NEONATAL JAUNDICE Prof Kavitha K Objectives Define neonatal

NEONATAL JAUNDICE Prof. Kavitha K

Objectives • Define neonatal jaundice • Describe the Types of neonatal jaundice • Enlist the Causes of neonatal jaundices • Explain the Management of neonatal jaundice • List the complications
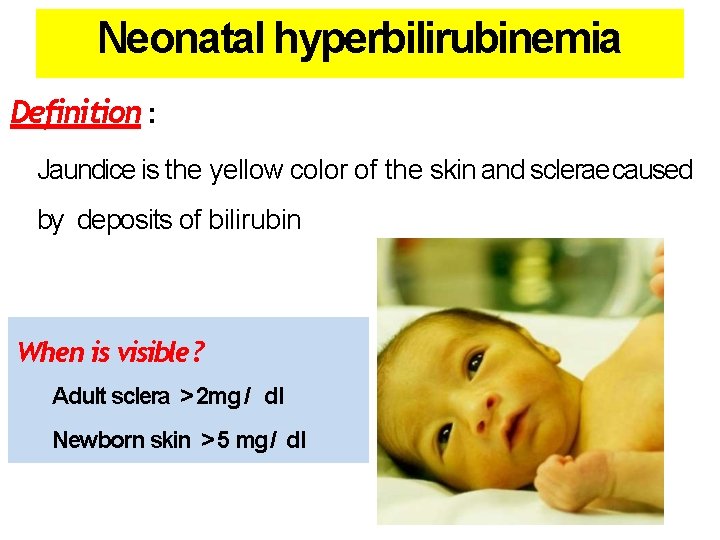
Neonatal hyperbilirubinemia Definition : Jaundice is the yellow color of the skin and sclerae caused by deposits of bilirubin When is visible ? Adult sclera > 2 mg / dl Newborn skin > 5 mg / dl

Incidence of neonatal jaundice Term : Occurs in 60% Preterm : 80% of preterm neonates Jaundice is the most common condition that requires medical attention in newborns.
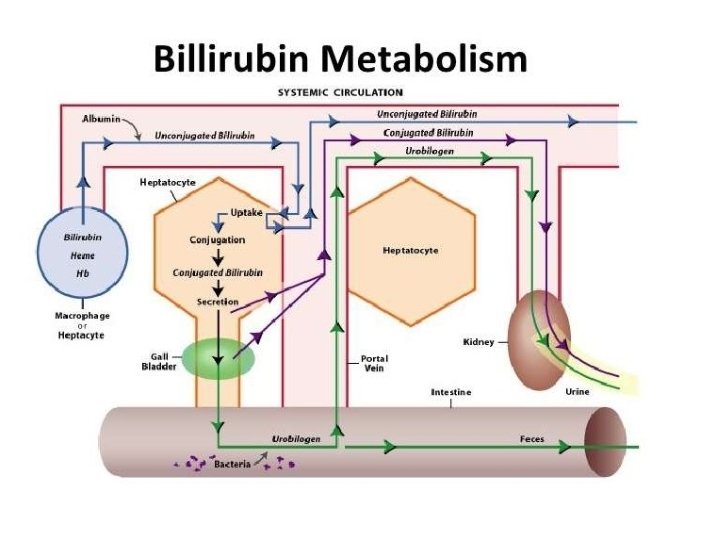
Bilirubin Metabolism
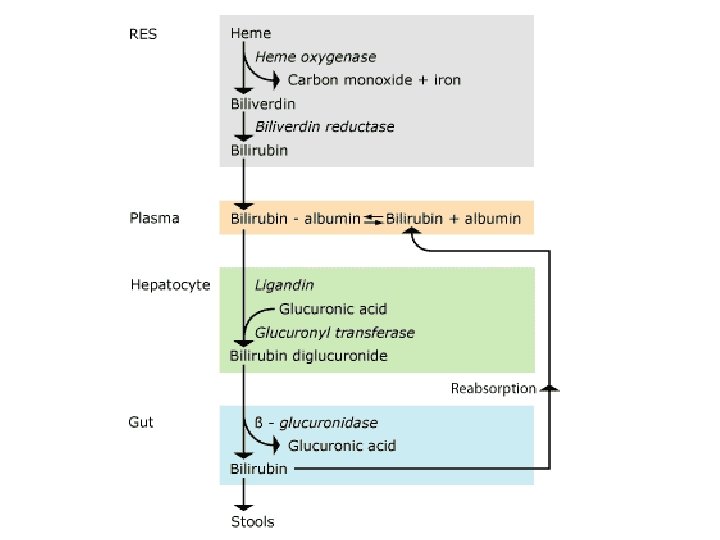

Types of bilirubin Unconjugated bilirubin (Indirect ) Conjugated bilirubin (Direct ) • Bind to albumen • Conjugated with glucoronic acid • Fat soluble • Water soluble • Can cross blood brain barrier • Excreted in urine and stool • Toxic in high level to brain • Not toxic

Etiology Of neonatal Jaundice

CAUSES

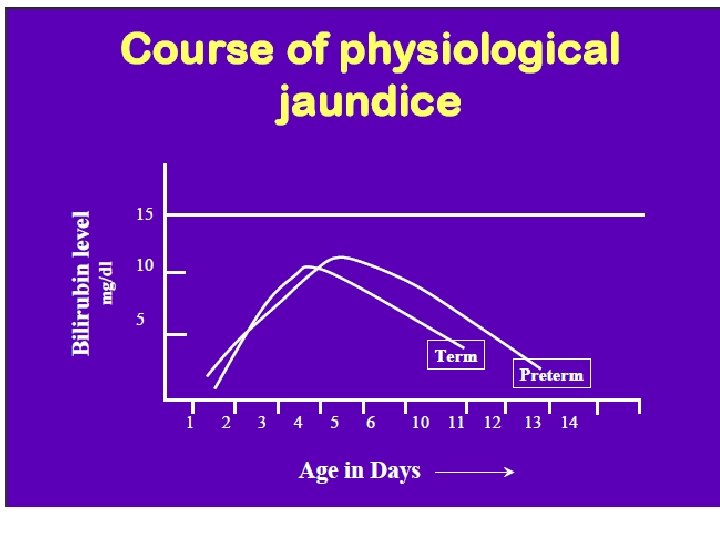
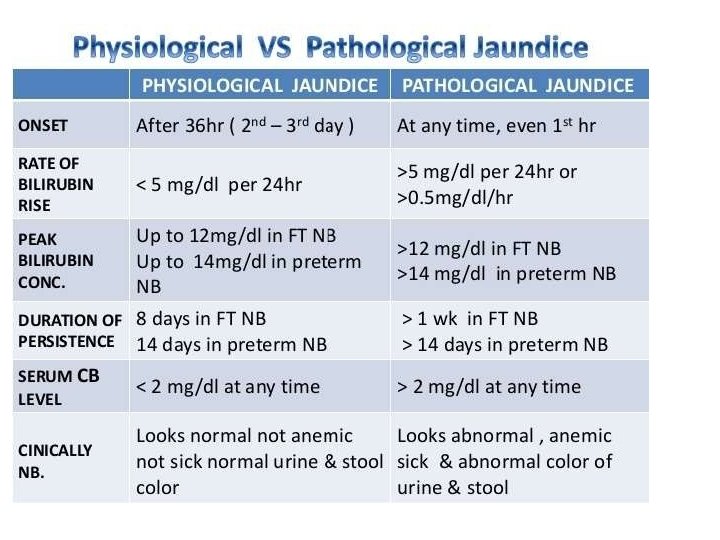
Physiological Jaundice Characteristics • Appears after 24 hours • Total bilirubin rises by less than 5 mg/dl per day • Maximum intensity by 4 th-5 th day in term & 7 th day in preterm • Serum level less than 15 mg / dl • Clinically not detectable after 14 days

Why does physiological jaundice develop? • Increased bilirubin load • Defective conjugation • Increased entero-hepatic circulation • Incidence – Term in 60% – Preterm 80%

Breast milk jaundice – It is caused by prolonged increased enterohepatic circulation of bilirubin. (β-GD↑) – Bilirubin peaks at 10 -15 days of age. – The level of unconjugated bil. is Breast-milk jaundice; is at 10 -30 mg/d. L – If nursing is interrupted for 24 hours, the bilirubin level falls quickly the commonest cause of Prolonged jaundice in term infants β glucuronidase present in the breast milk of somemothers)

Pathological Jaundice

Pathological jaundice 1. Appears age Appears within 24 hours of age 2. Increase of bilirubin > 5 mg / dl / day 3. Serum bilirubin > 15 mg / dl 4. Jaundice days Jaundice persisting after 14 days 5. Stool clay / white colored and urine staining yellow staining clothes 6. Direct bilirubin > 2 mg / dl
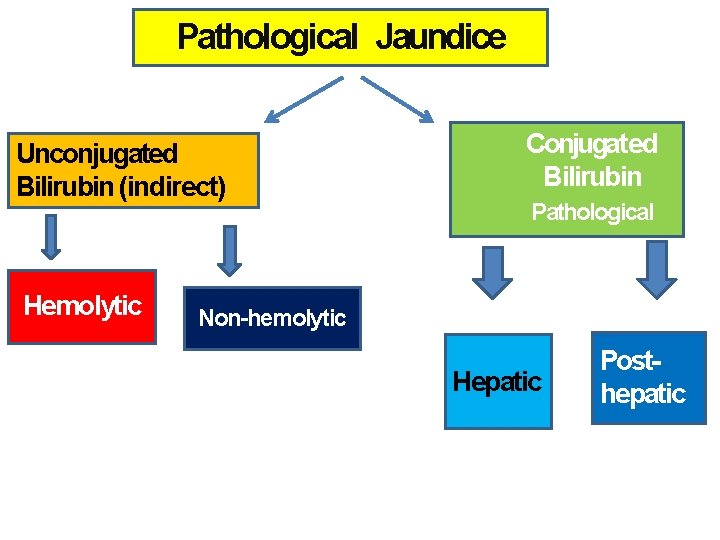
Pathological Jaundice Unconjugated Bilirubin (indirect) Hemolytic Conjugated Bilirubin Pathological Non-hemolytic Hepatic Posthepatic

Pathological jaundice 1 Unconjugated (Indirect) hyperbilirubinemia 1. Hemolysis • • • Rh , ABO and other blood group incompatibilities spherocytosis , elliptocytosis, Alpha thalassemia Sepsis , DIC Hematomas Polycythemia 2. Non hemolytic • • • Breast milk jaundice Crigler-Najjar syndrome, types I and II Gilbert syndrome

Hemolytic disease of the newborn – It is an isoimmunity hemolysis associated with – Rh incompatibility or – ABO
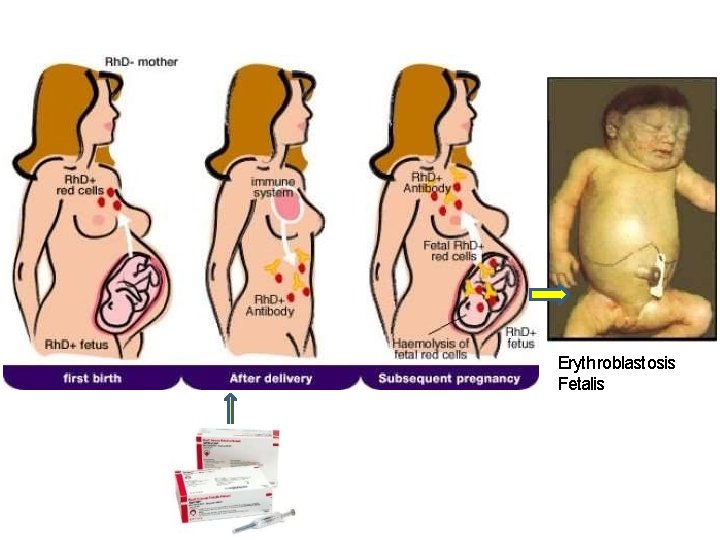
Erythroblastosis Fetalis

Hemolytic disease of the newborn due to ABO incompatibility • Mothers with type O blood may have circulating antibodies of Ig G class to other red cell antigens that can cross the placenta and cause hemolytic disease in a baby with a different blood type, such as blood type A or B. (ABO incompatibility ) • The baby develop jaundice in the 1 st day of life
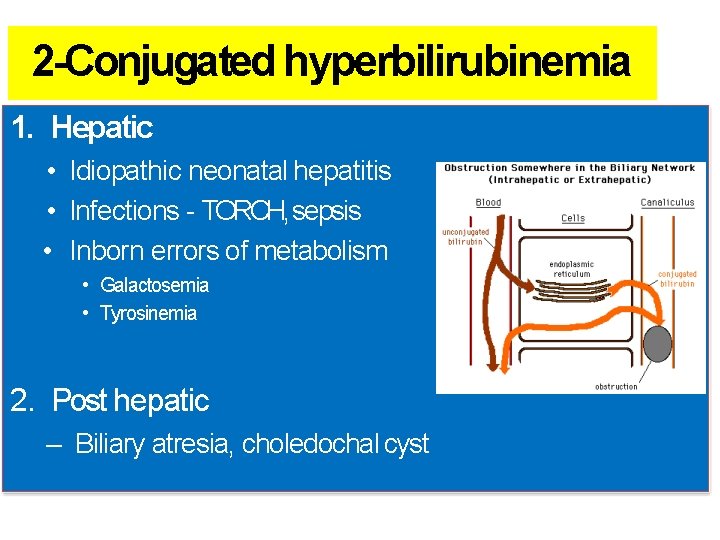
2 -Conjugated hyperbilirubinemia 1. Hepatic • Idiopathic neonatal hepatitis • Infections - TORCH, sepsis • Inborn errors of metabolism • Galactosemia • Tyrosinemia 2. Post hepatic – Biliary atresia, choledochal cyst

Jaundice accompanying G 6 PD deficiency: • Patients having G 6 PD deficiency also have genetic defects in bilirubin conjugation as seen in gilbert's disease. • It is uncommon to have jaundice in G 6 PD def infant due to severe hemolytic attack. • Those G 6 PD deficient neonates who develop higher maximal serum total bilirubin values had significantly lower serum conjugated bilirubin fractions.


• Crigler-Najjar syndrome type I - rare • Complete absence of UDPGT and is characterized by severe hyperbilirubinemia with the ongoing risk of kernicterus at any point during an individual's lifespan. • Currently, liver transplantation is the only definitive therapy • Patients with Crigler-Najjar syndrome type II partial absence of UDPGT similar to type I but dramatically respond to therapy with phenobarbital, which is how the diagnosis is made Glucuronyl transferase


Risk factors for jaundice • J- jaundice within first 24 hrs of life or premature • A - a sibling who was jaundiced as neonate • U - unrecognized hemolysis (ABO) • N nursing – non-optimal sucking/nursing • D - deficiency of G 6 PD , DRUGS, Ceftriaxone, • I - infection • C – Cephalhematoma /bruising • E- East Asian/North Indian

Assessment of jaundiced baby 1. Determine birth weight, gestation and postnatal age 2. Assess clinical condition (well or ill) , degree of jaundice 3. Decide whether jaundice is physiological or pathological 4. Look for evidence of kernicterus in deeply jaundiced NB
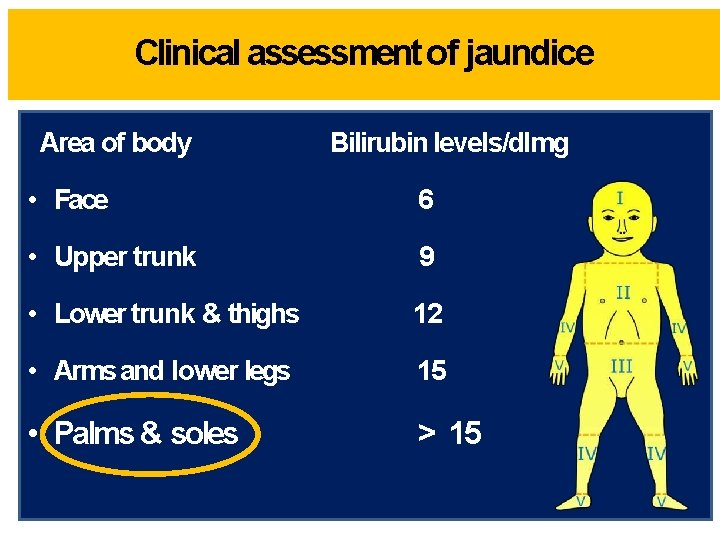
Clinical assessment of jaundice Area of body Bilirubin levels/dlmg • Face 6 • Upper trunk 9 • Lower trunk & thighs 12 • Arms and lower legs 15 • Palms & soles > 15
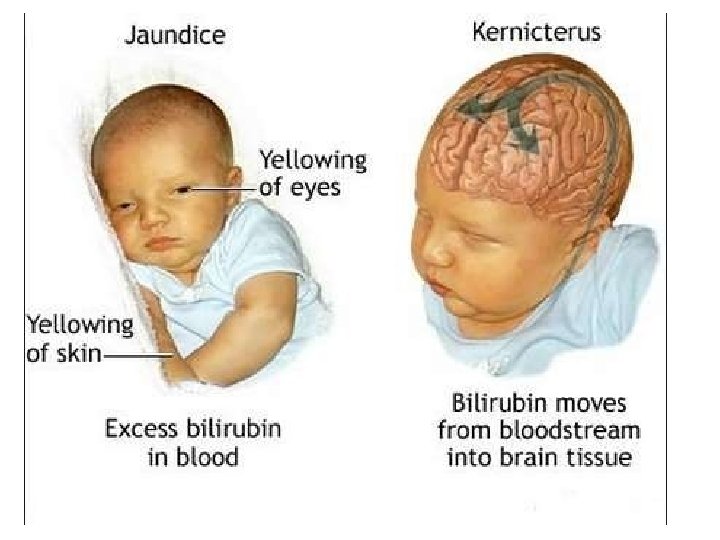
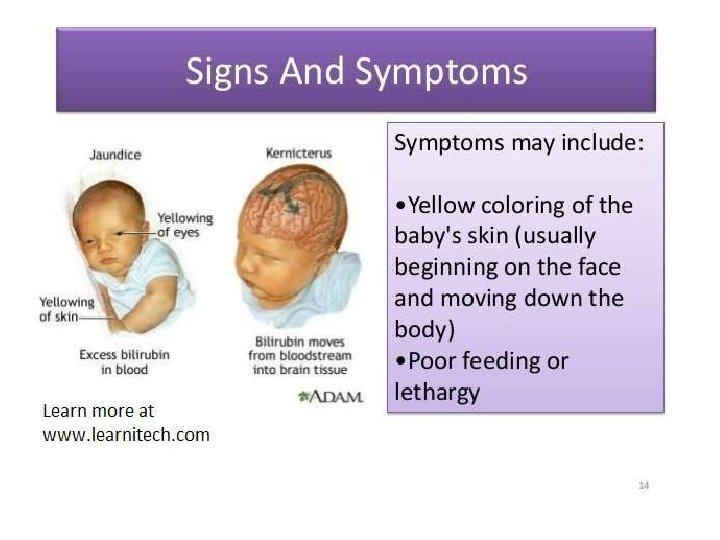
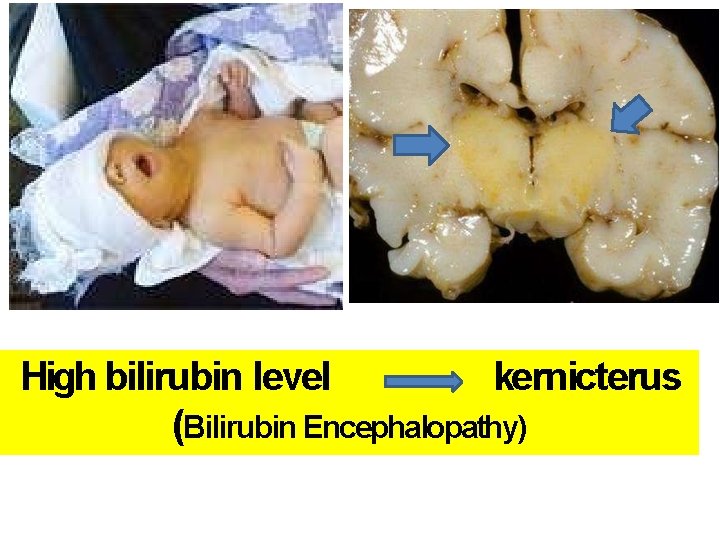
High bilirubin level kernicterus (Bilirubin Encephalopathy)
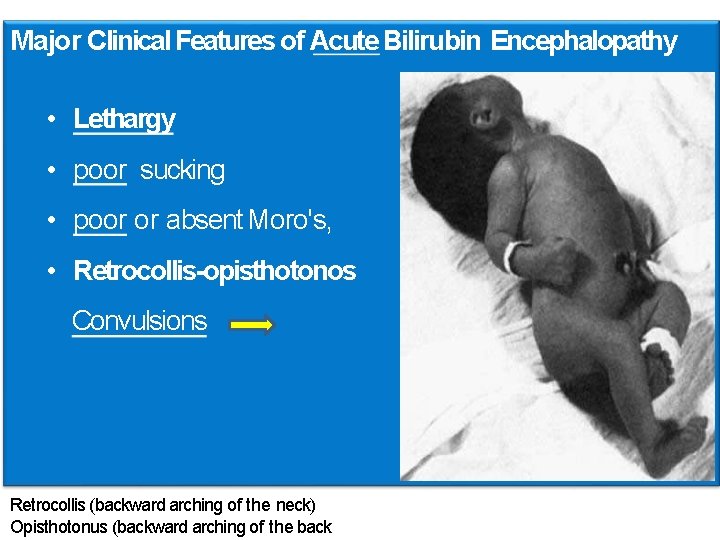
Major Clinical Features of Acute Bilirubin Encephalopathy • Lethargy • poor sucking • poor or absent Moro's, • Retrocollis-opisthotonos Convulsions Retrocollis (backward arching of the neck) Opisthotonus (backward arching of the back
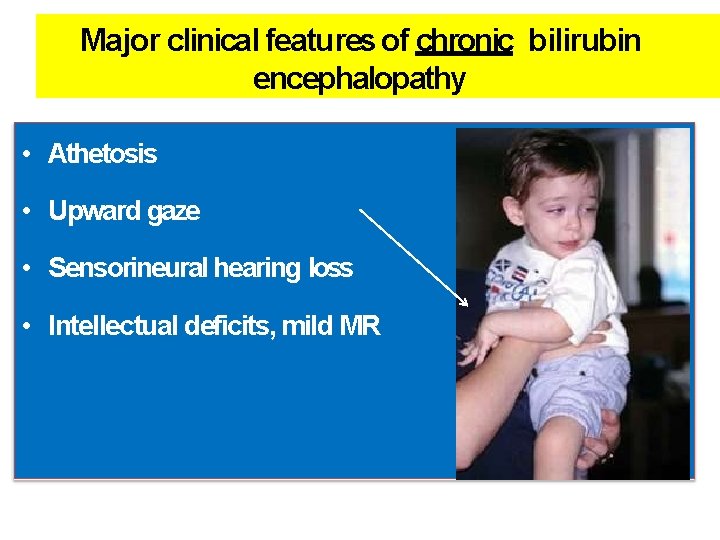
Major clinical features of chronic bilirubin encephalopathy • Athetosis • Upward gaze • Sensorineural hearing loss • Intellectual deficits, mild MR

Laboratory tests • • Total & direct bilirubin* Blood group and Rh for mother and baby* Hematocrit, retic count and peripheral smear* G 6 PD assay • Coomb’s test • • • Sepsis screen Liver and thyroid function TORCH titers Liver scan when conjugated hyperbilirubinemia Ultrasonography of the liver and bile ducts in cholestatsis (must in all)*
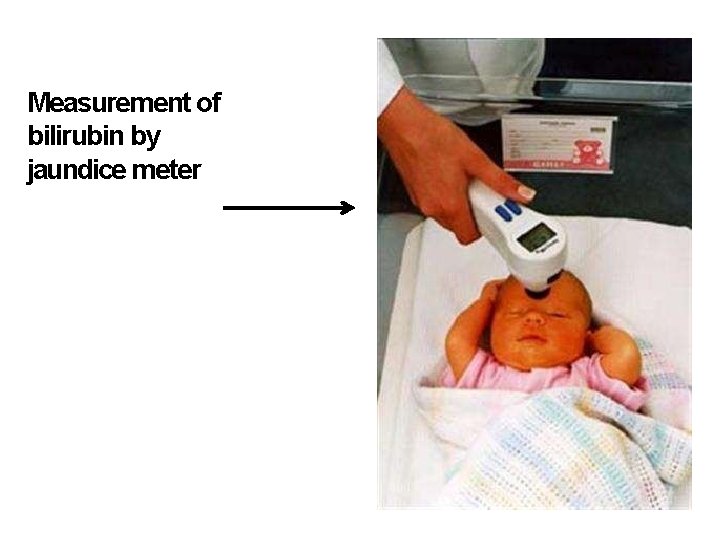
Measurement of bilirubin by jaundice meter

Laboratory Diagnosis Laboratory Features Of Hemolytic Disease Laboratory Features Rh blood type of Mother Rh negative blood type of Infant Rh positive ABO O A or B Anemia Marked Minimal Direct Commb’s test Positive Negative Indirect Commb’s test Positive Usually positive

Reticulocyte count (>7 mg/d. L) can indicate the presence of an ongoing hemolytic process in neonates Direct hyperbilirubinemia in the neonate is defined as a direct fraction more than 2 mg/d. L • or more than 20% of the total bilirubin concentration is always pathologic.

Liver function tests: • Aspartate aminotransferase (ASAT or SGOT)and alanine aminotransferase (ALAT or SGPT)levels are elevated in hepatocellular disease. • Alkaline phosphatase and γ -glutamyltransferase (GGT) levels are often elevated in cholestatic disease. • A γ -GT/ALAT ratio of more than 1 is strongly suggestive of biliary obstruction. However, it does not distinguish between intrahepatic and extrahepatic cholestasis (do ultrasoud) Reducing substance in urine: is a useful screening test for galactosemia, provided the infant has received sufficient quantities of milk.

Other Tests • Hearing tests (Brainstem auditory-evoked potentials) should be obtained in aftermath of severeneonatal jaundice to exclude sensorineural hearing loss. • MRI in kernicterus

Management 1. Phototherapy 2. intravenous immune globulin (IVIG) 3. Exchange transfusion 4. Drugs


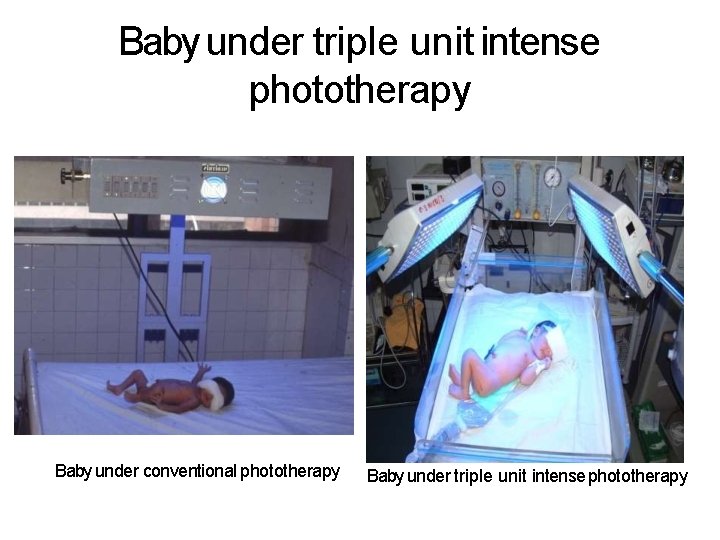
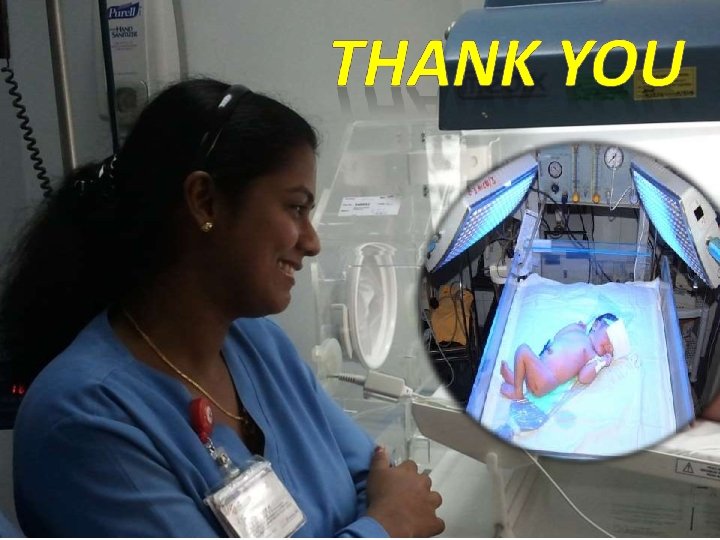
Baby under triple unit intense phototherapy Baby under conventional phototherapy Baby under triple unit intense phototherapy
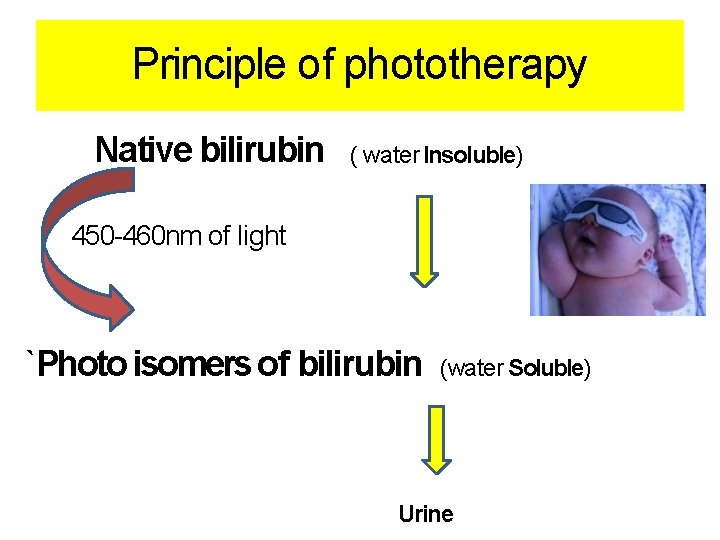
Principle of phototherapy Native bilirubin ( water Insoluble) 450 -460 nm of light `Photo isomers of bilirubin (water Soluble) Urine
Phototherapy Technique • • • Perform hand wash Place baby naked in cradle or incubator Fix eye shades Keep baby at least 45 cm from lights Start phototherapy Frequent extra breast feeding every 2 hourly Turn baby after each feed Temperature record 2 to 4 hourly Weight record- daily Monitor urine frequency Monitor bilirubin level

Side effects of phototherapy • • • Increased insensible water loss Loose stools Skin rash Bronze baby syndrome Hyperthermia May result in hypocalcemia

Intravenous immune globulin • IVIG in infants with Rh or ABO isoimmunization can significantly reduce the need for exchange transfusions. • Now IVIG has replaced exchange transfusion as the second-line treatment in infants with isoimmune jaundice. • 1 gm/kg/dose IV


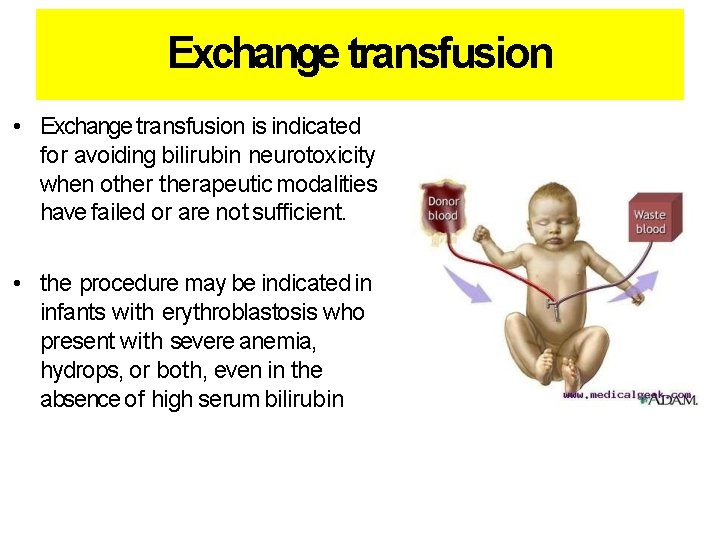
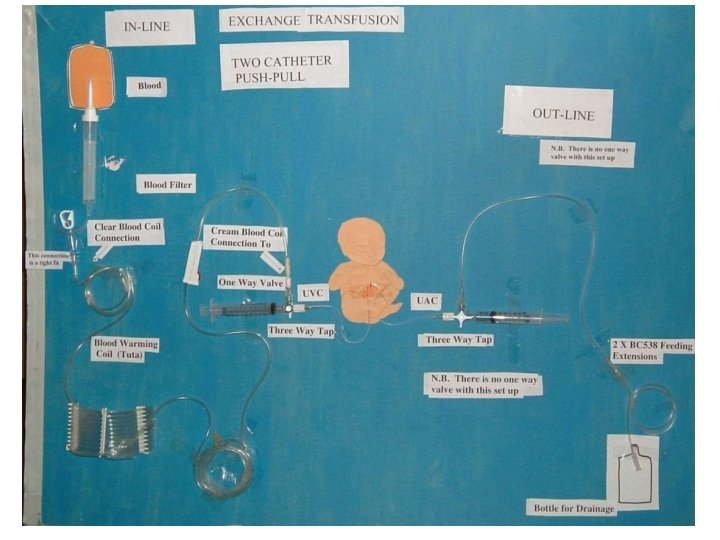
Exchange transfusion • Exchange transfusion is indicated for avoiding bilirubin neurotoxicity when otherapeutic modalities have failed or are not sufficient. • the procedure may be indicated in infants with erythroblastosis who present with severe anemia, hydrops, or both, even in the absence of high serum bilirubin

Phenobarbital (Luminal) • Hyperbilirubinemia: 3 -8 mg/kg/d PO/IV initially; may increase up to 12 mg/kg/d Not to exceed IV administration rate of 1 mg/kg/min or 30 mg/min for infants
Prolonged indirect jaundice Causes • Breast milk jaundice • Hypothyroidism • Pyloric stenosis • Ongoing hemolysis • Crigler Najjar syndrome

Conjugated hyperbilirubinemia Suspect • High colored urine • White or clay colored stool Caution • Always refer to hospital for investigations so that biliary atresia or metabolic disorderscan be diagnosed and managed early

Remember that: • Jaundice is the most frequent cause of admission after early discharge from nursery. • It is not physiological if: appear in first 24 hrs, increases by > 0. 5 mg/d. L/hr , evidence of hemolysis, abnormal examination, direct bilirubin is > 20% of total, or persists > 3 weeks. • Jaundice present in the first 24 hrs of life must be investigated and treated as an emergency.
- Slides: 60