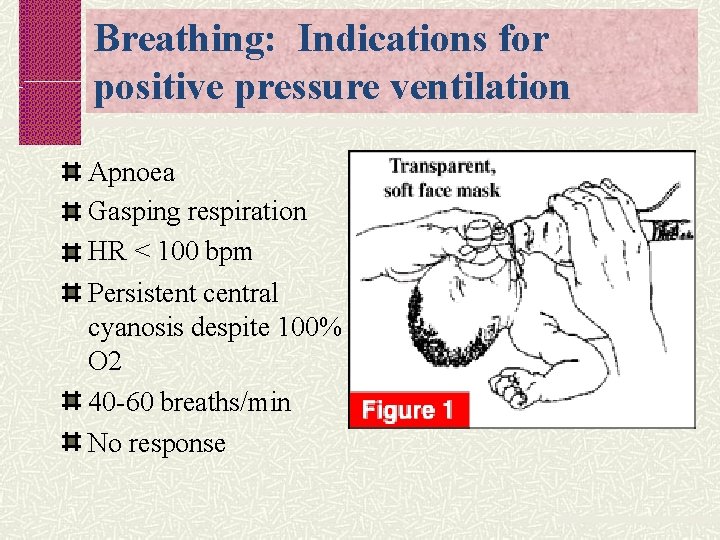
Breathing: Indications for positive pressure ventilation Apnoea Gasping respiration HR < 100 bpm Persistent central cyanosis despite 100% O 2 40 -60 breaths/min No response
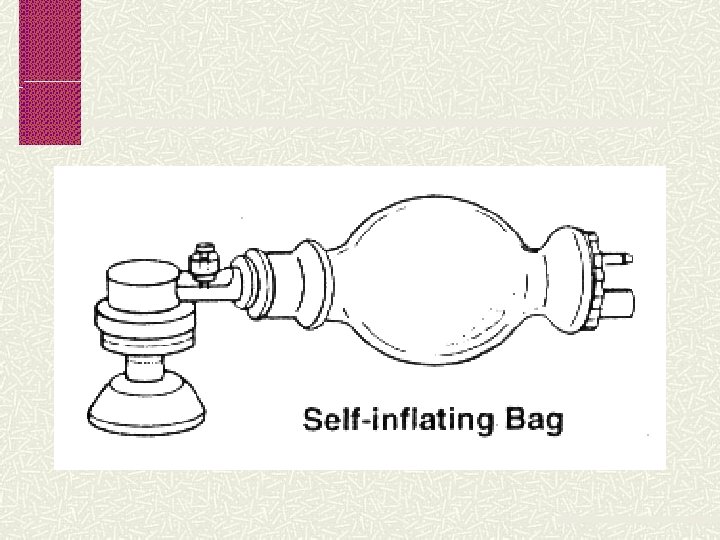
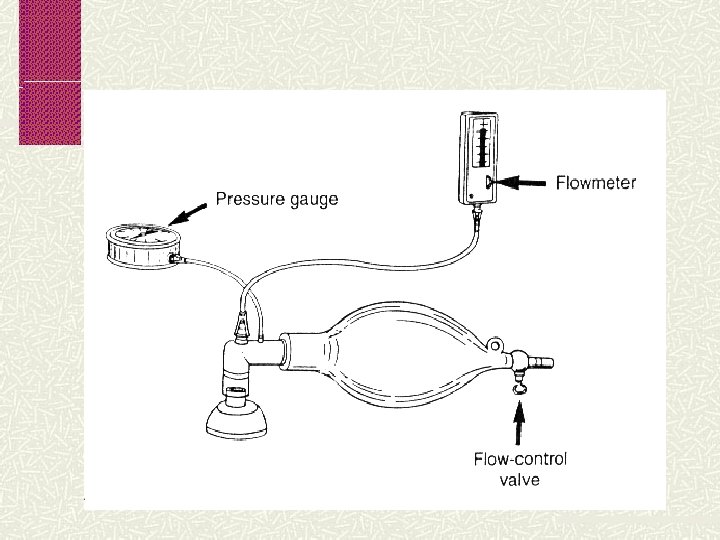

Watch for slight rise of chest Rate is 40 -60
Indications of endo-tracheal Intubation Prolonged positive-pressure ventilation (PPV) required Bag & mask ineffective: Inadequate chest expansion If chest compressions required: Intubation may facilitate coordination and efficiency of ventilation Tracheal suction required

Steps in Resuscitation - ABCDE Circulation Assessment of heart rate and response to previous measures Umbilical arteries Apex beat Auscultation
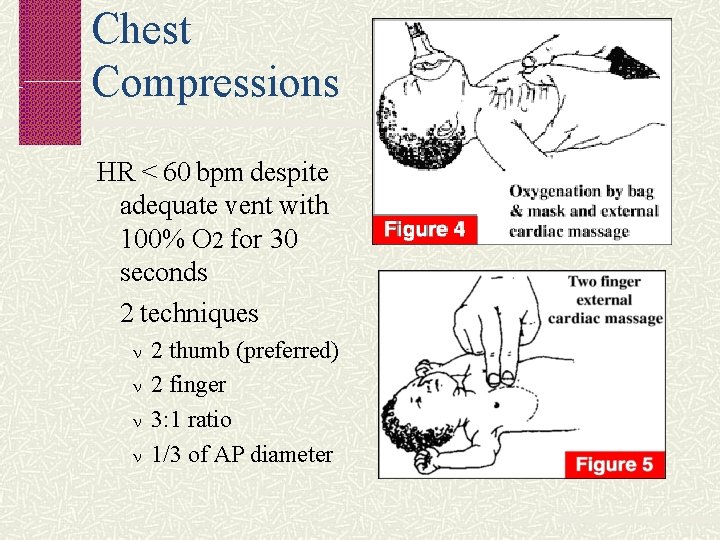
Chest Compressions HR < 60 bpm despite adequate vent with 100% O 2 for 30 seconds 2 techniques 2 thumb (preferred) 2 finger 3: 1 ratio 1/3 of AP diameter
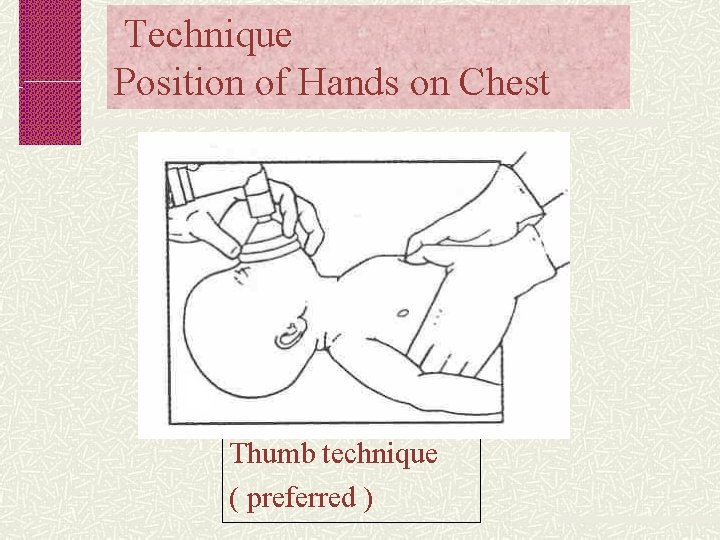
Technique Position of Hands on Chest Thumb technique ( preferred )
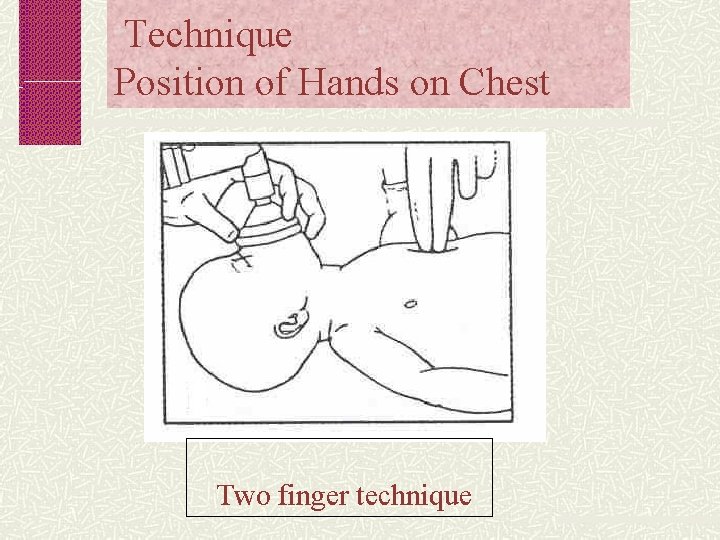
Technique Position of Hands on Chest Two finger technique
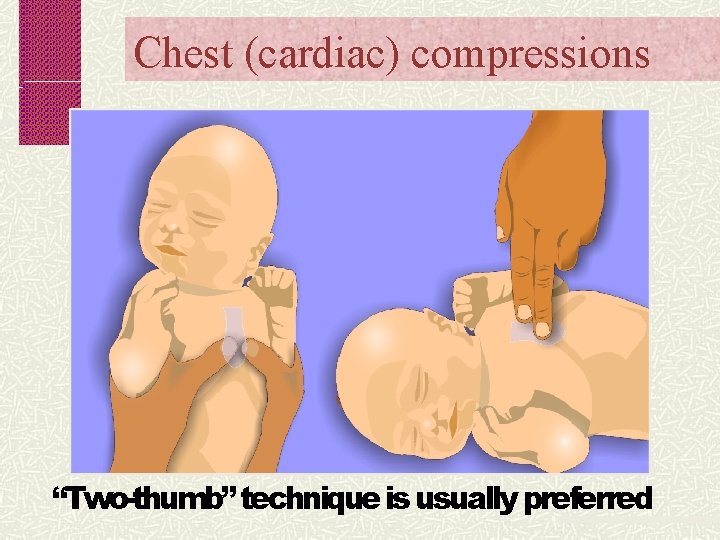
Chest (cardiac) compressions “Two-thumb” technique is usually preferred

Steps in resuscitation - ABCDE Drugs Adrenaline Volume Expanders Naloxone

Epinephrine Indications HR <60 /min after PPV & CC for 30 secs Route of administration Intravenous Endotracheal route (when I. V line is not secured ) Recommended Conc. – 1: 10, 000 (0. 1 mg/ml) Route – UVC/ IV Dose – 0. 01 -0. 03 mg/kg , (0. 05 -0. 1 mg/kg E. T) Rate of admn. – as rapidly as possible Repeat dose if no response after 60 seconds Now, intravenous route is first preferred route

Volume Expander Indications: Poor response to other resuscitative measures Evidence of blood loss or suspected ( pale skin, poor perfusion, weak pulse) Crystalloid Normal Saline Ringer Lactate or O-negative blood cross-matched with mother’s blood Dose – 10 ml/kg Route – Umbilical vein Preparation – large syringe Rate of administration – 5 -10 min

Naloxone Narcotic antagonist Indications : A history of maternal narcotic administration within the past 4 hours Severe respiratory depression is present after PPV has restored a normal HR & color Recommended Concentration: 1. 0 mg/ml Route: Intravenous Dose: 0. 1 mg/kg

Meconium present and baby vigorous Vigorous Baby- Strong respiratory efforts, Good muscle tone, Heart rate > 100 bpm suction catheter or bulb syringe for suction of mouth or nose ET suction not required

Meconium baby Airway is aggressively cleared prior to drying if infant is meconium stained AND baby is NOT vigorous! Use ET tube as a suction device

Meconium present and baby not vigorous Insert laryngoscope Clear mouth and posterior pharynx Insert endotracheal tube into the trachea Attach the ET to suction source Apply suction as ET is slowly withdrawn Repeat as necessary until no meconium or heart rate indicates further resuscitation

What to do if still no improvement? If no improvement seen despite all efforts Ensure adequate ventilation, chest compressions, drug delivery If still HR < 60/min, consider Airway malformation Lung problems Pneumothorax Diaphragmatic hernia Cong. Heart disease If HR absent or no progress Ethical considerations of when to D/C Resuscitation

Discontinuing Resuscitative Effort Stop resuscitation, if HR remains undetectable for 10 - 15 min Also take into consideration factors such as presumed etiology of the arrest, gestation of the baby, presence or absence of complications
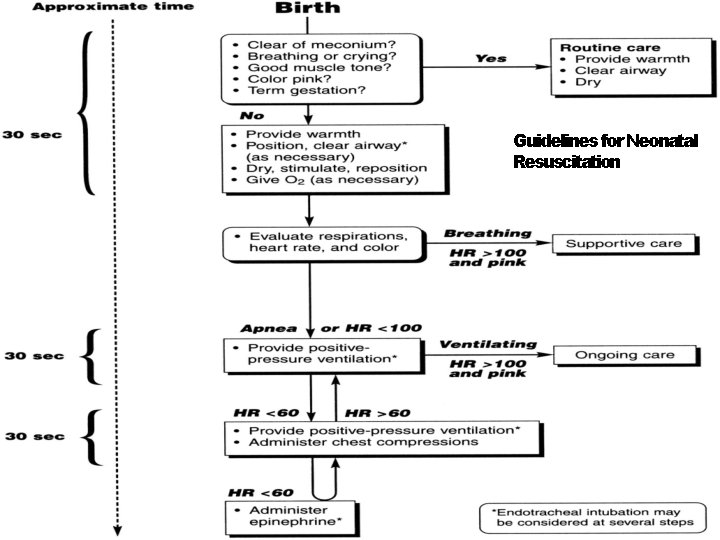
Guidelines for Neonatal Resuscitation

- Slides: 45