Neonatal resuscitation NNR Dr Renu Singh Burden of

Neonatal resuscitation (NNR) Dr. Renu Singh

Burden of the problem Birth asphyxia 23% of the 1 million neonatal deaths in India Long term neurological complications Death NNR (Neonatal resuscitation) : simple, inexpensive, cost effective method • Problem: NNR often not initiated, incorrect use of methods • • •

Successful NNR: factors 1. 2. 3. 4. Anticipation: call a skilled personnel Adequate preparation Accurate evaluation, algorithm based Prompt initiation of support

1. Anticipation: High risk delivery • Maternal condition – Advanced maternal age , DM, HT, stillbirth, fetal loss, early neonatal death • Fetal condition – Prematurity, post maturity, congenital anomalies, multiple gestations • Ante partum complications: APH, oligo /polyhydramnios • Delivery complications – Malpresentation, MSAF, instrumental delivery, antenatal asphyxia with abnormal FHR

2. Adequate preparation • Radiant warmer is turned on, & is heating • Oxygen source is open with adequate flow through the tubing • Suction apparatus tested, functioning properly • Laryngoscope is functional with bright light • Resuscitation bag & mask demonstrates an adequate seal & generation of pressure
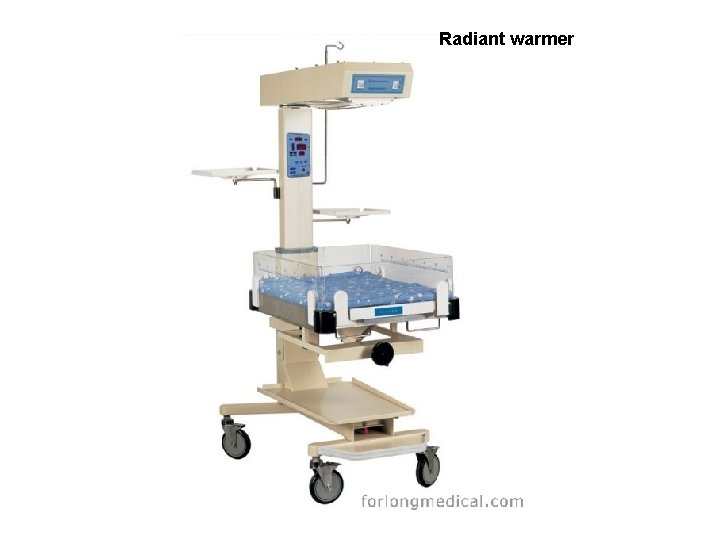
Radiant warmer





Successful NNR: factors 1. 2. 3. 4. Anticipation: call a skilled personnel Adequate preparation Accurate evaluation, algorithm based Prompt initiation of support

Evaluation, algorithm based • Rapid assessment of neonate clinical status • Is the infant full term? • Is the infant breathing or crying? • Does the infant has good muscle tone? • Yes: no resuscitation, routine neonatal care • No: needs resuscitation
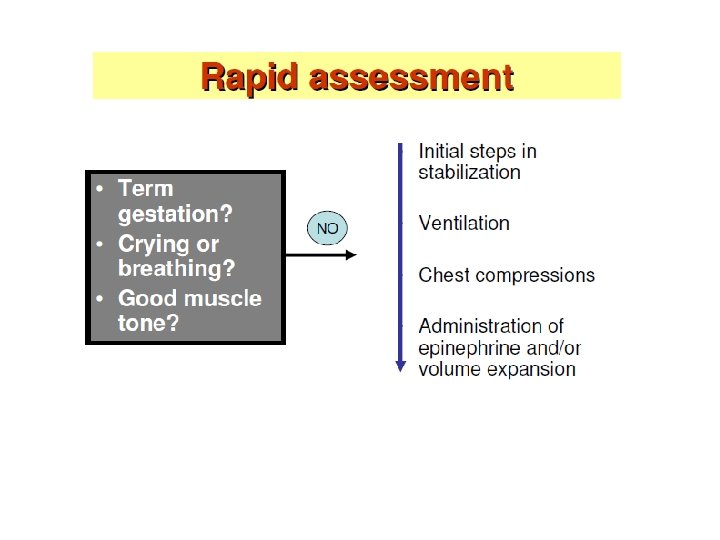

Approach to resuscitation 2010 AHA, AAP • A: initial steps(provide warmth, clear airway if necessary, dry, stimulate) • B: breathing(ventilation) • C: chest compressions (circulation) • D: administration of drugs &/or volume expansion

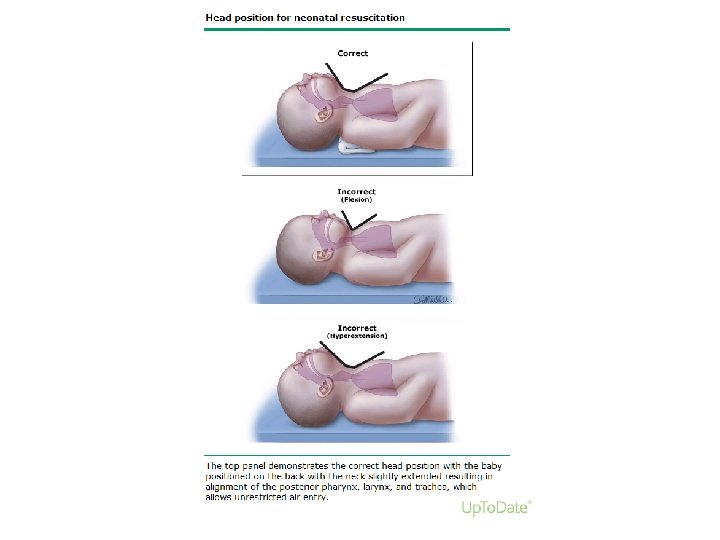
Resuscitation: initial steps • • • Provide warmth Head position “ sniffing position” Clearing the airway, if necessary Drying the baby Tactile stimulation for breathing
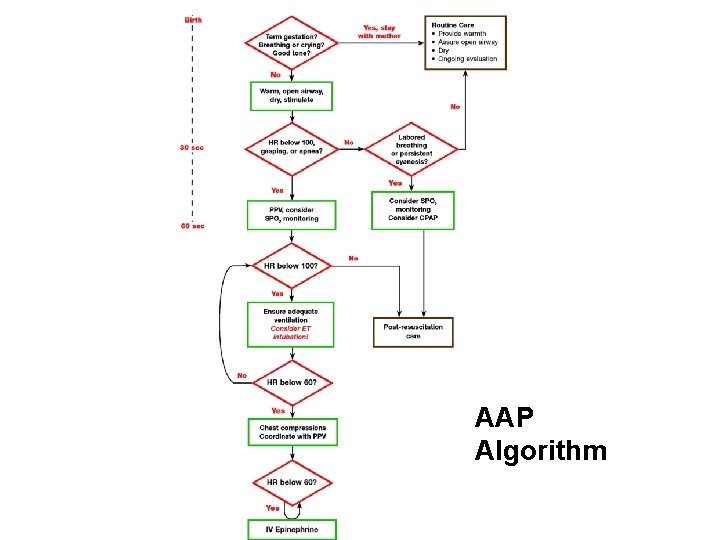
AAP Algorithm
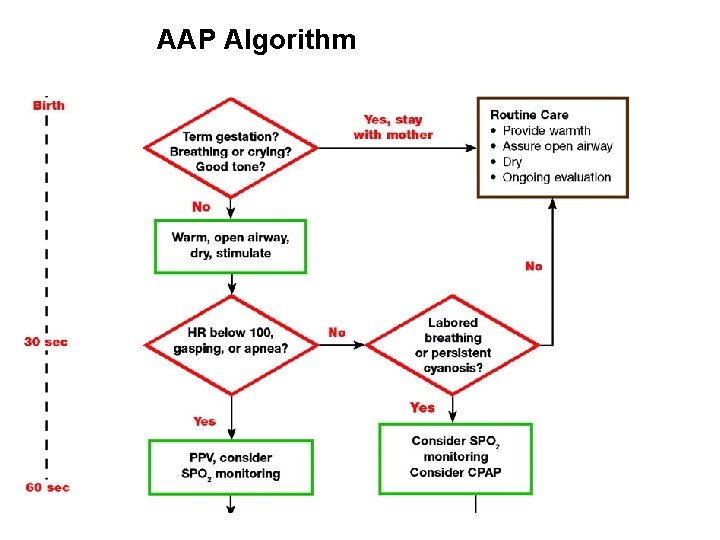
AAP Algorithm


PPV: Positive pressure ventilation Form of assisted ventilation Needed when there is no improvement in HR Also assess chest wall movements Should be delivered at rate of 40 -60 breaths /min, maintain HR>100 /min • Devices: BMV, ET (endotracheal tube), LMA(laryngeal mask airway) • •

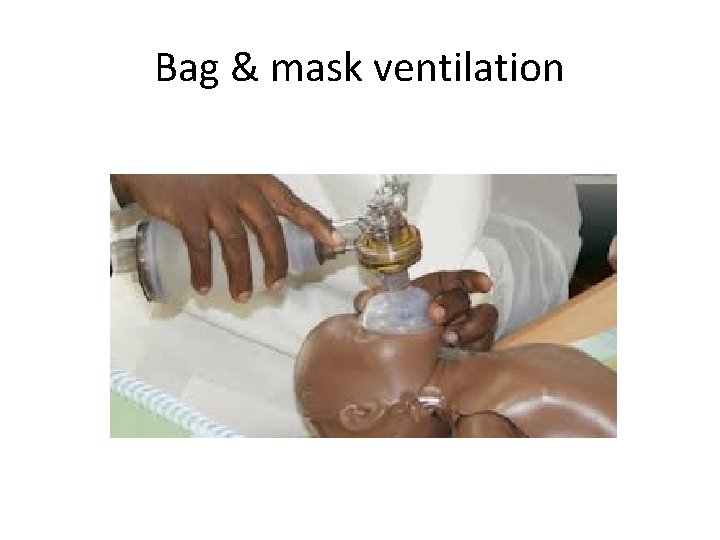
Bag & mask ventilation
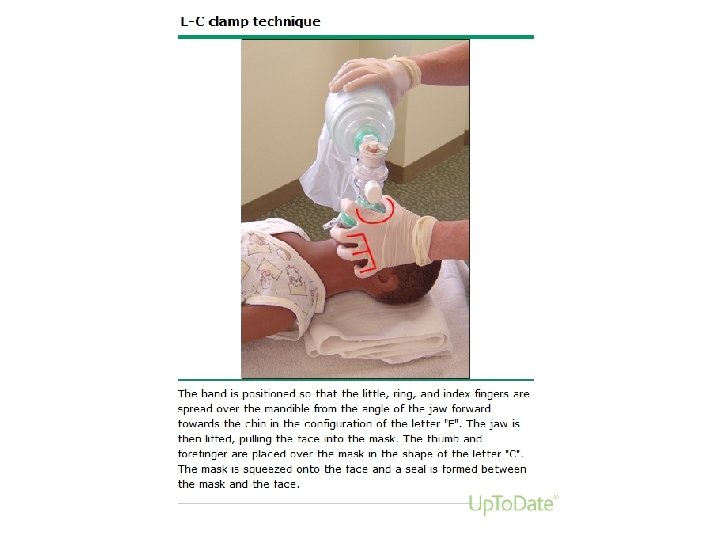

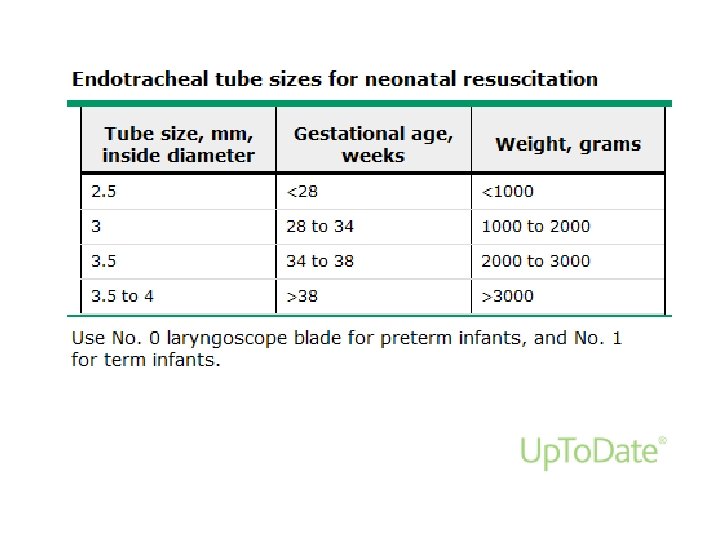
Endotracheal tube • If BMV is ineffective/prolonged • When chest compressions are performed • Initial endotracheal suctioning of non vigorous meconium stained newborn
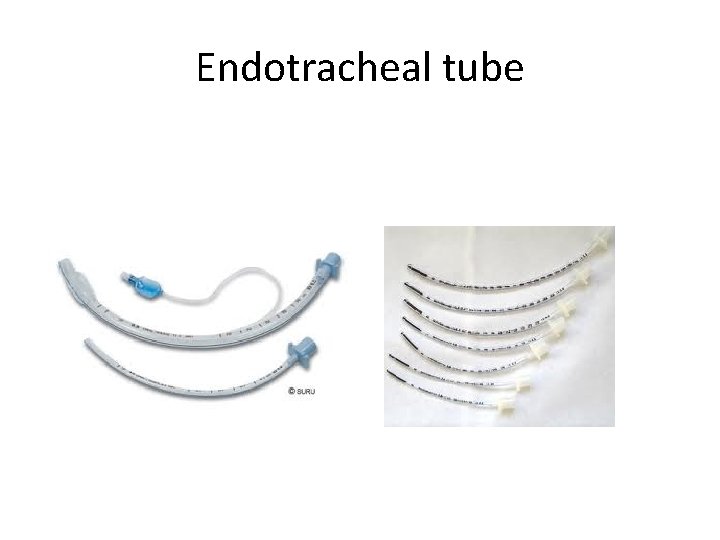
Endotracheal tube

LMA(Laryngeal mask airway) • Soft mask, fits over laryngeal inlet when inflated, occludes the oesophageal opening • Done when BMV is unsuccessful & tracheal intubation is unsuccessful or not feasible
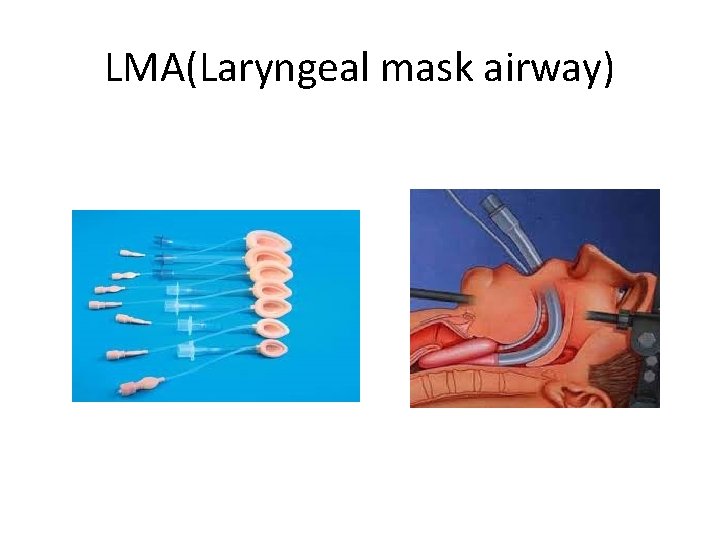
LMA(Laryngeal mask airway)
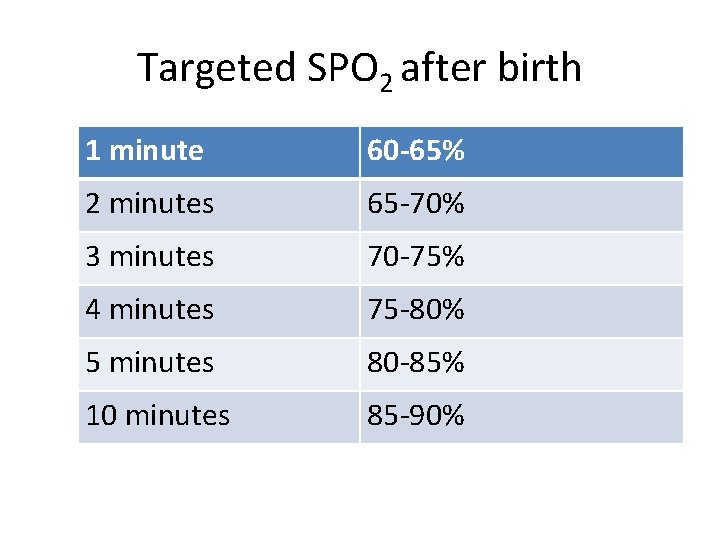
Targeted SPO 2 after birth 1 minute 60 -65% 2 minutes 65 -70% 3 minutes 70 -75% 4 minutes 75 -80% 5 minutes 80 -85% 10 minutes 85 -90%
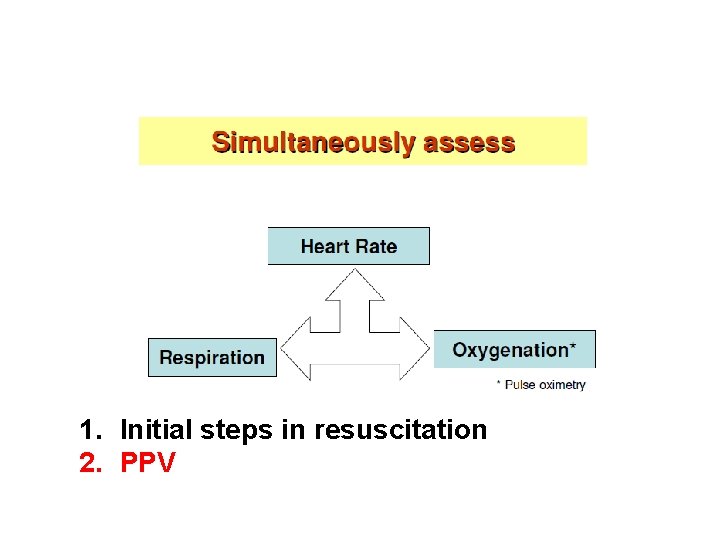
1. Initial steps in resuscitation 2. PPV
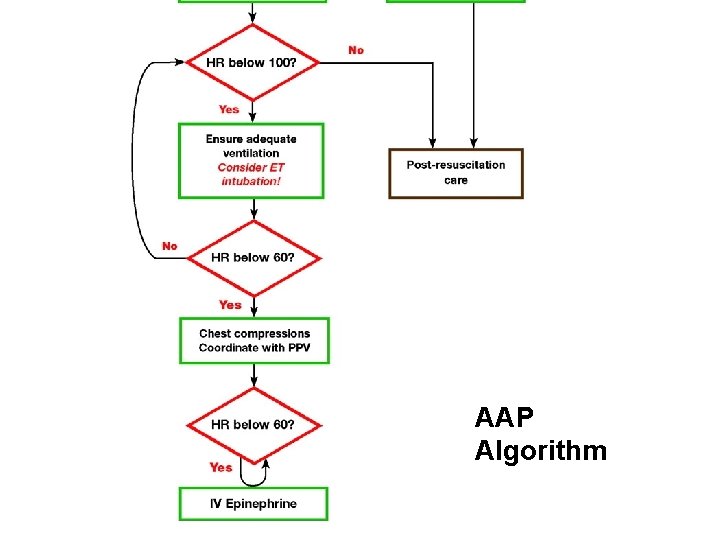
AAP Algorithm

Chest compressions • Started when HR<60 per minute despite adequate ventilation with 100% oxygen for 30 sec • Delivered at lower third of sternum, to depth 1/3 of AP diameter of chest • 2 techniques: – 2 thumb-encircling hands technique – Compression with 2 fingers , second hand supporting the back – 3: 1 ratio: : [ 90 comp: 30 ventilations]
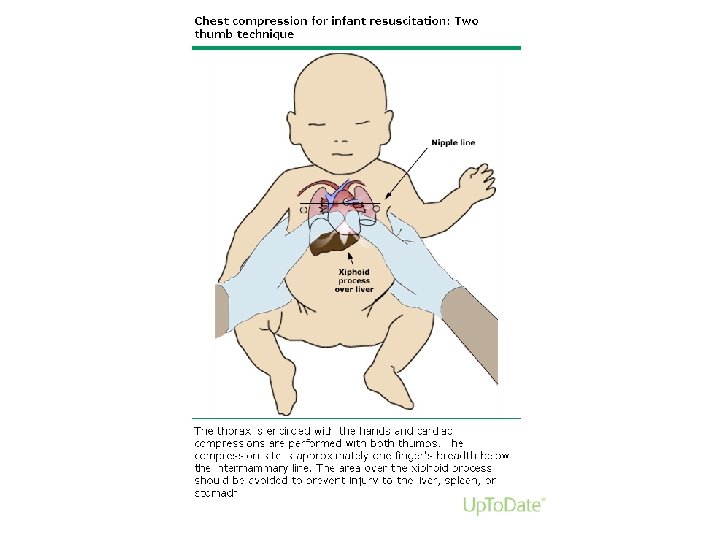
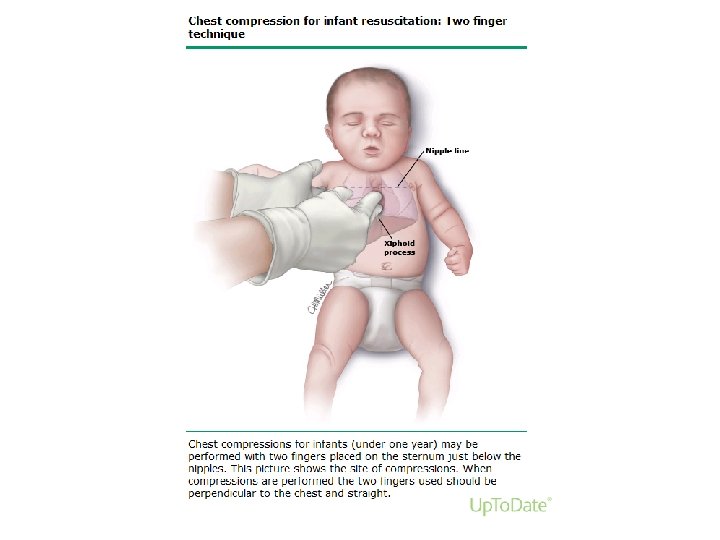
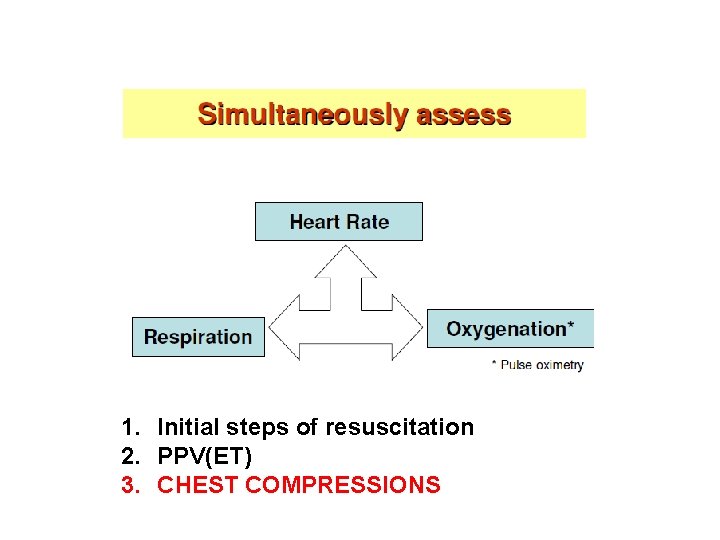
1. Initial steps of resuscitation 2. PPV(ET) 3. CHEST COMPRESSIONS

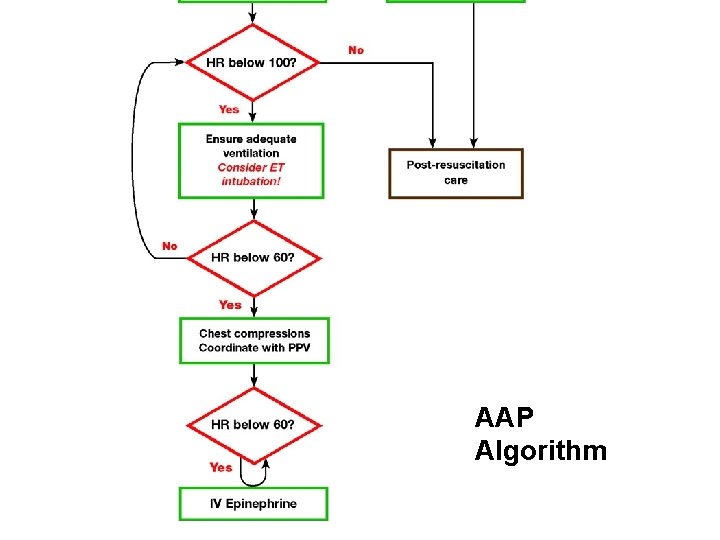
AAP Algorithm

Medications • Rarely indicated • Most important step to treat bradycardia is establishing adequate ventilation • HR remains <60 bpm, despite adequate ventilation(ET) with 100% Oxygen & chest compressions • Epinephrine or volume expansion or both

Epinephrine • Route of administration: intravenous(IV), ideal • Recommended dose: 0. 01 -0. 03 mg/kg per dose • Desired concentration: 1: 10, 000 0. 1 mg/ml

Volume expansion • • Suspected or known blood loss Isotonic crystalloid solution ; normal saline Blood Dose calculation: 10 ml/kg
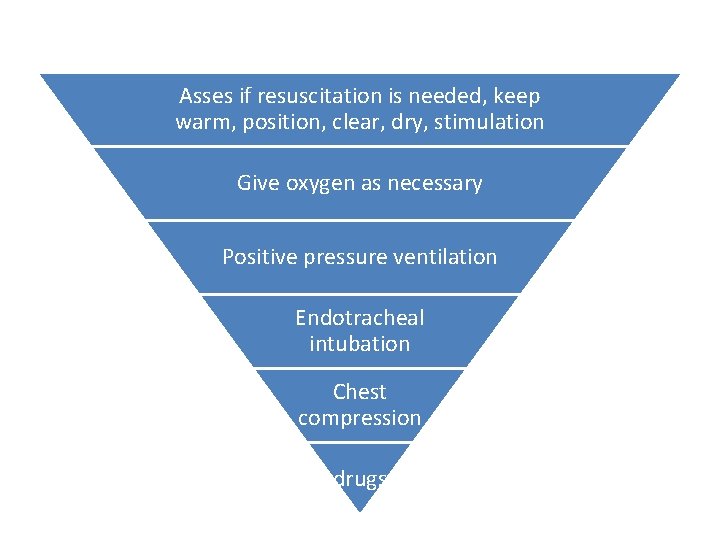
Asses if resuscitation is needed, keep warm, position, clear, dry, stimulation Give oxygen as necessary Positive pressure ventilation Endotracheal intubation Chest compression drugs

The golden minute • <30 seconds: complete initial steps • • Warmth Drying Clear airway if necessary Stimulate • 30 -60 seconds: assess 2 vital characteristics • Respiration (apnea/gasping/labored/unlabored) • Heart rate (<100/>100 bpm) • Golden Minute Project: skill based training
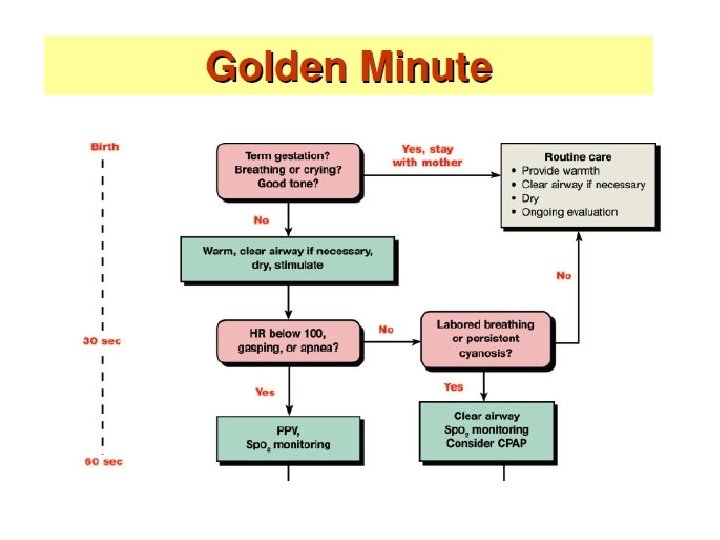
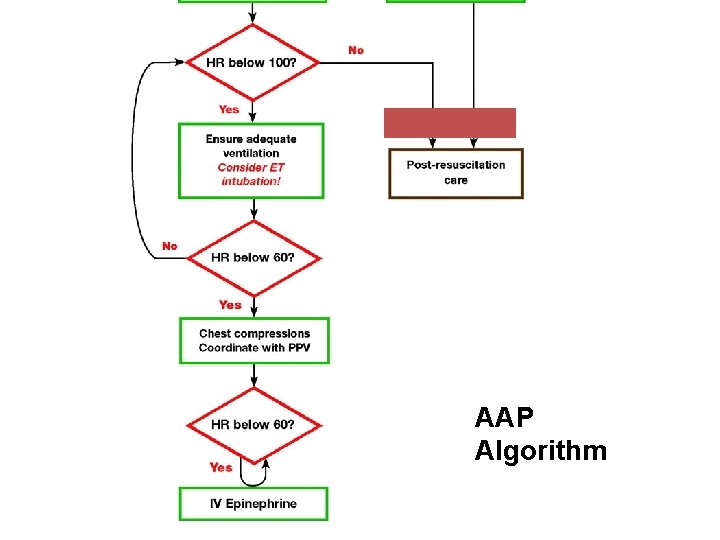
AAP Algorithm

Post resuscitation care • Needed for those who required PPV • At risk of deterioration – Hypo/hyperthermia , hypoglycemia, CNS complications(apnea, HIE), pulmonary complications(TTN, Pneumonia), hypotension • Need monitoring , evaluation • NICU may be necessary

NNR : not indicated • • • Conditions with certainly early death Extreme prematurity(GA<23 weeks) Birth weight<400 g Anencephaly Chromosomal abnormality: Trisomy 13

NNR: nearly always indicated • • High rate of survival Acceptable morbidity GA≥ 25 weeks Those with most congenital malformations

NNR? • Conditions associated with uncertain prognosis • Survival borderline • Parental desires concerning initiation of resuscitation should be supported

Discontinuing resuscitative efforts • Newborn with no detectable heart rate, consider stopping NNR if the heart rate remains undetectable for 10 minutes

Summary • Most infants transfer from intrauterine to extra uterine life • 10% need some intervention, 1% need extensive resuscitation • Anticipate the need for NNR • Adequate preparation for NNR • Evaluate the newborn as per AHA/AAP guidelines & follow the recommended protocol

MCQ 1 For successful neonatal resuscitation following is/are needed except: 1. Anticipation 2. Adequate preparation 3. Skilled personnel 4. Delayed initiation of support

MCQ 1 • For successful neonatal resuscitation following is/are needed except: 1. Anticipation 2. Adequate preparation 3. Skilled personnel 4. Delayed initiation of support

MCQ 2 • Following are true in relation to initial steps of neonatal resuscitation except 1. Provide warmth 2. Tactile stimulation 3. Endotracheal intubation 4. Drying the baby

MCQ 2 • Following are true in relation to initial steps of neonatal resuscitation except 1. Provide warmth 2. Tactile stimulation 3. Endotracheal intubation 4. Drying the baby

MCQ 3 • The following is the primary measure of adequate ventilation 1. Chest wall movement 2. Improvement in heart rate 3. Pink extremities 4. Spo 2 of 100%

MCQ 3 • The following is the primary measure of adequate ventilation 1. Chest wall movement 2. Improvement in heart rate 3. Pink extremities 4. Spo 2 of 100%

MCQ 4 Endotracheal intubation may be indicated at several points during neonatal resuscitation except 1. Ineffective BMV 2. During chest compressions 3. Vigorous meconium stained newborn 4. Non vigorous meconium stained newborn

MCQ 4 • Endotracheal intubation may be indicated at several points during neonatal resuscitation except 1. 2. 3. 4. Ineffective BMV During chest compressions Vigorous meconium stained newborn Non vigorous meconium stained newborn

MCQ 5 • The recommended compression to ventilation ratio in neonatal resuscitation is 1. 2: 1 2. 3: 1 3. 4: 1 4. 5: 1

MCQ 5 • The recommended compression to ventilation ratio in neonatal resuscitation is 1. 2: 1 2. 3: 1 3. 4: 1 4. 5: 1

MCQ 6 • The recommended dose(mg/kg per dose) and route of epinephrine in neonatal resuscitation 1. 0. 01 -0. 03, IV 2. 0. 01 -0. 03, IM 3. 0. 03 -0. 05, 1 V 4. 0. 05 -0. 1, IV

MCQ 6 • The recommended dose(mg/kg per dose) and route of epinephrine in neonatal resuscitation is 1. 0. 01 -0. 03, IV 2. 0. 01 -0. 03, IM 3. 0. 03 -0. 05, 1 V 4. 0. 05 -0. 1, IV

MCQ 7 • Recommended method/clinical indicator of confirming ET placement is 1. Condensation in ET 2. Chest movement 3. Equal breath sounds on auscultation 4. Exhaled C 02 Detection

MCQ 7 • Recommended method/clinical indicator of confirming ET placement is 1. Condensation in ET 2. Chest movement 3. Equal breath sounds on auscultation 4. Exhaled C 02 Detection
- Slides: 64